Volume 15, Number 5—May 2009
Letter
Ovine Herpesvirus 2 Infection in Foal, Brazil
To the Editor: Malignant catarrhal fever (MCF) is an acute, generalized, and usually fatal disease previously thought to be restricted to mammals of the order Artiodactyla, often members of the subfamilies Bovinae, Cervidae, and Suidae (1). Although animals of the order Perissodactyla, family Equidae, have previously been considered not susceptible to ovine herpesvirus 2 (OvHV-2), we show that horses may be infected by this virus.
In July 2006, in the state of Minas Gerais, Brazil, neurologic signs developed acutely in a 6-month-old foal; signs included muscle spasms, rigidity of the neck and limbs, difficulty standing, and hind-limb paralysis. The foal also had severe dyspnea and profuse sweating and died 1 day after the onset of clinical signs.
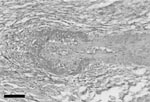
Histopathologic findings included a marked lympho-histiocytic fibrinoid necrotizing vasculitis affecting small blood vessels and arterioles in the kidney and liver (Figure) and associated with lymphocytic interstitial nephritis and mild multifocal granulomatous hepatitis. The vasculitis lesions were strikingly similar to those observed in cattle with MCF caused by OvHV-2 or alcelaphine herpesvirus 1. Both forms of the disease have a wide spectrum of clinical manifestations, but histopathologic findings for the 2 forms are similar (2,3). In addition, the foal had severe and diffuse interstitial pneumonia characterized by thickening of the alveolar walls and interstitial accumulation of macrophages, proliferation of type II pneumocytes, and accumulation of cell debri in the alveolar lumen. Granulomatous inflammation, characterized by mild multifocal to coalescent accumulation of epithelioid macrophages, was also observed in the spleen and lymph nodes. Surprisingly, the brain showed only moderate congestion and mild, multifocal, perivascular hemorrhage.
Although horses are not considered susceptible to OvHV-2, histopathologic findings in this case were consistent with MCF-like lesions. Thus, we looked for any history of direct or indirect contact between the affected foal and goats or sheep. Indeed, on this particular farm, horses shared food with 65 goats. On the basis of indirect contact with potential reservoirs of infection, the disease in the foal was suspected of being associated with a member of the MCF virus (MCFV) group (4).
To determine whether the disease in the foal was associated with an MCFV, we obtained tissue samples from the foal at necropsy and collected blood from all 3 adult horses, including the dam, and 10 randomly selected goats on the farm. DNA was extracted from these samples, and PCR was performed to detect members of the MCFV group, including OvHV-2 (5), caprine herpesvirus 2 (6), and alcelaphine herpesvirus 1 (7). The tissues from the foal as well as peripheral blood mononuclear cells from all 3 adult horses and 8 tested goats were positive for OvHV-2 only. The adult horses had no clinical signs of infection for at least 8 months after the outbreak.
To confirm the PCR detection of OvHV-2, we purified amplicons obtained from the dam of the affected foal, the affected foal, and 1 goat and processed them for automated sequencing. These nucleotide and deduced amino acid sequences were identical, and we deposited them in GenBank under accession nos. EU244694, EU718486, EU718487. PCR was conducted on tissue samples of the foal to test for differential diagnosis agents equine herpesvirus 1 (8), equine herpesvirus 4 (8), and equine arteritis virus (9). No amplification was observed. Considering that sheep and goats are the most important natural reservoirs of OvHV-2 (6), these results support the notion that infected goats were the most likely source of infection for horses in this outbreak.
To further support this diagnosis of OvHV-2 infection, we attempted to detect viral DNA in the vascular wall of the foal’s hepatic arterioles that contained fibrinoid necrotizing lympho-histiocytic vasculitis by using laser capture microdissection on sections stained with hematoxylin and eosin (10). DNA extracted from these areas was PCR positive for OvHV-2, which confirmed the co-localization of OvHV-2 DNA sequences in the site of MCF-like lesions.
Taken together, these findings confirm an emergent infectious disease associated with OvHV-2 infection in a horse, a species previously considered not susceptible to OvHV-2. The finding of vasculitis associated with intralesional OvHV-2 DNA sequences unequivocally demonstrates the pathogenic potential of this virus in foals. However, a cause-and-effect relationship between OvHV-2 infection and interstitial pneumonia as well as the granulomatous inflammation in the liver and spleen could not be established in this case. This report supports the notion that either equine infection is extremely rare or that this strain of OvHV-2 underwent recent modifications that expanded the host range.
Acknowledgments
We thank Maria do Carmo C. S. H. Lara for performing the equine arteritis diagnostic tests.
Financial support was provided by Conselho Nacional de Desenvolvimento Científico e Tecnológico, Coordenação de Aperfeiçoamento de Pessoal de Nível Superior, and Fundação de Amparo à Pesquisa do Estado de Minas Gerais.
References
- Animal Health Australia. Malignant catarrhal fever. Australian situation [cited 2008 Jul 26]. Available from http://www.animalhealthaustralia.com.au/programs/adsp/nahis/diseases/mcf.cfm
- O'Toole D, Li H, Roberts S, Rovnak J, DeMartini J, Cavender J, Chronic generalized obliterative arteriopathy in cattle: a sequel to sheep-associated malignant catarrhal fever. J Vet Diagn Invest. 1995;7:108–21.PubMedGoogle Scholar
- Anderson IE, Buxton D, Campbell I, Russell G, Davis WC, Hamilton MJ, Immunohistochemical study of experimental malignant catarrhal fever in rabbits. J Comp Pathol. 2007;136:156–66. DOIPubMedGoogle Scholar
- Simon S, Li H, O'Toole D, Crawford TB, Oaks JL. The vascular lesions of a cow and bison with sheep-associated malignant catarrhal fever contain ovine herpesvirus 2–infected CD8(+) T lymphocytes. J Gen Virol. 2003;84:2009–13. DOIPubMedGoogle Scholar
- Baxter SI, Pow I, Bridgen A, Reid HW. PCR detection of the sheep-associated agent of malignant catarrhal fever. Arch Virol. 1993;132:145–59. DOIPubMedGoogle Scholar
- Li H, Keller J, Knowles DP, Crawford TB. Recognition of another member of the malignant catarrhal fever virus group: an endemic gammaherpesvirus in domestic goats. J Gen Virol. 2001;82:227–32.PubMedGoogle Scholar
- Katz J, Seal B, Ridpath J. Molecular diagnosis of alcelaphine herpesvirus (malignant catarrhal fever) infections by nested amplification of viral DNA in bovine blood buffy coat specimens. J Vet Diagn Invest. 1991;3:193–8.PubMedGoogle Scholar
- Varrasso A, Dynon K, Ficorilli N, Hartley CA, Studdert MJ, Drummer HE. Identification of equine herpesviruses 1 and 4 by polymerase chain reaction. Aust Vet J. 2001;79:563–9. DOIPubMedGoogle Scholar
- Echeverria MG, Pecoraro MR, Galosi CM, Etcheverrigaray ME, Nosetto EO. The first isolation of equine arteritis in Argentina. Rev Sci Tech. 2003;22:1029–33.PubMedGoogle Scholar
- Emmert-Buck MR, Bonner RF, Smith PD, Chuaqui RF, Zhuang Z, Goldstein SR, Laser capture microdissection. Science. 1996;274:998–1001. DOIPubMedGoogle Scholar
Figure
Cite This ArticleRelated Links
Table of Contents – Volume 15, Number 5—May 2009
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Érica Azevedo Costa, Laboratório de Patologia Molecular, Departamento de Clínica e Cirurgia Veterinárias, Escola de Veterinária, Universidade Federal de Minas Gerais, Av Antônio Carlos, 6627, CEP 30123-970, Belo Horizonte, MG, Brazil
Top