Volume 22, Number 3—March 2016
Letter
Mycobacterium arupense as an Emerging Cause of Tenosynovitis
Cite This Article
Citation for Media
To the Editor: Mycobacterium arupense was identified in 2006 as a novel species within the M. terrae complex with close similarity to M. nonchromogenicum (1). Since then, 8 cases describing clinically notable disease have been published (2–8), including 5 cases of tenosynovitis. We report M. arupense tenosynovitis in an immunocompromised person who received the selective interleukin (IL) 1 β-inhibitor canakinumab.
In July 2014, a 62-year-old man sought treatment at the emergency department, Northwestern Memorial Hospital (Chicago, Illinois, USA), after 1 week of pain and swelling in the right hand. During the previous 5 years, he had received multiple immunomodulatory drugs for treatment of natural killer cell deficiency, hyper–IL-6 syndrome, recurrent polychondritis, and Sweet syndrome. His medications were prednisone (42.5 mg/d), intravenous immunoglobulin (400 mg/kg monthly), and subcutaneous canakinumab (180 mg every 8 weeks, which began 3 weeks before onset of symptoms).
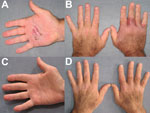
His first symptom was a tender red nodule on the right palm that increased in size and became extremely tender over the following week (Figure, panels A, B). He did not recall any trauma and denied fever or chills. No improvement was seen after he received oral linezolid for 5 days. A skin punch biopsy specimen showed a neutrophilic interstitial infiltrate with no granulomas; results of microbiological stains, including acid-fast bacilli, were negative, . His prednisone dosage was increased to 60 mg/d for suspected Sweet syndrome and, subsequently, to 80 mg/d when no improvement was observed after 2 weeks. A second dose of canakinumab was administered 8 weeks after the first. Shortly after, he was readmitted to the hospital with progression of edema and pain and signs consistent with carpal tunnel syndrome and trigger finger syndrome of the right index finger. Magnetic resonance imaging showed extensive tenosynovitis of the carpal tunnel flexor tendons and no bone erosions. Surgical release and tenosynovectomy of the carpal tunnel was performed; pathologic features demonstrated chronic inflammation of the synovium and absence of granulomas. Results of microbiological stains were negative.
M. arupense grew on Löwenstein-Jensen culture from the skin biopsy specimen after 35 days and from a synovium specimen after 22 days. No growth was observed on liquid culture media. Empiric treatment was started immediately after the first positive culture: clarithromycin (500 mg 2×/d), ethambutol (1,200 mg/d), and rifabutin (300 mg/d). Prednisone was decreased to 45 mg/d, and canakinumab was discontinued. Susceptibility testing confirmed the M. arupense strain’s susceptibility to clarithromycin, ethambutol, and rifabutin (MICs <4.0, <1.25, and <0.12, respectively); intermediate resistance to rifampin and amikacin (MIC 4.0); and resistance to moxifloxacin and ciprofloxacin (MIC >4.0) and to kanamycin (MIC >8.0). Clinical improvement occurred after 8 weeks of treatment; the condition resolved after 6 months (Figure, panels C, D). Treatment was continued for 12 months.
Five other cases of M. arupense tenosynovitis have been reported (2,4,5,7,8); all patients were immunocompetent or minimally immunocompromised (i.e., diabetes mellitus) (Technical Appendix). The hand was the site of infection in all cases, and 4 of 5 patients reported prior trauma to the affected area, which suggests that inoculation was the infection mechanism. In the case we describe, the disease appeared to progress much faster than in the immunocompetent patients (weeks vs. months to years). Acid-fast bacilli stain was negative in all of the cases where it was performed (2,7,8; this study), and growth on solid Löwenstein-Jensen stain or Middlebrook media was seen after a prolonged incubation time, ranging from 27 days to 2 months. Liquid culture media appears to be unreliable for the growth of M. arupense (8; this study).
A combination of tenosynovectomy and prolonged antimycobacterial treatment, guided by in vitro strain susceptibility, was used in all the reported cases; a positive outcome was achieved in 6–14 months. The strain susceptibility results we found are comparable with those in the previous cases, showing consistent susceptibility to clarithromycin, ethambutol, and rifabutin; variable susceptibility to linezolid, streptomycin, and amikacin; and resistance to rifampin and quinolones.
Two cases of M. arupense infection have been reported in immunosuppressed persons, both in HIV/AIDS patients (manifesting as pulmonary infection in 1 patient and disseminated disease in the other) (6). In our study, the immunocompromised patient with M. arupense tenosynovitis received canakinumab, a relatively new biologic agent with a prolonged selective IL-1 β-blockade. Even though the contribution of canakinumab in this case is confounded by concomitant immune deficiencies (natural killer cell deficiency, high-dose corticosteroids), the temporal association between initiation of canakinumab and the onset of symptoms raises concern of a possible association. Animal studies have shown that IL-1 plays a key role in host resistance to mycobacterial infections by regulating Th1/Th2 immune responses and inducing granuloma formation (9). Clinical trials and systematic reviews assessing the safety of IL-1 inhibitors, including anakinra, rilonacept, and canakinumab, have not shown that these drugs lead to an increased risk of tuberculosis or other mycobacterial infections (10). Nonetheless, our report provides increased evidence that M. arupense is an emerging cause of tenosynovitis and that it is potentially associated with immunosuppression.
References
- Cloud JL, Meyer JJ, Pounder JI, Jost KC Jr, Sweeney A, Carroll KC, Mycobacterium arupense sp. nov., a non-chromogenic bacterium isolated from clinical specimens. Int J Syst Evol Microbiol. 2006;56:1413–8. DOIPubMedGoogle Scholar
- Tsai TF, Lai CC, Tsai IC, Chang CH, Hsiao CH, Hsueh PR. Tenosynovitis caused by Mycobacterium arupense in a patient with diabetes mellitus. Clin Infect Dis. 2008;47:861–3. DOIPubMedGoogle Scholar
- Neonakis IK, Gitti Z, Kontos F, Baritaki S, Petinaki E, Baritaki M, Mycobacterium arupense pulmonary infection: antibiotic resistance and restriction fragment length polymorphism analysis. Indian J Med Microbiol. 2010;28:173–6. DOIPubMedGoogle Scholar
- Senda H, Muro H, Terada S. Flexor tenosynovitis caused by Mycobacterium arupense. J Hand Surg Eur Vol. 2011;36:72–3. DOIPubMedGoogle Scholar
- Legout L, Ettahar N, Massongo M, Veziris N, Ajana F, Beltrand E, Osteomyelitis of the wrist caused by Mycobacterium arupense in an immunocompetent patient: a unique case. Int J Infect Dis. 2012;16:e761–2. DOIPubMedGoogle Scholar
- Heidarieh P, Hashemi-Shahraki A, Khosravi AD, Zaker-Boustanabad S, Shojaei H, Feizabadi MM. Mycobacterium arupense infection in HIV-infected patients from Iran. Int J STD AIDS. 2013;24:485–7. DOIPubMedGoogle Scholar
- Lee SJ, Hong SK, Park SS, Kim EC. First Korean case of Mycobacterium arupense tenosynovitis. Ann Lab Med. 2014;34:321–4.
- Beam E, Vasoo S, Simner PJ, Rizzo M, Mason EL, Walker RC, Mycobacterium arupense flexor tenosynovitis: case report and review of antimicrobial susceptibility profiles for 40 clinical isolates. J Clin Microbiol. 2014;52:2706–8. DOIPubMedGoogle Scholar
- Mayer-Barber KD, Barber DL, Shenderov K, White SD, Wilson MS, Cheever A, Caspase-1 independent IL-1 beta production is critical for host resistance to Mycobacterium tuberculosis and does not require TLR signaling in vivo. J Immunol. 2010;184:3326–30. DOIPubMedGoogle Scholar
- Cantarini L, Lopalco G, Caso F, Costa L, Iannone F, Lapadula G, Effectiveness and tuberculosis-related safety profile of interleukin-1 blocking agents in the management of Behçet’s disease. Autoimmun Rev. 2015;14:1–9. DOIPubMedGoogle Scholar
Figure
Cite This ArticleRelated Links
Table of Contents – Volume 22, Number 3—March 2016
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Fiorella Krapp Lopez, Division of Infectious Diseases, Department of Medicine, Northwestern University, 645 N Michigan Ave, Ste 900, Chicago, IL 60611, USA
Top