Volume 16, Number 7—July 2010
Dispatch
Dogs as Sentinels for Human Infection with Japanese Encephalitis Virus
Cite This Article
Citation for Media
Abstract
Because serosurveys of Japanese encephalitis virus (JEV) among wild animals and pigs may not accurately reflect risk for humans in urban/residential areas, we examined seroprevalence among dogs and cats. We found that JEV-infected mosquitoes have spread throughout Japan and that dogs, but not cats, might be good sentinels for monitoring JEV infection in urban/residential areas.
Japanese encephalitis virus (JEV), a common cause of serious acute encephalitis in humans, is primarily transmitted by Culex tritaeniorhynchus mosquitoes and is widely endemic to Southeast Asia and the Western Pacific region (1). Annual incidence of Japanese encephalitis (JE) is ≈50,000 cases,with 10,000 deaths (2). In Japan during the 1950s, several thousand JE cases occurred each year. However, as a result of a JEV vaccination program, isolation of pig farms, and reduction of mosquitoes, the number of JE cases in Japan has decreased markedly, to <10 cases per year since 1992 (3). In 2005, the strong recommendation for JE vaccination was halted because of a severe vaccine-associated side effect in 1 person; however, since 2009, a newly developed JE vaccine has been available and vaccination has been resumed.
Annual serosurveys for JEV antibodies in pigs, the main amplifiers of JEV, tend to show high seropositivity in western Japan (3). Our previous study of JEV in wild animals in the Kinki district also showed high seroprevalence: 83% among wild boars and 59% among raccoons (4). These data indicate that JEV remains endemic to Japan.
However, serosurveys of wild animals and pigs may not accurately reflect risk for humans because these animals remain separate from human populations and thus may not indicate the prevalence of JEV in urban/residential areas of Japan. Therefore, additional monitoring of the risk for JEV infection in humans in these areas, in addition to annual surveillance of pigs, is needed. To determine seroprevalence in family-owned dogs and cats, which share living space with humans, we conducted serosurveys of JEV in these species.
First, to examine whether dogs and cats were infected with JEV, we analyzed serum samples from 100 dogs and 292 cats in Yamaguchi Prefecture, which is in the western part of Honshu, Japan. Dog samples were collected during 2006–2007, and cat samples were collected during 1997–1999 and 2004–2005. An 80% plaque-reduction neutralizing test using virus JEV/sw/Chiba/88/2002 was performed as described (4). Virus JEV/sw/Chiba/88/2002 is genetically classified as genotype I (5). To analyze the results statistically, we performed χ2 and Fisher exact probability tests. The significance level was p<0.05.
Results showed that 17% of dogs and 1% of cats were seropositive for JEV; thus, seropositivity was ≈10-fold higher among dogs than among cats (Table 1). In addition, outdoor-only dogs (38%) were 3.7-fold more likely to be seropositive than were indoor-only dogs (10%) (p<0.05). Antibody prevalence did not differ significantly between male (14%) and female (20%) dogs (p>0.05; data not shown).
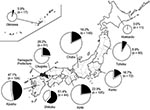
Next, serum samples from 652 dogs in every district in Japan during 2006–2007 were examined for seroprevalence of JEV. The results showed that 25% of dogs had virus-neutralizing antibodies against JEV. In northern Japan, 0% and 9% of dogs from the Hokkaido and Tohoku districts, respectively, were seropositive; these levels were significantly lower than those for other districts (p<0.05). In contrast, in southern Japan, 61% and 47% of dogs in the Shikoku and Kyushu districts, respectively, were seropositive; these levels were significantly higher than those for other districts (p<0.05). Seropositivity to JEV in the Kanto (17%), Chubu (18%), Kinki (23%), and Chugoku (26%) districts showed no significant differences (p>0.05) (Figure). In addition, 45% of outdoor-only dogs and 8% of indoor-only dogs were seropositive for JEV, thus confirming that outdoor-only dogs were 5.5-fold more likely than indoor-only dogs to be seropositive (p<0.05) (Table 2). Regarding the areas of residence, 21% of dogs in urban/residential areas and 43% of dogs in rural areas were seropositive; the results for rural areas were significantly higher than those for urban/residential areas (Table 2). No significant correlation was found between ages of dogs and JEV seropositivity (data not shown).
Our findings of significantly higher JEV seropositivity among dogs than cats are similar to those found in a 1954–1955 study in which 55% of dogs and 10% of cats were seropositive for JEV (6). Studies of another mosquito-vectored virus found 26% of dogs and 9% of cats in Louisiana and 5% of dogs and no cats in New York to be seropositive for West Nile virus (WNV) (7,8). Previous reports on host feeding patterns of JEV and WNV vectors showed that although Culex spp. mosquitoes feed on various mammals, including dogs, cats, and humans, they tend to feed more on dogs than on cats or humans (9,10). These reports are consistent with our finding that seropositivity was higher among dogs than among cats and humans and indicate that some JEV vectors do occasionally feed on humans.
Our nationwide serosurvey indicated that JEV prevalence was significantly lower in the Hokkaido and Tohoku districts and significantly higher in the Kyushu and Shikoku districts (Figure). Annual serosurveys of pigs have also shown that JEV seropositivity rates are higher for pigs in western than in northern Japan. In addition, during 2005–2007 in Japan, 24 JE cases in humans were reported, most of which occurred in western Japan (11). This finding is consistent with our data, suggesting that serosurveys in dogs accurately reflect JEV infection risk for humans in Japan.
Our finding that 45% of outdoor-only dogs were seropositive for JEV is similar to the finding of a previous study, conducted during a WNV epidemic among humans, that 69% of outdoor-only dogs were seropositive for WNV (7). A serosurvey in the Kanto district of Tokyo during 1954–1955 showed that 49% of stray dogs were seropositive for JEV (6). Results of these studies are similar to our results, indicating that risk for JEV infection remains high in Japan, particularly in the western part. In addition, confirmation of seropositivity among indoor-only dogs (8%) indicates that JEV-infected mosquitoes may enter houses; thus, infants and elderly persons, who tend to go outside less frequently, might also be at risk for JEV infection.
That seropositivity in rural areas (43%) was significantly higher than that in urban/residential areas (21%) suggests that pig farms and rice paddies in rural areas are associated with JEV. However, the relatively high seropositivity in urban/residential areas suggests that JEV infection risk for humans remains high, even in areas with few pig farms and rice paddies. Because pigs are housed away from humans, serosurveys of pigs in urban/residential areas are limited. Therefore, dogs, which are found in all areas of Japan, may be better sentinels for JEV infection in these areas. However, information such as whether dogs become viremic after JEV infection or how long anti-JEV antibodies last in them remains unclear.
In conclusion, using dogs as sentinels indicated that the risk for human infection with JEV remains high, even in urban/residential areas. Therefore, to assess the continuing risk for JEV infection in humans in urban/residential areas of Japan, we recommend JEV surveillance among pigs every year and surveillance among dogs every several years.
Mr Shimoda is a student in the Department of Veterinary Medicine, Yamaguchi University, Yamaguchi, Japan. His research interest is zoonoses.
Acknowledgments
We thank Tomohiko Takasaki for kindly providing virus JEV/sw/Chiba/88/2002.
This work was supported by a grant for Research on Emerging and Re-emerging Infectious Diseases from the Ministry of Health, Labour and Welfare of Japan (H20-Shinko-Ippan-003) and by a grant from The Morinaga Foundation.
References
- Mackenzie JS, Chua KB, Daniels PW, Eaton BT, Field HE, Hall RA, Emerging viral diseases of Southeast Asia and the Western Pacific. Emerg Infect Dis. 2001;7:497–504. DOIPubMedGoogle Scholar
- Erlanger TE, Weiss S, Keiser J, Utzinger J, Wiedenmayer K. Past, present, and future of Japanese encephalitis. Emerg Infect Dis. 2009;15:1–7. DOIPubMedGoogle Scholar
- Arai S, Matsunaga Y, Takasaki T, Tanaka-Taya K, Taniguchi K, Okabe N, ; Vaccine Preventable Diseases Surveillance Program of Japan. Japanese encephalitis: surveillance and elimination effort in Japan from 1982 to 2004. Jpn J Infect Dis. 2008;61:333–8.PubMedGoogle Scholar
- Ohno Y, Sato H, Suzuki K, Yokoyama M, Uni S, Shibasaki T, Detection of antibodies against Japanese encephalitis virus in raccoons, raccoon dogs and wild boars in Japan. J Vet Med Sci. 2009;71:1035–9. DOIPubMedGoogle Scholar
- Nerome R, Tajima S, Takasaki T, Yoshida T, Kotaki A, Lim CK, Molecular epidemiological analyses of Japanese encephalitis virus isolates from swine in Japan from 2002 to 2004. J Gen Virol. 2007;88:2762–8. DOIPubMedGoogle Scholar
- Nakamura J. Japanese encephalitis in animals [in Japanese]. Shinkei Kenkyu No Shimpo. 1967;11:19–29.PubMedGoogle Scholar
- Kile JC, Panella NA, Komar N, Chow CC, MacNeil A, Robbins B, Serologic survey of cats and dogs during an epidemic of West Nile virus infection in humans. J Am Vet Med Assoc. 2005;226:1349–53. DOIPubMedGoogle Scholar
- Komar N, Panella NA, Boyce E. Exposure of domestic mammals to West Nile virus during an outbreak of human encephalitis, New York City, 1999. Emerg Infect Dis. 2001;7:736–8. DOIPubMedGoogle Scholar
- Mitchell CJ, Chen PS, Boreham PF. Host-feeding patterns and behavior of 4 Culex species in an endemic area of Japanese encephalitis. Bull World Health Organ. 1973;49:293–9.PubMedGoogle Scholar
- Molaei G, Andreadis TG, Armstrong PM, Bueno R Jr, Dennett JA, Real SV, Host feeding pattern of Culex quinquefasciatus (Diptera: Culicidae) and its role in transmission of West Nile virus in Harris County, Texas. Am J Trop Med Hyg. 2007;77:73–81.PubMedGoogle Scholar
- Japanese encephalitis, Japan, 2003–2008. Infectious Agents Surveillance Report. 2009;30:147–8.
Figure
Tables
Cite This ArticleTable of Contents – Volume 16, Number 7—July 2010
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Ken Maeda, Laboratory of Veterinary Microbiology, Faculty of Agriculture, Yamaguchi University, 1677-1 Yoshida, Yamaguchi 753-8515, Japan
Top