Volume 20, Number 2—February 2014
Dispatch
Reemergence of Rift Valley Fever, Mauritania, 2010
Abstract
A Rift Valley fever (RVF) outbreak in humans and animals occurred in Mauritania in 2010. Thirty cases of RVF in humans and 3 deaths were identified. RVFV isolates were recovered from humans, camels, sheep, goats, and Culex antennatus mosquitoes. Phylogenetic analysis of isolates indicated a virus origin from western Africa.
Rift Valley fever (RVF) is an acute febrile viral disease that affects domestic ruminants and humans. The disease in animals is characterized by abortions among pregnant females and high mortality rates for offspring (1). The causative pathogen, RVF virus (RVFV), is a member of the family Bunyaviridae, genus Phlebovirus, and its genome consists of 3 RNA segments: large (L), medium (M), and small (S) (2). In human infections, symptoms are generally mild but may evolve to severe symptoms, such as hemorrhaging, meningoencephalitis, and retinopathy, with fatal outcomes (3). RVF is endemic to sub-Saharan Africa, Egypt, Saudi Arabia, and Yemen (4). In western Africa, a major RVF outbreak occurred in Mauritania and Senegal in 1987 and resulted in 220 human deaths (5). This outbreak was followed by epizootics/epidemics in 1998 and 2003 in different provinces in Mauritania (Hodh El Gharbi, Assaba, Brakna, Trarza, and Gorgol Provinces) (6,7).
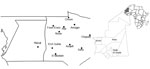
In October 2010, the health services of Adrar Province in Mauritania were informed of the deaths of 2 girls with hemorrhagic syndromes and 2 persons with acute fever, arthralgia, and headaches in Amogjar Province. Blood samples collected from a sick patient were sent to Institut Pasteur in Dakar, Senegal where RVFV IgM and RVFV genome were detected. During October 28–November 11, 2010, suspected RVF cases were identified in several cities Adar Province (Atar, Aoujeft, Chinguetti), Inchiri Province (Akjoujt), and Hodh el Gharbi Province (Tintane, Kobeni) (Figure 1), and high mortality rates among camels, sheep, and goats were reported in Adrar and Inchiri Provinces (8). Clinical samples from humans and animals with suspected RVF were positive for this virus.
These cases led to identification of 2 additional confirmed cases of acute RVF (positive for IgM against RVFV or RVFV RNA) in Adrar and Inchiei Provinces. Multidisciplinary investigations involving epidemiologists, virologists, entomologists, and veterinary teams in areas where the cases occurred were conducted in December 2010 as part of other investigations (8), describe the extent of the outbreak, and investigate possible RVF reemergence factors in Mauritania. We report results of laboratory and field investigations among humans, animals, and mosquitoes during the 2010 outbreak.
During October–December 2010, surveillance and investigation teams collected 80 clinical samples from 36 humans with suspected RVF and 44 of their contacts in Atar, Aoujeft, Akjoujt, Chingetti, Kobeni, and Tintane Moughatas (Figure 1). A human with a suspected case of RVF was defined as any patient with fever associated with or without hemorrhage, jaundice, or neurologic symptoms during October–December. A human contact was defined as a healthy person living within the immediate environment (i.e., same household or neighborhood) of a human or animal with a confirmed case of RVF. Serum samples from suspected case-patients were tested by using real time reverse transcription PCR, ELISA (for detection of IgM), and virus isolation.
Samples were obtained from animals living near suspected or confirmed case-patients, and a questionnaire about the species, sex, age and reproductive status of female animals was completed by their owners. Sampling of mosquitoes was conducted in December 2010 by using animal-baited traps placed in and around houses in which suspected and/or confirmed case-patients were identified. RVFV isolation and identification was performed on mosquitoes and human serum samples as described (9). Coding regions for RVFV nonstructural protein and glycoprotein 2 were amplified by using reverse transcription PCR and described sets of primers (10,11) and then purified after electrophoresis on agarose gels, and sequenced for phylogenetic analyses.
IgM against RVFV or viral RNA genome was detected in 30 (37.5%) of 80 patients, and 6 RVFV isolates were recovered (Table 1). The dates of symptom onset for confirmed cases of RVF in humans indicated that the outbreak probably started at the end of October, peaked in November, and decreased the second week of December. Among 30 patients (8 contacts and 22 suspected case-patients) with acute RVFV infections, the male: female ratio was 5:1 (25:5), and the median age was 35 years (range 17–70 years); 3 deaths were reported. Except for 1 man (a teacher), all infected men were herdsmen and all infected women were housewives.
For the animal investigation, serum samples were obtained and processed from 83 small ruminants (70 goats and 13 sheep) with a median age 4 years (range 1–10 years) from all localities tested (Table 2, Appendix). IgM against RVFV was detected in 23 (27.7%) of 83 animals. In addition, samples from 5 sick camels were collected in neighborhoods of persons with suspected and confirmed cases of RVF, and RVFV RNA was detected in 3 of these samples. Information for populations living in Adrar indicated that the first probable case of the disease among animals was in a sick camel in Aoujeft during the last week of October (8).
A total of 2,741 mosquitoes belonging to 5 genera and 11 species were collected for entomologic investigation. Culex antennatus was the most abundant mosquito species (83%), followed by Anopheles gambiae (9%) and An. rufipes (2%) mosquitoes (Table 3). Three RVFV strains were isolated from Cx. antennatus mosquitoes collected in Safia (Adrar Province).
Phylogenetic analysis based on RVFV partial small and medium RNA sequences showed a low level of variation between isolates from humans, animals, and mosquitoes. Isolates belonged to the West Africa lineage and were closely related to strains from Diawara (1998) and Hodh El Garbi (1998) in Mauritania and from Kenya (1965), Zimbabwe (1974), and Zambia (1975) (Figure 2).
After a 4-fold increase in rainfall in Mauritania from 2009 through 2010 (59 mm vs. 196 mm; (Aoujeft Weather Station). RVF clinical cases were confirmed in Adrar and Inchiri Provinces. Although RVF was reported in some provinces of Mauritania in 1987, 1998, and 2003 (5–7), cases in humans from Adrar and Inchiri Provinces have not been previously reported. However, in 2010 a total of 30 laboratory-confirmed human case-patients were recorded in these 2 provinces; 3 of the case-patients died. Both areas had a drought in recent years or their average rainfall was not >60 mm before 2010. The study showed animal abortion rates of 26.13% (23/88) and 30.68% (27/88) in 2 groups of small ruminants living near patients with recent RVFV infections. Three camels were infected with RVFV, and the cases were probably linked to human infections. The first human death from RVF was reported on November 11 in the village of Tawaz, in which a high mortality rates were observed in camel populations (11).
Serologic evidence of RVF in camels from northern Sudan and southern Egypt in 1977 (12) led to camels being suspected as key contributors in RVFV transmission (13). The involvement of camels in human infections could explain the high male:female ratio (25:5) for infections in humans because men are more involved in animal husbandry. In 2006, a similar sex difference for infection was observed in Kenya, where men had a prevalence rate of IgG against RVFV that was 3 times higher than that in women (14).
Entomologic investigations in Mauritania showed that only Cx. antennatus mosquitoes were infected with RVFV. Similar finding were reported for previous RVF outbreaks in Mauritania. Furthermore, Cx. antennatus mosquitoes were found to be infected with RVFV in Nigeria in 1967 and in Kenya during 1981–1984, and vector competence was demonstrated in laboratory studies (15). Phylogenetic analysis suggests reemergence of the local RVFV focus and emphasizes the need to strengthen RVF surveillance and other control measure in Mauritania after heavy rainfall.
Dr Ousmane Faye is a virologist and acarologist at the Arbovirus and Viral Hemorrhagic Fever Unit, Institut Pasteur, Dakar, Senegal. His primary research interests include the virology and vectorial transmission of arboviruses and viral hemorrhagic fevers.
Acknowledgments
We thank Magueye Ndiaye, Oumar Ndiaye, Carlos Fortez, Moussa Dia, Mireille Mondo, and Roughyetou Sylla providing for excellent technical assistance with laboratory and field investigations; and the authorities and the field agents of the Ministry of Health of Mauritania for facilitating investigation of this outbreak.
This study was supported by grants from the Institut Pasteur de Dakar, Senegal.
References
- Daubney R, Hudson JR, Garnham PC. Enzootic hepatitis or Rift Valley fever: an undescribed virus disease of sheep, cattle, and man from east Africa. J Pathol Bacteriol. 1931;34:545–79. DOIGoogle Scholar
- Murphy FA, Fauquet CM, Bishop DH, Ghabrial SA, Jarvis AW, Martelli GP, Family Bunyaviridae. In: Virus taxonomy. Classification and nomenclature of viruses. Sixth report of the International Committee on Taxonomy of Viruses. New York: Springer-Verlag; 1995. p. 300–15.
- Laughlin LW, Meegan JM, Strausbaugh LJ, Morens DM, Watten RH. Epidemic Rift Valley fever in Egypt: observations of the spectrum of human illness. Trans R Soc Trop Med Hyg. 1979;73:630–3. DOIPubMedGoogle Scholar
- Balkhy HH, Memish ZA. Rift Valley fever: an uninvited zoonosis in the Arabian Peninsula. Int J Antimicrob Agents. 2003;21:153–7. DOIPubMedGoogle Scholar
- Digoutte JP, Peters CJ. General aspects of the 1987 Rift Valley fever epidemic in Mauritania. Res Virol. 1989;140:27–30. DOIPubMedGoogle Scholar
- Nabeth P, Kane Y, Abdalahi MO, Diallo M, Ndiaye K, Ba K, Rift Valley fever outbreak in Mauritania in 1998: seroepidemiological, virological, entomological and zoological investigation. Emerg Infect Dis. 2001;7:1052–4. DOIPubMedGoogle Scholar
- Faye O, Diallo M, Diop D, Bezeid OE, Bâ H, Niang M, Rift Valley fever outbreak with East-Central African virus lineage in Mauritania, 2003. Emerg Infect Dis. 2007;13:1016–23. DOIPubMedGoogle Scholar
- El Mamy AB, Baba MO, Barry Y, Isselmou K, Dia ML, El Kory MO, Unexpected Rift Valley fever outbreak, northern Mauritania. Emerg Infect Dis. 2011;17:1894–6. DOIPubMedGoogle Scholar
- Digoutte JP, Calvo-Wilson MA, Mondo M, Traore-Lamizana M, Adam F. Continuous cell lines and immune ascite fluid pools in arbovirus detection. Res Virol. 1992;143:417–22. DOIPubMedGoogle Scholar
- Muller R, Saluzzo JF, Lopez N, Dreier T, Turell M, Smith J, Characterization of clone 13, a naturally attenuated avirulent isolate of Rift Valley fever virus, which is altered in the small segment. Am J Trop Med Hyg. 1995;53:405–11 .PubMedGoogle Scholar
- Takehara K, Min MK, Battles JK, Sugiyama K, Emery VC, Dalrymple JM, Identification of mutations in the M RNA of a candidate vaccine strain of Rift Valley fever virus. Virology. 1989;169:452–7. DOIPubMedGoogle Scholar
- Davies FG, Koros J, Mbugua H. Rift Valley fever in Kenya: the presence of antibodies to the virus in camels (Camelus dromedarius). J Hyg (Lond). 1985;94:241–4. DOIPubMedGoogle Scholar
- Eisa M, Obeid HMA, El Sawi AS. Rift Valley fever in the Sudan. I. Results of field investigations of the first epizootic in Kosti District, 1973. Bull Anim Health Prod Afr. 1977;24:343–7.
- LaBeaud AD, Muchiri EM, Ndzovu M, Mwanje MT, Muiruri S, Peters CJ, Interepidemic Rift Valley fever virus seropositivity, northeastern Kenya. Emerg Infect Dis. 2008;14:1240–6. DOIPubMedGoogle Scholar
- Linthicum KJ, Davies FG, Kairo A, Bailey CL. Rift Valley fever virus (family Bunyaviridae, genus Phlebovirus). Isolations from Diptera collected during an inter-epizootic period in Kenya. J Hyg (Lond). 1985;95:197–209 . DOIPubMedGoogle Scholar
Figures
Tables
Cite This ArticleTable of Contents – Volume 20, Number 2—February 2014
| EID Search Options |
|---|
|
|
|
|
|
|

Please use the form below to submit correspondence to the authors or contact them at the following address:
Amadou A. Sall, Unité des Arbovirus et Virus de Fièvre Hémorragique, Institut Pasteur, 36 Ave Pasteur, Boîte Postale 220, Dakar, SenegalAmadou A. Sall, Unité des Arbovirus et Virus de Fièvre Hémorragique, Institut Pasteur, 36 Ave Pasteur, Boîte Postale 220, Dakar, Senegal
Top