Volume 15, Number 4—April 2009
THEME ISSUE
The Amazon Region
Letter
Lobomycosis in Inshore and Estuarine Dolphins
Cite This Article
Citation for Media
To the Editor: Lobomycosis is a chronic dermal infectious disease affecting humans and some species of dolphins but not, to date, freshwater dolphins. Because this disease is still considered rare despite the increasing number of reported cases in humans and cetaceans, clinical and epidemiologic information must be accurately reported to help clarify many of the unknown aspects of this disease.
We address this point because after carefully reading the excellent report by Elsayed et al. on the first human case of lobomycosis in Canada, we noticed that the authors describe the natural disease as occurring in humans and marine and freshwater dolphins only (1). However, this information is only partially correct because to date lobomycosis has not been described in freshwater dolphins. What is more worrisome is that this information is beginning to be referenced in other published articles (2). So far, lobomycosis has been confirmed in 2 species of inshore and estuarine Delphinidae: 1) the common bottlenose dolphin (Tursiops truncatus) from Brazil, the Atlantic coast of the United States, and Europe and 2) the Guiana dolphin (Sotalia guianensis) from the Surinam River estuary (3–8).
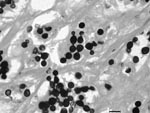
The fact that lobomycosis is endemic in humans in the Amazon basin could logically raise the suspicion that other animal species in this area may act as reservoirs or even be affected by the disease. However, the infection has never, to our knowledge, been reported in botos (Inia geoffrensis) or tucuxis (Sotalia fluviatilis) from the Amazon and Orinoco Rivers. Preliminary field studies, like the one carried out by da Silva et al., failed to demonstrate the disease in any of the 385 live-captured I. geoffrensis boto specimens from the Mamirauá Reserve in the central Amazon region of Brazil (9); similarly, our observational studies in the Venezuelan Orinoco River failed to detect the disease. On the other hand, despite the absence of indigenous cases of lobomycosis in humans reported in the United States, the disease is endemic in dolphins from the Indian River Lagoon in Florida (7), suggesting that no apparent epidemiologic link may exist between humans and cetaceans. Unfortunately, the etiologic agent of lobomycosis, Lacazia loboi (Figure), has not been cultured in vitro (10) despite exhaustive attempts, making its isolation from probable and suspected environmental sources impossible.
Dolphin-to-human transmission of lobomycosis has been reported only 1 time; the case-patient was an aquarium attendant who had had close physical contact with an affected dolphin (5). However, because the possibility of zoonotic transmission of this disease remains latent and because many pathologic and clinical aspects of the disease remain poorly understood, it is imperative to clarify these ecological concepts. Up-to-date molecular epidemiology studies to compare the strains affecting humans and dolphins and their possible phylogenetic relationship are needed.
Acknowledgment
We thank Vera da Silva for her valuable help and are most grateful to Marie-Francoise Van Bressem and the reviewers for their precise comments on the article.
References
- Elsayed S, Kuhn SM, Barber D, Church DL, Adams S, Kasper R. Human case of lobomycosis. Emerg Infect Dis. 2004;10:715–8.PubMedGoogle Scholar
- Pfaller MA, Diekema DJ. Unusual fungal and pseudofungal infections of humans. J Clin Microbiol. 2005;43:1495–504. DOIPubMedGoogle Scholar
- De Vries GA, Laarman JJ. A case of Lobo’s disease in the dolphin Sotalia guianensis. Aquat Mamm. 1973;1:26–33.
- Caldwell DK, Caldwell MC, Woodard JC, Ajello L, Kaplan W, McClure HM. Lobomycosis as a disease of the Atlantic bottle-nosed dolphin (Tursiops truncatus Montagu, 1821). Am J Trop Med Hyg. 1975;24:105–14.PubMedGoogle Scholar
- Symmers WS. A possible case of Lôbo’s disease acquired in Europe from a bottle-nosed dolphin (Tursiops truncatus). Bull Soc Pathol Exot Filiales. 1983;76:777–84.PubMedGoogle Scholar
- Simões-Lopes PC, Paula GS, Xavier FM, Scaramelo AC. First case of lobomycosis in bottlenose dolphin from southern Brazil. Mar Mamm Sci. 1993;9:329–31. DOIGoogle Scholar
- Reif JS, Mazzoil MS, McCullogh SD, Varela R, Goldstein JD, Fair P, Lobomycosis in Atlantic bottlenose dolphins from the Indian River Lagoon, Florida. J Am Vet Med Assoc. 2006;228:104–8. DOIPubMedGoogle Scholar
- Van Bressem M-F, Van Waerebeek K, Reyes JC, Felix F, Echegaray M, Siciliano S, A preliminary overview of skin and skeletal diseases and traumata in small cetaceans from South American waters. Latin Journal of Aquatic Mammals. 2007;6:7–42.
- da Silva VM, Martin AR, Mikesh E. Skin disease and lesions in the boto Inia geoffrensis in the central Amazon. Abstracts of the 2008 Workshop on Cetacean Skin Diseases; 2008 May 30–31; Santiago de Chile, Chile. Cambridge (UK): International Whaling Commission; 2008. Abstract: SC/60/DW5.
- Taborda PR, Taborda VA, McGinnis MR. Lacazia loboi gen. nov., comb. nov., the etiologic agent of lobomycosis. J Clin Microbiol. 1999;37:2031–3.PubMedGoogle Scholar
Figure
Cite This ArticleRelated Links
Table of Contents – Volume 15, Number 4—April 2009
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Alberto Enrique Paniz-Mondolfi, Department of Pathology and Laboratory Medicine, St. Luke’s-Roosevelt-Beth Israel Medical Center, University Hospital of Columbia University College of Physicians and Surgeons, 1000 10th Ave, New York, NY 10019, USA
Top