Volume 27, Number 6—June 2021
Research Letter
Atypical Brucella inopinata–Like Species in 2 Marine Toads
Cite This Article
Citation for Media
Abstract
We describe the isolation of atypical Brucella inopinata–like species and unique clinicopathologic findings in 2 adult marine toads (Rhinella marina), including oophoritis in 1 toad. These findings represent a novel emerging disease in toads and a possible zoonotic pathogen.
Brucellosis is a worldwide zoonosis caused by gram-negative, intracellular Brucella coccobacilli. Expanding from 6 species classically associated with abortion in mammals (B. melitensis, B. suis, B. abortus, B. ovis, B. canis, and B. neotomae), the genus now includes novel strains from marine mammals (B. ceti, B. pinnipedialis), baboons (B. papionis), and foxes (B. vulpis). Two of these (B. ceti, B. pinnipedialis) are also considered atypical Brucella species similar to B. microti and B. inopinata (1). Atypical Brucella lesions in humans, wild mammals, amphibians, and fish range from localized manifestations to systemic infection with high death rates (2–8); however, reproductive lesions more typical of mammalian brucellosis are rare in amphibians. Previous reports of Brucella in amphibians have also included asymptomatic infections, suggesting that Brucella may be a commensal microorganism or opportunistic pathogen (9). The precise epidemiology, pathogenesis, and zoonotic potential of Brucella in amphibians remains largely unknown. We report atypical Brucella infection in 2 marine toads.
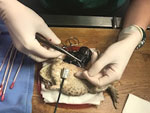
Cases 1 and 2 originated from the same captive breeding marine toad (Rhinella marina) colony; the 2 toads cohabited before toad 1’s transfer to a different zoological institution, resulting in a 4-year period with no contact before death. Case 1 was in an adult female marine toad with a 1.5-cm subcutaneous mass near the parotid gland. A second mass was palpated within the coelom, and ultrasound suggested ovarian origin. The toad was anesthetized for exploratory celiotomy, and both masses were excised and submitted for histopathology and culture. The coelomic mass was encapsulated within the left ovary, measured 3 × 2 × 2 cm, and contained purulent material (Figure). Histologically, the masses contained multifocal regions of necrosis and amorphous eosinophilic material with sheets of macrophages containing numerous intracytoplasmic, gram-negative, non–acid-fast coccobacilli (Appendix Figure). Diagnosis led to euthanasia; postmortem findings included mild coelomic effusion, lymphohistiocytic pericarditis, and fibrinous peritonitis. Case 2 was in an adult male marine toad, which was submitted for necropsy after being found dead in its enclosure. The toad was in poor body condition with no other lesions found on gross and histologic examination.
We used fresh ovarian tissue from the female toad and pooled fresh tissues (liver, kidney, and spleen) from the male toad for bacterial culture. We incubated duplicate culture plates at 37°C with 5% CO2 and in ambient conditions (21 + 2°C, no CO2). After 24 hours of ovarian mass culture incubation, we observed numerous pure bacterial colonies on blood and MacConkey agar at both 37°C and ambient conditions (colony size was smaller at ambient temperature). The pooled samples from the male toad contained mixed bacterial cultures after 24 hours of incubation. We identified the bacterial colony from the female toad with matrix-assisted laser desorption ionization-time of flight mass spectrometry (Microflex LT; Bruker Daltonics, https://www.bruker.com) as Brucella sp. (isolate no. 3278), whereas we identified bacterial colonies from the male toad as Brucella sp. (isolate no. 5043). Both Brucella isolates grew on MacConkey, Thayer-Martin, and blood agar at both 37°C and ambient conditions. The isolates were positive for catalase, oxidase, urease (<5 min), and hydrogen sulfide production and negative on gel formation test (Appendix). We used the DNA from isolates 3278 and 5043 for the Brucella Laboratory Response Network real-time PCR; the DNA tested positive for all 3 targets. We performed partial 16S rDNA PCR assays on isolates 3278 and 5048 and partial recA PCR on isolate 3278. For both isolates, the 16s rDNA sequences had 100% sequence similarity to an atypical Brucella sp. isolated from a big-eyed tree frog in Germany (GenBank accession no. HE608873) (5). The sequences from both isolates had only 95% coverage and 99.8% sequence similarity to B. inopinata strain BO1 (GenBank accession no. NR116161) (10). The recA sequence of isolate 3278 had 100% sequence similarity to the Brucella sp. isolated from a big-eyed tree frog (GenBank accession no. HE608874). The recA sequence had only 64% coverage and 98.71% sequence similarity to B. inopinata strain BO1 (GenBank accession no. FM177719). We submitted the DNA sequences from isolates 3278 and 5043 to GenBank (accession nos. MT471347, MT471348, and MT482342).
We isolated atypical Brucella inopinata–like sp. from 2 adult marine toads, one an asymptomatic carrier and the second with oophoritis, a classic lesion described in mammalian Brucella infections. Our results suggest that marine toads are another amphibian species susceptible to atypical Brucella bacteria and that infection can result in long-term asymptomatic carriers as well as more typical reproductive lesions. Furthermore, this organism was isolated in 2 toads from different zoological institutions but with identical origin, suggesting that infection originated from a common source at least 4 years previously. After leaving the breeding colony, all toads were housed only with conspecifics and, for a short period of time, with one other species group. Skin swab specimens from all other contacted amphibians at the zoos tested negative for Brucella. Diet consisted of a variety of insect species, making 2 separate introductions of Brucella from an outside source possible but unlikely. These findings highlight the need for additional testing of atypical Brucella spp., a potential emerging disease in amphibians, and warrants precautions when handling amphibians because of the potential for zoonoses.
Dr. Glabman is a veterinary anatomic pathologist and PhD candidate at the National Cancer Institute, Center for Cancer Research, at the National Institutes of Health in Bethesda, Maryland, in partnership with Michigan State University. Her primary research interests include comparative and investigative pathology of human and animal models of disease.
Acknowledgment
We thank the staff at the Binder Park and John Ball Zoo and Amy Hill, Victoria Watson, and Michelle Magagna.
References
- Al Dahouk S, Köhler S, Occhialini A, Jiménez de Bagüés MP, Hammerl JA, Eisenberg T, et al. Brucella spp. of amphibians comprise genomically diverse motile strains competent for replication in macrophages and survival in mammalian hosts. Sci Rep. 2017;7:44420. DOIPubMedGoogle Scholar
- Fischer D, Lorenz N, Heuser W, Kämpfer P, Scholz HC, Lierz M. Abscesses associated with a Brucella inopinata-like bacterium in a big-eyed tree frog (Leptopelis vermiculatus). J Zoo Wildl Med. 2012;43:625–8. DOIPubMedGoogle Scholar
- Eisenberg T, Hamann HP, Kaim U, Schlez K, Seeger H, Schauerte N, et al. Isolation of potentially novel Brucella spp. from frogs. Appl Environ Microbiol. 2012;78:3753–5. DOIPubMedGoogle Scholar
- Whatmore AM, Dale E, Stubberfield E, Muchowski J, Koylass M, Dawson C, et al. Isolation of Brucella from a White’s tree frog (Litoria caerulea). JMM Case Rep. 2015;2:1–5. DOIGoogle Scholar
- Soler-Lloréns PF, Quance CR, Lawhon SD, Stuber TP, Edwards JF, Ficht TA, et al. A Brucella spp. isolate from a Pac-Man frog (Ceratophrys ornata) reveals characteristics departing from classical Brucellae. Front Cell Infect Microbiol. 2016;6:116. DOIPubMedGoogle Scholar
- Scholz HC, Mühldorfer K, Shilton C, Benedict S, Whatmore AM, Blom J, et al. The change of a medically important genus: worldwide occurrence of genetically diverse novel Brucella species in exotic frogs. PLoS One. 2016;11:
e0168872 . DOIPubMedGoogle Scholar - Shilton CM, Brown GP, Benedict S, Shine R. Spinal arthropathy associated with Ochrobactrum anthropi in free-ranging cane toads (Chaunus [Bufo] marinus) in Australia. Vet Pathol. 2008;45:85–94. DOIPubMedGoogle Scholar
- Helmick KE, Garner MM, Rhyan J, Bradway D. Clinicopathologic features of infection with novel Brucella organisms in captive waxy tree frogs (Phyllomeduca sauvagii) and Colorado river toads (Incilius alvarius). J Zoo Wildl Med. 2018;49:153–61. DOIPubMedGoogle Scholar
- Mühldorfer K, Wibbelt G, Szentiks CA, Fischer D, Scholz HC, Zschöck M, et al. The role of ‘atypical’ Brucella in amphibians: are we facing novel emerging pathogens? J Appl Microbiol. 2017;122:40–53. DOIPubMedGoogle Scholar
- De BK, Stauffer L, Koylass MS, Sharp SE, Gee JE, Helsel LO, et al. Novel Brucella strain (BO1) associated with a prosthetic breast implant infection. J Clin Microbiol. 2008;46:43–9. DOIPubMedGoogle Scholar
Figure
Cite This ArticleOriginal Publication Date: May 07, 2021
Table of Contents – Volume 27, Number 6—June 2021
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Dalen Agnew, Michigan State University Veterinary Diagnostic Laboratory, 4125 Beaumont Road, Lansing, MI 48910
Top