Volume 26, Number 10—October 2020
Research Letter
Effects of COVID-19 Prevention Measures on Other Common Infections, Taiwan
Cite This Article
Citation for Media
Abstract
To determine whether policies to limit transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) hinder spread of other infectious diseases, we analyzed the National Health Insurance database in Taiwan. Rates of other infections were significantly lower after SARS-CoV-2 prevention measures were announced. This finding can be applied to cost-effectiveness of SARS-CoV-2 prevention.
Drawing from experience with the severe acute respiratory syndrome epidemic in 2003, the Taiwan government has established a central command system for a quick response to epidemics arising from China (1). Since the first confirmed case of coronavirus disease (COVID-19) in Taiwan was reported, Taiwan officials acted immediately with regard to border control, public health education (mask wearing and handwashing), ensuring adequate medical equipment, and early suspension of classes. These policies may not only reduce the spread of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) but may also have similar effects on spread of other infectious diseases (2,3). Using nationwide weekly surveillance data (4), we compared the activity of common infections during 2015–2020 with the timeline of actions and policies implemented to protect against spread of SARS-CoV-2 in Taiwan.
The Taiwan National infectious Disease Statistics System (4) from the Taiwan Centers for Disease Control monitors emergency and outpatient visits for patients with acute infections, diagnosed according to clinical manifestations and laboratory results in 181 hospitals (covering 97.5% of emergency visits), through the National Health Insurance database and reports weekly statistical data. Using these data, we compared the number of outpatient visits for influenza, pneumonia, enterovirus infection, and scarlet fever and the number of confirmed cases of severe complicated influenza in the 2019–20 influenza season (week 40 in 2019 through week 18 in 2020; 1,931,471 cases) versus the same data for the 5 previous influenza seasons (10,688,851 total cases).
To estimate the change in outpatient visits or confirmed case numbers (hereafter called activity) after the COVID-19 outbreak (weeks 1–18 in 2020), we used a difference-in-difference regression model. The model included a categorical variable for each week, a categorical variable for each year, and the interaction variables for each week after the outbreak and for the 2019–20 season. Because of concerns about the COVID-19 pandemic, during the first quarter of 2020, the overall number of hospital visits in Taiwan dropped by 14%. We conducted a sensitivity analysis by multiplying 1/(1 – 0.14) times the number of cases for the 5 selected diseases during these periods. Institutional board review was not required because we used only deidentified, secondary statistical data for this study.
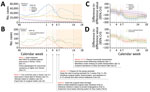
Overall infection activity was lower during the 2019–20 season than during the 5 previous seasons. For the 2019–20 season, activities of all 5 diseases notably decreased after weeks 6–7 (Figure). According to the difference-in-difference analysis, activities of influenza and severe complicated influenza were significantly lower after week 7 during the 2019–20 season than during the 5 previous seasons. Comparing the 2019–20 season with the 5 previous seasons, outpatient pneumonia activity was lower after week 8, enterovirus activity after week 16, and scarlet fever activity after week 10 (Table; Figure).
In Taiwan, infection rates for 5 selected diseases were lower in 2020 than in previous seasons. This observation correlates with implementation of actions and policies against COVID-19, such as early vigilance and taking proactive measures to prevent droplet and contact transmission in public and at schools. The effect of social distancing in Taiwan was unclear because related measures were not officially announced until the COVID-19 pandemic started subsiding in early April (4). These policies potentially have indirect effects on noninfectious diseases associated with acute viral infections, such as myocardial infarction and ischemic stroke (5,6). By comparing the cost of SARS-CoV-2 prevention and the effect on the economy and health during the pandemic in Taiwan and other areas, we could evaluate the cost-effectiveness of these measures and use this information to develop policies for future disease control.
Dr. Lee is a postdoctoral fellow in the Department of Radiology, New York University School of Medicine. His research focuses on retrieving microstructural information of the human brain via diffusion magnetic resonance imaging techniques, segmentation and analysis of microscopy data in the brain white matter, Monte Carlo simulation of diffusion in realistic tissue microgeometry, and the medical imaging processing pipeline.
References
- Wang CJ, Ng CY, Brook RH. Response to COVID-19 in Taiwan: big data analytics, new technology, and proactive testing. JAMA. 2020;323:1341. DOIPubMedGoogle Scholar
- Sakamoto H, Ishikane M, Ueda P. Seasonal influenza activity during the SARS-CoV-2 outbreak in Japan. JAMA. 2020;323:1969. DOIPubMedGoogle Scholar
- Kuo SC, Shih SM, Chien LH, Hsiung CA. Collateral benefit of COVID-19 control measures on influenza activity, Taiwan. Emerg Infect Dis. 2020;26:1928–30. DOIPubMedGoogle Scholar
- Taiwan Centers for Disease Control. Taiwan National Infectious Disease Statistics System [cited 2020 Jul 5]. https://nidss.cdc.gov.tw
- Vardeny O, Madjid M, Solomon SD. Applying the lessons of influenza to coronavirus during a time of uncertainty. Circulation. 2020;141:1667–9. DOIPubMedGoogle Scholar
- Lindsberg PJ, Grau AJ. Inflammation and infections as risk factors for ischemic stroke. Stroke. 2003;34:2518–32. DOIPubMedGoogle Scholar
Figure
Table
Cite This ArticleOriginal Publication Date: July 30, 2020
Table of Contents – Volume 26, Number 10—October 2020
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Sheng-Hsuan Lin, Assembly Building I, 1001 University Rd, Institute of Statistics, National Chiao Tung University, Hsinchu 30010, Taiwan
Top