Volume 5, Number 4—August 1999
Dispatch
Cyclospora cayetanensis Among Expatriate and Indigenous Populations of West Java, Indonesia
Abstract
From January 1995 through July 1998, we investigated the occurrence of Cyclospora cayetanensis infection associated with gastrointestinal illness or diarrhea in foreign residents and natives of West Java, Indonesia. We found that C. cayetanensis was the main protozoal cause of gastrointestinal illness and diarrhea in adult foreign residents during the wet season. The parasite rarely caused illness in the indigenous population or in children.
Cyclospora cayetanensis is a newly recognized coccidian parasite associated with sudden onset of gastrointestinal illness and chronic diarrhea. In developing countries, cases occur sporadically, in a seasonal pattern, and primarily among western expatriates and travelers (1,2).
We recently reported multiple symptomatic cases of C. cayetanensis infection among European expatriates living in Jakarta, Indonesia; C. cayetanensis and Giardia lamblia were the intestinal parasites most frequently identified (6.4%) in cases of gastroenteritis or chronic diarrhea (3). We report here the results of a longitudinal evaluation of Cyclospora infection among expatriate populations of Jakarta and the results of two recent surveys of intestinal parasite infections in Indonesian children.
Three clinical diagnostic laboratories, each serving subpopulations of expatriate residents of Jakarta, Indonesia, participated in the longitudinal evaluation. The medical unit of the Embassy of the Federal Republic of Germany, a diagnostic center for an estimated 300 European expatriates, screened for ova and parasites in cases of gastrointestinal illness and diarrhea from January 1995 through July 1998. The Parasitology Department of the U.S. Naval Medical Research Unit No. 2 (NAMRU-2) provided diagnostic services for U.S. military staff and their families living in Jakarta during January 1996 to January 1998. The U.S. Embassy Medical Unit in Jakarta performed diagnostic parasitic tests for approximately 500 U.S. expatriate residents from January to December 1998.
All three laboratories performed wet-mount microscopy of fresh and formalin-ethyl acetate-concentrated feces stained with dilute iodine or merthiolate-iodine-formalin solution. All specimens were from persons with self-reported cases of gastrointestinal illness and diarrhea who sought medical attention. Confirmation of Cyclospora was based primarily on size and morphologic features relative to reference slides provided by J.H. Cross, Uniformed Service University of Health Sciences, Washington, D.C., and secondarily on acid-fast staining characteristics. The NAMRU-2 laboratory also routinely applied a modified, 22 mm x 40 mm Kato thick-smear technique to estimate parasite/ova density. Analyses were limited to autochthonous cases by evaluating patient histories and excluding those that were probably acquired outside Indonesia.
All 8- to 10-year-old Indonesian children attending 10 public schools in rural Sukaraja District, West Java, Indonesia, were examined for parasites and ova during December 1995. Direct wet-mount microscopy and modified Kato thick-smear examination of a fresh fecal specimen were performed. Two independent examinations were performed on each sample by clinical parasitologists. After informed parental consent, a subsample of 83 children was enrolled into a prospective study to monitor episodes of diarrhea following mebendazole de-worming. Stool samples were collected weekly or during gastrointestinal illness or diarrhea over 13 consecutive weeks of posttreatment observation (March to June 1996). Specimens were screened for parasites and ova as described above.
A hospital-based study to determine the causes of diarrhea among Indonesian residents of Jakarta was initiated in July 1997 as a collaborative study between the Departments of Microbiology and Parasitology, the Health Research Branch of the Indonesian Ministry of Health, and several participating Jakarta hospitals. A single stool sample was collected for testing from study participants who reported to the clinic with diarrhea lasting >72 hours. Preliminary analysis for parasitic causes associated with diarrhea was done in cases of children < 3 years old who were screened during the first 12 months (July 1997 to June 1998) of this 3-year study.
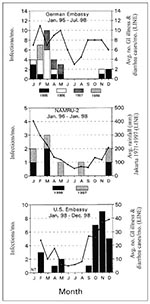
C. cayetanensis was the dominant pathogenic intestinal parasite, present in 29 (11.5%) of 253 cases of gastrointestinal illness and diarrhea among European expatriates who sought medical care during January 1995 to January 1998 (Table). C. cayetanensis was the most frequently identified pathogenic intestinal parasite each year, accounting for 8.6% to 15.1% of the annual diagnoses. All but one of these cases were in adults (30 years of age or older). Cases were clustered during the wet season (November– May), suggesting a seasonality of risk (Figure).
The second Jakarta-based laboratory that performed parasitologic screening on predominantly American families identified C. cayetanensis in 9 (9.1%) of 99 persons with gastrointestinal illness or diarrhea who sought care during a 24-month period. Cyclospora oocyst counts per gram of feces from these symptomatic C. cayetanensis cases were 100 to 327,600/gm; the highest counts were associated with early onset and acute symptoms. All nine C. cayetanensis cases were in adults.
The U.S. Embassy Health Unit in Jakarta identified 28 C. cayetanensis infections among 206 patients (13.6%) with gastrointestinal illness or diarrhea who were examined during an 11-month period in 1998. Pediatric infections, seen only in teenagers, accounted for 2 of the 28 cases. An apparent association was found between expatriates' risk for infection and the cooler wet season (October-May) (Figure).
A well population of 348 Indonesian schoolchildren was screened for intestinal parasite infections. The prevalence of intestinal helminth and protozoan infections among the children was 84% and 77%, respectively. Asymptomatic, low-density C. cayetanensis infections were found in 2 (0.6%) children.
A prospective study of 83 of these children was performed for 1,006 weeks of follow-up (average 12.2 weeks per child). Single or multiple samples of loose or watery stool (230 per 1,006 total samples) were collected from 71 of the 83 children. Although generally well and attending school, 26 (31.3%) of these 71 children had loose or watery stools at least four times during follow-up. Low-density C. cayetanensis infections were identified in two (2.4%) children, for an incidence of two infections per 19.3 person-years.
In the first year of the 3-year Jakarta diarrhea study, 263 Indonesians were screened for parasites; 170 (64.6%) of these were children younger than 3 years of age (ave. = 10.9 months, SD = 7.5 months). No Cyclospora infections were found.
The relatively sudden appearance, since 1995, of C. cayetanensis infections among long-term expatriate residents of Jakarta may indicate either a new ability of local diagnostic laboratories to recognize an established parasite or new establishment of this pathogen in the urban environment of Indonesia. Recent parasitologic surveys conducted throughout Indonesia may not have been undertaken with sufficient sensitivity to detect C. cayetanensis and may have been conducted during periods of low transmission.
The high frequency with which C. cayetanensis infections were found in expatriate patients cannot be attributed to new staining or concentration methods. Three laboratories applied direct wet-mount microscopy to identify this agent, and each laboratory independently classified C. cayetanensis as the dominant pathogenic parasite associated with diarrhea. Despite moderately enhanced recovery of C. cayetanensis oocysts by formalin-ethyl acetate sedimentation, virtually all diagnoses were made from the initial findings of the direct wet-mount or the modified Kato thick smear and were not dependent on the concentration step.
Cyclospora infections were identified in the cross-sectional prevalence survey and the prospective study of rural schoolchildren but not in the diarrhea specimens from Jakarta infants during the year-long study. Unlike the C. cayetanensis infections among foreign residents of Jakarta, infections by this parasite in rural Indonesian children were rare and characterized by low parasite density, absence of symptoms, and sporadic appearance.
These disparate findings suggest various possibilities: 1) The absence of Cyclospora infection in young children with diarrhea, both expatriate and native Indonesian, may result from their lack of exposure to foods or other risk factors to which older children and adults are exposed. Additionally, Indonesian infants may be protected by maternally acquired passive immunity. 2) Fecal contamination of food and water in rural Indonesia may be sufficiently high that local children, by the age of 8 to 10 years, have effective clinical and parasitologic immunity to Cyclospora and other pathogens. Infection of Indonesian children by other enteric pathogens may confer cross-protective immunity. 3) Urban transmission of Cyclospora may predominate among expatriate residents of Jakarta because of their atypical food preferences (imported, varied, fresh fruit and vegetables, restaurant-prepared) and preparations (prepared by servants, frequent use of raw garnish and salads).
The paucity of Cyclospora infections associated with loose stool or diarrhea in the rural and urban Indonesian children may not be atypical for these age groups. Among children of Bangkok (<5) who were screened for diarrheal causes during 1985 to 1986, Cryptosporidium was the only protozoon associated with illness (4). If Cyclospora was also present in this population but classified as Cryptosporidium spp., these organisms collectively accounted for only 1.8% of cases and 0.3% of controls.
Among nearly 900 Jakarta expatriates of all ages, we saw relatively few pediatric cases of Cyclospora and suspect that infections in this age group may also go undetected. Our methods may not have been sufficiently sensitive to detect mild infections of Cyclospora in highly susceptible young persons or in asymptomatic older persons who have been sensitized, even without prior exposure to C. cayetanensis, by repeated new contact and long-term maintenance of other commensal and pathogenic parasite infections.
Despite the likelihood that pathogenic bacterial and viral agents are the principal causes of gastrointestinal illness and diarrhea among native and expatriate residents of Indonesia (5,6), our results clearly identify C. cayetanensis as commonly associated with these health problems.
Dr. Fryauff heads the Parasitic Disease Program of the U.S. Navy Medical Research Unit No. 2 in Jakarta, Indonesia. His principal research interest is in malaria: drug trials for prevention and treatment, monitoring drug resistance, evaluating rapid diagnostics, and immunologic and epidemiologic studies.
Acknowledgments
The authors thank Aftab Ansari for critical review of the manuscript. They also thank Wolfgang Benkel, Regional Medical Officer of the German Embassy, Jakarta, Indonesia; Carol Francis, Registered Medical Technologist, American Embassy, Jakarta, Indonesia; and collaborating investigators of the Health Research Branch of the Indonesian Ministry of Health (LITBANGKES), Harapan Kita, Sumber Waras, and Persahabatan Public Hospitals of Jakarta, Indonesia, for their contributions. This work was conducted in accordance with U.S. Navy and Republic of Indonesia regulations governing the protection of human subjects in medical research.
Portions of this work were supported by U.S. Naval Medical Research and Development Command work unit number 623002A.
References
- Ortega YR, Sterling CR, Gilman RH, Cama VA, Diaz F. Cyclospora species—a new protozoan pathogen of humans. N Engl J Med. 1993;328:1308–12. DOIPubMedGoogle Scholar
- Mintz ED, Long EG. CLB: an emerging infectious cause of chronic diarrhea. CDC/NCID report. Infect Dis Clin Pract. 1994;3:315–20. DOIGoogle Scholar
- Fryauff DJ, Krippner R. Purnomo, Ewald C, Echeverria P. Case report of Cyclospora infection acquired in Indonesia and treated with cotrimoxazole. Am J Trop Med Hyg. 1996;55:584–5.PubMedGoogle Scholar
- Echeverria P, Taylor DN, Lexsomboon U, Bhaibulaya M, Blacklow NR, Tamura K, Case-control study of endemic diarrheal disease in Thai children. J Infect Dis. 1989;159:543–8.PubMedGoogle Scholar
- Subekti D, Lesmana M, Komalarini S, Tjaniadi P, Burr D, Pazzaglia G. Enterotoxigenic Escherichia coli and other causes of infectious pediatric diarrheas in Jakarta, Indonesia. SE Asian J Trop Med Pub Hlth. 1993;24:420–4.
- Richie E, Punjabi NH, Corwin A, Lesmana M, Rogayah I, Lebron C, Enterotoxigenic Escherichia coli diarrhea among young children in Jakarta, Indonesia. Am J Trop Med Hyg. 1997;57:85–90.PubMedGoogle Scholar
Figure
Table
Cite This ArticleTable of Contents – Volume 5, Number 4—August 1999
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
David J. Fryauff, U.S. NAMRU-2, Box 3, APO AP 96520-8132; fax: 62-21-424-4507
Top