Volume 17, Number 7—July 2011
Letter
Aircraft and Risk of Importing a New Vector of Visceral Leishmaniasis
Cite This Article
Citation for Media
To the Editor: Kala-azar, or visceral leishmaniasis, is a parasitic disease that leads to fever, anemia, and hepatosplenomegaly. Death is the usual outcome when infection is not treated. The majority of infections are caused by the protozoan Leishmania donovani, restricted to India and eastern Africa, but the most widespread are caused by L. infantum, found from People’s Republic of China to the New World, where it infects humans, dogs, and wild canids. All Mediterranean countries are affected by L. infantum, where most patients are co-infected with HIV. Several species of sand flies transmit the disease (1).
During the 1980s, urban transmission of kala-azar became a major problem in Brazil. More than 3,000 cases are reported annually, and the disease has spread from northeastern Brazil westward to the Amazon region, as well as to the industrialized southeast. Several as yet unproven explanations for the urbanization of kala-azar in Brazil have been proposed (2), but whatever the reason, it is associated with proliferation of Lutzomyia longipalpis sand flies, which, in turn, are strongly associated with human environments. The vector can easily spread by entering buses or trains looking for food at night or for hiding places at dawn. Invasion of new areas by sand flies through transportation of ornamental plants has been observed (R. Brazil, pers. comm.), possibly by insect eggs or larvae being carried in organic matter.
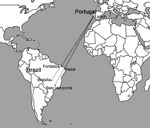
Kala-azar has now reached the temperate Brazilian south and Argentina. This spread of the disease warns us of the danger of introduction in other temperate areas. Europe is particularly vulnerable because of the existing natural transmission of L. infantum. This risk is increased by recently created daily direct flights to Lisbon from Fortaleza, Natal, Brasília, and Belo Horizonte (Figure), Brazilian cities where epidemics of the disease have occurred. Lisbon is suitable to canine infection, and >10% of dogs may be infected (3). The climate is a barrier for the introduction of many vectors outside their normal range, such as Anopheles gambiae mosquitoes in temperate zones (4,5), but the threshold of change for L. longipalpis sand flies is minimal. The Mediterranean area is as dry as northeastern Brazil, where the disease is now highly endemic. Furthermore, the annual average temperature and cooler months in Lisbon (at 38°44′N) are only 3–4°C lower than those of São Borja, Rio Grande do Sul state, the southernmost city where L. longipalpis transmits kala-azar, and even warmer than Chajarí, Argentina (at 30°46′S, ≈500 km from Buenos Aires and only 8° farther from a pole than Lisbon), at the highest southern latitude where this vector is found (6).
Human kala-azar is less common in Europe, possibly because sand flies there are less anthropophilic. If aircraft introduce anthropophilic L. longipalpis sand flies in Lisbon, the situation could change dramatically, and kala-azar might become a major urban disease in Europe. The International Health Regulations recommends disinfection of aircraft by preflight and blocks-away spraying with pyrethroids (7). However, significantly reduced susceptibility to pyrethroids in wild populations of L. longipalpis sand flies was recently described in Brazil (8). Centuries after its introduction to South America by Iberian colonizers, kala-azar may make its way back to Europe with a more forceful vector—this time by air, not by sea. To reduce this risk, much information needs to be known about the biology of L. longipalpis sand flies, such as minimum temperature tolerance, mechanisms of urban spread, presence in aircraft, and role in inducing more severe disease.
References
- Costa CH. Characterization and speculations on the urbanization of visceral leishmaniasis in Brazil. Cad Saude Publica. 2008;24:2959–63. DOIPubMedGoogle Scholar
- Abranches P, Silva-Pereira CD, Conceição-Silva FM, Santos-Gomes GM, Janz JG. Canine leishmaniasis: pathological and ecological factors influencing transmission of infection. J Parasitol. 1991;77:557–61. DOIPubMedGoogle Scholar
- Gratz NG, Steffen R, Cocksedge W. Why aircraft disinfection? Bull World Health Organ. 2000;78:995–1004.PubMedGoogle Scholar
- Tatem AJ, Rogers DJ, Hay SI. Estimating the malaria risk of African mosquito movement by air travel. Malar J. 2006;5:57–63. DOIPubMedGoogle Scholar
- Salomón OD, Fernández MS, Santini MS, Saavedra S, Montiel N, Ramos MA, Distribución de Lutzomyia longipalpis en la Mesopotamia Argentina, 2010. Medicina (B Aires). 2011;71:22–6.PubMedGoogle Scholar
- Hardiman M, Wilder-Smith A. The revised international health regulations and their relevance to travel medicine. J Travel Med. 2007;14:141–4. DOIPubMedGoogle Scholar
- Alexander B, Barros VC, de Souza SF, Barros SS, Teodoro LP, Soares ZR, Susceptibility to chemical insecticides of two Brazilian populations of the visceral leishmaniasis vector Lutzomyia longipalpis (Diptera: Psychodidae). Trop Med Int Health. 2009;14:1272–7. DOIPubMedGoogle Scholar
Figure
Cite This ArticleRelated Links
Table of Contents – Volume 17, Number 7—July 2011
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Carlos H.N. Costa, Federal University of Piaui–Institute of Tropical Diseases Natan Portella, Rua Artur de Vasconcelos 151-Sul, Teresina PI 64049-750, Brazil
Top