Volume 16, Number 9—September 2010
Research
Pediatric Pneumococcal Serotypes in 4 European Countries
Abstract
After heptavalent pneumococcal conjugate vaccine (PCV7) was marketed in France, Spain, Belgium, and England and Wales (United Kingdom), invasive disease from non-PCV7 serotypes (NVT) increased. Adjusted serotype-specific incidences among children <15 years of age were compared between 1999–2002 (prevaccine) and 2005–2006 (postmarketing). Vaccine coverage increased to ≈32%–48% in France, Spain, and Belgium but remained <1% in England and Wales. Serotype 1 incidence rose in all age groups and countries (incidence rate ratio [IRR] 1.3–4.2; p<0.004), independently of PCV7 use, but incidence of serotypes 7F and 19A increased most in France, Spain, and Belgium (IRR 1.9–16.9 in children <5 years; p<0.001), where PCV7 coverage was greater. Vaccine-induced replacement of PCV7 serotypes possibly contributed to NVT increases, as did secular trends. New vaccines targeting these serotypes are available, but serotype dynamics needs further exploration that accounts for underreporting and prevaccine trends.
Streptococcus pneumoniae is a leading cause of meningitis and septicemia worldwide. More than 90 serotypes have been identified for S. pneumoniae, but serotype distribution differs by area and changes over time (1–3). The heptavalent pneumococcal conjugate vaccine (PCV7) targets the 7 serotypes—4, 6B, 9V, 14, 18C, 19F, and 23F—that most commonly caused pediatric invasive pneumococcal disease (IPD) in the United States. Widespread PCV7 use in the United States since 2000 led to rapid and dramatic decreases in vaccine serotypes and an overall decrease of IPD incidence (4).
In Europe, PCV7 was licensed for pediatric use in 2001 and marketed in Spain and France in 2001, England and Wales in 2002, and Belgium in 2004; the 7 serotypes accounted for 68%–77% of IPD cases in children <2 or <5 years of age (5–8). Vaccination policies from marketing to introduction of PCV7 into the universal vaccination schedule differed among countries. In Spain, Belgium, and France, vaccination aimed to reach a progressively increasing proportion of children <2 years of age, resulting in low but increasing vaccine coverage (36%–50% of young children in 2005–2006) because PCV7 was not free for all of them (6,7). In England and Wales, until late 2006 PCV7 was recommended only for medical risk groups, and population-level vaccine coverage was negligible. PCV7 was introduced in the national universal program and delivered free in France and England and Wales in 2006 and Belgium in 2007. In Spain, free universal vaccination was limited to the Madrid region beginning in 2006.
Several PCV7 postlicensure studies in the United States and European countries have described substantial increases in non-PCV7 vaccine serotypes (NVTs) (6,7,10–13). These findings raised concern that vaccine use could lead to replacement of PCV7 serotypes by NVTs, as occurred with pneumococcal carriage (14).
In Spain, Belgium, France, and England and Wales, NVT disease increased substantially between marketing and introduction of PCV7 into the universal schedule, when vaccine use was moderate in Spain, Belgium, and France and negligible in England and Wales. Considering that a 10-valent vaccine and a 13-valent conjugate vaccine are licensed in the European Union (EU), a better understanding of the dynamics of the additional serotypes is needed to help decision making on future vaccine strategies. This study describes and compares temporal trends of PCV7 serotypes and NVTs among children in 4 European countries, taking into account the levels of PCV7 use. We focused on the emergence of serotypes 1, 7F, and 19A because they were responsible for most of the NVT increase.
This population-based study is based on surveillance data collected prospectively by the national reference laboratories (NRLs) of Spain, Belgium, France, and England and Wales during July 1996–June 2006. (In the United Kingdom, Scotland and Northern Ireland were not included in this study because they use separate surveillance systems.) IPD isolates were referred by laboratories throughout each country to the NRL. IPD surveillance among children was enhanced in England and Wales, France, and Belgium starting in 1996, 2002, and 2005, respectively, by encouraging microbiologists to systematically refer pneumococcal isolates to the NRL for typing.
Definitions and Inclusion Criteria
We included all IPD cases, defined by isolation of S. pneumoniae from a normally sterile fluid in children <15 years of age and referred to the NRL of their country. One isolate per disease episode was used in the analysis. Serotypes targeted by PCV7 were grouped as vaccine types (PCV7 types). All other serotypes were considered NVTs. Meningitis was defined as isolation of S. pneumoniae in cerebrospinal fluid (CSF).
An epidemiologic year was July through June. A prevaccine period was defined as the 3 epidemiologic years during July 1999–June 2002. The postmarketing period was 2005–2006.
Microbiologic Testing
Serotype and antimicrobial susceptibility were determined by each NRL as described (9,15–17). In Spain, all strains of serogroups 6 and 19 were subjected to PCR serotype identification (18). In Belgium during 1996–2004 (before PCV7 marketing), 36% of isolates had the serogroup but not the serotype determined (17% for serogroup 19). However, all serogroup 19 isolates from children <2 years of age were typed, and during the postmarketing period, the serotype was determined for all isolates received. Isolates with missing serotype were assumed to follow the same serotype distribution as isolates from the same serogroup, by year and patient age group.
Isolates were considered susceptible, intermediate, or resistant to antimicrobial drugs according to Clinical and Laboratory Standards Institute criteria (penicillin intermediate and resistant, MIC 0.12–1.0 mg/L and MIC >1 mg/L, respectively; erythromycin resistant, MIC >0.5 mg/L) (19). England and Wales data on antimicrobial drug resistance were not available for this study.
Vaccine Coverage and Macrolide Use
Because studies estimating vaccine coverage used different methods among countries, we used vaccine doses to estimate a proxy of vaccine coverage. Data on monthly vaccine doses sold or distributed were provided by the PCV7 manufacturer (Wyeth, Brussels, Belgium; Madrid, Spain; Maidenhead, UK; and Paris, France) and by the Health Protection Agency for doses distributed by the UK Department of Health. Assuming that all doses were administered to children <2 years of age at an average of 3 doses per child (allowing for missed doses and catch-up schedules), we calculated the proportion of children <2 years of age who should have received an average of 3 PCV7 doses. We also calculated the number of vaccine doses distributed per 1,000 children <5 years of age for comparison with serotype-specific incidences in children <5 years of age.
We collected data on use of antimicrobial drugs from the European Surveillance of Antimicrobial Consumption (20). We compared these data with the serotype-specific incidence of antimicrobial drug–resistant isolates.
Data Analysis
For all incidence calculations, we adjusted numbers of cases to the rate of underreporting to the NRL to estimate total numbers of cases and control for surveillance enhancement over time. Underreporting rates were calculated by country, year, and age group by dividing the respective number of cases with an isolate typed at the NRL by the total number of laboratory-confirmed IPD cases estimated in the country. Total numbers of IPD cases were estimated by different methods: in Belgium and France, through periodic capture–recapture studies and correction for laboratory coverage (7,21); in England and Wales, by reconciliation of 2 large datasets (22); in Spain, by calculation of hospital underreporting rates as a proxy (23). Age-specific incidence rates were computed by dividing adjusted numbers of cases by the respective midperiod population of each country and age group, by using population figures from Eurostat for Spain and from the national institutes for statistics of Belgium, France, and England and Wales. For serotype-specific incidence calculations, cases with missing serotype data were accounted for by multiplying the overall incidence by the yearly proportions of serotype-specific disease in each age group (12).
Trends in incidence over time were tested for linear model by the t test, except for France because of missing data points; this model showed an overall better fit for the 3 studied serotypes. Correlation between vaccine doses per 1,000 children <5 years of age and serotype-specific incidence over years was tested by the Pearson correlation test, allowing for a 6-month lag between vaccine use and incidence. We also compared the annual average of serotype-specific incidence of the prevaccine period with the postmarketing period and computed incidence rate ratios (IRRs) and their exact 95% confidence intervals; p values were calculated by the Fisher exact test. We considered p values <0.05 significant. All statistical analyses were calculated by using STATA version 10.1 (StataCorp, College Station, TX, USA).
PCV7 Coverage
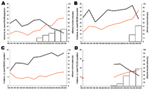
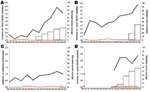
PCV7 use began in Spain in 2000–2001, France in 2001–2002, Belgium in 2004–2005, and England and Wales in 2005–2006 and increased gradually in the first 3 countries (Figure 1). In 2005–2006, the proportion of children <2 years of age who had received an average of 3 PCV7 doses was ≈33% in Spain, ≈48% in France, ≈42% in Belgium, and <1% in England and Wales.
Overall Incidence
During July 1996–June 2006, the NRLs of the 4 countries reported 13,584 IPD cases among children <15 years of age: 3,170 cases in Spain, 2,862 in Belgium, 2,188 in France, and 5,364 in England and Wales. Data were not available from France from 1997–98 through 2000–2001 because NRL activities stopped in 1997 and began again in 2001. The proportion of confirmed IPD cases typed at the NRLs increased during the study period because of improving reporting of each NRL (Table 1). IPD incidence per 100,000 children <15 years of age increased during the 10-year period in Spain, Belgium, and England and Wales from 14.0 to 18.5, 20.1 to 28.2, and 6.1 to 10.6, respectively, but remained fairly stable in France, ≈7.0.
Isolates from CSF represented 15% of invasive isolates in patients <15 years in Spain, 11% in Belgium, 16% in England and Wales, and 32% in France. Because blood isolates were underrepresented in France, NRL data were adjusted to the CSF/blood distribution reported by national epidemiologic surveillance, by year and age group (7). Only adjusted data are presented here.
PCV7-Type and NVT IPD Cases
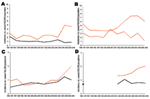
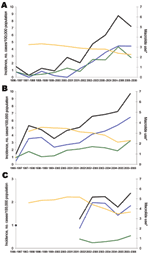
In children <5 years of age, incidence of PCV7-type disease started to decrease shortly after PCV7 introduction in Spain, Belgium, and France; the decrease was inversely related to increasing vaccine sales (Figure 1). Between the prevaccine period and the last study year (2005–2006), PCV7-type IPD significantly declined by 58%, 22%, and 52%, respectively, in these 3 countries (Table 2). In England and Wales, where vaccine sales were negligible, PCV7-type IPD increased by 25%, but the proportion of IPD caused by PCV7-type decreased slightly, from 75% to 70% (p = 0.004). In older children, PCV7-type IPD showed no clear trend, except in Belgium, where it significantly decreased (Figure 2; Table 3).
In contrast, incidences of NVT significantly increased in all 4 countries during the 10-year period (p<0.001), mainly from 2000–2002 onward (Figures 1, 2). From the prevaccine period to 2005–2006, NVT IPD increased significantly in both the <5-year and the 5–14-year age groups in all countries (Tables 2, 3). In each country, NVT IPD in the <5-year age group began to increase before PCV7 was introduced and gradually increased from year to year during 2002–2006. In children 5–14 years of age, NVT IPD fluctuated during the study period but mostly increased during 2002–2006. Serotypes 1, 7F, and 19A contributed most to this increase, representing 61% (range 57%–63%) of NVT IPD in children <15 years of age in 2005–2006. The dynamics of these 3 serotypes differed in terms of time trends and age groups affected.
Serotype 1
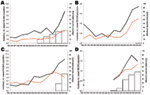
Serotype 1 disease increased significantly in each country during the 10-year period in both age groups (Figure 3). In children <5 years of age, the increase in serotype 1 began before PCV7 sales began. However, the largest increases occurred from 1999–2002 to 2005–2006, when incidence increased by 2–4-fold in both age groups in all countries (Tables 2, Table 3). Increases in the incidence of serotype 1 did not correlate significantly with PCV7 sales, except in France (Pearson r = 0.903, p = 0.036). In the 5–14-year age group, incidences were lower, but in 2005–2006, serotype 1 constituted in average 50% of IPD in that age group compared with 13% in children <5 years of age. All serotype 1 isolates were susceptible to penicillin. Incidence and proportion of erythromycin-resistant serotype 1 was low but increased in Belgium in 2004–2006.
Serotype 7F
Most (74%) serotype 7F cases occurred among children <5 years of age. In this group, IPD increased substantially in each country, mostly during 2004–2006, and correlated significantly with PCV7 sales, except in France (Pearson r = 0.901, p = 0.037 in Spain; r = 0.988, p = 0.002 in Belgium; r = 0.965, p = 0.008 in England and Wales; and r = 0.746, p = 0.148 in France) (Figure 4). From the prevaccine period to 2005–2006, incidence increased most in Spain and least in England and Wales (Table 2). In children 5–14 years of age, incidence rates also increased (Table 3), but numbers of cases were small. All serotype 7F isolates were susceptible to penicillin, and only 6/315 isolates in children <5 years of age were erythromycin resistant.
Serotype 19A
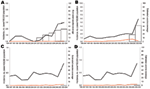
Serotype 19A disease affected predominantly children <5 years of age (94% of cases), for whom incidence rates more than doubled (IRR range 2.4–6.8) over the period (Figure 5). Incidence had already increased before PCV7 sales started in Belgium, Spain, and England and Wales, but the trend was significant only in Belgium (during 1996–2004). After PCV7 marketing, increases correlated significantly with vaccine sales in Spain and Belgium (Pearson r = 0.929 and 0.884, p = 0.022 and 0.047, respectively). From the prevaccine period to 2005–2006, 19A incidence significantly increased in Spain, France, and Belgium (Table 2); in England and Wales, the 27% increase was not significant. In children 5–14 years of age, numbers of cases were too small to identify any significant change.
Serotype 19A isolates showed high and increasing levels of antimicrobial drug resistance in Belgium, Spain, and particularly in France (data unavailable from England and Wales). In the <5-year age group, the prevalence of nonsusceptible strains ranged 0%–50% in 1996–1997 and increased in 2005–2006 to 21%, 48%, and 86% for penicillin and 67%, 61%, and 77% for macrolides in Belgium, Spain, and France, respectively. Full penicillin resistance was rare (0%–6% of isolates). Spain and Belgium shared similar patterns: incidence of penicillin-susceptible 19A increased more than resistant strains; incidence of erythromycin-resistant strains increased more than erythromycin-susceptible strains (Figure 6); in 1998–2006, the use of penicillin in ambulatory setting, calculated in defined daily doses per 1,000 inhabitants per day, increased slightly, and macrolide use declined by 31%–38%. In France, where nonsusceptible isolates predominated, use of penicillin and macrolides initially was much higher than that in the other countries but declined (–17% and –37%, respectively) until 2006. In England and Wales where use of antimicrobial drugs was initially lower, macrolide use became similar to Belgium and Spain from 2004 onward, but data on resistance were not available.
Evolution of Meningitis
Numbers of meningitis cases caused by individual serotypes were small, especially for serotype 1. In children <5 years of age, the incidence of meningitis from serotypes 19A and 7F combined also increased significantly in Spain, Belgium, and France from the prevaccine period to 2005–06 (IRR 3.8, 4.9 and 2.3, respectively, p<0.001); in England and Wales, it did not increase significantly (IRR 1.3, p = 0.283).
This study compared the dynamics of NVT disease in 4 countries before universal PCV7 vaccination. In Spain, Belgium and France, serotype 1, 7F and 19A incidence increased considerably under rising (though moderate) vaccine coverage. In England and Wales, where PCV7 use was negligible, serotype 1 disease increased substantially, 7F disease rose less than in the other countries, and 19A disease increased nonsignificantly. The proportion of IPD caused by serotype 19A remained stable in England and Wales, and the incidence of meningitis caused by 19A and 7F did not change significantly, suggesting that an increase in case detection caused part of the changes in 19A and 7F incidence. Indeed, a study showed that the 21% increase in IPD incidence in southwest England during 1996–2005 was no longer observed after adjustment for annual blood-culturing rates (24).
In Spain, the marked increase in NVT occurred concomitantly with PCV7 use, which led several studies to conclude that vaccine-induced replacement of serotypes had largely contributed to this increase (6,11). On the basis of our study findings, we suggest that vaccine use contributed to the increase in serotypes 7F and 19A. Both serotypes increased markedly under increasing PCV7 coverage and remained stable or increased less in the countries not using PCV7. Increases in 19A and 7F incidences correlated significantly with increasing vaccine sales in Spain and Belgium and were more pronounced in children <5 years of age, at whom PCV7 was aimed, than in older children. In Belgium and Spain, where both serotypes had already increased before PCV7 introduction, its slope escalated after PCV7 use. Although these data were observed under moderate PCV7 coverage, recent data from Belgium, England and Wales, and France indicate additional increases in the adjusted incidences of serotypes 7F and 19A under universal vaccination (2007–08) and high vaccine coverage (25–27).
However, we also suggest that vaccine-induced serotype replacement alone cannot explain the increase in NVT. First, serotype 1 rose well before PCV7 marketing in Belgium and Spain, affected predominantly older age groups, and increased in England and Wales in the absence of vaccine use. Second, serotype 19A increased in Belgium and Spain before PCV7 use. Similarly, serotype 7F or 19A disease also increased in countries not using PCV7 (28–30). Third, some EU countries with widespread PCV7 use did not experience similar rises (31,32).
Other factors most likely contributed to the increases. Cyclical trends of serotype 1 were described in Scandinavian countries before any PCV7 use (3,33,34). A wave of serotype 1 (and possibly 7F) may have occurred in these 4 neighboring countries. Conversely, the high use of antimicrobial drugs, especially macrolides, allegedly favored the increase of nonsusceptible serotype 19A (14,35). A modeling study suggested that use of antimicrobial drugs played a larger role than did PCV7 use in the increase of resistant 19A in the United States (36). In 3 countries in our study where 19A incidence (and resistant strains) increased, use of antimicrobial drugs was higher than in England and Wales where 19A stayed stable. However, incidence of penicillin- and erythromycin-susceptible 19A strains also increased in Spain and Belgium. Macrolide use decreased 37%–41% during 1998–2006 in the 3 countries, whereas 19A incidence increased 80%–253%. Similarly, serotype 19A incidence increased in England and Wales after universal PCV7 vaccination despite stable macrolide use (26). The role of antimicrobial drugs is thus difficult to delineate and suggests a synergistic effect of antimicrobial drugs and PCV7. Other factors for replacement have been raised (high prevalence of NVT carriage and low vaccine coverage), but they conflict with current knowledge (37): 7F is a rarely carried serotype, and 19A and 7F increased further under higher PCV7 coverage. These conflicting views suggest that factors leading to replacement disease are still not fully understood; its cause is probably multifactorial and population dependant.
Our study has several limitations. First, enhancement of pediatric IPD surveillance and possible changes in blood culture practices could not be completely controlled by our methods of adjusting for underreporting. This limitation certainly applied to England and Wales, where reconciliation of 2 datasets could not totally adjust for the increase in case reporting and blood culturing, which most likely contributed to the increased incidence in nearly all serotypes studied, probably leading to overestimation of the NVT increase in England and Wales. Increase in blood culturing over time in the other countries is not suggested by the sharp decrease in PCV7-type IPD, the similar trends in serotype-specific meningitis incidence (based on CSF isolation), and data on blood cultures in hospitals in Belgium (+13% from 1999–2002 to 2005–2006 while NVT IPD increased 210%). Second, missing serotype data (more frequent in the prevaccine period) may have led to imprecision in serotype distributions; however, similar age-specific PCV7-type and NVT distributions and trends were observed in other studies in Belgium, France, Spain, and England (5–8,24), PCV7 serotype coverage did not vary with the geographic origin of pneumococcal strains in France (7), and the age and sample distribution of children for whom serotype information was available did not differ from that of other children in the Belgium dataset. Finally, estimation of vaccine coverage assumed that all PCV7 doses were administered at an average schedule of 3 doses for children <2 years of age. This method may overestimate PCV7 coverage because a proportion of children are likely to be incompletely vaccinated given the high cost of PCV7 paid for by parents (38), but it may also underestimate coverage because many children received fewer doses in catch-up vaccination. However, coverage values were close to those estimated by population surveys (6,7,11,38).
Such an ecologic study cannot determine which rise in disease incidence is attributable to vaccine, secular trends, or use of antimicrobial drugs, and other possible factors may have contributed. However, the strength of this study is in the comparison of epidemiologic changes in 4 countries showing variations in serotype dynamics, vaccine use, and antimicrobial drug use.
The increase in incidence of serotypes 1, 7F, and 19A has partly countered the positive impact of PCV7 on overall IPD incidence in the first 2–5 years of nonuniversal vaccine use in Belgium, France, and Spain. The new 10-valent (1 and 7F) or 13-valent (1, 7F, and 19A) conjugate vaccines include these serotypes. However, a better understanding of serotype dynamics and contribution of vaccine and antimicrobial drug use is essential to guide decisions on the implementation of new vaccines and to assess their impact. Multicountry studies are useful for comparing serotype dynamics among population groups that have different levels of vaccine and antimicrobial drug use, but analyses should account for underreporting and prevaccine trends.
Dr Hanquet is a physician and epidemiologist. She was working for the Scientific Institute of Public Health in Belgium when this study was conducted and now works for the Belgian Health Care Agency and as a freelance epidemiologist. Her research interests include the epidemiology of vaccine-preventable diseases and the assessment of vaccination impact.
Acknowledgments
We thank William Hausdorff for his technical advice and critical reading of an early draft of the manuscript; Ron Dagan, Daniel Levy-Bruhl, Anne Vergison, and Herman van Oyen for their critical reading and useful suggestions on the last versions of this manuscript; Anne Perrocheau for her revision of an early draft of the manuscript; and David Prieto for his statistical advice. We are grateful to Dolores Vicioso, Isabel Hernández, Olga Robledo, Estelle Marchal, Sophie Grondin, Siobhan Martin, Sylvie Simon, J. Vandeven, and N. Verbiest for their technical assistance; and Pauline Weight for extraction of data for England and Wales.
Molecular typing of isolates in Spain was made possible by a grant from the “Fondo de Investigaciones Sanitarias” of the Spanish Government. GlaxoSmithKline paid travel costs for D.T., A.F., R.G., and E.V. to a meeting for data exchange. J.V. is advisor for a study on invasive pneumococcal disease among adults in Belgium, which is sponsored by Wyeth. E.V. received travel grants from GlaxoSmithKline, Sanofi-Aventis, Wyeth, and honoraria from Sanofi-Aventis. R.G. received travel grants from GlaxoSmithKline and Wyeth.
References
- Feikin DR, Klugman KP. Historical changes in pneumococcal serogroup distribution: implications for the era of pneumococcal conjugate vaccines. Clin Infect Dis. 2002;35:547–55. DOIPubMedGoogle Scholar
- Hausdorff WP, Siber G, Paradiso PR. Geographical differences in invasive pneumococcal disease rates and serotype frequency in young children. Lancet. 2001;357:950–2. DOIPubMedGoogle Scholar
- Henriques Normark B, Ortqvist A, Kalin M, Olsson-Liljequist B, Hedlund J, Svenson SB, Changes in serotype distribution may hamper efficacy of pneumococcal conjugate vaccines in children. Scand J Infect Dis. 2001;33:848–50.PubMedGoogle Scholar
- Whitney CG, Farley MM, Hadler J, Harrison LH, Bennett NM, Lynfield R, Active Bacterial Core Surveillance of the Emerging Infections Program Network. Decline in invasive pneumococcal disease after the introduction of protein-polysaccharide conjugate vaccine. N Engl J Med. 2003;348:1737–46. DOIPubMedGoogle Scholar
- Vergison A, Tuerlinckx D, Verhaegen J, Malfroot A; Belgian Invasive Pneumococcal Disease Study Group. Epidemiologic features of invasive pneumococcal disease in Belgian children: passive surveillance is not enough. Pediatrics. 2006;118:e801–9. DOIPubMedGoogle Scholar
- Muñoz-Almagro C, Jordan I, Gene A, Latorre C, Garcia-Garcia JJ, Pallares R. Emergence of invasive pneumococcal disease caused by nonvaccine serotypes in the era of 7-valent conjugate vaccine. Clin Infect Dis. 2008;46:174–82. DOIPubMedGoogle Scholar
- Lepoutre A, Varon E, Georges S, Gutmann L, Lévy-Bruhl D. Impact of infant pneumococcal vaccination on invasive pneumococcal diseases in France, 2001–2006. Euro Surveill. 2008;13:pii=18962.
- Farrell DJ, Felmingham D, Shackcloth J, Williams L, Maher K, Hope R, Non-susceptibility trends and serotype distributions among Streptococcus pneumoniae from community-acquired respiratory tract infections and from bacteraemias in the UK and Ireland, 1999 to 2007. J Antimicrob Chemother. 2008;62(Suppl 2):ii87–95. DOIPubMedGoogle Scholar
- Flamaing J, Verhaegen J, Vandeven J, Verbiest N, Peetermans WE. Pneumococcal bacteraemia in Belgium (1994–2004): the preconjugate vaccine era. J Antimicrob Chemother. 2008;61:143–9. DOIPubMedGoogle Scholar
- Dias R, Caniça M. Invasive pneumococcal disease in Portugal prior to and after the introduction of pneumococcal heptavalent conjugate vaccine. FEMS Immunol Med Microbiol. 2007;51:35–42. DOIPubMedGoogle Scholar
- Barricarte A, Castilla J, Gil-Setas A, Torroba L, Navarro-Alonso JA, Irisarri F, Effectiveness of the 7-valent pneumococcal conjugate vaccine: a population-based case-control study. Clin Infect Dis. 2007;44:1436–41. DOIPubMedGoogle Scholar
- Hicks LA, Harrison LH, Flannery B, Hadler JL, Schaffner W, Craig AS, Incidence of pneumococcal disease due to non-pneumococcal conjugate vaccine (PCV7) serotypes in the United States during the era of widespread PCV7 vaccination, 1998–2004. J Infect Dis. 2007;196:1346–54. DOIPubMedGoogle Scholar
- Singleton RJ, Hennessy TW, Bulkow LR, Hammitt LL, Zulz T, Hurlburt DA, Invasive pneumococcal disease caused by nonvaccine serotypes among Alaska Native children with high levels of 7-valent pneumococcal conjugate vaccine coverage. JAMA. 2007;297:1784–92. DOIPubMedGoogle Scholar
- Hanage WP. Serotype replacement in invasive pneumococcal disease: where do we go from here? J Infect Dis. 2007;196:1282–4. DOIPubMedGoogle Scholar
- Johnson AP, Waight P, Andrews N, Pebody P, George RC, Miller E. Pneumococcal meningitis, associated deaths and serotypes of causative pneumococci in England, 1998–2005. J Infect. 2007;55:394–9. DOIPubMedGoogle Scholar
- Cohen R, Levy C, de La Rocque F, Gelbert N, Wollner A, Fritzell B, Impact of pneumococcal conjugate vaccine and of reduction of antibiotic use on nasopharyngeal carriage of nonsusceptible pneumococci in children with acute otitis media. Pediatr Infect Dis J. 2006;25:1001–7. DOIPubMedGoogle Scholar
- Fenoll A, Jado I, Vicioso D, Casal J. Dot blot assay for the serotyping of pneumococci. J Clin Microbiol. 1997;35:764–6.PubMedGoogle Scholar
- Tarragó D, Fenoll A, Sánchez-Tatay D, Arroyo LA, Muñoz-Almagro C, Esteva C, Identification of pneumococcal serotypes from culture-negative clinical specimens by novel real-time PCR. Clin Microbiol Infect. 2008;14:828–34. DOIPubMedGoogle Scholar
- Clinical and Laboratory Standards Institute. Performance standards for antimicrobial susceptibility testing; 16th informational supplement. CLSI document M100–S16. Wayne (PA): The Institute; 2008.
- European Surveillance of Antimicrobial Consumption (ESAC). Antibiotic consumption; online interactive database [cited 2010 May 21]. http://www.esac.ua.ac.be/esac_service/applet/eidb.html
- Kissling E, Lernout T, Vergison A, an der Heiden M, Hanquet G. Capture–recapture analysis comparing two paediatric studies: do we need incentives? In: Abstract book of the 2008 European Scientific Conference on Applied Infectious Disease Epidemiology; Berlin, Germany; 2008 Nov 19–21. Stockholm (Sweden): European Centre for Disease Prevention and Control (ECDC); 2008. p. 227.
- Johnson AP, Potz N, Waight P, Gungabissoon U, Livermore DM, Pebody R, Susceptibility of pneumococci causing meningitis in England and Wales to first-line antimicrobial agents, 2001–2004. J Antimicrob Chemother. 2005;56:1181–2. DOIPubMedGoogle Scholar
- Fenoll A, Granizo JJ, Aguilar L, Giménez MJ, Aragoneses-Fenoll L, Hanquet G, Temporal trends of invasive Streptococcus pneumoniae serotypes and antimicrobial resistance patterns in Spain from 1979 to 2007. J Clin Microbiol. 2009;47:1012–20. DOIPubMedGoogle Scholar
- Ihekweazu CA, Dance DA, Pebody R, George RC, Smith MD, Waight P, Trends in incidence of pneumococcal disease before introduction of conjugate vaccine: south west England, 1996–2005. Epidemiol Infect. 2008;136:1096–102. DOIPubMedGoogle Scholar
- Verhaegen J, Vandeven J, Verbiest N, Lagrou K, Kissling E, Hanquet G. Dynamic changes of pneumococcal serotypes after introduction of PCV7 in Belgium [abstract G1–1531]. 49th Interscience Conference on Antimicrobial Agents and Chemotherapy, San Francisco, CA, September 12–15, 2009.Washington: American Society for Microbiology; 2009.
- Kaye P, Malkani R, Martin S, Slack M, Trotter C, Jit M, Invasive pneumococcal disease (IPD) in England & Wales after 7-valent conjugate vaccine (PCV7); potential impact of 10 and 13-valent vaccines. Poster presented at the 27th Annual Meeting of the European Society for Paediatric Infectious Disease, Brussels, 9–13 June 2009. Pediatr Infect Dis J. 2009;28:e133–4.
- Varon E, Janoir C, Gutmann L; National Reference Centre for Pneumococci. (France). Activity report 2008. Epidemiology 2007 [in French] 2008 [cited 2010 Mar 27]. http://www.invs.sante.fr/surveillance/cnr/rapports_pneumocoques2008.pdf
- Choi EH, Kim SH, Eun BW, Kim SJ, Kim NH, Lee J, Streptococcus pneumoniae serotype 19A in children, South Korea. Emerg Infect Dis. 2008;14:275–81. DOIPubMedGoogle Scholar
- Dagan R, Givon-Lavi N, Leibovitz E, Greenberg D, Porat N. Introduction and proliferation of multidrug-resistant Streptococcus pneumoniae serotype 19A clones that cause acute otitis media in an unvaccinated population. J Infect Dis. 2009;199:776–85. DOIPubMedGoogle Scholar
- Rückinger S, von Kries R, Reinert RR, van der Linden M, Siedler A. Childhood invasive pneumococcal disease in Germany between 1997 and 2003: variability in incidence and serotype distribution in absence of general pneumococcal conjugate vaccination. Vaccine. 2008;26:3984–6. DOIPubMedGoogle Scholar
- Vestrheim DF, Løvoll O, Aaberge IS, Caugant DA, Høiby EA, Bakke H, Effectiveness of a 2+1 dose schedule pneumococcal conjugate vaccination programme on invasive pneumococcal disease among children in Norway. Vaccine. 2008;26:3277–81. DOIPubMedGoogle Scholar
- Rückinger S, van der Linden M, Reinert RR, von Kries R, Burckhardt F, Siedler A. Reduction in the incidence of invasive pneumococcal disease after general vaccination with 7-valent pneumococcal conjugate vaccine in Germany. Vaccine. 2009;27:4136–41. DOIPubMedGoogle Scholar
- Henriques Normark B, Kalin M, Ortqvist A, Akerlund T, Liljequist BO, Hedlund J, Dynamics of penicillin-susceptible clones in invasive pneumococcal disease. J Infect Dis. 2001;184:861–9. DOIPubMedGoogle Scholar
- Konradsen HB, Kaltoft MS. Invasive pneumococcal infections in Denmark from 1995 to 1999: epidemiology, serotypes, and resistance. Clin Diagn Lab Immunol. 2002;9:358–65. PubMedGoogle Scholar
- Dagan R. Serotype replacement in perspective. Vaccine. 2009;27(Suppl 3):C22–4. DOIPubMedGoogle Scholar
- Van Effelterre T, Moore MR, Fierens F, Whitney CG, White L, Pelton SI, A dynamic model of pneumococcal infection in the United States: implications for prevention through vaccination. Vaccine. 2010;28:3650–60. DOIPubMedGoogle Scholar
- Hanage WP. Serotype-specific problems associated with pneumococcal conjugate vaccination. Future Microbiol. 2008;3:23–30. DOIPubMedGoogle Scholar
- Robert E, Swennen B. Vaccine coverage survey in children aged 18–24 months in French community in 2006 [in French]. PROVAC, School of Public Health ULB, Brussels 2007.
Figures
Tables
Cite This Article1Current affiliation: Belgian Healthcare Agency, Brussels, Belgium.
Table of Contents – Volume 16, Number 9—September 2010
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Germaine Hanquet, Avenue de Jette, 64, B-1081 Brussels, Belgium
Top