Volume 17, Number 4—April 2011
Letter
Livestock-associated Staphylococcus aureus in Childcare Worker
Cite This Article
Citation for Media
To the Editor: Carriage of Staphylococcus aureus sequence type (ST) 398 has primarily been reported as occurring among persons in contact with livestock, including swine and cattle (1,2). This association has given rise to the characterization of this strain as livestock associated (3). However, ST398 colonization or infection in persons lacking identified livestock-associated risk factors have been reported (4,5). We report ST398 colonization in a childcare worker in Iowa, USA.
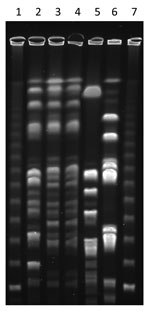
As part of a surveillance study of S. aureus carriage in child daycare facilities, samples were collected from employees, children, and environmental surfaces. Nasal samples were taken from participating children, and nasal and pharyngeal samples were taken from participating employees. All samples were cultured, and S. aureus isolates were examined by pulsed-field gel electrophoresis, spa typing, and antimicrobial drug susceptibility testing and tested for the Panton-Valentine leukocidin gene. One participant was colonized in the nose and throat with t571, a spa type previously reported to correspond to ST398 (1). The isolates were nontypeable when SmaI was used, also a characteristic of ST398 (6). They were digested with Cfr9I and found to be closely related to an ST398 isolate of spa type t034 of swine origin but distinct from S. aureus isolated from 2 other employees at the facility (Figure). Both ST398 isolates were susceptible to methicillin.
The colonized employee was a 24-year-old woman who had worked at the facility for ≈5 years. She reported a history of melanoma but was not currently taking any chemotherapy drugs and had not been hospitalized in the previous 12 months. She reported having a family member who worked in a hospital and had direct contact with patients, but the employee lived alone and responded negatively to questions about whether she or immediate family members had had contact with animals or worked in a processing plant.
ST398 may be transmitted from livestock to community members and then from person to person. It can potentially be transmitted in food; several studies have documented ST398 in raw meats (7,8), and we identified this strain in retail meat products in Iowa (T.C. Smith et al., unpub. data). Secondary transmission of ST398 from colonized persons to contacts has also been suggested, but the few publications reporting this suggest that ST398 seems to be less transmissible by this route than are common human strains (9).
We cannot be sure whether either of these routes played a role in acquisition of ST398 by this employee. Although no other tested persons in this childcare facility were found to carry ST398, only 24 (40%) of the 60 employees and 8 (4.8%) of the 168 children participated, suggesting the possibility of a reservoir in the facility among those who were not tested. Of the 24 employees who participated, 2 reported occupational contact with any animals, 2 reported contact with swine, and 3 reported contact with cattle. However, no participant reported having animals other than cats or dogs on their property. It is possible that >1 sampled employee may have been a transient ST398 carrier but negative at the time of our sampling.
Reports of ST398 in persons who had no direct contact with livestock in the United States are rare (10). To provide a better understanding of the epidemiology of this novel strain, further examination of the emergence of this isolate in community settings and on farms is needed.
Acknowledgments
We thank the childcare centers for allowing us to study their children and employees, and we thank Blake Hanson for laboratory support.
Research was approved by the University of Iowa Institutional Review Board (no. 200805708). This project was funded by the National Institute for Occupational Safety and Health through a small project grant provided by the Heartland Center for Occupational Health and Safety and by general funds through the Center for Emerging Infectious Diseases at the University of Iowa. Fellowship support was provided by the Occupational Epidemiology Training Program within the National Institute for Occupational Safety and Health-funded Heartland Center for Occupational Safety and Health (T42 OH008491-03).
References
- Wulf MW, Sorum M, van Nes A, Skov R, Melchers WJ, Klaassen CH, Prevalence of methicillin-resistant Staphylococcus aureus among veterinarians: an international study. Clin Microbiol Infect. 2008;14:29–34. DOIPubMedGoogle Scholar
- Smith TC, Male MJ, Harper AL, Kroeger JS, Tinkler GP, Moritz ED, Methicillin-resistant Staphylococcus aureus (MRSA) strain ST398 is present in midwestern U.S. swine and swine workers. PLoS ONE. 2009;4:e4258. DOIPubMedGoogle Scholar
- Wulf M, Voss A. MRSA in livestock animals—an epidemic waiting to happen? Clin Microbiol Infect. 2008;14:519–21. DOIPubMedGoogle Scholar
- Golding GR, Bryden L, Levett PN, McDonald RR, Wong A, Wylie J, Livestock-associated methicillin-resistant Staphylococcus aureus sequence type 398 in humans, Canada. Emerg Infect Dis. 2010;16:587–94.PubMedGoogle Scholar
- Wulf MW, Markestein A, van der Linden FT, Voss A, Klaassen C, Verduin CM. First outbreak of methicillin-resistant Staphylococcus aureus ST398 in a Dutch hospital, June 2007. Euro Surveill. 2008;13: pii: 8051.
- Bens CC, Voss A, Klaassen CH. Presence of a novel DNA methylation enzyme in methicillin-resistant Staphylococcus aureus isolates associated with pig farming leads to uninterpretable results in standard pulsed-field gel electrophoresis analysis. J Clin Microbiol. 2006;44:1875–6. DOIPubMedGoogle Scholar
- Pu S, Han F, Ge B. Isolation and characterization of methicillin-resistant Staphylococcus aureus from Louisiana retail meats. [PMID: 18978079]. Appl Environ Microbiol. 2009;75:265–7. Epub 2008 Oct 31. DOIPubMedGoogle Scholar
- de Boer E, Zwartkruis-Nahuis JT, Wit B, Huijsdens XW, de Neeling AJ, Bosch T, Prevalence of methicillin-resistant Staphylococcus aureus in meat. Int J Food Microbiol. 2009;134:52–6. DOIPubMedGoogle Scholar
- van Rijen MM, Van Keulen PH, Kluytmans JA. Increase in a Dutch hospital of methicillin-resistant Staphylococcus aureus related to animal farming. Clin Infect Dis. 2008;46:261–3. DOIPubMedGoogle Scholar
- Bhat M, Dumortier C, Taylor BS, Miller M, Vasquez G, Yunen J, Staphylococcus aureus ST398, New York City and Dominican Republic. Emerg Infect Dis. 2009;15:285–7. DOIPubMedGoogle Scholar
Figure
Cite This ArticleRelated Links
Table of Contents – Volume 17, Number 4—April 2011
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Tara C. Smith, 200 Hawkins Drive C21F GH, Iowa City, IA 52242, USA
Top