Volume 18, Number 6—June 2012
Research
Community Survey after Rabies Outbreaks, Flagstaff, Arizona, USA
Cite This Article
Citation for Media
Abstract
Flagstaff, Arizona, USA, experienced notable outbreaks of rabies caused by a bat rabies virus variant in carnivore species in 2001, 2004, 2005, 2008, and 2009. The most recent epizootic involved transmission among skunk and fox populations and human exposures. Multiple, wide-ranging control efforts and health communications outreach were instituted in 2009, including a household survey given to community members. Although the Flagstaff community is knowledgeable about rabies and the ongoing outbreaks in general, gaps in knowledge about routes of exposure and potential hosts remain. Future educational efforts should include messages on the dangers of animal translocation and a focus on veterinarians and physicians as valuable sources for outreach. These results will be useful to communities experiencing rabies outbreaks as well as those at current risk.
More than 90% of rabies cases in the United States are in wild animals. Most reported cases of rabies occur among carnivores, including raccoons, skunks, and foxes, in addition to many bat species. Despite the elimination of canine rabies virus variants in the United States, domestic animals, including cats and dogs, are infected each year from exposures to rabid wildlife. In addition, ≈2–4 human rabies cases are reported each year in the United States (1), and exposure to rabid animals or animals suspected of being rabid is common, with ≈35,000–38,000 persons receiving rabies postexposure prophylaxis (PEP) each year (1,2). One of the primary methods for rabies prevention and control is practical and accurate public health information. Recognition of the signs and severity of rabies, exposure routes, behavioral and environmental risk factors, and appropriate domestic animal welfare are critical messages for disease prevention and require appropriate public education for persons of all ages (3,4).
Rabies virus is generally transmitted among members of the same species, and specific rabies virus variants are associated geographically with independent reservoir species. Spillover of rabies virus variants from 1 species to another occurs, but sustained transmission of such variants in nonreservoir species is rare (4). The area around Flagstaff, Arizona (Coconino County), USA, was free of sustained rabies virus transmission until 2001, when a spillover of a bat rabies virus variant was followed by a suspected host shift, with increased transmission in striped skunk (Mephitis mephitis) populations (5). Control measures were launched to halt rabies spread in skunks and limit the potential for human exposures (6). These efforts appeared to control rabies spread in skunk populations until 2004, when 5 striped skunks and 1 gray fox (Urocyon cinereorgenteus) were diagnosed as rabid, and rabies was confirmed in an additional striped skunk, a gray fox, and a feral cat (Felis catus) in 2005 (5). Rabies was quiescent after this resurgence in 2004/2005 until fall 2008 when the disease was confirmed in several gray foxes and striped skunks (4). The establishment of rabies in fox populations was troubling because the extensive home range of foxes threatened its containment in the Flagstaff area. Given the size of this epizootic, the potential for spread to other areas, and several notable human exposures, a large, interagency effort was launched to control the resurgence of rabies in Flagstaff.
In October 2009, a survey was distributed to Flagstaff households in an area where rabid animals had been captured in 2008 and 2009. This area also had a history of rabies epizootics since 2001 (5,6). Attitudes and practices regarding management of exposure to domestic and wild animals are essential to define in areas where persons and their pets may have an increased chance of coming into contact with a rabid animal. An assessment of community knowledge of rabies and interactions with animal reservoirs can help target educational messages during seasonal disease peaks or at the beginning of an epizootic. We present an update on the most recent outbreak and the results of a community survey in Flagstaff.
Data Sources and Survey Design
Surveillance data for Coconino County of the numbers of rabid animals identified during 2000–2009, were obtained from the Arizona Department of Health Services. Emergency department admission data, in which the chief complaint included animal bites during 2005–2009, were obtained from the infection control office for the Flagstaff Medical Center.
Addresses of all households in the quarantine area of Flagstaff were provided by the Coconino County Public Health Services District. Occupancy status of the households was not available, and names associated with each address were permanently removed and not shared for the mailings. In October 2009, surveys were mailed to all households, and 1 adult from each household was asked to complete the survey. Respondents could complete the survey online or by an included paper-based form and returned in a prepaid envelope by mail. The surveys were anonymous and were not linked to a name or address. Educational material on rabies was not included, but for more information, respondents could request printed materials on a separate request form and were directed to the rabies website of the Centers for Disease Control and Prevention (CDC) (Atlanta, GA, USA) (7). The community survey was determined to be public health nonresearch by CDC. The survey elicited information from respondents on knowledge of rabies, the Flagstaff rabies outbreak, practices regarding domestic and wild animals, and adherance to quarantine restrictions. Survey questions are included in Table A1.
Data Analysis
A general definition of “knowledge of rabies” was defined as the answer of “yes” when the respondent correctly identified that bites, scratches, and saliva were modes of rabies virus transmission and also identified 1 other incorrect mode of transmissions as a mode of transmission or did not identify any incorrect mode of transmission. A more specific definition of “knowledge of rabies in Flagstaff” was defined as “yes” if the respondent knew about the outbreak in Flagstaff and knew the 3 main animals which had rabies in Flagstaff (bat, skunk, and fox).
Univariate and multivariate analyses were conducted for 4 separate resident subpopulations to further characterize the groups. The outcomes of interest were 1) knowledge of rabies in Flagstaff, 2) pet owners, 3) dog owners, and 4) translocators (persons who trapped and moved wild animals on their property). Odds ratios with 95% CIs for individual characteristics were calculated by using logistic regression. Characteristics that were considered associated (p<0.1) with each outcome in the univariate analysis were further assessed through multivariate logistic regression models (8).
Update on Rabies Epizootic
After a period of quiescence from 2005, another rabies epizootic occurred in Flagstaff during 2008 (Figure 1, panel A). Seven rabid animals were reported in Coconino County, including 2 foxes and 2 skunks (Table 1). No human exposures to rabid animals were reported in 2008, but several companion animal exposures occurred, including 6 cats exposed to rabid bats, 2 dogs exposed to rabid skunks, and 1 dog exposed to a rabid fox. In 2009, Coconino County reported 35 rabid animals. All rabies viruses typed from the immediate Flagstaff area (from 14 foxes and 1 ringtail cat) were identified as a bat rabies virus variant. Two human exposures to rabid animals were identified in 2009: one person had been bitten by a rabid fox and the other person had been bitten by a rabid skunk. Also, 3 companion dog exposures to rabid foxes were reported. A review of Emergency Department discharge data at Flagstaff Medical Center specified a total of 88 animal bite–related admissions during 2005–2009. In 2009, 25 animal bite–related admissions were recorded, and 12 (48%) persons received PEP.
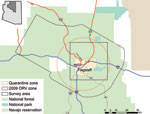
The number of rabid animals and control measures that were initiated in Coconino County in 2009 are shown in Figure 1, panel B. During July 21–24, the US Department of Agriculture, Animal and Plant Health Inspection Service, Wildlife Services, distributed 140,000 oral rabies vaccination (ORV) baits containing a vaccinia–rabies glycoprotein vaccine (Merial, Duluth, GA, USA) by air and ground over a 191-km2 area in Coconino County, targeting gray foxes (Figure 2). The vaccinia–rabies glycoprotein vaccine is not effective for vaccinating skunks against rabies (9). A 6-week trap, vaccinate, release campaign targeting skunks was initiated in the eastern portion of Flagstaff at the end of July. Additional control initiatives included prohibiting relocation of nuisance wildlife, comprehensive public education on rabies, rabies vaccine clinics for pets, a leash policy for pets on trails, and quarantine. The quarantine was established from April 7 through September 13, 2009, for a 15-mile-radius area centered on Flagstaff and later expanded to the entire ORV zone. The following measures were mandatory: do not disrupt ORV baits, do not feed wild animals, enclose compost bins and piles, do not leave pet food outside after sundown, confine cats and dogs to an enclosure on the owner’s property, keep pets on a leash when off of the owner’s property, and maintain current rabies vaccination for cats and dogs.
Demographic and Rabies-related Characteristics of Household Respondents
A total of 3,141 surveys were mailed, but 172 were returned because of an incorrect address or no occupancy of household, and 1,058 were completed and returned (35.6%); 1,039 written and 19 website-based. Most respondents had lived in Flagstaff for ≥10 years (74%), lived in Flagstaff year round (98%), were ≥51 years of age (68%), female (59%), and had at least a college degree (75%). A summary of responses is shown in Table A1.
Most respondents recognized that rabies virus can be transmitted to humans from infected animals through a bite (97%), scratch (73%), or contact with saliva (74%). More than half of respondents thought rabies virus can be transmitted by contact with blood, almost a quarter by contact with an infected animal’s urine or feces, and 13% identified skunk spray as infectious. Most residents were aware that skunks and foxes in Flagstaff may have rabies (89% and 73%, respectively), but only 52% were aware that bats in Flagstaff had rabies. Information about the current outbreak was ascertained by many methods, with newspapers or magazines being the most frequently cited source (78%).
Most (70%) respondents reported that if they were bitten or scratched by a domestic animal they would wash the wound with soap and water and likely seek medical care. More persons indicated they would seek medical care if they had an encounter with a wild (90%) animal than with a domestic (72%) animal. Most respondents indicated they would call one of 3 public agencies (city animal control, county health department, fish and game department) if they saw a sick animal than if they were bitten or scratched by an animal. Sixty residents (6%) reported seeing a sick wild animal on their property in the last 6 months. Of those that specified the type of animal, 21 persons (38%) reported a sick skunk, 20 (36%) a sick fox, and 1 (2%) a sick bat; 38% of responses were listed as “other.” Thirty-six percent of the residents reported doing nothing after seeing the ill animal, while 36% called animal control, and 17% called the county health department.
Seventy-three respondents (7%) reported that they would trap and translocate a nuisance animal themselves. Ninety-five persons (9%) have personally relocated a wild nuisance animal that was on their property. Furthermore, 57% translocated the animals >5 miles from their property. Skunks were the most frequent animal to be translocated (56%).
Eighty-four percent of respondents were aware of the rabies quarantine, and 82% of those stated that they complied with quarantine restrictions. Twelve percent of respondents did not believe the requirement to keep pets on a leash at all times would help prevent rabies exposures.
One half of all households owned dogs, and 29% of all households owned cats (Table 2). The overall proportion of dogs vaccinated was 96%. A higher proportion of outdoor cats (90%) was vaccinated than were indoor (76%) or indoor/outdoor (84%), and the overall reported proportion of cats vaccinated was 81%.
Rabies Knowledge in Flagstaff, Pet Ownership, Dog Ownership, and Translocation
Persons who had knowledge of rabies in Flagstaff were more likely to have knowledge of other aspects regarding rabies (Table A2), including the quarantine and concern about rabies in Flagstaff; these characteristics were independently associated with knowledge of rabies in Flagstaff (Table 3). Male respondents were more likely to have knowledge of rabies in Flagstaff than female respondents. Multivariate analysis did not identify an independent association between those who have knowledge of rabies in Flagstaff and contact with a nuisance wild animal.
Pet and dog owners were more likely to have had contact with a sick domestic animal and to be aware of the rabies quarantine than those who did not own pets (Table A2). Pet ownership in general was associated with knowledge of rabies. In multivariate analyses, pet owners were less likely to believe that the leash policy prevents exposures to rabid animals than non–pet owners. Dog owners were more likely to be aware of the 2009 quarantine (Table 3). There was significant interaction between age group and potential for contact with sick domestic animals, and for respondents <60 years of age, those that indicated potential for contact with a sick domestic animal were more likely to be general pet owners or dog owners. Among women, general pet owners were more likely to be aware of the quarantine than non–pet owners; this association was not seen for men. Men and women were similarly aware of the quarantine (83% and 84%, respectively).
Persons who had translocated nuisance animals were more likely to be male and to not own a pet (Table A2), although these associations did not remain independently significant in the multivariate analysis (Table 3). In the multivariate analyses, those who moved animals from their property were more likely to have a potential for contact with a wild animal and to have lived in Flagstaff for at least 10 years.
An extensive outbreak control and education campaign took place in 2009. As observed in past interventions, the epizootic waned and in 2010 only 4 rabid bats were reported from Coconino County. This decline in rabid animals is likely attributable, in part, to the broad interagency control campaigns. Whether another epizootic will occur in Flagstaff remains to be determined. However, the multiple outbreaks over the last decade have resulted in a substantial change in rabies epizootiology in northern Arizona. The repercussions of a potential perpetuation of a bat rabies virus variant in gray fox populations are a concern, given the wide-ranging movements of these carnivores. In addition, these outbreaks have been associated with an increased number of visits to the emergency department of a local hospital, where 48% of persons with animal bite-related visits required rabies PEP in 2009. Heightened vigilance and continued laboratory-based surveillance are warranted in the immediate vicinity and surrounding areas.
Educational efforts were initiated by Coconino County during the current and previous epizootics (6). Residents of Flagstaff have received educational messages about rabies and the existing outbreaks through many methods, which likely had a positive effect on the extent of knowledge retained by community members.
Although residents had a general knowledge of rabies as a disease, a large number of persons did not give correct answers to some general knowledge questions, including routes of exposure and animals that can be infected. These misconceptions have been noted in other surveys (10,11). Future efforts should consider including information about which animals have been reported as rabid in the community and what animals are susceptible. Furthermore, education efforts should focus on specific exposure routes of concern and address possible misconceptions regarding the infectious nature of other bodily fluids such as blood, urine, feces, or skunk spray. This information could play a key role in reducing public concern about rabies virus exposure from noninfectious routes.
Most respondents reported appropriate medical responses to being bitten or scratched by an animal, which include washing of the wound and seeking medical care. Decisions on the risk for rabies and administration of rabies PEP should be made by medical professionals with consultation from local or state public health professionals (12). Information about appropriate actions after animal exposure should be maintained in future outreach materials.
The City of Flagstaff Animal Control and Coconino County Public Health Services District Animal Management Office respond to calls related to wild and domestic animals, while the Arizona Game and Fish Department responds only to calls related to wild animals. In contrast to a large number of respondents (>40%) indicating that they would notify one of the agencies of an ill animal on their property, 32% of persons who had seen an ill animal (including bat, skunk, and fox) did nothing. Regardless of these differences, clear, concise instruction about which agency should be notified would be useful for residents and may help streamline notification.
During the recent rabies outbreak in Flagstaff, human and pet exposures occurred from encounters with rabid foxes and skunks. Rabid animals exhibit aggressive or altered behavior which puts others at risk. However, in some circumstances, human-animal contact is a result of the person initiating contact with the animal. Some respondents indicated that they would put themselves in direct contact with ill or nuisance wild animals, and some have trapped and translocated nuisance animals, primarily skunks. The county provides traps for residents to use, with the request that residents bring trapped animals to animal control. This service increases the likelihood that some residents will 1) come into contact with an unknown animal and 2) may translocate that animal. This analysis identified living in Flagstaff for at least 10 years as a characteristic associated with translocators. Long-term residents may be more aware of traps provided by the county.
Approximately half of respondents who have translocated animals moved the animal to an area >5 miles from their property. Thus, long range movement of reservoirs, possibly outside of the trap-vaccinate-release area, has probably occurred. Consequently, not only does translocation expand the range of an outbreak, but removal of target species could diminish local herd immunity by removal of vaccinated animals. Translocation of animals threatens the success of control programs and the spread of rabies has been attributed to translocation (13,14). Continued outreach, to the community and nuisance operators, should emphasize the risks of translocation to humans, animal populations, and rabies control programs. No local ordinances address the topic or prohibit translocation in Coconino County. State and local ordinances and enforcement should be considered to prevent translocation of rabies reservoirs.
This study found that pet owners had a basic knowledge of rabies and the quarantine. A recent survey conducted in Texas found that dog owners knew more specific facts about rabies than persons who did not own dogs (15). Several respondents in Flagstaff noted learning about the outbreak from their veterinarian. This survey did not assess specifics of veterinarian instruction to pet owners; however, this would be a useful avenue of study (15). Dog owners were less likely to believe that a mandatory leash policy would help prevent exposure to rabid animals. Local trails are popular destinations for dog owners, and dogs are frequently taken off the leash on these trails. Outreach about exposures and risks to humans and their pets may be warranted for dog owners in particular.
The households in the quarantine area that participated in this study have a larger number of dogs (0.71 for every household) than the estimated national average of 0.63, and an average number of cats the same as the national average (0.48 per household) (16). Whether the high proportion of vaccinated animals found in this survey is a reflection of the demographics of the households or a result of the ongoing outbreak and quarantine regulations, is unknown. Vaccination of dogs, but not cats, is required in Arizona (1), and Arizona utilizes the vaccination scheme recommended in the 2008 Compendium of Animal Rabies Prevention and Control which recommends that dogs and cats be vaccinated at 3 months of age, 12 months of age, and a receive a booster every year or every 3 years, depending on vaccine label specifications (17). Cats are the leading domestic animal reported with rabies in the United States, and consequently, cats are responsible for a substantial proportion of rabies exposures to persons (18). Vaccination of companion animals that have regular human contact is a basic, simple, and critical barrier to exposure. Veterinarians and public health, and animal control personnel should emphasize vaccination of domestic dogs and cats. Continued education and vaccination measures will help alleviate risk to companion animals, and subsequently, to humans.
This study has several limitations. First, only household members in Flagstaff who responded to the survey are characterized in this study, and without characterization of nonresponders, a nonresponse bias cannot be evaluated. Also, not all questions were answered by all respondents. Compared with the 2000 US Census data for Flagstaff (19), the survey respondents were older (68% vs. 5.3% >65 years of age), more likely to have a college degree (75% vs. 39.4%), and more likely to be female (59% vs. 50.4%). Taken together, these demographics may have biased the study in regards to rabies knowledge, but these differences are not necessarily correlated with increased rabies knowledge. In addition, this survey was paper-based with the option to respond to an online version. Less than 2% of completed surveys were Internet-based. The results may be biased and reflect a population that is more likely to complete a paper-based survey versus using social media or a survey administered through email. Also, data from factors such as language barriers and social economic status were not collected, and the results may be affected by such factors.
The findings of this study provide helpful information for county public health in support of their community outreach efforts and where additional efforts might be focused. In particular, a focus on reinforcing rabies virus transmission routes and exposure guidelines should help reduce public concern about nonexposure events and possibly reduce inquiries to health authorities about such events. This information will be helpful in the event of a future outbreak in Flagstaff or for reference in surrounding areas, especially if rabies expands outside Flagstaff and Coconino County. Rabies has not been reported on the adjacent Navajo Nation for many years. Additional measures would be necessary to tailor prevention and control activities if rabies was to reemerge in this area. In addition to existing messages distributed by media, local public agencies may wish to bolster their existing internet information for the community, as well as outreach through local veterinarians. Outreach to physicians should also be conducted, to reinforce current Advisory Committee on Immunization Practices recommendations on human rabies prevention and PEP administration, as well as to encourage consultation with local and state public health officials to assist with exposure assessment.
Dr McCollum is an epidemiologist in the Poxvirus and Rabies Branch, CDC. Her scientific interests include the epidemiology, ecology, and molecular genetics of infectious diseases.
Acknowledgments
We thank the community of Flagstaff, Arizona, for participation in this survey. We greatly appreciate the support of this activity by the US Department of Agriculture, Animal and Plant Health Inspection Service, Wildlife Services.
Financial support was provided by CDC.
References
- Blanton JD, Palmer D, Rupprecht CE. Rabies surveillance in the United States during 2009. J Am Vet Med Assoc. 2010;237:646–57. DOIPubMedGoogle Scholar
- Christian KA, Blanton JD, Auslander M, Rupprecht CE. Epidemiology of rabies post-exposure prophylaxis—United States of America, 2006–2008. Vaccine. 2009;27:7156–61. DOIPubMedGoogle Scholar
- Rupprecht CE, Willoughby R, Slate D. Current and future trends in the prevention, treatment, and control of rabies. Expert Rev Anti Infect Ther. 2006;4:1021–38. DOIPubMedGoogle Scholar
- Blanton JD, Robertson K, Palmer D, Rupprecht CE. Rabies surveillance in the United States during 2008. J Am Vet Med Assoc. 2009;235:676–89. DOIPubMedGoogle Scholar
- Leslie MJ, Messenger S, Rohde RE, Smith J, Cheshier R, Hanlon C, Bat-associated rabies virus in skunks. Emerg Infect Dis. 2006;12:1274–7. DOIPubMedGoogle Scholar
- Engeman RM, Christensen KL, Pipas MJ, Berhman DL. Population monitoring in support of a rabies vaccination program for skunks in Arizona. J Wildl Dis. 2003;39:746–50.PubMedGoogle Scholar
- Centers for Disease Control and Prevention. Rabies [cited 2012 Apr 6]. http://www.cdc.gov/RABIES.
- Kleinbaum DG, Klein M. Logistic regression: a self-learning text. New York: Springer-Verlag; 2002.
- Grosenbaugh DA, Maki JL, Rupprecht CE, Wall DK. Rabies challenge of captive striped skunks (Mephitis mephitis) following oral administration of a live vaccinia-vectored rabies vaccine. J Wildl Dis. 2007;43:124–8.PubMedGoogle Scholar
- Schopler RL, Hall AJ, Cowen P. Survey of wildlife rehabilitators regarding rabies vector species. J Am Vet Med Assoc. 2005;227:1568–72. DOIPubMedGoogle Scholar
- Ichhpujani RL, Chhabra M, Mittal V, Bhattacharya D, Singh J, Lal S. Knowledge, attitude, and practices about animal bites and rabies in general community—a multi-centric study. J Commun Dis. 2006;38:355–61.PubMedGoogle Scholar
- Rupprecht CE, Briggs D, Brown CM, Franka R, Katz SL, Kerr HD, Use of a reduced (4-dose) vaccine schedule for postexposure prophylaxis to prevent human rabies: recommendations of the advisory committee on immunization practices. MMWR Recomm Rep. 2010;59(RR-2):1–9.PubMedGoogle Scholar
- Chomel BB, Belotto A, Meslin FX. Wildlife, exotic pets, and emerging zoonoses. Emerg Infect Dis. 2007;13:6–11. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Translocation of coyote rabies—Florida, 1994. MMWR Morb Mortal Wkly Rep. 1995;44:580–1.PubMedGoogle Scholar
- Bingham GM, Budke CM, Slater MR. Knowledge and perceptions of dog-associated zoonoses: Brazos County, Texas, USA. Prev Vet Med. 2010;93:211–21. DOIPubMedGoogle Scholar
- American Veterinary Medical Association. U.S. pet ownership and demographics sourcebook. Schaumberg (IL): The Association; 2007.
- National Association of State Public Health Veterinarians, Inc. Compendium of animal rabies prevention and control. MMWR Morb Mortal Wkly Rep. 2008;57:1–5.PubMedGoogle Scholar
- Blanton JD, Bowden NY, Eidson M, Wyatt JD, Hanlon CA. Rabies postexposure prophylaxis, New York, 1995–2000. Emerg Infect Dis. 2005;11:1921–7. DOIPubMedGoogle Scholar
- US Census Bureau. Summary file 1, general demographic characteristics, Table DP-1, Flagstaff City, Arizona. 2000.
Figures
Tables
Cite This ArticleTable of Contents – Volume 18, Number 6—June 2012
| EID Search Options |
|---|
|
|
|
|
|
|

Please use the form below to submit correspondence to the authors or contact them at the following address:
Andrea M. McCollum, Centers for Disease Control and Prevention, 1600 Clifton Rd NE, Mailstop A30, Atlanta, GA 30333, USA:
Top