Volume 18, Number 9—September 2012
Dispatch
Antimicrobial Drug Use and Macrolide-Resistant Streptococcus pyogenes, Belgium
Figure 1
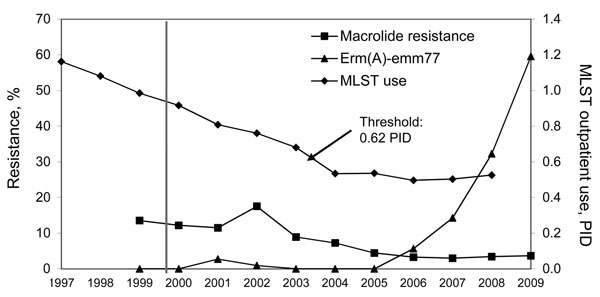
Figure 1. . Prevalence of macrolide-resistant Streptococcus pyogenes and proportions of the erm(A)-emm77 geno-emm-type among macrolide-resistant strains during 1999–2009, and macrolides, lincosamides, streptogramins B, and tetracycline (MLST) use data expressed in packages/1,000 inhabitants/day (PID) during 1997–2007 in Belgium. Threshold indicates the critical level of macrolide, lincosamide, streptogramins B, and tetracycline use below which low-level macrolide-resistant S. pyogenes and selection of an inducible resistance mechanism with a lower fitness cost might be facilitated. Dotted line indicates start of the public health campaigns to reduce antimicrobial drug prescribing. The sharp increase in macrolide resistance in 2002 was linked to a local clonal outbreak of mef(A)-emm1 harboring S. pyogenes.