Volume 28, Number 9—September 2022
Research
Revised Definitions of Tuberculosis Resistance and Treatment Outcomes, France, 2006–2019
Abstract
Definitions of resistance in multidrug-resistant tuberculosis (MDR TB) and extensively drug-resistant tuberculosis (XDR TB) have been updated. Pre–XDR TB, defined as MDR TB with additional resistance to fluoroquinolones, and XDR TB, with additional resistance to bedaquiline or linezolid, are frequently associated with treatment failure and toxicity. We retrospectively determined the effects of pre-XDR/XDR TB resistance on outcomes and safety of MDR TB treatment in France. The study included 298 patients treated for MDR TB at 3 reference centers during 2006–2019. Of those, 205 (68.8%) cases were fluoroquinolone-susceptible MDR TB and 93 (31.2%) were pre-XDR/XDR TB. Compared with fluoroquinolone-susceptible MDR TB, pre-XDR/XDR TB was associated with more cavitary lung lesions and bilateral disease and required longer treatment. Overall, 202 patients (67.8%) had favorable treatment outcomes, with no significant difference between pre-XDR/XDR TB (67.7%) and fluoroquinolone-susceptible MDR TB (67.8%; p = 0.99). Pre-XDR/XDR TB was not associated with higher risk for serious adverse events.
Rifampin-resistant tuberculosis (RR TB) and multidrug-resistant tuberculosis (MDR TB), defined as TB resistant to both rifampin and isoniazid, are a global public health threat. In 2019, there were 465,000 incident cases of RR TB, among which 78% were MDR TB (1). In France, the yearly incidence of MDR TB cases was stable at ≈50 cases during 2006–2010, dramatically increased in the next 4 years (2) to >100 cases in 2014 (3), and slightly decreased afterwards to 75 cases in 2019 (4).
RR/MDR TB cases are difficult to treat, and patients need prolonged treatment courses, which are burdened by frequent drug-related adverse events. Global treatment success for RR/MDR TB was 59% in 2018 (1). At that time, fluoroquinolones were considered the cornerstone of RR/MDR TB treatment. In 2018, the World Health Organization (WHO) published new treatment guidelines, relying on a large-scale meta-analysis (5), which revolutionized the traditional hierarchy of anti-TB drugs (6). In those guidelines, newer and repurposed drugs, such as bedaquiline and linezolid, were recommended for all MDR TB patients in addition to fluoroquinolones; second-line injectables would be reserved for cases where no other options are available.
Globally, 16.2% of RR/MDR TB isolates have acquired resistance to fluoroquinolones (1), indicating the need for an update in resistance definitions. Thus, in January 2021, WHO defined pre–extensively drug-resistant TB (pre-XDR TB) as MDR TB with additional resistance to fluoroquinolones, and XDR TB as pre-XDR TB with additional resistance to >1 additional group A drug (bedaquiline and linezolid as of July 2022) (7).
Resistance to fluoroquinolones is classically considered a risk factor for treatment failure (5,8,9). However, recent studies from countries with both low (10) and high (11) TB prevalence did not confirm this finding in high-income settings in which diagnostics and group A drugs are widely available. Furthermore, evidence on the effect of fluoroquinolone resistance on treatment safety is scarce (11).
We assessed whether pre-XDR TB and XDR TB status (i.e., additional resistance to any fluoroquinolone) affected outcomes and safety of MDR TB treatment for TB in France, a high-income, low TB incidence country. The Institutional Review Board of the Bligny Hospital (Briis-sous-Forges, France) granted ethical clearance (CRE 2021 08).
Study Design and Participants
In this retrospective observational cohort study, we included all consecutive MDR TB patients confirmed at the French National Reference Center for Mycobacteria (NRC; Paris, France) who initiated treatment at 3 referral hospitals (Bligny, in Briis-sous-Forges, and Pitié-Salpêtrière and Bichat-Claude Bernard, both in Paris) during January 1, 2006–December 31, 2019. Patients were followed up for 2 years after the end of treatment. We considered only the first episode of MDR TB within the study period. We retrieved the latest data on December 31, 2021.
We reviewed medical records to retrieve demographic and clinical features, as well as results of laboratory, radiographic, and microbiological tests. We extracted routinely collected data from medical records and anonymized the data; the investigator who extracted data was not involved in patient care. We obtained comprehensive drug susceptibility testing (DST) profiles from the database of the NRC laboratory.
Definitions
We performed phenotypic DST at the NRC using the Löwenstein–Jensen proportion method (12). We obtained genotypic DST through commercially available line-probe assays (GenoType MTBDRplus and GenoType MTBDRs; Hain Lifescience, https://www.hain-lifescience.de) or targeted DNA sequencing. We used new definitions of drug-resistant TB (7): we defined MDR TB as TB resistant to isoniazid and rifampin, pre-XDR TB as MDR TB with resistance to any fluoroquinolone, and XDR TB as MDR TB with additional resistance to any fluoroquinolone and another WHO group A drug (bedaquiline or linezolid). We classified patients as new or previously treated according to WHO definitions. Sputum smear and cultures were routinely performed at treatment start, every 14 days until culture conversion, and monthly thereafter. We defined sputum culture conversion as 2 consecutive negative cultures collected at least 30 days apart. We defined treatment outcomes using 2020 WHO definitions (13). Of note, we defined treatment outcome as not evaluated for patients for whom no treatment outcome was assigned; this definition includes cases transferred out to another treatment unit and those whose treatment outcome was unknown but excludes those who did not attend follow-up appointments and did not respond to attempted contact from clinical staff, which we categorized as lost to follow-up.
Treatment Regimens
Throughout the study period, treatment regimens were designed in accordance with WHO treatment guidelines and in consultation with the French MDR TB Consilium, a multidisciplinary team coordinated by the France NRC (14–17). Of note, linezolid has been used for MDR TB treatment in France since 2006 and bedaquiline since 2011. Drugs were considered to be part of the treatment regimen if they were administered for >30 days.
Outcomes
The primary study outcome was the proportion of treatment success (defined as the sum of cured and treatment completed). Secondary outcomes were time to sputum culture conversion and proportion of treatment-emergent serious adverse events (SAE), as defined by the US Food and Drug Administration (18).
Statistical Analysis
Sample Size
Based on NRC surveillance data for the period under review, we estimated that ≈300 MDR TB patients, 200 with fluoroquinolone-susceptible MDR TB and 100 with pre-XDR/XDR TB, could be included. Taking into account the results of a large meta-analysis comparing MDR TB treatment outcomes according to different resistance patterns (5), we estimated a relative risk of 1.59 for an unfavorable treatment outcome in pre-XDR/XDR TB compared with fluoroquinolone-susceptible MDR TB cases. With these assumptions, the expected sample size would provide a power of 93% with a 2-sided α risk of 2.5% to detect a difference between the 2 groups.
Statistical Methods
We collected the extracted data on standardized forms, entered them into a database located at the NRC, and ran analyses using Stata version 16 (StataCorp, https://www.stata.com). We performed sensitivity analyses focusing on patients treated after 2011, the year bedaquiline was introduced in France.
For descriptive statistics, we reported continuous variables as medians with interquartile range (IQR) and compared them using the Wilcoxon rank-sum test or 2-sample t-test, as appropriate. We reported categorical variables as frequencies with percentages and compared using the Fisher exact test or χ2 test, as appropriate. A 2-sided α<0.05 was considered statistically significant. Because the cohort included few XDR TB patients, we performed most analyses by grouping together pre-XDR TB and XDR TB cases.
To identify risk factors associated to the dependent categorical variables (treatment success and SAE), we fitted unconditional logistic regression models. We included explanatory variables in the initial models if associated with the dependent variable at p<0.20 in univariate analysis. We then performed backward analysis: we kept explanatory variables associated with the dependent variable that had p<0.20, in addition to the variable of interest (pre-XDR/XDR TB), in the model.
As secondary objectives, we performed survival analyses to describe time from treatment start to sputum culture conversion (for patients with positive sputum cultures at treatment start) and unfavorable treatment outcome (for all patients). We estimated Kaplan-Meier curves and performed log-rank tests to assess the effects of pre-XDR/XDR TB. We fitted multivariable Cox proportional-hazard models to identify predictive factors of sputum culture conversion. We included variables into multivariable Cox proportional hazards models if they predicted the outcome at p<0.20 in univariate analysis and if they fulfilled the proportional hazards assumption at baseline or, if appropriate, after addition of a time interaction. We reported hazard ratios with 95% CI.
For both logistic regression and Cox models, we performed complete case analyses to identify the variables included in the model and then imputed missing data with multiple imputation using chained equations with 10 imputed datasets. Overall, the proportion of missing observations in the included variables was 0%–9%.
Population Characteristics
The study population was made up of 298 MDR TB patients, including 84 (28.2%) with pre-XDR TB and 9 (3.0%) with XDR TB. Sixty-six patients (22.1%) were treated during 2006–2010 and 232 (77.9%) during 2011–2019. The median age at admission was 34 years (IQR 27–42), and 202 (67.8%) patients were male. Patients were mainly born in the WHO Europe region (54.6%) (Table 1). Pre-XDR/XDR TB patients were more frequently born in the WHO Europe region; had more frequently precarious housing, past imprisonment history, and active drug abuse (alcohol, smoking, intravenous drugs); and had more severe pulmonary tuberculosis, including cavitary lesions and bilateral disease. Patients with pre-XDR/XDR TB more frequently had additional resistance to cycloserine, second-line injectables, pyrazinamide, and P-aminosalicylic acid.
Treatment and Outcomes
Overall, 94.3% patients were treated with >1 group A drug (levofloxacin, moxifloxacin, bedaquiline, or linezolid) and 76.8% with >1 group B drug (clofazimine or cycloserine). Linezolid (89.3% vs. 69.8%, p<0.001) and bedaquiline (74.2% vs. 28.3%, p<0.001) were more frequently used in pre-XDR/XDR TB cases. A large part of our study population received second-line injectables (85.2%), including similar proportions in the 2 groups of interest (81.7% vs. 86.8%). Total treatment duration was longer in pre-XDR/XDR TB patients (median 21.2 months vs. 17.3 months; p<0.001) (Table 2).
Overall, 202 patients (67.8%) had treatment success, including cure (62.1%) and treatment completion (5.7%) (Table 3). Ninety-six patients (32.2%) had unfavorable or other outcomes. Of those, 3 patients had treatment failure and 5 died; 54 were lost to follow-up, and 34 did not have treatment outcomes evaluated (Table 3). Of note, 67.9% of patients with pre-XDR TB and 66.7% patients with XDR TB had treatment success. For the 5 patients who died during TB treatment, causes of death were malignancy progression (2 patients), septic shock (urinary tract sepsis for 1 patient and disseminated candidemia for 1 patient), and decompensated cirrhosis (1 patient). Among patients with treatment success, 145 (71.8%) were followed up to 12 months after end of treatment and 129 (63.9%) up to 24 months. Two patients with pre-XDR/XDR TB relapsed in the first year and 1 in the second year of follow-up after end of treatment. One patient with fluoroquinolone-susceptible MDR TB relapsed in the second year of follow-up.
Predictors of Treatment Outcome
Multivariable analysis showed that pre-XDR/XDR TB status was not independently associated with treatment outcome (adjusted odds ratio [aOR] 0.81, 95% CI 0.47–1.41); conversely, previous anti-TB treatment (aOR 1.80, 95% CI 1.13–2.89) and poor treatment adherence (aOR 1.19, 95% CI 1.07–1.33) were independently associated with unfavorable treatment outcome (Table 4). Multivariable Cox proportional hazard model for unfavorable outcome was consistent with these findings (Appendix Table 2). We confirmed these results by a sensitivity analysis restricting the sample to patients who started treatment during 2011–2019 (Appendix Table 3).
Sputum Culture Conversion
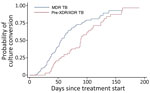
Among 214 patients with positive sputum culture at baseline, pre-XDR/XDR TB patients showed longer time to sputum culture conversion than MDR TB patients (median 88 days vs. 50 days; p = 0.001 by log rank test) (Figure). Time to sputum culture conversion in XDR TB patients was 114 days (95% CI 60–191 days). In a multivariable Cox proportional hazard model, pre-XDR/XDR TB (adjusted hazard ratio [aHR] 0.59, 95% CI 0.42–0.84) and alcohol abuse (aHR 0.61, 95% CI 0.38–0.99) were independently associated with slower sputum culture conversion (Table 5).
Adverse Drug Reactions
Overall, 152 patients (51.0%) had >1 SAE while being treated for MDR TB (Table 6). SAE were more frequent in pre-XDR/XDR TB case-patients than in fluoroquinolone-susceptible MDR TB case-patients (62.4% vs. 45.9%; p = 0.02). Peripheral neuropathy was the most frequent SAE (27.5%), regardless of TB resistance status; in all cases, peripheral neuropathy was attributed to linezolid. Severe ototoxicity occurred more frequently in pre-XDR/XDR TB than in fluoroquinolone-susceptible MDR TB cases (38.7% vs. 20.5%; p = 0.01) (Appendix Table 4); all cases of severe ototoxicity were attributed to amikacin. In multivariable analysis (Table 7), pre-XDR/XDR TB was not independently associated with severe toxicity (aOR 1.31, 95% CI 0.76–2.26; p = 0.34), whereas poor treatment adherence was associated with a higher risk for SAE (aOR 1.24 95% CI 1.04–1.47; p = 0.01).
Overall, we did not detect a significant effect of pre-XDR and XDR TB resistance, in accordance with the revised WHO definitions, on treatment outcomes of MDR TB in France during 2006–2019. The global treatment success proportion in MDR TB patients was 67.8%; previous TB treatment and poor treatment adherence were each independently associated with unfavorable outcome. Pre-XDR/XDR TB patients showed longer time to sputum culture conversion compared with fluoroquinolone-susceptible MDR TB. Pre-XDR/XDR TB resistance status was not independently associated with higher risk for SAEs.
In the literature, pre-XDR/XDR TB has been consistently associated with treatment failure (19–22). Indeed, in a meta-analysis published by Ahmad et al., the pooled successful treatment proportion for fluoroquinolone-susceptible MDR TB was estimated at 62%–73%, whereas that of pre-XDR/XDR TB was 51%–57% during the same period (2009–2016) (5). However, MDR/XDR TB treatment outcomes have improved with the introduction of bedaquiline and delamanid (23–25), together with repurposed TB drugs such as linezolid, clofazimine, and carbapenems (26–29). In our cohort, treatment success proportions were comparable between fluoroquinolone-susceptible MDR TB, pre-XDR TB, and XDR TB patients. These results are consistent with previous studies from high-income countries such as Italy (10) and South Korea (11). In those countries, as in France, these results may be explained by the routine availability of rapid molecular testing, therapeutic drug monitoring, newer and repurposed drugs, and treatment design in consultation with a MDR TB consilium (16,17,30).
The finding that fluoroquinolone resistance does not affect treatment outcomes reflects the early access and use of new and repurposed drugs in France. However, the proportion of treatment success in our cohort (67.8%) may appear low compared with clinical trials, which usually achieve >80% success (31,32). A likely explanation is the high proportion of lost-to-follow-up (18.1%) and nonevaluated (11.4%) outcomes, which account for 92% of all unfavorable outcomes in our real-world cohort. This reasoning is consistent with previous findings showing that even high-income settings have room to improve with respect to supports provided to MDR TB patients (33), especially when a high proportion is not locally born and may not be permanent residents.
In our study, pre-XDR/XDR TB was associated with substantially longer time to sputum culture conversion than was fluoroquinolone-susceptible MDR TB. However, the difference did not affect treatment outcomes; this finding is consistent with previous studies in which time to culture conversion was not a good predictor of treatment outcome (34,35). In our study, the pre-XDR/XDR TB and fluoroquinolone-susceptible MDR TB populations were very different. Indeed, pre-XDR/XDR TB patients had more severe TB pulmonary disease, as previously reported (10,11). In addition, social indicators of precarity and psychiatric disorders were more frequently observed in the pre-XDR/XDR TB population. Despite these differences in baseline characteristics that we expected to cause worse outcome in pre-XDR/XDR TB patients, fluoroquinolone-resistant MDR TB patients yielded treatment success rate similar to that of fluoroquinolone-susceptible MDR TB patients, and pre-XDR/XDR TB resistance was not independently associated with unfavorable treatment outcomes.
Our study also highlights that the revised definition of XDR TB concerns a limited number of patients in France, as previously reported (36). Indeed, only 9 patients >14 years of age, corresponding to 3% of the total MDR TB patients, could be classified as XDR TB in our cohort. The small number of patients affected by XDR TB prevented us from performing planned subgroup analyses. Overall, treatment outcome and safety in this group seemed comparable with other MDR TB patients, whereas time to sputum culture conversion was longer.
In multivariable logistic regression, previous TB treatment and poor treatment adherence, but not pre-XDR/XDR TB status, were independently associated with treatment failure. In the literature, numerous risk factors were reported for treatment failure, including age, lower body mass index, history of drug abuse, and comorbidities (10,11,37,38). We tested and confirmed the absence of interaction between previous TB treatment and poor treatment adherence before including those variables in multivariable models; however, we could hypothesize that previous treatment that led to poor outcome could be associated with lower adherence to medical visits (i.e., a patient’s lack of confidence in treatment after failure of a previous TB treatment).
A strength of our study is that it includes a multivariable evaluation of safety of treatment in fluoroquinolone-susceptible MDR TB compared with pre-XDR/XDR TB (11). In univariate analysis, serious adverse events were more frequent in pre-XDR/XDR TB cases than in fluoroquinolone-susceptible MDR TB cases, but this difference was not confirmed in multivariable analysis. The higher proportion of SAE in the pre-XDR/XDR group is likely linked to a longer duration of treatment and to a more frequent use of poorly tolerated drugs, such as linezolid, in this group, as described previously (39).
Our analysis had the inherent limitations of retrospective studies; one was the issue of missing data, which we managed using multiple imputation. Overall, the rate of loss to-follow-up was high in our cohort, and we were not able to collect data up to 2 years after end-of-treatment outcome for all patients. Furthermore, we focused on retrieving only SAEs, without considering nonserious adverse events that, for instance, might have compromised treatment adherence. In addition, we included 3 referral centers in the metropolitan Paris area. A large part of the more complex patients from all areas in France are known to be referred to those 3 centers. Hence, we have a potential bias in extrapolating our conclusions to all cases of MDR TB in France.
In summary, in our cohort of MDR TB patients treated in France during 2006–2019, the proportion of treatment success was only 67.8% because of high rates of patients who did not complete follow-up and unevaluated outcomes. We were unable to detect any differences in success rates between fluoroquinolone-susceptible MDR TB and pre-XDR/XDR TB patients; this finding may be linked to the high proportion of pre-XDR/XDR TB patients receiving newly defined group A drugs and to individually tailored treatment regimens through a multidisciplinary consilium. As expected, SAEs were frequent and affected more than half our cohort patients, which underlines the need for better management of the more toxic drugs such as linezolid.
Dr. Kherabi is an infectious diseases specialist particularly interested in drug-resistant tuberculosis management in France. She is also involved in educational affairs through the European Society of Clinical Microbiology and Infectious Diseases.
Members of the MDR TB Management Group (in alphabetical order by affiliation): Alexandra Aubry, Isabelle Bonnet, Johannes Eimer, Florence Morel, Nicolas Veziris (Sorbonne Université, INSERM, U1135, Centre d'Immunologie et des Maladies Infectieuses, Cimi-Paris, équipe 2, Paris, France); Emmanuelle Cambau, Emmanuel Lecorché, Faiza Mougari (Centre National de Référence des Mycobactéries et de la Résistance des Mycobactéries aux Antituberculeux, AP-HP, Paris, France); Claire Andrejak, Anne Bourgarit, Elise Klement, Bénédicte Rivoire, Guillaume Thouvenin, Simone Tunesi, Marie Wicky (French MDR TB Consilium) ; Marie Jaspard (Groupe Hospitalier Universitaire Sorbonne Université, Hôpital Pitié-Salpêtrière, Service de Maladies Infectieuses et Tropicales, AP-HP, Paris, France); Corentine Alauzet (Laboratoire de Bactériologie, CHRU de Nancy, Université de Lorraine, Vandoeuvre-Lès-Nancy, France); Lelia Escaut (Service de Maladies Infectieuses et Tropicales, Hôpital Kremlin-Bicêtre, AP-HP, Le Kremlin-Bicêtre, France); Sophie Ellis-Corbet (CLAT des Côtes d’Armor, Saint-Brieuc, France); Anne-Laure Roux (Service de Microbiologie, Hôpital Ambroise Paré, AP-HP, Boulogne, France).
Acknowledgment
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
References
- World Health Organization. Global tuberculosis report 2021. 2021 [cited 2021 Nov 7]. https://www.who.int/teams/global-tuberculosis-programme/tb-reports/global-tuberculosis-report-2021
- Bernard C, Brossier F, Sougakoff W, Veziris N, Frechet-Jachym M, Metivier N, et al.; MDR-TB Management group of the NRC. A surge of MDR and XDR tuberculosis in France among patients born in the Former Soviet Union. Euro Surveill. 2013;18:20555. DOIPubMedGoogle Scholar
- Guthmann J-P, Comolet T, Trébucq A. EMC [in French]. Pneumologie. 2019;1:1–16.
- Tuberculosis in France: epidemiological data 2019 [in French]. 2021 [cited 2021 Oct 15]. https://www.santepubliquefrance.fr/les-actualites/2021/tuberculose-en-france-donnees-epidemiologiques-2019
- Ahmad N, Ahuja SD, Akkerman OW, Alffenaar JC, Anderson LF, Baghaei P, et al.; Collaborative Group for the Meta-Analysis of Individual Patient Data in MDR-TB treatment–2017. Treatment correlates of successful outcomes in pulmonary multidrug-resistant tuberculosis: an individual patient data meta-analysis. Lancet. 2018;392:821–34. DOIPubMedGoogle Scholar
- World Health Organization. WHO consolidated guidelines on drug-resistant tuberculosis treatment. Licence: CC BY-NC-SA 3.0 IGO. Geneva: The Organization. 2019.
- World Health Organization. Meeting report of the WHO expert consultation on the definition of extensively drug-resistant tuberculosis [cited 2021 May 17]. https://www.who.int/publications-detail-redirect/meeting-report-of-the-who-expert-consultation-on-the-definition-of-extensively-drug-resistant-tuberculosis
- Ahuja SD, Ashkin D, Avendano M, Banerjee R, Bauer M, Bayona JN, et al.; Collaborative Group for Meta-Analysis of Individual Patient Data in MDR-TB. Multidrug resistant pulmonary tuberculosis treatment regimens and patient outcomes: an individual patient data meta-analysis of 9,153 patients. PLoS Med. 2012;9:
e1001300 . DOIPubMedGoogle Scholar - Roelens M, Battista Migliori G, Rozanova L, Estill J, Campbell JR, Cegielski JP, et al. Evidence-based definition for extensively drug-resistant tuberculosis. Am J Respir Crit Care Med. 2021;204:713–22. DOIPubMedGoogle Scholar
- Riccardi N, Saderi L, Borroni E, Tagliani E, Cirillo DM, Marchese V, et al. Therapeutic strategies and outcomes of MDR and pre-XDR-TB in Italy: a nationwide study. Int J Tuberc Lung Dis. 2021;25:395–9. DOIPubMedGoogle Scholar
- Lee EH, Yong SH, Leem AY, Lee SH, Kim SY, Chung KS, et al. Improved fluoroquinolone-resistant and extensively drug-resistant tuberculosis treatment outcomes. Open Forum Infect Dis. 2019;6:ofz118. DOIGoogle Scholar
- World Health Organization. Policy guidance on drug-susceptibility testing (DST) of second-line antituberculosis drugs. 2008 [cited 2020 Aug 4]. https://apps.who.int/iris/handle/10665/70500
- World Health Organization. Meeting report of the WHO expert consultation on drug-resistant tuberculosis treatment outcome definitions; Geneva, Switzerland; November 17–19, 2020 [cited 2021 Oct 15]. https://www.who.int/publications-detail-redirect/9789240022195
- World Health Organization. Consolidated guidelines on tuberculosis. Module 4: treatment—drug-resistant tuberculosis treatment [cited 2021 Nov 7]. https://www.who.int/publications-detail-redirect/9789240007048
- High Council for Public Hygiene. Tuberculosis with resistant bacilli: diagnosis and management. HCSP report [in French]. 2014 Dec [cited 2020 Aug 2]. https://www.hcsp.fr/explore.cgi/avisrapportsdomaine?clefr=483
- Guglielmetti L, Jaffré J, Bernard C, Brossier F, El Helali N, Chadelat K, et al. Multidisciplinary advisory teams to manage multidrug-resistant tuberculosis: the example of the French Consilium. Int J Tuberc Lung Dis. 2019;23:1050–4.
- D’Ambrosio L, Bothamley G, Caminero Luna JA, Duarte R, Guglielmetti L, Muñoz Torrico M, et al. Team approach to manage difficult-to-treat TB cases: Experiences in Europe and beyond. Pulmonology. 2018;24:132–41. DOIPubMedGoogle Scholar
- US Food and Drug Administration. What is a serious adverse event? 2020 Sep 9 [cited 2021 Oct 15]. https://www.fda.gov/safety/reporting-serious-problems-fda/what-serious-adverse-event
- Kim H-R, Hwang SS, Kim HJ, Lee SM, Yoo C-G, Kim YW, et al. Impact of extensive drug resistance on treatment outcomes in non-HIV-infected patients with multidrug-resistant tuberculosis. Clin Infect Dis. 2007;45:1290–5. DOIPubMedGoogle Scholar
- Kim DH, Kim HJ, Park S-K, Kong S-J, Kim YS, Kim T-H, et al. Treatment outcomes and long-term survival in patients with extensively drug-resistant tuberculosis. Am J Respir Crit Care Med. 2008;178:1075–82. DOIPubMedGoogle Scholar
- Kwak N, Kim H-R, Yoo C-G, Kim YW, Han SK, Yim J-J. Changes in treatment outcomes of multidrug-resistant tuberculosis. Int J Tuberc Lung Dis. 2015;19:525–30. DOIPubMedGoogle Scholar
- Falzon D, Gandhi N, Migliori GB, Sotgiu G, Cox HS, Holtz TH, et al.; Collaborative Group for Meta-Analysis of Individual Patient Data in MDR-TB. Resistance to fluoroquinolones and second-line injectable drugs: impact on multidrug-resistant TB outcomes. Eur Respir J. 2013;42:156–68. DOIPubMedGoogle Scholar
- Diacon AH, Pym A, Grobusch MP, de los Rios JM, Gotuzzo E, Vasilyeva I, et al.; TMC207-C208 Study Group. Multidrug-resistant tuberculosis and culture conversion with bedaquiline. N Engl J Med. 2014;371:723–32. DOIPubMedGoogle Scholar
- Skripconoka V, Danilovits M, Pehme L, Tomson T, Skenders G, Kummik T, et al. Delamanid improves outcomes and reduces mortality in multidrug-resistant tuberculosis. Eur Respir J. 2013;41:1393–400. DOIPubMedGoogle Scholar
- Bastard M, Guglielmetti L, Huerga H, Hayrapetyan A, Khachatryan N, Yegiazaryan L, et al. Bedaquiline and repurposed drugs for fluoroquinolone-resistant multidrug-resistant tuberculosis: how much better are they? Am J Respir Crit Care Med. 2018;198:1228–31. DOIPubMedGoogle Scholar
- Lee M, Lee J, Carroll MW, Choi H, Min S, Song T, et al. Linezolid for treatment of chronic extensively drug-resistant tuberculosis. N Engl J Med. 2012;367:1508–18. DOIPubMedGoogle Scholar
- Lee M, Cho SN, Barry CE III, Song T, Kim Y, Jeong I. Linezolid for XDR-TB—final study outcomes. N Engl J Med. 2015;373:290–1. DOIPubMedGoogle Scholar
- Tang S, Yao L, Hao X, Zhang X, Liu G, Liu X, et al. Efficacy, safety and tolerability of linezolid for the treatment of XDR-TB: a study in China. Eur Respir J. 2015;45:161–70. DOIPubMedGoogle Scholar
- Dooley KE, Sayre P, Borland J, Purdy E, Chen S, Song I, et al. Safety, tolerability, and pharmacokinetics of the HIV integrase inhibitor dolutegravir given twice daily with rifampin or once daily with rifabutin: results of a phase 1 study among healthy subjects. J Acquir Immune Defic Syndr 2013;62:21–7.
- Guglielmetti L, Le Dû D, Veziris N, Caumes E, Marigot-Outtandy D, Yazdanpanah Y, et al.; MDR-TB Management Group of the French National Reference Center for Mycobacteria and the Physicians of the French MDR-TB Cohort. Is bedaquiline as effective as fluoroquinolones in the treatment of multidrug-resistant tuberculosis? Eur Respir J. 2016;48:582–5. DOIPubMedGoogle Scholar
- Conradie F, Diacon AH, Ngubane N, Howell P, Everitt D, Crook AM, et al.; Nix-TB Trial Team. Treatment of highly drug-resistant pulmonary tuberculosis. N Engl J Med. 2020;382:893–902. DOIPubMedGoogle Scholar
- Nunn AJ, Phillips PPJ, Meredith SK, Chiang C-Y, Conradie F, Dalai D, et al.; STREAM Study Collaborators. A trial of a shorter regimen for rifampin-resistant tuberculosis. N Engl J Med. 2019;380:1201–13. DOIPubMedGoogle Scholar
- Kherabi Y, Mollo B, Gerard S, Lescure F-X, Rioux C, Yazdanpanah Y. Patient-centered approach to the management of drug-resistant tuberculosis in France: How far off the mark are we? PLOS Glob Public Health. 2022;2:
e0000313 . DOIGoogle Scholar - Kurbatova EV, Gammino VM, Bayona J, Becerra MC, Danilovitz M, Falzon D, et al. Predictors of sputum culture conversion among patients treated for multidrug-resistant tuberculosis. Int J Tuberc Lung Dis. 2012;16:1335–43. DOIPubMedGoogle Scholar
- Bastard M, Sanchez-Padilla E, Hayrapetyan A, Kimenye K, Khurkhumal S, Dlamini T, et al. What is the best culture conversion prognostic marker for patients treated for multidrug-resistant tuberculosis? Int J Tuberc Lung Dis. 2019;23:1060–7. DOIPubMedGoogle Scholar
- Veziris N, Bonnet I, Morel F, Guglielmetti L, Maitre T, Ray LFL, et al. Impact of the revised definition of extensively drug resistant tuberculosis. Eur Respir J. 2021 Jan 1 [cited 2021 Nov 1]. https://erj.ersjournals.com/content/early/2021/04/08/13993003.00641-2021
- Oliveira O, Gaio R, Correia-Neves M, Rito T, Duarte R. Evaluation of drug-resistant tuberculosis treatment outcome in Portugal, 2000-2016. PLoS One. 2021;16:
e0250028 . DOIPubMedGoogle Scholar - Heyckendorf J, van Leth F, Kalsdorf B, Olaru ID, Günther G, Salzer HJF, et al. Relapse-free cure from multidrug-resistant tuberculosis in Germany. [cited 2021 Nov 27]. Eur Respir J. 2018;51:
1702122 . DOIPubMedGoogle Scholar - Lan Z, Ahmad N, Baghaei P, Barkane L, Benedetti A, Brode SK, et al.; Collaborative Group for the Meta-Analysis of Individual Patient Data in MDR-TB treatment 2017. Drug-associated adverse events in the treatment of multidrug-resistant tuberculosis: an individual patient data meta-analysis. Lancet Respir Med. 2020;8:383–94. DOIPubMedGoogle Scholar
Figure
Tables
Cite This ArticleOriginal Publication Date: August 09, 2022
Table of Contents – Volume 28, Number 9—September 2022
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Yousra Kherabi, Sorbonne Université, INSERM U1135, Centre d’Immunologie et des Maladies Infectieuses, Cimi-Paris, Équipe 2, Paris, France
Top