Volume 28, Supplement—December 2022
SUPPLEMENT ISSUE
Workforce
COVID-19 Response Roles among CDC International Public Health Emergency Management Fellowship Graduates
Cite This Article
Citation for Media
Abstract
Since 2013, the US Centers for Disease Control and Prevention has offered the Public Health Emergency Management Fellowship to health professionals from around the world. The goal of this program is to build an international workforce to establish public health emergency management programs and operations centers in participating countries. In March 2021, all 141 graduates of the fellowship program were invited to complete a web survey designed to examine their job roles and functions, assess their contributions to their country’s COVID-19 response, and identify needs for technical assistance to strengthen national preparedness and response systems. Of 141 fellows, 89 successfully completed the survey. Findings showed that fellowship graduates served key roles in COVID-19 response in many countries, used skills they gained from the fellowship, and desired continuing engagement between the Centers for Disease Control and Prevention and fellowship alumni to strengthen the community of practice for international public health emergency management.
Public health emergencies originating from outbreaks of emerging infectious diseases have fueled the need for countries to develop their capacities to prevent, detect, and respond to public health threats (1–6). To manage responses to these threats, countries around the world, beginning in about 2012, began to establish public health emergency operations centers (PHEOCs) (7). PHEOCs serve as command centers for coordinating various functions of health emergency responses, such as information management, risk communications, logistics, and operations (7,8). Establishing PHEOCs introduced the need for trained personnel to manage and operate these facilities. In 2013, the US Centers for Disease Control and Prevention (CDC) responded to this need by establishing the Public Health Emergency Management (PHEM) Fellowship program (https://www.cdc.gov/cpr/eoc/EmergencyManagementFellowship.htm) to help build a workforce to strengthen emergency management capacity among international public health communities (9–11). The PHEM Fellowship program trains international midcareer public health professionals in emergency management principles using a competency-based curriculum that incorporates lectures, case studies, and participation in real-world experiences. As of 2020, CDC had trained 141 fellows, representing 36 countries worldwide, in 12 semiannual cohorts conducted during August 2013–May 2020.
The magnitude of the COVID-19 pandemic highlighted the need in many countries for experts with public health emergency management skills to organize, lead, and streamline response efforts. Although anecdotes from the field demonstrated notable roles by PHEM Fellowship program graduates in providing emergency management leadership in COVID-19 response efforts, details of their roles and skills had not been systematically captured. Also, although some fellowship alumni have requested remote technical guidance during the COVID-19 pandemic, the type and extent of technical assistance needed had not been systematically surveyed. Identifying COVID-19 response roles and remaining training needs of PHEM Fellowship graduates can inform curriculum development for future training activities.
To quantify program graduates’ contributions during COVID-19 and training and assistance needs, CDC staff, in 2021, designed and administered a survey. The objectives of the survey were to assess the number and proportion of total graduates engaged in COVID-19 response in the public health emergency management system in the respondent’s country; identify the organizations served and positions filled by graduates within the country’s public health emergency management system before and during the COVID-19 response; identify public health emergency response skills acquired through the PHEM Fellowship program that the respondent considered useful after graduation; identify additional technical skills related to public health emergency management needed to sustain the COVID-19 response; and identify modes of technical assistance support (remote or onsite) preferred by graduates.
We developed a 21-question web-based survey that could be answered in 10–15 minutes designed to address the 5 survey objectives (Appendix). We analyzed responses grouped by semiannual cohort (n = 12) and region. On March 20, 2021, we sent an email with a secure link to the survey to all persons who had graduated from the PHEM Fellowship program by that date (n = 141). The survey remained open for 5 weeks; reminder emails were sent 2 and 4 weeks after the initial mailing. CDC reviewed the activity and determined that it did not involve human subject research and therefore did not require Institutional Review Board approval.
The survey collected deidentified information on respondents’ countries, roles, graduation month and year (cohort), and organization type of current and any previous employment. Survey questions required multiple-choice, multiple-answer, free text, or 5-point Likert scale responses (12). We created the survey in the Epi-Info Secure Web Survey tool (https://www.cdc.gov/epiinfo/index.html) and included relevant skip patterns to simplify entry for respondents. We used the number of graduates of the PHEM Fellowship program from each country and cohort to determine the expected number of responses, then compared those to survey responses to identify and remove duplicates.
Once the survey closed, we combined French and English responses based on common data elements, then cleaned and analyzed the data using Epi Info and Microsoft Power BI (https://powerbi.microsoft.com). We calculated response rates using standard definitions (13). We calculated 95% CIs around percentages with the finite population correction factor for known population size (n = 141 graduates). To examine differences by region, we organized respondents by their corresponding World Health Organization (WHO) regional offices (Table 1).
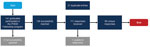
We successfully reached 136/141 (96.5%) PHEM Fellowship program graduates. Overall, respondents submitted 111 completed surveys; 21 were duplicates, and 1 did not include country name and cohort (Figure). Duplicates were most likely to occur right after the respondent’s first submission or shortly after reminder emails were distributed. After excluding duplicates and the 1 incomplete response, we analyzed data from the remaining 89 surveys, a response rate of 74.2% (13). Respondents from WPRO (Western Pacific Regional Office) countries had a 42.9% response rate, lower than those for other WHO regions: AFRO (Africa), 77.5%; SEARO (South-East Asia), 91.7%; EMRO (Eastern Mediterranean), 100%; and EURO (Europe), 100%. There were no PHEM Fellowship program graduates from the Americas at the time the survey was conducted. Overall, the first 2 cohorts had lower response rates (0% for cohort 1 and 14.3% for cohort 2) and cohort 10 had a higher response rate (93.8%) than those for the other groups combined. The distribution of survey participants by WHO region was similar to the overall distribution of total fellowship participants by region (Table 1). We analyzed the survey data to assess the 5 predetermined survey objectives.
Objective 1: Assess Number and Proportion of Graduates Engaged in the Country’s PHEM System during the COVID-19 Response
Overall, 80/89 (89.9%) survey respondents have supported their country’s COVID-19 response in various PHEM roles. At the time of the survey, 49/89 (55.1%) respondents had spent 76%–100% of their work time on emergency preparedness or response activities for COVID-19 or any other public health emergency; 17 (19.1%) had spent 51%–75%, 10 (11.2%) had spent 26%–50%, 6 (6.7%) had spent 1%–25%, and 1 (1.1%) had spent no time on these activities. Of the 62 respondents from AFRO, 35 (56.5%) had spent 76%–100% of their time working on emergency management preparedness or response activities, compared with 2/5 (40.0%) EMRO respondents, 4/11 (36.4%) SEARO respondents, and 7/9 (77.8%) WPRO respondents.
Objective 2: Identify Organizations and Positions of Graduates in the Country’s Emergency Management System before the PHEM Fellowship and during the COVID-19 Response
The 89 respondents reported diverse professional backgrounds, and many had served in several different positions before participating in the PHEM Fellowship program. More respondents (n = 60, 67.4%) worked for the country’s ministry of health than any other organization type. During the COVID-19 pandemic, more respondents reported engaging in emergency response functions after graduating from the fellowship program than before. More than half (n = 47, 52.8%) served in managerial or nonmanagerial roles in emergency operations centers to support COVID-19 and other public health responses (Table 2). Among respondents, 80/89 (89.9%) supported the COVID-19 response in a variety of traditional incident management system (IMS) functional roles as incident managers or in operations, planning, or logistics support (Table 3). Most respondents reported being involved in COVID-19–related scientific technical assistance (n = 38, 47.5%) or planning (n = 34, 42.5%).
Objective 3: Identify Public Health Emergency Response Skills Acquired through the PHEM Fellowship that Have Been Useful after Graduation
Among respondents, 81/89 (91.0%) indicated they had used >1 specific emergency management skill in the context of COVID-19 and other public health emergencies since graduating from the fellowship program. Among respondents, 97.4% agreed that the fellowship program had provided useful training skills in IMS, coordination, and communication; 96.5% in developing policies, plans, and procedures; 97.5% in preparedness, exercises, and evaluation; and 93.3% in other emergency management skills. Of 19 public health emergency management skills detailed in the survey, respondents reported performing a median of 13 (interquartile range 9–18); 16 respondents reported performing 18/19 skills. When asked about their confidence in performing those skills, 79.9% felt confident performing tasks associated with IMS, coordination, and communication; 69.3% felt confident developing emergency response policies, plans, and procedures; and 73.9% felt confident in their skills for preparedness, exercises, and evaluation (Table 3).
Objective 4: Identify Current Technical Needs Related to Emergency Management that Are Critical to the COVID-19 Response
To address COVID-19 response needs, 65/89 respondents (73.0%) requested >1 type of technical support from CDC emergency management specialists. Among the 65 respondents that requested emergency management technical support, 57 (87.7%) requested general support for workforce development in their country, 35 (53.8%) technical support to develop plans and standard operating procedures, 30 (46.2%) support on the PHEOC physical infrastructure, 31 (47.6%) technical support on rapid-response training, and 31 (47.7%) technical support on exercises related to developing, executing, and evaluating responses.
Objective 5: Identify Methods of Technical Assistance Desired by Graduates
Among respondents from all cohorts and regions, 73/89 (82.0%) said they would participate in additional PHEM training opportunities, among whom 49/73 (67.1%) preferred a combination of in-person and virtual training modalities, 17 (23.3%) preferred in-person training, 6 (8.2%) virtual training; 1 person (1.4%) did not answer that question. Capacity development support between graduates was common. Among respondents from all cohorts and regions, 55 (61.8%) indicated they had either provided support to or received support from other PHEM fellowship program graduates, 18 (20.2%) had not given or received support, and 16 (18.0%) did not answer that question; 63 respondents (70.8%) said they would be willing to present in future PHEM trainings.
This survey provided information on how participation in the PHEM Fellowship program contributed to improving international workforce capacity to manage public health emergencies. The PHEM Fellowship program provides standard training and mentorship and networking components that enable countries to build systems unique to their needs and context. Nearly 90% of respondents indicated that they held a role in their country’s COVID-19 response, demonstrating the relevance of a trained public health emergency management workforce during emergencies. Program graduates credited the fellowship with developing skills essential for public health emergency management, including conducting risk assessments, developing response plans, aiding with training and exercises, and managing resources, and most expressed interest in sharing their experiences.
PHEM fellowship program graduates are likely more culturally aware of local politics, resources, languages, and challenges than are US-based experts. Anecdotal examples from the survey of initiatives by graduates in the field included conducting reciprocal site visits between Uganda and Sierra Leone to observe how other nations operate their PHEOCs and providing technical assistance (e.g., Cameroon supporting the Democratic Republic of the Congo by sharing risk assessment and response plans). Other opportunities for in-depth, longitudinal relationship management with PHEM graduates are likely and could be modeled after the alumni engagement networks of other CDC training programs.
All data were self-reported and therefore possibly subject to biases that tend toward overestimates. Respondents might have been more likely to rate their skills and confidence more positively (social desirability bias) and attribute skills gained from a CDC program more highly on a survey conducted by CDC (acquiescence bias) (14). Several factors might have suppressed the overall response rate, including differences in language understanding and perception, length of time since participation in the fellowship, lack of time because of engagement in the COVID-19 response, or incorrect contact information. Regions such as WPRO were underrepresented in survey responses compared with AFRO, which could affect generalizability of the results and subsequent programmatic recommendations.
Overall, our findings indicated that fellowship graduates served key roles in country COVID-19 responses, used skills gained from participating in the fellowship, and desired ongoing engagement between CDC and fellowship alumni to continue strengthening the community of practice for international public health emergency management. Investments in this program could address the growing demand for public health emergency responders with the expertise to combat future epidemics and pandemics (15,16). Response needs prompted by the COVID-19 pandemic have increased interest from more countries and regions to provide applicants to future fellowship cohorts (CDC PHEM Fellowship Program, unpub. data).
Strong investments in building international workforce capacity should combine time-limited intensive in-person learning with ongoing mentorship and cultivated alumni networks. CDC is working to expand the fellowship’s curriculum, develop advanced training opportunities, and translate materials into additional languages. The goal of these training improvements and advancement of peer-to-peer mentoring is to continue strengthening international public health emergency management workforce capacity. Using a combination of virtual and in-person trainings, peer-to-peer learning, and sharing best practices can strengthen the nascent global network of fellowship graduates and other public health emergency management experts. As the field of public health emergency management continues to advance, systematic evaluations are needed to understand how best to support PHEM fellowship program graduates and identify strengths and gaps of the program at large. CDC is developing an evaluation framework and evaluation plan to address this need.
CDR. Krishnan of the US Public Health Service, an emergency management specialist in CDC’s Center for Preparedness and Response, Division of Emergency Operations, provides training and technical assistance on public health emergency management to ministries of health in Indonesia, Bangladesh, India, Burkina Faso, Cote D’Ivoire, Thailand, and Zambia. She is also an instructor in CDC’s Public Health Emergency Management Fellowship program.
Acknowledgment
The authors thank the following staff members of the Centers for Disease Control and Prevention for their contributions to the survey underlying this manuscript: Kerre Avery, Shivani Dama, Ashley L. Greiner, Eric Marble, Wilton (Chuck) Menchion, Mike Phipps, and Mays Shamout.
References
- Redd SC, Frieden TR. CDC’s evolving approach to emergency response. Health Secur. 2017;15:41–52. DOIPubMedGoogle Scholar
- Rico A, Sanders CA, Broughton AS, Andrews M, Bader FA, Maples DL. CDC’s emergency management program activities—worldwide, 2013–2018. MMWR Morb Mortal Wkly Rep. 2021;70:36–9. DOIPubMedGoogle Scholar
- Papagiotas SS, Frank M, Bruce S, Posid JM. From SARS to 2009 H1N1 influenza: the evolution of a public health incident management system at CDC. Public Health Rep. 2012;127:267–74. DOIPubMedGoogle Scholar
- Frieden TR, Damon IK. Ebola in west Africa—CDC’s role in epidemic detection, control, and prevention. Emerg Infect Dis. 2015;21:1897–905. DOIPubMedGoogle Scholar
- Redd SC, Frieden TR, Schuchat A, Briss PA. 1918 and 2009: a tale of two pandemics. Public Health Rep. 2010;125(Suppl 3):3–5. DOIGoogle Scholar
- Fitzmaurice AG, Mahar M, Moriarty LF, Bartee M, Hirai M, Li W, et al.; GHSA Implementation Group. Contributions of the US Centers for Disease Control and Prevention in implementing the global health security agenda in 17 partner countries. Emerg Infect Dis. 2017;23:S15–24. DOIPubMedGoogle Scholar
- World Health Organization. Framework for a public health emergency operations centre [cited 2022 Sep 12]. https://www.who.int/publications/i/item/framework-for-a-public-health-emergency-operations-centre
- Rose DA, Murthy S, Brooks J, Bryant J. The evolution of public health emergency management as a field of practice. Am J Public Health. 2017;107(S2):S126–33. DOIPubMedGoogle Scholar
- Greiner AL, Stehling-Ariza T, Bugli D, Hoffman A, Giese C, Moorhouse L, et al. Challenges in public health response team management. Health Secur. 2020;18(S1):S8–13. DOIPubMedGoogle Scholar
- Balajee SA, Pasi OG, Etoundi AGM, Rzeszotarski P, Do TT, Hennessee I, et al. Sustainable model for public health emergency operations centers for global settings. Emerg Infect Dis. 2017;23:S190–5. DOIPubMedGoogle Scholar
- Brencic DJ, Pinto M, Gill A, Kinzer MH, Hernandez L, Pasi OG. CDC support for global public health emergency management. Emerg Infect Dis. 2017;23:S183–9. DOIPubMedGoogle Scholar
- Likert R. A technique for the measurement of attitudes. Arch Psychol. 1932;22:55.
- American Association for Public Opinion Research. 2016. Standard definitions: final dispositions of case codes and outcome rates for surveys, 9th edition [cited 2022 Sep 12]. https://www.aapor.org/AAPOR_Main/media/publications/Standard-Definitions20169theditionfinal.pdf
- Moorman RH, Podsakoff PM. A meta-analytic review and empirical test of the potential confounding effects of social desirability response sets in organizational behaviour research. J Occup Organ Psychol. 1992;65:131–49. DOIGoogle Scholar
- Clara A, Dao ATP, Tran Q, Tran PD, Dang TQ, Nguyen HT, et al. Testing early warning and response systems through a full-scale exercise in Vietnam. BMC Public Health. 2021;21(1):409. DOIGoogle Scholar
- World Health Organization. Global strategy on human resources for health: Workforce 2030 [cited 2022 Sep 12]. https://www.who.int/publications/i/item/9789241511131
Figure
Tables
Cite This ArticleOriginal Publication Date: December 09, 2022
Table of Contents – Volume 28, Supplement—December 2022
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Sharanya Krishnan, Centers for Disease Control and Prevention, 1600 Clifton Rd NE, Mailstop D-75, Atlanta, GA 30329-4027, USA
Top