Volume 17, Number 3—March 2011
Dispatch
Increasing Drug Resistance in Extensively Drug-Resistant Tuberculosis, South Africa
Figure 1
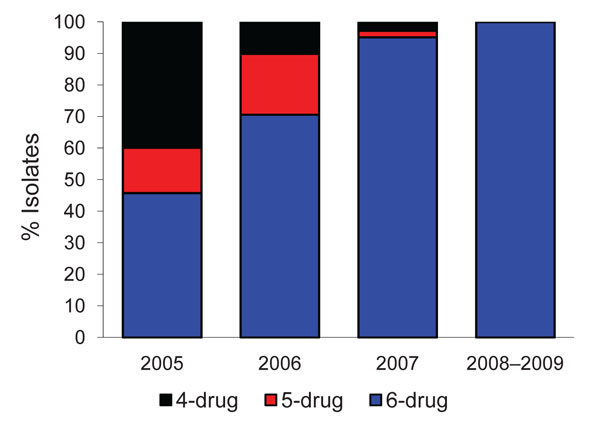
Figure 1. Drug resistance among extensively drug-resistant tuberculosis isolates from Tugela Ferry, South Africa, 2005–2009: 4-drug resistance = isoniazid (INH), rifampin (RIF), ofloxacin (OFL), and kanamycin (KM); 5-drug resistance = INH, RIF, OFL, KM, and ethambutol (EMB) or streptomycin (SM); 6-drug resistance = INH, RIF, OFL, KM, EMB, and SM. Column for 2008–2009 indicates study population.
Page created: July 25, 2011
Page updated: July 25, 2011
Page reviewed: July 25, 2011
The conclusions, findings, and opinions expressed by authors contributing to this journal do not necessarily reflect the official position of the U.S. Department of Health and Human Services, the Public Health Service, the Centers for Disease Control and Prevention, or the authors' affiliated institutions. Use of trade names is for identification only and does not imply endorsement by any of the groups named above.