Volume 8, Number 1—January 2002
Dispatch
Absence of Mycoplasma Contamination in the Anthrax Vaccine
Cite This Article
Citation for Media
Abstract
Mycoplasma contamination of the licensed anthrax vaccine administered to military personnel has been suggested as a possible cause of Persian Gulf illness. Vaccine samples tested by nonmilitary laboratories were negative for viable mycoplasma and mycoplasma DNA and did not support its survival. Mycoplasma contamination of anthrax vaccine should not be considered a possible cause of illness.
Anthrax Vaccine Adsorbed (AVA, BioPort Corporation, Lansing, MI) is a licensed vaccine for anthrax that was administered to approximately 150,000 U.S. military personnel during the Persian Gulf War. It was used more recently as part of a comprehensive vaccination policy for Department of Defense (DOD) service members. The vaccine, which is administered subcutaneously over an 18-month schedule, is derived from sterile, acellular filtrates of microaerophilic cultures of the avirulent, nonencapsulated V770-NP1-R strain of Bacillus anthracis. The cultures are grown in a sterile synthetic liquid medium devoid of enriched supplements such as serum. The filtrates predominantly contain the protective antigen of anthrax. The final vaccine formulation contains protective antigen adsorbed to aluminum hydroxide (<2.4 mg/0.5 mL) as an adjuvant. Formaldehyde (<0.02%) is added as a stabilizer and benzethonium chloride (0.0025%) as a preservative. The final product is checked for potency and safety according to U.S. Food and Drug Administration (FDA) regulations.
Approximately 1.9 million doses of AVA were administered in the United States from January 1990 through August 2000 (1), with 1,544 adverse reactions (0.08% of all injections) reported through the Vaccine Adverse Event Reporting System (2). Most of these adverse reactions were limited to the injection site; local hypersensitivity, edema, and pain were the most commonly reported, although 76 (4.9%) of the adverse reactions were classified as serious.
Recently, Nicolson et al. (3) suggested that contamination of this vaccine with Mycoplasma fermentans could have been responsible for human illness specifically associated with Persian Gulf syndrome. Mycoplasma contamination is considered to be a potential problem for vaccines that are produced in cell cultures. Such vaccines have to meet specific FDA testing requirements to demonstrate the absence of mycoplasma contamination, which is considered unlikely in vaccines that are not cell culture-derived, such as AVA,. However, in response to the continuing controversy surrounding this vaccine, the possibility of its being contaminated with mycoplasma was examined by two different techniques.
AVA was administered to U.S. personnel during Operation Desert Storm/Desert Shield (ODS/DS), including lots FAV 001 through FAV 007. Although the lots tested in this study were not administered to U.S. personnel deployed during ODS/DS, the filling and potency testing of lot FAV 008 in March 1991 were contemporaneous with that of FAV 007 and were subject to the same regulatory criteria for lot release and use. Its use in the current vaccination program was permitted through shelf life extension based on satisfactory potency testing.
Twenty vials of AVA, including samples from four lots, were obtained from eight DOD vaccination clinics across the United States (Table). The tested lots represented all unexpired vaccine available to the DOD at the time of testing. Testing of unexpired material was deemed necessary to avoid potential uncertainty regarding degradation of vaccine components or analytes.
These vials were divided into two matched sets and were sent to two nonmilitary laboratories for testing for mycoplasma contamination. One set was tested by culture techniques for the presence of live organisms at the Mycoplasma Laboratory, Science Applications International Corporation, National Cancer Institute, Frederick Research and Development Center, Frederick, MD. A commercial nongovernment facility, Charles River Tektagen, tested the second set for mycoplasma DNA by polymerase chain reaction (PCR) assay.
Ten anthrax vaccine vials were tested for the presence of mycoplasma by standardized cultivation methods (4–6) with three different media. The media used for isolation were SP-4 (4), DM-1 (5), and M-CMRL (6); all three supported the growth of Mycoplasma organisms. Vaccine samples were removed under Biosafety Level-2 conditions and tested both undiluted and at a 10-fold dilution to reduce the concentrations of stabilizer and preservative. Each culture plate was inoculated with 0.1 mL of vaccine. M-CMRL plates were incubated aerobically at 36°C, and SP-4 and DM-1 plates were incubated anaerobically at 36°C. After 10 days, all plates were examined microscopically. No evidence of Mycoplasma colonies was found in any of the culture plates inoculated with the AVA samples.
To determine if Mycoplasma organisms could survive in the vaccine, which contains formaldehyde and benzethonium chloride, a fifth lot of vaccine (FAV038) was obtained and evaluated. This vaccine lot also tested negative. To test the ability of Mycoplasma to survive in the vaccine, M. fermentans strain incognitus (7) was inoculated at a concentration of 1.54 x 108 CFU per 0.1 mL into 5 mL of vaccine and mixed. Eight serial 10-fold dilutions of this “time 0" sample were immediately plated on SP-4 agar plates. The remaining vaccine-Mycoplasma mixture was held at 4°C and sampled at 24, 48, and 72 hours. Tenfold serial dilutions of these sequential samples were immediately plated as described for the time 0 sample.
All SP-4 plates were incubated for a minimum of 10 days and examined for viable colonies. The colony growth on the time 0 plates was atypical, with much debris on the low dilution plates. The titer of mycoplasma from the time 0 sample was 4.2 x 105 CFU per 0.1 mL. Inactivation of the organisms by the preservatives in the vaccine was rapid, as no growth was detected on plates inoculated with samples taken from the mycoplasma-vaccine mixtures held at 4°C for 24, 48, or 72 hours.
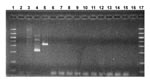
Testing for the presence of mycoplasma DNA in the second set of AVA samples, representing four lots, was performed by a commercial testing facility (Charles River Tektagen, Malvern, PA) that used the Detection of Mycoplasma by PCR kit (#90-100K, American Type Culture Collection, Rockville, MD). Samples were tested first for the presence of any mycoplasma DNA; the species was then determined for samples that tested positive. The vaccine samples were centrifuged (12,000 x g for 10 minutes at 4°C) and processed for DNA extraction according to the kit’s instructions. Samples were amplified in a nested PCR reaction and examined by gel electrophoresis. The positive control samples were M. pirum and Acholeplasma laidlawii, and the negative control samples were mycoplasma broth, Hut78 cell extract, and sterile RNase-free water. All 10 of the tested AVA samples were negative for the presence of mycoplasma DNA (Figure).
No evidence was found either from culture or mycoplasma-specific nucleic acid amplification methods to suggest that a mycoplasma contaminant was present in the vaccine lots tested. These results are consistent with those of a previous report that found no evidence of such contamination in another anthrax vaccine (8). Additionally, Mycoplasma organisms deliberately added to AVA did not survive for even 1 day, presumably because of the preservatives added to the vaccine formulation to retard adventitious agent growth.
These results argue against assertions that this vaccine was contaminated with Mycoplasma organisms and that such putative contamination contributed to human illness. This finding is consistent with a serologic study of pre- and post-Gulf War serum samples from symptomatic and asymptomatic military personnel, which found no evidence of an association between Gulf War illness and infection with M. fermentans (9).
Dr. Hart is chief of the Department of Cell and Host Responses in the Virology Division of the U.S. Army Medical Research Institute of Infectious Diseases, where she supervises the Cell Culture and Hybridoma Production facilities. Her research focuses on immune responses to viruses.
Acknowledgment
We thank J.G. Tully for supplying the culture of Mycoplasma fermentans strain incognitus and John Kondig and Julie Gillen for technical assistance. We also thank Marc Caouette and John Grabenstein for coordinating the procurement of the vaccine samples.
References
- Centers for Disease Control and Prevention. Use of anthrax vaccine in the United States: recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Morb Mortal Wkly Rep. 2000;49(RR-15):7–10.
- Chen RT, Rastogi SC, Mullen JR, Hayes SW, Cochi SL, Donlon JA, The vaccine adverse event reporting system (VAERS). Vaccine. 1994;12:542–50. DOIPubMedGoogle Scholar
- Nicolson GL, Nass M, Nicolson NL. Anthrax vaccine: controversy over safety and efficacy. Antimicrobics and Infectious Disease Newsletter. 2000;18:1–6. DOIGoogle Scholar
- Tully JG. A culture medium formulation for primary isolation and maintenance of mollicutes. In: Tully JG, Razin S, editors. Molecular and diagnostic procedures in mycoplasmology. Vol I. New York: Academic Press; 1995. p. 33-9.
- Del Giudice RA, Tully JG. Isolation of mycoplasma from cell cultures by axenic techniques. In: Tully JG, Razin S, editors. Molecular and diagnostic procedures in mycoplasmology. Vol I. New York: Academic Press; 1995. p. 411-8.
- Del Giudice RA. M-CMRL, a new axenic medium to replace indicator cell cultures for the isolation of all strains of M. hyorhinis. In Vitro Cell Dev Biol Anim. 1998;34:88–9. DOIPubMedGoogle Scholar
- Saillard C, Carle P, Bove JM, Bebear C, Lo SC, Shih JW, Genetic and serologic relatedness between Mycoplasma fermentans strains and a mycoplasma recently identified in tissues of AIDS and non-AIDS patients. Res Virol. 1990;141:385–95. DOIPubMedGoogle Scholar
- Alshawe A, Alkhateeb G. Test of Iraqi anthrax vaccine and other vaccines. J Biol Sci Res. 1987;17:1–16.
- Gray GC, Kaiser KS, Hawksworth AW, Watson HL. No serological evidence of an association found between Gulf War service and Mycoplasma fermentans infection. Am J Trop Med Hyg. 1999;60:752–7.PubMedGoogle Scholar
Figure
Table
Cite This ArticleTable of Contents – Volume 8, Number 1—January 2002
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
George Korch, USAMRIID, 1425 Porter Street, Frederick, MD 21702, USA; fax: 301-619-4625;
Top