Volume 18, Number 8—August 2012
Letter
Identification of Cause of Posttransplant Cachexia by PCR
To the Editor: A man, 56 years of age, was admitted to the hospital for epigastric pain, fever, and fatigue 8 years after a cardiac transplant. His immunosuppressive regimen consisted of cyclosporine A, mycophenolate mofetil, and steroids. Clinical examination revealed a 4-kg weight loss within 3 months without peripheral lymph node enlargement.
Laboratory test results showed moderate anemia, severe lymphopenia, and moderately increased C-reactive protein. Serologic results for HIV, Brucella spp., Coxiella burnetii, and Francisella tularensis were negative. Whole-body computed tomography scanning showed enlarged mediastinal and abdominal lymph nodes. Bone marrow histopathologic results ruled out lymphoma or granuloma but showed a histiocytic infiltrate and intracellular acid-fast bacilli (AFB) with positive Ziehl–Neelsen staining. Sputum, urine, gastric aspirates, and bronchoalveolar lavage specimens revealed no AFB. A mediastinal lymph node biopsy showed few AFB, suggesting M. tuberculosis or nontuberculous mycobacteria. Isoniazid, rifampin, ethambutol, and clarithromycin were prescribed for 2 months, followed by rifampin, ethambutol, and clarithromycin. Cultures for mycobacteria remained negative.
Five months after treatment initiation, the patient experienced severe abdominal pain, diarrhea, and continued weight loss. Lymph node biopsy was repeated; results showed intramacrophagic coccobacilli tinted with Ziehl-Neelsen, Gram, and periodic acid–Schiff (PAS) stains. Two diagnoses were considered: malakoplakia and Whipple disease (WD). Screening results from quantitative real-time PCR (qPCR) for Tropheryma whipplei were negative for blood, saliva, stools, urine, and lymph nodes.
Although no characteristic Michaelis–Gutmann bodies were seen, the staining characteristics of the intracellular coccobacilli were compatible with Rhodococcus equi, a pathogen associated with malakoplakia. Combined treatment with ertapenem, teicoplanin, and amikacin was implemented but failed to induce clinical improvement. Culture of the biopsy specimen failed to grow R. equi or mycobacteria, and the result of 16S rRNA PCR was negative. To investigate the cause of the diarrhea, the patient underwent endoscopy, which showed a thickened duodenal wall. A duodenal biopsy specimen displayed a massive histiocytic infiltrate, with positive PAS and Gram staining but negative Ziehl-Neelsen staining. Cultures remained negative for mycobacteria.
Acting on the hypothesis of WD, we administered doxycycline and hydroxychloroquine for 4 weeks, then discontinued for ineffectiveness. Four weeks after cessation of antimicrobial drug treatment, a third lymph node biopsy was performed, in which the T. whipplei PCR result was positive. Antibacterial drug treatment for WD was resumed, but the patient’s condition worsened.
Simultaneously, extracted DNA and fresh tissue of all biopsy specimens were sent to the Unité de Recherche sur les Maladies Infectieuses et Tropicales Emergentes, (Marseille, France), a reference laboratory for WD. Immunohistochemical analysis, DNA extraction, and T. whipplei qPCR were performed as described (1,2). Biopsy specimens were subjected to a systematic molecular approach, which included 16S rRNA PCR and several specific PCRs (3) (Table A1).
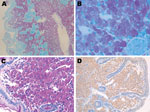
Histopathologic results of the duodenal biopsy revealed PAS-positive and diastase-resistant macrophages (Figure) with faint immunohistochemical staining. Results of T. whipplei PCRs targeting 2 different sequences were negative for the duodenal and lymph node biopsy specimens. These specimens were also negative by PCR for 16S rRNA, Bartonella spp., and F. tularensis. Conversely, Ziehl–Neelsen staining showed numerous AFB. Results of PCRs were negative for M. tuberculosis and M. avium but positive for Mycobacterium spp.
Sequencing facilitated identification of Mycobacterium genavense (99.6% of homology with the isolate with GenBank accession no. HM022216). Combined treatment with amikacin, rifabutin, moxifloxacin, clarithromycin, and ethambutol was implemented. To enhance the chances of eradicating M. genavense, mycophenolate mofetil was discontinued and cyclosporine A reduced. The patient’s condition was largely unimproved; clinical improvement was observed 9 months after treatment reinitiation. Cardiac allograft function remained unaltered. Optimal duration of therapy is unknown; treatment had been ongoing for nearly 12 months at time of publication. More than the choice of antimycobacterial agents, we believe that it is the reduction in immunosuppression and the duration of therapy that eventually facilitated clinical improvement.
M. genavense is a slow-growing, nontuberculous mycobacterium that infects immunocompromised hosts (4). Only 3 cases of M. genavense infection in solid-organ transplant recipients have been reported (5–7). M. genavense has a predilection for the digestive tract, which explains the severity of the gastrointestinal symptoms (4). Moreover, it can mimic the endoscopic and histopathological features of WD (8).
In this case, the positive PAS-staining, the weak positivity of immunochemical staining for T. whipplei, and the false-positive results for 1 PCR temporarily delayed diagnosis. False-positive PCR results have been mainly reported when molecular diagnosis for T. whipplei was based on 16S rRNA PCR (9). Thus, positivity of a first PCR should be confirmed by using a second PCR with another target (10).
Bacteria responsible for lymph node enlargement are rarely isolated by culture. Molecular methods performed on lymph node biopsy specimens are useful diagnostic tools, but the common single molecular approach using 16S rRNA PCR lacks sensitivity, which delayed diagnosis for this patient (3). To address this issue, simultaneously to performing 16S rRNA PCR, we followed a strategy of systematic qPCR for lymph node specimens that targeted Bartonella spp., F. tularensis, T. whipplei, and Mycobacterium spp (3). This report confirms the power of this systematic molecular approach, which enabled us to identify a rare bacterial agent scarcely reported for transplant patients.
Acknowledgment
We thank Didier Raoult for his advice and critical review and Marielle Bedotto-Buffet for the technical help.
References
- Fenollar F, Laouira S, Lepidi H, Rolain JM, Raoult D. Value of Tropheryma whipplei quantitative PCR assay for the diagnosis of Whipple’s disease— usefulness of saliva and stool specimens for first line screening. Clin Infect Dis. 2008;47:659–67. DOIPubMedGoogle Scholar
- Lepidi H, Fenollar F, Gerolami R, Mege JL, Bonzi MF, Chappuis M, Whipple’s disease: immunospecific and quantitative immunohistochemical study of intestinal biopsy specimens. Hum Pathol. 2003;34:589–96. DOIPubMedGoogle Scholar
- Angelakis E, Roux V, Raoult D, Rolain JM. Real-time PCR strategy and detection of bacterial agents of lymphadenitis. Eur J Clin Microbiol Infect Dis. 2009;28:1363–8. DOIPubMedGoogle Scholar
- Charles P, Lortholary O, Dechartres A, Doustdar F, Viard JP, Lecuit M, Mycobacterium genavense infections: a retrospective multicenter study between 1996 and 2007 in France. Medicine. 2011;90:223–30. DOIPubMedGoogle Scholar
- Doggett JS, Strasfeld L. Disseminated Mycobacterium genavense with pulmonary nodules in a kidney transplant recipient: case report and review of the literature. Transpl Infect Dis. 2011;13:38–43. DOIPubMedGoogle Scholar
- Nurmohamed S, Weenink A, Moeniralam H, Visser C, Bemelman F. Hyperammonemia in generalized Mycobacterium genavense infection after renal transplantation. Am J Transplant. 2007;7:722–3. DOIPubMedGoogle Scholar
- de Lastours V, Guillemain R, Mainardi JL, Aubert A, Chevalier P, Lefort A, Early diagnosis of disseminated Mycobacterium genavense infection. Emerg Infect Dis. 2008;14:346–7. DOIPubMedGoogle Scholar
- Albrecht H, Rusch-Gerdes S, Stellbrink HJ, Greten H, Jackle S. Disseminated Mycobacterium genavense infection as a cause of pseudo-Whipple’s disease and sclerosing cholangitis. Clin Infect Dis. 1997;25:742–3. DOIPubMedGoogle Scholar
- Fenollar F, Fournier PE, Robert C, Raoult D. Use of genome selected repeated sequences increases the sensitivity of PCR detection of Tropheryma whipplei. J Clin Microbiol. 2004;42:401–3. DOIPubMedGoogle Scholar
Figure
Table
Cite This ArticleRelated Links
Table of Contents – Volume 18, Number 8—August 2012
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Joelle Guitard, Unité de Transplantation d’Organes, Centre Hospitalier Universitaire Rangueil, Toulouse, France
Top