Volume 11, Number 10—October 2005
Research
Evolution of H5N1 Avian Influenza Viruses in Asia
Cite This Article
Citation for Media
Abstract
An outbreak of highly pathogenic avian influenza A (H5N1) has recently spread to poultry in 9 Asian countries. H5N1 infections have caused >52 human deaths in Vietnam, Thailand, and Cambodia from January 2004 to April 2005. Genomic analyses of H5N1 isolates from birds and humans showed 2 distinct clades with a nonoverlapping geographic distribution. All the viral genes were of avian influenza origin, which indicates absence of reassortment with human influenza viruses. All human H5N1 isolates tested belonged to a single clade and were resistant to the adamantane drugs but sensitive to neuraminidase inhibitors. Most H5N1 isolates from humans were antigenically homogeneous and distinct from avian viruses circulating before the end of 2003. Some 2005 isolates showed evidence of antigenic drift. An updated nonpathogenic H5N1 reference virus, lacking the polybasic cleavage site in the hemagglutinin gene, was produced by reverse genetics in anticipation of the possible need to vaccinate humans.
Highly pathogenic avian influenza viruses of the H5N1 subtype are circulating in eastern Asia with unprecedented epizootic and epidemic effects (1). Nine Asian countries reported H5N1 outbreaks in poultry in 2004: Cambodia, China, Indonesia, Japan, Laos, Malaysia, South Korea, Thailand, and Vietnam (1). Between 2004 and the first 3 months of 2005, a total of 89 laboratory-confirmed human infections, 52 of which were fatal, were reported to the World Health Organization (WHO) by public health authorities in Vietnam, Thailand, and Cambodia. These records indicate that this outbreak of human H5N1 infections is the largest documented since its emergence in humans in 1997 (2). Efficient viral transmission among poultry caused the virus to spread regionally, leading to the loss of >100 million birds from disease and culling. In contrast, human-to-human transmission of the virus is exceptional but has been described, most recently in a family cluster in Thailand (3).
The 3 viral envelope proteins of influenza A virus are most medically relevant. The hemagglutinin (HA), neuraminidase (NA), and M2 are essential viral proteins targeted by host antibodies or antiviral drugs such as oseltamivir and rimantadine (4–6). The HA glycoprotein forms spikes at the surface of virions, mediating attachment to host cell sialoside receptors and subsequent entry by membrane fusion. The NA forms knoblike structures on the surface of virus particles and catalyzes their release from infected cells, allowing virus spread. The M2 is a transmembrane protein that forms an ion channel required for the uncoating process that precedes viral gene expression.
We report on phylogenetic, phenotypic, and antigenic analysis of H5N1 viruses from the 2004–2005 outbreak, focusing on these 3 genes, to address questions relevant to the public health response to the outbreak: 1) What is the genetic diversity of H5N1 viruses involved in human infections? 2) Can the relationship between human and avian H5N1 isolates help explain the source of infection? 3) Do genetic changes correlate with enhanced viral transmissibility in humans? 4) How sensitive are H5N1 isolates to antiviral drugs? 5) What is the antigenic similarity between human H5N1 viruses and current candidate vaccines? and 6) Can candidate vaccine reference stocks be developed in time for an effective public health response?
All work involving infectious H5N1 influenza was performed in government-approved biosafety level 3–enhanced containment facilities with experimental protocols in compliance with applicable federal statutes and institutional guidelines. Influenza A (H5N1) viruses isolated in Asia and A/Puerto Rico/8/34 (PR8) (H1N1) were propagated in embryonated chicken eggs or in Madin-Darby canine kidney (MDCK) cells. The African green monkey kidney Vero cell line was from a cell bank certified for human vaccine production.
Viral RNA was extracted by using a commercial lysis solution and resin kit and amplified by reverse transcriptase–polymerase chain reaction with specific oligonucleotide primers. Nucleotide sequencing reactions were performed with a cycle sequencing kit and resolved on an ABI 3100 Genetic Analyzer (Applied Biosystems, Foster City, CA, USA). DNA sequence analysis was performed by using version 10 of the GCG sequence analysis package (7), and phylogeny was inferred by using a neighbor-joining tree reconstruction method implemented in the Phylip package (8).
Postinfection ferret antisera were prepared as previously described (9). Hemagglutination inhibition (HI) testing was performed as previously described with turkey erythrocytes (10).
Median inhibitory concentration (IC50) values for oseltamivir and zanamivir were determined by using NA-Star substrate and Light Emission Accelerator IITM (Applied Biosystems, Bedford, MA, USA) as previously described (11). Biological susceptibility to rimantadine was determined by recording the yield of viral progeny in MDCK cells infected with the H5N1 strains of interest at a multiplicity of >10 median egg infectious doses in the absence or presence of 2 μg/mL rimantadine.
Plasmids with full-length cDNA from the 6 internal genes (PB1, PB2, PA, NP, M, NS) of influenza virus PR8 strain (12), flanked by human RNA polymerase I (PolI) promoter and polyadenylation site at the 3´ end and a PolI terminator as well as a PolII promoter at the 5´ end, were generated as described previously (12–14). The cDNA of N1 NA or H5 HA genes of VN/1203/2004 or VN/1194/2004 (VN/04-like) were inserted into plasmids as described above. The 4 basic amino acid codons from the cleavage site of HA were deleted by overlap extension PCR, as described previously (sequences available upon request) (13,15–17).
PR8 reassortant viruses with HA and NA from VN/04-like viruses were generated by plasmid DNA-based reverse genetics in Vero cell under good laboratory practice conditions appropriate for future human use. Candidate vaccine reference reagent reassortant viruses were generated at the National Institute of Biological Standards and Control (NIBSC), South Mimms, United Kingdom; Saint Jude Children's Research Hospital (SJCRH), Memphis, Tennessee, USA; and Centers for Disease Control and Prevention (CDC), Atlanta, Georgia, USA. For brevity, the reverse genetics derivation method described represents a consensus of the institutions; minor unpublished protocol details unique to each laboratory were not described and are available upon request. The VN/04x/PR8 reassortant virus was recovered in embryonated eggs and identified in the allantoic fluid by HA assay. The genetic and antigenic properties of the resulting reassortant virus were determined as described previously (15,18–20). Candidate vaccine stocks were subjected to virulence studies in avian, murine, and ferret models to establish their safety (19).
Analysis of HA, NA, and M2 Genes from H5N1 Viruses
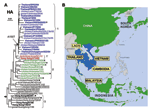
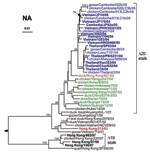
Phylogenetic analyses of the H5 HA genes from the 2004 and 2005 outbreak showed 2 different lineages of HA genes, termed clades 1 and 2. Viruses in each of these clades are distributed in nonoverlapping geographic regions of Asia (Figure 1). The H5N1 viruses from the Indochina peninsula are tightly clustered within clade 1, whereas H5N1 isolates from several surrounding countries are distinct from clade 1 isolates and belong in the more divergent clade 2. Clade 1 H5N1 viruses were isolated from humans and birds in Vietnam, Thailand, and Cambodia but only from birds in Laos and Malaysia. The clade 2 viruses were found in viruses isolated exclusively from birds in China, Indonesia, Japan, and South Korea. Viruses isolated from birds and humans in Hong Kong in 2003 and 1997 made up clades 1´ and 3, respectively.
The HA genes from H5N1 viruses isolated from human specimens were closely related to HA genes from H5N1 viruses of avian origin; human HA gene sequences differ from the nearest gene from avian isolates from the same year in 2–14 nucleotides (<1% divergence). These findings are consistent with the epidemiologic data that suggest that humans acquired their infections by direct or indirect contact with poultry or poultry products (21).
Analysis of the amino acid sequences showed that both clades of H5 HAs from the 2004–2005 outbreak have a multiple basic amino acid motif at the cleavage site, a defining feature of highly pathogenic avian influenza viruses. Among all H5N1 isolates collected in east Asia since 1997, only those in clades 1, 1´, and 3 appear to be associated with fatal human infections (22,23). We compared amino acid sequences of HA from contemporary isolates (clades 1 and 2) with those of the fatal H5N1 infections in Hong Kong in 1997 and 2003 to identify changes that may correlate with patterns of human infection (Table 1). Thirteen polymorphic sites were identified when the HA1 from the 4 consensus sequences were compared. One change in the 2004–2005 viruses is serine 129 to leucine (S129L). This change affects receptor binding because S129 makes atomic contact with cellular sialoside receptors (24). A second structural change in HA was the A156T substitution, which resulted in glycosylation of asparagine 154 and is predicted to reduce its affinity for sialosides. This change is commonly associated with viral adaptation to terrestrial poultry and increased virulence for these birds (25–27).
Because of the heightened alert due to H5N1 infections in Vietnam during the first months of 2005, we examined the HA sequences for evidence of shared amino acid changes. The HA of viruses isolated in the first 3 months of 2005 showed several amino acid changes relative to 2004 viruses (Table 1). None of the changes in the HA were common to all the 2005 viruses, which suggests that these variant viruses are cocirculating independently in poultry. The most commonly observed changes are located within short distances of the receptor-binding site. For example, positions D94, L175, and T188 may modulate the interaction of Y91, H179, and L190 with sialosides. One of the isolates from a fatal infection in 2005 showed a substitution of serine 223 to asparagine, which is predicted to facilitate binding of sialosides commonly found in mammalian species (Table 1).
The growing H5N1 epizootic in eastern Asia could expand the environmental load of virus and cause more infections in mammals (35), which would increase the probability that a highly transmissible virus will emerge in mammals. We therefore analyzed the medically relevant genes from viruses isolated from the beginning of the outbreak until March 2005 to evaluate parameters relevant to public health.
The origin of the HA genes of the 2004–2005 outbreak as well as an earlier isolate from a fatal human infection in Hong Kong in 2003 (clade 1´) can be traced back to viruses isolated in 1997 in Hong Kong (clade 3) and from geese in China (goose/Guangdong/96) (Figure 1A). The phylogeny also shows that viruses with HK/97-like HA may have circulated in avian hosts continuously after 1997, without causing any reported human infections until the 2 confirmed cases in Hong Kong in February 2003 (28).
The 2004–2005 H5N1 isolates are sensitive to 2 neuraminidase inhibitors that are recommended for prophylactic or therapeutic intervention against human infections with recent H5N1 strains. Rapidly testing potentially pandemic influenza viruses for their susceptibility to licensed drugs is essential to establish appropriate control measures.
An effective H5N1 vaccine is a public health priority and the cornerstone for pandemic prevention and control. Reverse genetics approaches allow the rapid production of high-growth PR8 reassortant viruses by engineering a virus with a homologous HA gene lacking the polybasic amino acids associated with high virulence. These candidate H5N1 pandemic vaccine viruses have been made available to vaccine manufacturers to produce pilot lots for clinical trials and are available for possible large-scale manufacturing should the need arise.
Genetic and antigenic analyses have shown that, compared to previous H5N1 isolates, 2004–2005 isolates share several amino acid changes that modulate antigenicity and perhaps other biological functions. Furthermore, our molecular analysis of the HA from isolates collected in 2005 suggests that several amino acids located near the receptor-binding site are undergoing change, some of which may affect antigenicity or transmissibility. For example, an isolate (VN/JP12-2/05) showed a change from serine to asparagine at position 223 of the HA1 (S223N) that may affect receptor-binding specificity (36). The VN/30321/05 isolate demonstrated considerable antigenic drift from VN/04-like isolates, which have been selected as the candidate vaccine antigens. Further surveillance to determine the prevalence of such variants in poultry will be critical to determine if these variants compromise the efficacy of the candidate vaccine or increase the efficiency of transmission.
The phylogenies of the 8 genomic segments from the clade 1 and 2 isolates from 2004–2005 showed that all genes are of avian origin. All H5N1 isolates from both clades belong to 1 of the genotypes recently circulating in Eastern and Southern Asia, e.g., genotypes V and Z (1,37). The influenza virus genome has remarkable plasticity because of a high mutation rate and its segmentation into 8 separate RNA molecules. This segmentation allows frequent genetic exchange by segment reassortment in hosts co-infected with 2 different influenza viruses. No evidence has been seen that the 2004–2005 H5N1 isolates have acquired nonavian influenza genes by reassortment. However, continued surveillance is important because genetic reassortment may facilitate the evolution of viruses with increased virulence or expanded host range.
The currently circulating H5N1 viruses were reported to infect domestic or wild captive felids, such as tigers, feeding on infected bird carcasses, and the infected cats can transmit H5N1 to pen mates (38). Furthermore, circumstantial evidence indicates that tiger-to-tiger transmission of H5N1 has occurred at a zoo in Thailand (39). Recent evidence of person-to-person transmission and the clustering of H5N1 cases raise the level of concern for a pandemic of H5N1 influenza (3). Therefore, sustained and aggressive efforts to control H5N1 circulation in poultry are mandatory to avoid possible catastrophic public health consequences.
Acknowledgments
We thank Ruben O. Donis for drafting the manuscript on behalf of the WHO team, Michael Shaw for phylogenetic analyses, WHO Geneva for coordinating access to specimens, and Catherine Macken for providing access to the Influenza Sequence Database. The WHO Global Influenza Surveillance Network would like to thank WHO regional offices for Southeast Asia and the Western Pacific and WHO country offices for their generous and valuable support in sharing viruses and specimens between affected countries and WHO.
Research at St. Jude Hospital was supported in part by grant AI95357 from the National Institutes of Health.
References
- Li KS, Guan Y, Wang J, Smith GJ, Xu KM, Duan L, Genesis of a highly pathogenic and potentially pandemic H5N1 influenza virus in eastern Asia. Nature. 2004;430:209–13. DOIPubMedGoogle Scholar
- World Health Organization. Confirmed human cases of avian influenza A(H5N1) since 28 January 2004 [on the Internet]. 2005 Jan 26 [cited 2005 Aug 1]. Available from http://www.who.int/csr/disease/avian_influenza/country/cases_table_2005_01_26/en/
- Ungchusak K, Auewarakul P, Dowell SF, Kitphati R, Auwanit W, Puthavathana P, Probable person-to-person transmission of avian influenza A (H5N1). N Engl J Med. 2005;352:333–40. DOIPubMedGoogle Scholar
- Wilson IA, Cox NJ. Structural basis of immune recognition of influenza virus hemagglutinin. Annu Rev Immunol. 1990;8:737–71. DOIPubMedGoogle Scholar
- Welliver R, Monto AS, Carewicz O, Schatteman E, Hassman M, Hedrick J, Effectiveness of oseltamivir in preventing influenza in household contacts: a randomized controlled trial. JAMA. 2001;285:748–54. DOIPubMedGoogle Scholar
- Hay AJ, Wolstenholme AJ, Skehel JJ, Smith MH. The molecular basis of the specific anti-influenza action of amantadine. EMBO J. 1985;4:3021–4.PubMedGoogle Scholar
- Devereux J. Comprehensive set of sequence analysis programs for the VAX NAR. Nucleic Acids Res. 1986;12:387–95. DOIGoogle Scholar
- Felsenstein J. PHYLIP Phylogeny Inference Package Version 3.2. Cladistics. 1989;5:164–6.
- Kendal AP, Pereira MS, Skehel JJ. Hemagglutination inhibition. In: Kendal AP, Pereira MS, Skehel JJ, editors. Concepts and procedures for laboratory-based influenza surveillance. Atlanta: Centers for Disease Control and Prevention and Pan-American Health Organization; 1982. p. B17–35.
- Stephenson I, Wood JM, Nicholson KG, Zambon MC. Sialic acid receptor specificity on erythrocytes affects detection of antibody to avian influenza haemagglutinin. J Med Virol. 2003;70:391–8. DOIPubMedGoogle Scholar
- Mungall BA, Xu X, Klimov A. Surveillance of influenza isolates for susceptibility to neuraminidase inhibitors during the 2000–2002 influenza seasons. Virus Res. 2004;103:195–7. DOIPubMedGoogle Scholar
- Fodor E, Devenish L, Engelhardt OG, Palese P, Brownlee GG, Garcia-Sastre A. Rescue of influenza A virus from recombinant DNA. J Virol. 1999;73:9679–82.PubMedGoogle Scholar
- Neumann G, Watanabe T, Ito H, Watanabe S, Goto H, Gao P, Generation of influenza A viruses entirely from cloned cDNAs. Proc Natl Acad Sci U S A. 1999;96:9345–50. DOIPubMedGoogle Scholar
- Hoffmann E, Webster RG. Unidirectional RNA polymerase I-polymerase II transcription system for the generation of influenza A virus from eight plasmids. J Gen Virol. 2000;81:2843–7.PubMedGoogle Scholar
- Webby RJ, Perez DR, Coleman JS, Guan Y, Knight JH, Govorkova EA, Responsiveness to a pandemic alert: use of reverse genetics for rapid development of influenza vaccines. Lancet. 2004;363:1099–103. DOIPubMedGoogle Scholar
- Schickli JH, Flandorfer A, Nakaya T, Martinez-Sobrido L, Garcia-Sastre A, Palese P. Plasmid-only rescue of influenza A virus vaccine candidates. Philos Trans R Soc Lond B Biol Sci. 2001;356:1965–73. DOIPubMedGoogle Scholar
- Hoffmann E, Neumann G, Kawaoka Y, Hobom G, Webster RG. A DNA transfection system for generation of influenza A virus from eight plasmids. Proc Natl Acad Sci U S A. 2000;97:6108–13. DOIPubMedGoogle Scholar
- Nicolson C, Major D, Wood JM, Robertson JS. Generation of influenza vaccine viruses on Vero cells by reverse genetics: an H5N1 candidate vaccine strain produced under a quality system. Vaccine. 2005;23:2943–52. DOIPubMedGoogle Scholar
- World Health Organization. Production of pilot lots of inactivated influenza vaccine in response to a pandemic threat: an interim biosafety risk assessment. Wkly Epidemiol Rec. 2003;78:405–8.PubMedGoogle Scholar
- Subbarao K, Chen H, Swayne D, Mingay L, Fodor E, Brownlee G, Evaluation of a genetically modified reassortant H5N1 influenza A virus vaccine candidate generated by plasmid-based reverse genetics. Virology. 2003;305:192–200. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Outbreaks of avian influenza A (H5N1) in Asia and interim recommendations for evaluation and reporting of suspected cases—United States, 2004. MMWR Morb Mortal Wkly Rep. 2004;53:97–100.PubMedGoogle Scholar
- Sturm-Ramirez KM, Ellis T, Bousfield B, Bissett L, Dyrting K, Rehg JE, Reemerging H5N1 influenza viruses in Hong Kong in 2002 are highly pathogenic to ducks. J Virol. 2004;78:4892–901. DOIPubMedGoogle Scholar
- Tumpey TM, Suarez DL, Perkins LE, Senne DA, Lee J, Lee YJ, Evaluation of a high-pathogenicity H5N1 avian influenza A virus isolated from duck meat. Avian Dis. 2003;47(Suppl):951–5. DOIPubMedGoogle Scholar
- Ha Y, Stevens DJ, Skehel JJ, Wiley DC. X-ray structures of H5 avian and H9 swine influenza virus hemagglutinins bound to avian and human receptor analogs. Proc Natl Acad Sci U S A. 2001;98:11181–6. DOIPubMedGoogle Scholar
- Baigent SJ, McCauley JW. Glycosylation of haemagglutinin and stalk-length of neuraminidase combine to regulate the growth of avian influenza viruses in tissue culture. Virus Res. 2001;79:177–85. DOIPubMedGoogle Scholar
- Mitnaul LJ, Matrosovich MN, Castrucci MR, Tuzikov AB, Bovin NV, Kobasa D, Balanced hemagglutinin and neuraminidase activities are critical for efficient replication of influenza A virus. J Virol. 2000;74:6015–20. DOIPubMedGoogle Scholar
- Perdue ML, Suarez DL. Structural features of the avian influenza virus hemagglutinin that influence virulence. Vet Microbiol. 2000;74:77–86. DOIPubMedGoogle Scholar
- Guan Y, Poon LL, Cheung CY, Ellis TM, Lim W, Lipatov AS, H5N1 influenza: a protean pandemic threat. Proc Natl Acad Sci U S A. 2004;101:8156–61. DOIPubMedGoogle Scholar
- Bender C, Hall H, Huang J, Klimov A, Cox N, Hay A, Characterization of the surface proteins of influenza A (H5N1) viruses isolated from humans in 1997–1998. Virology. 1999;254:115–23. DOIPubMedGoogle Scholar
- Matrosovich M, Zhou N, Kawaoka Y, Webster R. The surface glycoproteins of H5 influenza viruses isolated from humans, chickens, and wild aquatic birds have distinguishable properties. J Virol. 1999;73:1146–55.PubMedGoogle Scholar
- Leneva IA, Roberts N, Govorkova EA, Goloubeva OG, Webster RG. The neuraminidase inhibitor GS4104 (oseltamivir phosphate) is efficacious against A/Hong Kong/156/97 (H5N1) and A/Hong Kong/1074/99 (H9N2) influenza viruses. Antiviral Res. 2000;48:101–15. DOIPubMedGoogle Scholar
- Subbarao K. Influenza vaccines: present and future. Adv Virus Res. 1999;54:349–73. DOIPubMedGoogle Scholar
- Kilbourne ED. Future influenza vaccines and the use of genetic recombinants. Bull World Health Organ. 1969;41:643–5.PubMedGoogle Scholar
- Hoffmann E, Krauss S, Perez D, Webby R, Webster RG. Eight-plasmid system for rapid generation of influenza virus vaccines. Vaccine. 2002;20:3165–70. DOIPubMedGoogle Scholar
- Keawcharoen J, Oraveerakul K, Kuiken T, Fouchier R, Amonsin A, Payungporn S, Avian influenza H5N1 in tigers and leopards. Emerg Infect Dis. 2004;10:2189–91.PubMedGoogle Scholar
- Harvey R, Martin AC, Zambon M, Barclay WS. Restrictions to the adaptation of influenza a virus h5 hemagglutinin to the human host. J Virol. 2004;78:502–7. DOIPubMedGoogle Scholar
- Mase M, Tsukamoto K, Imada T, Imai K, Tanimura N, Nakamura K, Characterization of H5N1 influenza A viruses isolated during the 2003–2004 influenza outbreaks in Japan. Virology. 2005;332:167–76. DOIPubMedGoogle Scholar
- Kuiken T, Rimmelzwaan G, van Riel D, van Amerongen G, Baars M, Fouchier RA, Avian H5N1 influenza in cats. Science. 2004;306:241. DOIPubMedGoogle Scholar
- Thanawongnuwech R, Amonsin A, Tantilertcharoen R, Damrongwatanapokin S, Theamboonlers A, Payungporn S, Probable tiger-to-tiger transmission of avian influenza H5N1. Emerg Infect Dis. 2005;11:699–701.PubMedGoogle Scholar
Figures
Tables
Cite This Article1Members of the World Health Organization Global Influenza Program and collaborating laboratories: Jean-Thierry Aubin, Saliha Azebi, Amanda Balish, Jill Banks, Niranjan Bhat, Rick A. Bright, Ian Brown, Philippe Buchy, Ana-Maria Burguiere, Hua-lan Chen, Peter Cheng, Nancy J. Cox, Alice Crosier, Aaron Curns, Frédérique Cuvelier, Guohua Deng, Julia Desheva, Stéphanie Desvaux, Nguyen Hong Diep, Ruben O. Donis, Alan Douglas, Scott F. Dowell, Nguyen Tien Dung, Lindsay Edwards, Keiji Fukuda, Rebecca Garten, Elena Govorkova, Victoria Gregory, Alan Hampson, Nguyen Thi Hong Hanh, Scott Harper, Alan Hay, Erich Hoffmann, Diane Hulse, Masaki Imai, Shigeyuki Itamura, Samadhan Jadhao, Patricia Jeannin, Chun Kang, Jackie Katz, Jae-Hong Kim, Alexander Klimov, Yong-kuk Kwon, Chang-Won Lee, Phuong Song Lien, Yanbing Li, Wilina Lim, Yi Pu Lin, Stephen Lindstom, LaMorris Loftin, Jan Mabry, Le Quynh Mai, Taronna Maines, Jean-Claude Manuguerra, Masaji Mase, Yumi Matsuoka, Margaret McCarron, Marie-Jo Medina, Doan Nguyen, Ai Ninomiya, Masatsugu Obuchi, Takato Odagiri, Malik Peiris, Michael L. Perdue, Jean-Marc Reynes, James Robertson, Claudine Rousseaux, Takehiko Saito, Somchai Sangkitporn, Michael Shaw, James M. Simmerman, M. Slomka, Catherine Smith, San Sorn, Erica Spackman, Klaus Stöhr, David L. Suarez, Haan Woo Sung, David E Swayne, Maryse Tardy-Panit, Masato Tashiro, Pranee Thawatsupha, Terrence Tumpey, Timothy Uyeki, Phan Van Tu, Sylvie van der Werf, Sirenda Vong, Richard Webby, Robert Webster, John Wood, Xiyan Xu, Guan Yi, and Wenqing Zhang. For author affiliations, please Download PDF (37 KB, 2 pages).
Table of Contents – Volume 11, Number 10—October 2005
| EID Search Options |
|---|
|
|
|
|
|
|