Volume 19, Number 3—March 2013
Letter
Armillifer armillatus Pentastomiasis in African Immigrant, Germany
To the Editor: Pentastomiasis is a parasitic zoonotic disease with an incremental number of reported human infections caused by larval stages (nymphs) of pentastomes (1–3). The vermiform parasites are in their own phylum and are related to branchiuran crustaceans (2). Most human infections with these parasites are caused by Armillifer armillatus (2), a parasite endemic to western and central Africa. Most cases are reported from the Congo region and Nigeria, and occasionally infections in African immigrants to Europe and North America have been reported (4,5). Imported cases to Germany have not been reported. A. grandis, a related parasite from central Africa, has been rarely found (6), but A. moniliformis, a pentastome species from Asia, has recently reemerged and caused a human infection after ≈40 years in Malaysia (1).
Adult Armillifer spp. inhabit the respiratory tract of large snakes (Python spp.). These dioecious parasites produce large amounts of ova that are shed into the environment by snake feces and secretions. When intermediate hosts, such as rodents or other small mammals, ingest ova, larvae hatch, migrate to the viscera, encyst, and molt several times (3). Humans become accidental intermediate hosts after uptake of environmental parasite ova or by consumption of contaminated snake meat. We report an infection with A. armillatus in an African immigrant to Germany that was diagnosed by histopathologic analysis and confirmed by PCR.
In 2005, a 23-year-old man from Togo who had immigrated to Germany 3 years earlier showed development of acute myeloid leukemia. He subsequently underwent stem cell transplantation, which was followed by graft versus host disease. The patient died of sudden intracerebral hemorrhage and leukencephalopathy. His medical history also included α-thalassemia and a heterocygotous sickle cell trait, chronic hemolytic anemia, splenomegaly, and cardiomyopathy. He had been treated for schistosomiasis and filariasis.
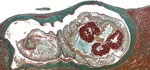
An autopsy specimen showed several living pentastome nymphs of ≈2 cm in size, which were found in the subscapular region of liver parenchyma. A presumptive diagnosis of visceral pentastomiasis caused by A. armillatus nymphs was made in accordance with the origin of the patient and the geographic distribution of the parasite.
Microscopic slides from patient specimens were retrieved from an archive and reanalyzed (Figure, Technical Appendix Figure). A pentastome-specific PCR targeting the 18S rRNA gene (2,7) was conducted after DNA extraction from formalin-fixed tissue on a remaining unstained microscope slide. The resulting 383-bp amplicon was sequenced, and BLAST analysis (www.ncbi.nlm.hih.gov/blast) confirmed 100% identity with A. armillatus (GenBank accession no. HM756289.1) and 99% homology with A. agkistrodontis (FJ607339.1) and A. moniliformis (HM048870.1).
Visceral pentastomiasis in humans is often asymptomatic and an incidental finding during surgery (1,3) or autopsy (8,9). In a large autopsy series from Malaysia, a pentastomiasis prevalence of 45.5% was found in adult Aborigines (8). In Nigeria, a rate of 33% was seen during autopsies of patients who had died of malignancies (9). However, a few severe and even lethal cases have been described for heavy A. armillatus and A. grandis infections in persons from Africa (4,6).
Diagnosis is achieved by gross pathologic and histopathologic analyses. Nymphs are found in the serosa around the liver and spleen, in liver parenchyma, mesenterium, intestine wall, and abdominal lymph nodes. The lungs or pleura are occasionally infected (3). Radiographic analysis may show typical C-shaped chest or abdominal calcifications (10). Species identification is performed by counting annulations (A. armillatus 18–22, A. grandis >25) and measuring the size of larval parasites (3). Recently, PCR has been used for diagnosis in veterinary infections (2,7).
For the patient in our study, molecular analysis identified human pentastomiasis by using a formalin-fixed microscope slide that had been stored for 7 years. A difference of 2 nt each was seen when the amplified nucleotide sequence was compared with database sequences of A. agkistrodontis and A. moniliformis. However, there is no database entry in GenBank for A. grandis, the geographically closest Armillifer species. Serologic assays have been developed for identification of A. armillatus (2), but no serum was available for retrospective analysis. In special settings, such as tropical snake farming and pet keeping, pentastomiasis may be a public health concern (2). However, most infections have been linked to consumption of undercooked snake meat or other snake products (1).
Most immigrants who were given a diagnosis of visceral pentastomiasis were from Nigeria or the Congo region, and diagnoses were made after death. Molecular analysis is particularly valuable when only autoptic paraffin-embedded patient material is available. For industrialized countries, where experience in morphologic identification of unusual parasite species is limited, molecular analysis is a valuable diagnostic tool. Our case-patient constitutes a record of imported Armillifer species pentastomiasis to Germany. Because of increasing international migration, more cases of pentastomiasis are likely to be seen.
References
- Latif B, Omar E, Heo CC, Othman N, Tappe D. Human pentastomiasis caused by Armillifer moniliformis in Malaysian Borneo. Am J Trop Med Hyg. 2011;85:878–81. DOIPubMedGoogle Scholar
- Tappe D, Meyer M, Oesterlein A, Jaye A, Frosch M, Schoen C, Transmission of Armillifer armillatus ova at snake farm, The Gambia, West Africa. Emerg Infect Dis. 2011;17:251–4. DOIPubMedGoogle Scholar
- Tappe D, Büttner DW. Diagnosis of human visceral pentastomiasis. PLoS Negl Trop Dis. 2009;3:e320. DOIPubMedGoogle Scholar
- Lavarde V, Fornes P. Lethal infection due to Armillifer armillatus (Porocephalida): a snake-related parasitic disease. Clin Infect Dis. 1999;29:1346–7. DOIPubMedGoogle Scholar
- Guardia SN, Sepp H, Scholten T, Morava-Protzner I. Pentastomiasis in Canada. Arch Pathol Lab Med. 1991;115:515–7.PubMedGoogle Scholar
- Cagnard V, Nicolas-Randegger J, Dago Akribi A, Rain B, Nozais JP, Essoh Nomel P, Generalized and lethal pentastomiasis due to Armillifer grandis (Hett, 1915) [in French]. Bull Soc Pathol Exot. 1979;72:345–52.PubMedGoogle Scholar
- Brookins MD, Wellehan JF, Roberts JF, Allison K, Curran SS, Childress AL, Massive visceral pentastomiasis caused by Porocephalus crotali in a dog. Vet Pathol. 2009;46:460–3. DOIPubMedGoogle Scholar
- Prathap K, Lau KS, Bolton JM. Pentastomiasis: a common finding at autopsy among Malaysian aborigines. Am J Trop Med Hyg. 1969;18:20–7 .PubMedGoogle Scholar
- Smith JA, Oladiran B, Lagundoye SB. Pentastomiasis and malignancy. Ann Trop Med Parasitol. 1975;69:503–12.
- Tiendrebeogo H, Levy D, Schmidt D. Human pentastomiasis in Abidjan. A report on 29 cases [in French]. Rev Fr Mal Respir. 1982;10:351–8 .PubMedGoogle Scholar
Figure
Cite This ArticleRelated Links
Table of Contents – Volume 19, Number 3—March 2013
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Dennis Tappe, Institute of Hygiene and Microbiology, University of Würzburg, Josef-Schneider-Str 2, 97080 Würzburg, Germany
Top