Volume 28, Number 7—July 2022
Research Letter
Strongyloides Hyperinfection Syndrome among COVID-19 Patients Treated with Corticosteroids
Cite This Article
Citation for Media
Abstract
Widespread use of corticosteroids for COVID-19 treatment has led to Strongyloides reactivation and severe disease in patients from endemic areas. We describe a US patient with COVID-19 and Strongyloides hyperinfection syndrome and review other reported cases. Our findings highlight the need for Strongyloides screening and treatment in high-risk populations.
Strongyloidiasis is caused by the soil-transmitted helminth Strongyloides stercoralis and affects ≈613.8 million persons worldwide (1). S. stercoralis infections can be asymptomatic or chronic or can cause life-threatening larva dissemination, especially in immunocompromised patients (2).
Among COVID-19 patients, dexamethasone is the standard treatment for persons requiring supplemental oxygen, but among persons from Strongyloides-endemic areas, exposure to corticosteroids can cause life-threatening S. stercoralis hyperinfection (3). We describe a case of Strongyloides hyperinfection syndrome in a COVID-19 patient and review other reported cases.
A 63-year-old man, who was originally from Cambodia, was admitted to a hospital in Central Valley, California, USA, for a 4-day history of fever, cough, and respiratory distress. His medical history included diabetes mellitus and alcohol use disorder. Admission laboratory testing showed a leukocyte count of 8,500 cells/μL (absolute lymphocyte count 660 cells/μL, reference range 800–4,800 cells/μL) and absolute eosinophil count of 0 cells/μL (reference range 0–800 cells/μL). A nasopharyngeal swab sample tested SARS-CoV-2–positive by PCR. Chest radiographs showed patchy bilateral airspace consolidations. By day 5 of hospitalization, the patient’s respiratory failure worsened, and he required supplemental oxygen via high-flow nasal cannula. Chest computed tomography imaging showed multifocal bilateral airspace opacities. The patient received intravenous dexamethasone (6 mg/d for 10 d); during the first 5 days of treatment, he also received baricitinib (10 mg 1×/d) and remdesivir (100 mg/d). The patient’s respiratory status improved, and he was discharged to a skilled nursing facility.
The patient returned to the hospital 6 days later with respiratory failure and altered mental status. He was febrile (temperature 39°C) and hypoxic and required intubation. Blood tests revealed a leukocyte of 5,300 cells/μL (absolute lymphocyte count 1,000 cells/μL) and absolute eosinophil count of 100 cells/μL. Blood and sputum cultures were positive for methicillin-sensitive Staphylococcus aureus, and we initiated intravenous cefazolin (2 g every 8 h for 10 d). The patient transiently improved, but then fever developed and persisted. After 10 days of broad-spectrum antimicrobial drug therapy, the patient’s blood cultures were negative. Echocardiography, magnetic resonance imaging, and computed tomography scans did not identify a focus of infection.
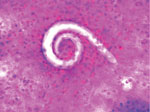
Because of the patient’s continued fever and worsening respiratory failure, we performed a diagnostic bronchoscopy on day 28 of his illness. Microscopic examination of the bronchoalveolar lavage fluid revealed parasitic worms consistent with Strongyloides spp. (Figure). Stool samples were negative for parasites, but Strongyloides serum IgG was positive. The patient’s absolute eosinophil count increased to 1,500 cells/μL, and we began oral ivermectin (200 µg/kg for 14 d).
Subsequent respiratory culture was positive for extended spectrum β-lactamase Escherichia coli. The patient continued to have encephalopathy, and we recommended a lumbar puncture, but the procedure was not performed because of his hemodynamic instability. We changed the patient’s therapy to intravenous meropenem (2 g every 8 h), but his condition did not improve. He was eventually transitioned to comfort care and died.
S. stercoralis parasites are endemic in tropical and subtropical regions, but data on strongyloidiasis prevalence is likely underreported, even in endemic areas (1). Patients can develop chronic S. stercoralis infection, but an immunocompetent host’s immune system can regulate infection by controlling adult worm population density in the intestines. However, when a host becomes immunocompromised, larval migration to organs can increase during the autoinfection cycle, causing Strongyloides hyperinfection syndrome. Exposure to corticosteroids, human T-cell leukemia virus type 1 co-infection, and solid organ transplantation can increase risk for Strongyloides hyperinfection syndrome (2). Dexamethasone is the standard treatment for COVID-19 patients who require oxygen therapy; other immunosuppressive agents, including interleukin-6 inhibitors such as tocilizumab, also are commonly used.
Other strongyloidiasis cases have been reported in COVID-19 patients (4–9) (Table). Strongyloides hyperinfection syndrome can cause signs and symptoms similar to those of severe COVID-19, including fever, chills, dyspnea, gastrointestinal symptoms, and rash. These vague symptoms can cause missed or delayed strongyloidiasis diagnosis, demonstrating the need for increased awareness of this condition and systematic screening of high-risk patients.
Algorithms to aid clinicians with risk assessment, screening, and treatment for Strongyloides infection in COVID-19 patients have been proposed (10). Strongyloides hyperinfection syndrome should be included in the differential diagnosis for patients from endemic areas who receive dexamethasone for COVID-19 and experience clinical decompensation, especially with gram-negative rod bacteremia, pneumonia, or meningitis. Serologic testing should be performed simultaneously and should not delay treatment. Presumptive oral ivermectin for 1–2 days can be considered for COVID-19 patients with higher risk for strongyloidiasis who need dexamethasone (10).
Chronic peripheral eosinophilia can be a marker for prompt Strongyloides screening. Several case studies have shown a pattern of initial eosinopenia in patients with chronic strongyloidiasis and COVID-19 suppressed with corticosteroids (4–6). Eosinophils became elevated in these patients because Strongyloides hyperinfection developed after corticosteroid administration. In some cases, eosinophilia improved with ivermectin treatment.
In conclusion, Strongyloides hyperinfection cases are rising in certain COVID-19 patients. Standardized protocols for Strongyloides screening and treatment are needed, especially for patients from endemic countries. To prevent this complication, clinicians should consider Strongyloides screening in COVID-19 patients from endemic areas who require corticosteroid treatment.
Dr. Kim is an infectious diseases fellow at the University of California San Francisco, Fresno, California. Her primary interests are HIV/AIDS and fungal infections.
References
- Buonfrate D, Bisanzio D, Giorli G, Odermatt P, Fürst T, Greenaway C, et al. The global prevalence of Strongyloides stercoralis infection. Pathogens. 2020;9:468. DOIPubMedGoogle Scholar
- Nutman TB. Human infection with Strongyloides stercoralis and other related Strongyloides species. Parasitology. 2017;144:263–73. DOIPubMedGoogle Scholar
- Pereira CVM, Mastandrea GRA, Medeiros ACCS, Gryschek RCB, Paula FM, Corral MA. COVID-19 and strongyloidiasis: what to expect from this coinfection? Clinics (São Paulo). 2021;76:
e3528 . DOIPubMedGoogle Scholar - Stylemans D, Van Cauwelaert S, D’Haenens A, Slabbynck H. COVID-19–associated eosinopenia in a patient with chronic eosinophilia due to chronic strongyloidiasis. Infect Dis Clin Pract (Baltim Md). 2021;29:e305–6. DOIPubMedGoogle Scholar
- Lier AJ, Tuan JJ, Davis MW, Paulson N, McManus D, Campbell S, et al. Case report: disseminated strongyloidiasis in a patient with COVID-19. Am J Trop Med Hyg. 2020;103:1590–2. DOIPubMedGoogle Scholar
- Marchese V, Crosato V, Gulletta M, Castelnuovo F, Cristini G, Matteelli A, et al. Strongyloides infection manifested during immunosuppressive therapy for SARS-CoV-2 pneumonia. Infection. 2021;49:539–42. DOIPubMedGoogle Scholar
- Gautam D, Gupta A, Meher A, Siddiqui F, Singhai A. Corticosteroids in Covid-19 pandemic have the potential to unearth hidden burden of strongyloidiasis. IDCases. 2021;25:
e01192 . DOIPubMedGoogle Scholar - Norman FF, Chamorro S, Braojos F, López-Miranda E, Chamorro J, González I, et al. Strongyloides in bronchoalveolar lavage fluid: practical implications in the COVID-19 era. J Travel Med. 2022;29: taab114 .
- Feria L, Torrado M, Anton-Vazquez V. Reactivation of Strongyloides stercoralis in patients with SARS-CoV-2 pneumonia receiving dexamethasone. Med Clin (Barc). 2022;158:242–3. DOIGoogle Scholar
- Stauffer WM, Alpern JD, Walker PF. COVID-19 and dexamethasone: a potential strategy to avoid steroid-related Strongyloides hyperinfection. JAMA. 2020;324:623–4. DOIPubMedGoogle Scholar
Figure
Table
Cite This ArticleOriginal Publication Date: June 09, 2022
Table of Contents – Volume 28, Number 7—July 2022
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Geetha Sivasubramanian, Division of Infectious Diseases, Department of Internal Medicine, University of California San Francisco, 155 N Fresno St, Ste 307, Fresno, CA 93701, USA
Top