Volume 18, Number 8—August 2012
Dispatch
Klebsiella pneumoniae in Gastrointestinal Tract and Pyogenic Liver Abscess
Abstract
To determine the role of gastrointestinal carriage in Klebsiella pneumoniae liver abscess, we studied 43 patients. Bacterial isolates from liver and fecal samples from 10 patients with this condition and 7 healthy carriers showed identical serotypes and genotypes with the same virulence. This finding indicated that gastrointestinal carriage is a predisposing factor for liver abscess.
Klebsiella pneumoniae has emerged as the predominant cause of pyogenic liver abscess in Taiwan and other countries in eastern and Southeast Asia (1–4). This condition is frequently associated with severe complications, including septic endophthalmitis and other extrahepatic lesions, especially in patients with diabetes (1).
In Taiwan, the annual incidence of pyogenic liver abscess has increased steadily from 11.15 cases/100,000 persons in 1996 to 17.59 cases/100,000 persons in 2004, and K. pneumoniae was found in 79.9% of culture-positive cases (5). We showed that >3,000 new cases of pyogenic liver abscess were found each year during 2005–2008 (6). However, the pathogenesis of K. pneumoniae liver abscess remains unclear, and the source of endogenous or exogenous infections has been debated.
To determine whether strains recovered from liver aspirate samples originated from gastrointestinal flora of patients, we investigated isolates from liver aspirate, nasal swab, saliva, and fecal samples by using genomic analysis. Using serotyping and molecular typing methods, we systematically investigated the association between isolates from liver aspirates and those from other body sites in patients with K. pneumoniae liver abscess. We also investigated K. pneumoniae isolates from healthy carriers that were genetically similar to liver abscess isolates to assess whether colonization of virulent K. pneumoniae occurs in these persons, which could subsequently lead to development of liver abscess.
During January 2009–December 2010, a total of 43 adult patients (mean age 68.2 years) with liver aspirate cultures positive for K. pneumoniae in Taipei Veterans General Hospital were consecutively enrolled in the study. All cases of K. pneumoniae liver abscess were community acquired. Clinical characteristics of patients are shown in Table 1.
To determine whether K. pneumoniae liver abscess originated from the gastrointestinal tract of patients, we concomitantly tested all liver aspirate, saliva, nasal swab, fecal, and blood samples by using bacterial culture before patients were treated with antimicrobial drugs. A total of 125 K. pneumoniae isolates from 43 patients were obtained. Information on culture-positive sites is shown in the Technical Appendix Table. To compare virulence and genetic relatedness of K. pneumoniae from liver abscess patients and healthy carriers, we obtained 1,000 K. pneumoniae isolates from fecal samples of asymptomatic adults during routine physical examinations at the Tri-Service General Hospital (Taipei, Taiwan).
All clinical K. pneumoniae isolates were serotyped by using countercurrent immunoelectrophoresis with serotype K antiserum. Isolates with serotypes K1 and K2 were confirmed by PCR (7). All K1 isolates were screened for CC23 representatives by detection of the allS gene by using PCR as described (7). Seroepidemiologic study of K. pneumoniae isolates from liver abscess patients showed that serotypes K1 and K2 were predominant, accounting for 61% (26/43) and 16% (7/43) of all isolates, respectively.
All K1 isolates had the allS gene, which is consistent with results of a study that showed that the virulent K1 clone of CC23 is associated pyogenic liver abscess (7). Although there was no difference in clinical characteristics between K1/K2 and non-K1/K2 patients, complications of distal septic metastasis (9%) and death (mortality rate 12%) were found for the K1/K2 group (Table 1).
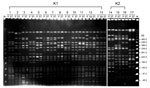
A total of 17 randomly selected pairs of representative K. pneumoniae isolates (from liver aspirate, saliva, and fecal samples), including serotypes K1 (13 isolates), K2 (3 isolates), and non-K1/K2 (1 isolate), from patients with liver abscess were subjected to pulsed-field gel electrophoresis (PFGE) analysis with XbaI. All liver aspirate isolates had a PFGE profile identical or closely related to those of fecal or saliva samples from the same patient (Figure 1). Isolates from different patients that belonged to serotypes K1 and K2 were distinguishable from each another, indicating epidemiologic unrelatedness of these strains.
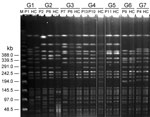
Among 17 patients, PFGE matching of liver aspirate K. pneumoniae isolates to isolates from fecal samples of 1,000 healthy adults was performed by using computer program analysis. PFGE showed that 7 groups of serotype K1 K. pneumoniae isolated from fecal samples from 10 patients and 7 healthy carriers had identical and >90% similarity in PFGE patterns (Figure 2). No serotype K2 or non-K1/K2 isolates could be matched with other isolates from healthy carriers.
The rmpA and aerobactin virulence genes were detected in all K1/K2 isolates (8). In vitro and in vivo assays to assess virulence were performed by using neutrophil phagocytosis and serum resistance assays as described (9). PCR showed that rmpA and aerobactin virulence genes were present in all 17 matched isolates from liver aspirate specimens and healthy carriers. Virulence assessment demonstrated that groups 1–6 (except patient 7) were resistant to phagocytosis and showed evidence of serum resistance (Table 2). In mouse lethality assays, various 50% lethal dose (LD50) were observed among 7 groups of isolates from liver aspirates. Similar LD50 values were observed among all 7 groups of isolates, indicating no difference in virulence between isolates from patients and those from healthy carriers, and that the healthy adults carried the virulent strains in their intestines
Molecular typing of the K. pneumoniae strains from different patients showed different patterns, indicating epidemiologic unrelatedness of these strains, a finding that excludes a common origin of K. pneumoniae and transmission between patients. All PFGE profiles for liver aspirate isolates were identical or clonally related to those for isolates from fecal samples, suggesting that these infections originated from patient flora.
A previous study showed that serotype K1 and K2 isolates with aerobactin and rampA genes were more virulent (10). We found 3 isolates from patient 7, patient 4, and healthy carrier 7 that had aerobactin and rmpA genes and were less virulent than other matched groups. This finding is compatible with results of our previous investigation (8). Thus, development of K. pneumoniae liver abscesses probably results from a combination of virulence determinants rather than a single factor (8). Furthermore, we found that 6 groups of serotype K1 K. pneumoniae strains isolated from liver abscess patients (not patient 7) and 6 from healthy carriers had identical PFGE profiles with the same virulence-associated genes and similar LD50 values. This finding indicated that healthy adults had virulent strains in their gastrointestinal tracts.
Although K. pneumoniae liver abscess might be induced by inhalation of K. pneumoniae and a bacteremic phase, we showed that none of 49 patients with community-acquired pneumonia and bacteremia caused by K. pneumoniae showed development of K. pneumoniae liver abscess concomitantly (11). A study from Japan reported familial spread of a virulent K1 clone causing K. pneumoniae liver abscess (12). In this study, 1 family member without K. pneumoniae liver abscess had the same clone in her feces (12). Thus, the route of entry is probably from the gastrointestinal tract. An animal study demonstrated that K. pneumoniae strains with genetic regulatory networks for translocation have the ability to cross the intestinal barrier and cause liver abscess (13).
Carrier rates of K. pneumoniae have differed considerably among studies. The rate of detection in fecal samples from healthy persons ranged from 19.4% to 38% in studies in Europe (14). In a recent investigation, we reported a fecal carriage rate of K. pneumoniae in healthy adults of 75% and high prevalence (23%, 17/76) of serotype K1/K2 isolates among typeable strains in Taiwan (15). The high carriage of virulent K. pneumoniae strains in feces is probably the reason why there are so many cases of K. pneumoniae liver abscess in Taiwan.
Our study demonstrated that intestinal colonization of virulent type K. pneumoniae is highly associated with pyogenic liver abscess. Early detection of colonization by K. pneumoniae, especially serotypes K1 and K2 in patients with diabetes, might help with making treatment decisions for infected patients.
Dr Fung is an attending physician at the Taipei Veterans General Hospital. His research interests included pathogenesis of K. pneumoniae infections and antimicrobial drug resistance.
Acknowledgment
This study was supported by a research grant (NSC-93-2314-B-010-062) from the National Science Council of Taiwan and partially supported by the National Health Research Institutes and Taipei Veterans General Hospital (V99C1-115).
References
- Fung CP, Chang FY, Lee SC, Hu BS, Kuo BI, Liu CY, A global emerging disease of Klebsiella pneumoniae liver abscess: is serotype K1 an important factor for complicated endophthalmitis? Gut. 2002;50:420–4. DOIPubMedGoogle Scholar
- Ko WC, Paterson DL, Sagnimeni AJ, Hansen DS, Von Gottberg A, Mohapatra S, Community-acquired Klebsiella pneumoniae bacteremia: global differences in clinical patterns. Emerg Infect Dis. 2002;8:160–6. DOIPubMedGoogle Scholar
- Yeh KM, Kurup A, Siu LK, Koh YL, Fung CP, Lin JC, Capsular serotype K1 or K2, rather than magA and rmpA, is a major virulence determinant for Klebsiella pneumoniae liver abscess in Singapore and Taiwan. J Clin Microbiol. 2007;45:466–71. DOIPubMedGoogle Scholar
- Chung DR, Lee SS, Lee HR, Kim HB, Choi HJ, Eom JS, Emerging invasive liver abscess caused by K1 serotype Klebsiella pneumoniae in Korea. J Infect. 2007;54:578–83. DOIPubMedGoogle Scholar
- Tsai FC, Huang YT, Chang LY, Wang JT. Pyogenic liver abscess as endemic disease, Taiwan. Emerg Infect Dis. 2008;14:1592–600. DOIPubMedGoogle Scholar
- Lin YT, Liu CJ, Chen TJ, Chen TL, Yeh YC, Wu HS, Pyogenic liver abscess as the initial manifestation of underlying hepatocellular carcinoma. Am J Med. 2011;124:1158–64. DOIPubMedGoogle Scholar
- Turton JF, Perry C, Elgohari S, Hampton CV. PCR characterization and typing of Klebsiella pneumoniae using capsular type-specific, variable number tandem repeat and virulence gene targets. J Med Microbiol. 2010;59:541–7. DOIPubMedGoogle Scholar
- Fung CP, Chang FY, Lin JC, Ho DM, Chen CT, Chen JH, Immune response and pathophysiological features of Klebsiella pneumoniae liver abscesses in an animal model. Lab Invest. 2011;91:1029–39. DOIPubMedGoogle Scholar
- Lin JC, Chang FY, Fung CP, Yeh KM, Chen CT, Tsai YK, Do neutrophils play a role in establishing liver abscesses and distant metastases caused by Klebsiella pneumoniae? PLoS ONE. 2010;5:e15005. DOIPubMedGoogle Scholar
- Yu VL, Hansen DS, Ko WC, Sagnimeni A, Klugman KP, von Gottberg A, Virulence characteristics of Klebsiella and clinical manifestations of K. pneumoniae bloodstream infections. Emerg Infect Dis. 2007;13:986–93. DOIPubMedGoogle Scholar
- Lin YT, Jeng YY, Chen TL, Fung CP. Bacteremic community-acquired pneumonia due to Klebsiella pneumoniae: clinical and microbiological characteristics in Taiwan, 2001–2008. BMC Infect Dis. 2010;10:307. DOIPubMedGoogle Scholar
- Harada S, Tateda K, Mitsui H, Hattori Y, Okubo M, Kimura S, Familial spread of a virulent clone of Klebsiella pneumoniae causing primary liver abscess. J Clin Microbiol. 2011;49:2354–6. DOIPubMedGoogle Scholar
- Tu YC, Lu MC, Chiang MK, Huang SP, Peng HL, Chang HY, Genetic requirements for Klebsiella pneumoniae–induced liver abscess in an oral infection model. Infect Immun. 2009;77:2657–71. DOIPubMedGoogle Scholar
- Smith GW, Blackwell CC, Nuki G. Faecal flora in spondyloarthropathy. Br J Rheumatol. 1997;36:850–4. DOIPubMedGoogle Scholar
- Lin YT, Siu LK, Lin JC, Chen TL, Tseng CP, Yeh KM, Seroepidemiology of Klebsiella pneumoniae colonizing the intestinal tract of healthy Chinese and overseas Chinese adults in Asian countries. BMC Microbiol. 2012;12:13. DOIPubMedGoogle Scholar
Figures
Tables
Cite This ArticleTable of Contents – Volume 18, Number 8—August 2012
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Chang-Phone Fung, Division of Infectious Diseases, Department of Medicine, Taipei Veterans General Hospital, No. 201, Section 2, Shih-Pai Rd, Taipei, 11217, Taiwan, Republic of China
Top