Volume 7, Number 2—April 2001
THEME ISSUE
4th Decennial International Conference on Nosocomial and Healthcare-Associated Infections
State of the Art
Can Managed Health Care Help Manage Health-Care-Associated Infections?
Abstract
Managed-care organizations have a unique opportunity, still largely unrealized, to collaborate with health-care providers and epidemiologists to prevent health care-associated infections. Several attributes make these organizations logical collaborators for infection control programs: they have responsibility for defined populations of enrollees and for their overall health, including preventive care; they possess unique data resources about their members and their care; and they are able to make systemwide changes in care. Health-care associated infections merit the attention and effort of managed-care organizations because these infections are common, incur substantial illness and costs, and can be effectively prevented by using methods that are unevenly applied in different health-care settings. Both national and local discussions will be required to enable the most effective and efficient collaborations between managed care organizations and health-care epidemiologists. It will be important to articulate clear goals and standards that can be readily understood and widely adopted.
The term managed care connotes a commitment to improving the delivery of health care. Most of the U.S. population receives its health care through some form of managed care (1). Thus, managed- care organizations have an enormous potential to affect the incidence and management of infectious diseases in their patients. Health-care associated infections, which are common, serious, and costly adverse outcomes of medical care, have been identified by a recent Institute of Medicine Report as among the most pressing problems of medical care (2).
The potential for managed-care organizations to improve prevention and management of infections derives from four of their defining characteristics. Such organizations are responsible for defined populations in all health-care settings and for the overall health (including health promotion and disease prevention) of their members; they create and use detailed information about their members, their health status, and the medical care they received (although this information is usually not complete, it is typically more comprehensive than that available from other sources); and they are able to make systemwide changes in care, including disseminating guidelines, supporting interventions to improve outcomes, feeding back actual performance data to providers, and setting standards. In each of these respects, managed-care organizations resemble traditional public health agencies, which have played an important role in reducing health-care associated infections.
Managed care's population base and health system strengths, combined with its involvement in the delivery of care to specific persons, create the opportunity to use new capabilities and resources to address health-care associated infections. Since this opportunity is still largely unrealized, there are relatively few directly relevant examples. The following three, dealing with prevention of neonatal group B streptococcal infection, surveillance for tuberculosis (TB), and surveillance for postoperative infection, illustrate ways in which managed care can contribute to the prevention or control of serious infections. Although the first two examples are not health care-associated per se, health-care epidemiologists are often involved in hospitals' programs to prevent, identify, manage, and report them.
Examples of Managed-Care Organizations' Contributions to Prevention and Control of Infectious Diseases
Neonatal Group B Streptococcal Infection
Adoption of guidelines developed by the Centers for Disease Control and Prevention (CDC), the American Academy of Pediatrics, and the American College of Obstetrics and Gynecology has led to a profound reduction in the occurrence of early onset neonatal Group B streptococcal infection (3). These guidelines changed the recommended date for screening pregnant women for vaginal or rectal carriage of group B streptococcus to weeks 35 to 37 of pregnancy, instead of the second trimester. The guidelines also recommend initiating prophylaxis at least 4 hours before delivery. Although the impact of these and other aspects of the guidelines is evident (3), their implementation poses new challenges to the health-care system. For example, ensuring effective communication between the physician's office, the microbiology laboratory, and hospital is essential, since the 35-to 37-week screening cultures are usually performed in obstetricians' offices, while the culture results are needed promptly in the hospital to guide management before delivery. This and other challenges have meant that the guidelines are imperfectly implemented in some settings and that developing systems that monitor adherence to guidelines is difficult.
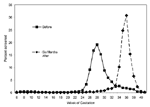
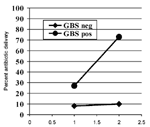
Group Health Cooperative of Puget Sound, working in collaboration with CDC, demonstrated the potential for rapid implementation of these guidelines (4). The managed-care organization's obstetricians and administrative staff created systems that facilitated a shift from their prior practice of performing screening cultures at the end of the second trimester of pregnancy to weeks 35 to 37 (Figure 1). Working in conjunction with hospital personnel, they created systems to speed communication of these culture results to the obstetrical services and made other changes in hospital procedures that led to a sharp increase in the proportion of culture-positive women who received antibiotics at least 4 hours before delivery, with no commensurate increase in antimicrobial-drug administration to women who were not colonized with group B streptococcus (Figure 2). This example shows the ability of a managed-care organization to enhance the dissemination of guidelines, improve coordination of care, and monitor adherence to guidelines. This form of coordination is most straightforward in staff model managed-care organizations, such as Group Health Cooperative, but other types of managed-care organizations can use some elements of this approach.
TB Surveillance and Management
A second example illustrates collaboration between managed- care organizations, clinicians, and public health agencies. Both providers and microbiology laboratories are required to report TB to departments of health. However, there is no effective mechanism to assess the completeness of clinicians' reporting of cases when no positive laboratory culture exists. In Massachusetts, a large managed-care organization examined its electronic diagnosis and treatment data, in conjunction with review of the medical records of patients with diagnoses or treatments consistent with TB. When data from the managed-care organization were compared with public health department records (5), 78% of cases were found by both, but the managed-care data revealed an additional 18% of reportable cases previously unknown to the public health department. Most of these cases had no positive culture, and therefore no laboratory-based reports had been generated.
Two additional notable findings emerged from this study. Although the managed-care organization had a rich array of data types available, pharmacy dispensing data alone proved to be the most useful information for identifying patients with active TB, almost all of whom were identifiable because they received at least two anti-TB drugs. Because these drugs are not often used for other purposes, it proved unnecessary to impose further conditions, such as requiring the drugs to be dispensed repeatedly or to be dispensed at the same time. In practice, the drugs were usually dispensed repeatedly and at the same time.
In addition, assessing the frequency and amount of dispensed drugs identified several persons who were poorly compliant with their treatment regimen, but who had not been recognized as such by their clinicians (6). If this result is confirmed in other settings, monitoring the dispensing of drugs for anti-TB therapy may become an important adjunct to TB surveillance and control programs. This investigation could only have been performed effectively in a managed-care setting, where access to diagnosis and treatment data and medical records existed. However, it produced a result that is applicable to other health-care settings in which there is only automated pharmacy data. In principle, this type of reporting could be performed by individual pharmacies or national pharmacy benefit management companies.
Surveillance for Surgical Site Infection
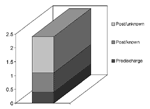
Collaboration between managed-care organizations and hospitals has provided convincing evidence that most surgical site infections are diagnosed after patients are discharged from the hospital, and many patients never return for care of the infection to the facility in which surgery was performed (Figure 3) (7). Further, this trend is increasing as patients are discharged on, or shortly after, the day of surgery. Because managed-care organizations have information on postoperative care delivered at all sites, including ambulatory settings and other hospitals, they can collaborate with hospitals that perform surgery on their members in conducting postdischarge surveillance that is otherwise difficult if not impossible to perform. Current work supported by CDC's Prevention Epicenters program is focused on developing methods to allow efficient use of computerized data to conduct ongoing surveillance, in conjunction with the hospitals in which surgery is performed (8). In a study of coronary artery bypass surgery performed at five hospitals, data from a managed-care organization identified twice as many surgical site infections as were identified by hospital-based surveillance (9). If this work is successfully extended, it should be possible to use existing automated data to enhance current surveillance capabilities, allowing uniform, objective surveillance for essentially all surgical procedures. This computer-based surveillance could supplement or in some cases replace existing hospital-based efforts that absorb considerable time and effort of skilled infection control professionals, resulting in a more complete and accurate monitoring system.
Successful collaborations require the identification of topics that both sides (the hospital-based health-care epidemiology community and managed-care organizations) agree are important. Therefore, the first step is to assign appropriate priority to health-care associated infections so that both parties can make informed decisions about the value of collaboration.
Setting Priorities
Managed-care organizations are accountable to the purchasers of their care. Usually these are employers, who fund services on behalf of their employees, or government agencies, who contract for services on behalf of Medicaid recipients, Medicare beneficiaries, or government employees. Managed-care organizations are also accountable to their members, and in some cases to accrediting agencies, such as the National Committee for Quality Assurance. Thus, managed-care organizations typically assign priorities on the basis of several considerations, including impact on members' health, members' preferences, cost and cost-effectiveness, society's preferences, and quality of care.
In assessing the impact of programs that address specific health problems, managed-care organizations consider a problem's burden of illness to their members, focusing on common, serious problems like asthma or osteoporosis. They also consider the strength of evidence that interventions can improve health outcome. An example is a standard, adopted by many managed-care organizations, for using beta-adrenergic blockers in survivors of myocardial infarction. This standard was adopted after it was appreciated that use of this relatively safe and simple treatment was not nearly as common as was appropriate, despite substantial clinical evidence of benefit.
Managed-care organizations also give priority to their members' preferences, even when they have no direct bearing on health outcomes or when clinical evidence is lacking. These organizations commit considerable resources to understanding issues that are important to their members and tracking their members' satisfaction. In addition to attending to members' perception of the quality of care they receive, managed-care organizations give priority to minimizing waiting time for appointments, the appearance of offices and inpatient facilities, and many other issues not directly related to health status.
Cost and cost-effectiveness are often important drivers of such organizations' decisions. These decisions are sometimes made from the purchaser's perspective, as in provision of pneumococcal immunizations for the elderly. At other times, decisions about cost-effectiveness are made from a societal perspective. Examples include smoking cessation or mammography screening programs, which typically yield their cost savings far enough in the future that the persons who avoid the adverse health outcomes are unlikely to still be members of the managed-care organization that paid for the care. In making these choices, managed-care organizations typically focus on the 25 conditions that account for nearly 80% of health-care costs (10).
Several dozen quality-of-care benchmarks are represented in managed-care organizations' accreditation standards (11). Examples include mandated performance with regard to childhood and adult immunization programs, cancer screening, diabetes care, substance abuse and mental health, and prenatal care.
Data Issues
Collaborations between managed-care organizations and the health-care epidemiology community are most likely to be successful when the managed-care organizations take advantage of their enrollment and demographic information, pharmacy dispensing data, and claims files. Such information is usually available in electronic databases and is used most often. Work with these data typically involves relatively small marginal costs, once the programs to create them are developed. In contrast, it is typically quite difficult for managed-care organizations to provide information from noncomputerized records, such as office records. Similarly, information on care that is delivered in hospitals or other organizations with which they contract for services may not be easily available unless these services generate an itemized bill for payment. For example, a managed-care organization would have information on intravenous antimicrobial-drug therapy delivered by a home-care company if the managed-care organization were charged for individual medications, but not for the same treatment if the charge for drugs were bundled into an overall medication administration fee.
Benefit to Managed-Care Organizations
Health-care associated infections merit the attention and effort of managed-care organizations according to the criteria noted above because these infections are common, they incur substantial illness and costs, and effective prevention methods exist but are currently unevenly applied in different health-care settings.
The Institute of Medicine Report highlighted postoperative infection as one of the most important categories of adverse events associated with medical care (2). One reason the burden of these infections is difficult to appreciate is that the impact of the adverse event is often "lost" in the overall outcome of the condition being treated. Thus, the fact that almost 20% of patients require > 9 days of antibiotic therapy because of confirmed or suspected infection after coronary artery surgery is not ordinarily a separately identified outcome of this procedure. However, the total cost of these infections in inpatients alone is estimated to be several billion dollars per year. Additionally, costs of infections that occur outside the hospital have not been adequately measured. Reductions in the occurrence of these infections could contribute to decreasing both illness and costs of care.
Evidence suggests that carefully implemented programs to prevent these infections are effective. Examples include reductions in bloodstream infections in intensive care units, postoperative surgical site infections, ventilator-associated pneumonias, and urinary tract infections. An additional reason that infection control programs merit the attention of managed- care organizations is that they are often the best organized and most effective quality improvement and error reduction programs in many hospitals. The National Nosocomial Infections Surveillance study has demonstrated how coordinated but decentralized systems can collect essential data about quality of care and make meaningful improvements in outcomes (12). Support of infection control programs in hospitals, nursing homes, and other facilities would create opportunities for managed-care organizations to engage more directly in the care provided by these facilities.
Benefit to Infection Control Programs
Managed care can contribute to infection control programs in several ways. It can help make infection control a priority for the entire health-care industry by jointly developing quality benchmarks with hospitals, nursing homes, and other components of the delivery system. The current interest in reducing medical errors can be an important foundation for such work. Managed care can use both its data and its ability to coordinate systemwide interventions to collaborate in research. Examples include better assessment of the epidemiology, risk factors, and consequences of health-care associated infections, as well as assessment of surveillance and prevention methods. Managed care can also have an impact through its considerable ability to bring about change in systems of care. The remarkable shift in the timing of group B streptococcus screening to a different stage of pregnancy in a single staff model managed-care organization demonstrates this potential. Managed care can play an important role in improving surveillance for these infections by contributing data about care delivered outside hospitals and integrating data across hospitals and other delivery sites. It can also assist in the implementation of infection control programs, especially in delivery sites such as physicians' offices, which currently have little organizational framework in which to develop or monitor such systems.
To take advantage of the potential benefits to patients, health-care epidemiologists need to strengthen the rationale for managed-care organizations to recognize the importance of health-care associated infections and the potential benefits of improved infection control programs. Most managed-care organizations, like other parts of the delivery system, are fully extended, so the addition of infection control priorities will require them either to displace an existing quality benchmark activity or to expand their roles, which will necessitate passing on new costs to their purchasers.
Both national and local discussions will be required to make the case for infection control collaborations. Nationally, the infection control parties best positioned to articulate overall themes and identify specific areas for collaboration are CDC, the Society of Healthcare Epidemiologists of America, and the Association for Professionals in Infection Control and Epidemiology (APIC). In the managed-care arena, the American Association of Health Plans, the Health Insurance Association of American, The Blue Cross Blue Shield Association, and the managed-care organizations with nationwide memberships are logical participants in these discussions. Other participants in these discussions should include accrediting agencies, such as the National Committee on Quality Assurance and the Joint Commission on Accreditation of Healthcare Organizations, and purchasers, such as the Washington Business Group On Health, the National Business Coalition on Health, and the Health Care Financing Administration. Local discussions between individual health-care facilities and the managed-care organizations with which they work will proceed more quickly within the context of a framework that emerges from national discussions.
Developing explicit technical standards for collecting and reporting infection surveillance data will also be important. This is necessary both to ensure that meaningful and interpretable information is collected and to allow the efficient development and dissemination of programs to perform the required work. This strategy has proved useful for other managed-care benchmarking activities, and it should be extended to the managed-care infection control arena. The actual work of creating technical standards is likely to require working groups with broad representation and deep technical expertise. Issues that need to be addressed include relatively straightforward ones of data availability, definitions, and reporting standards, plus some that will address new issues, such as the value of aggregating data across managed-care organizations and development of performance benchmarks.
Finally, it will be important to recognize that both parties to this discussion are evolving rapidly, as is health care itself. This means there will be a need for sustained engagement between managed care and health-care epidemiologists.
Dr. Platt is professor of ambulatory care and prevention at Harvard Medical School, hospital epidemiologist at Brigham and Women's Hospital, and director of research at Harvard Pilgrim Health Care, an HMO.
Dr. Caldwell is acting deputy director of the Division of Public Health Systems Development and Research, CDC. During the preparation of this manuscript, she was director of the Office of Health Care Partnerships, CDC.
Acknowledgment
The authors thank Robert Davis, who provided the information about implementation of Group B streptococcus guidelines at Group Health Cooperative of Puget Sound, and Julie L. Gerberding, for advice about the form and content of this manuscript.
References
- American Association of Health Plans. Enrollment, growth, accreditation. October 1999 http://www.aahp.org
- Committee on Quality of Health Care in America, Institute of Medicine. In: Kohn LT, Corrigan JM, Donaldson MS, editors. To err is human: building a safer health system. Washington: National Academy Press; 2000.
- Centers for Disease Control and Prevention. Prevention of perinatal group B streptococcal disease: a public health perspective. MMWR Morb Mortal Wkly Rep. 1996;45(No. RR-7).
- Davis RL, Hasselquist MB, Cardenas V, Zerr DM, Kramer J, Zavitkovsky A, Introduction of the new Centers for Disease Control Group B Streptococcal Prevention Guideline at a large west coast health maintenance organization. Am J Obstet Gynecol. 2001. In press. DOIPubMedGoogle Scholar
- Yokoe DS, Subramanyan GS, Nardell E, Sharnprapai S, McCray E, Platt R. Tuberculosis surveillance in a health maintenance organization using automated data. Emerg Infect Dis. 1999;5:779–87. DOIPubMedGoogle Scholar
- Subramanyan GS, Yokoe DS, Sharnprapai S, Nardell E, McCray E, Platt R. Assessing the management of tuberculosis using automated pharmacy records. Emerg Infect Dis. 1999;5:788–91. DOIPubMedGoogle Scholar
- Sands K, Vineyard G, Platt R. Surgical site infections occurring after hospital discharge: epidemiology and methods for detection. J Infect Dis. 1996;173:963–70. DOIPubMedGoogle Scholar
- Platt R, Yokoe DS, Sands K. Automated methods for surveillance of surgical site infection. Emerg Infect Dis. 2001;7. In press. DOIGoogle Scholar
- Sands K, Yokoe D, Hooper D, Tully J, Platt R. Multi-institutional comparison of surgical site infection surveillance by screening of administrative and pharmacy data. [Abstract #M35]. Society of Healthcare Epidemiologists, 1999 Annual meeting.
- Ray GT, Collin F, Lieu T, Fireman B, Colby CJ, Quesenberry CP, The cost of health conditions in a health maintenance organization. Med Care Res Rev. 2000;57:92–109. DOIPubMedGoogle Scholar
- National Committee for Quality Assurance. HEDIS 2000 List of Measures. Available at: URL: http://www.ncqa.org/pages/policy/hedis/h00meas.htm.
- Centers for Disease Control and Prevention. Monitoring hospital-acquired infections to promote patient safety--United States, 1990-1999. MMWR Morb Mortal Wkly Rep. 2000;49:149–53.PubMedGoogle Scholar
Figures
Cite This ArticleTable of Contents – Volume 7, Number 2—April 2001
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Richard Platt, 126 Brookline Ave., Suite 200, Boston, MA 02215, USA; fax: 617-859-8112
Top