Volume 10, Number 11—November 2004
Dispatch
Commercial Logging and HIV Epidemic, Rural Equatorial Africa
Cite This Article
Citation for Media
Abstract
We found a high seroprevalence of HIV among young women in a commercial logging area in Cameroon. The vulnerability of these young women could be related to commercial logging and the social and economic networks it induces. The environmental changes related to this industry in Equatorial Africa may facilitate HIV dissemination.
More than 20 years after the beginning of the HIV epidemic, the Joint United Nations Programme on HIV/AIDS (UNAIDS) stated that the epidemic was now taking hold in many African countries (1). An estimated 25.0–28.2 million persons are already infected in sub-Saharan Africa, accounting for 70% of all infections worldwide, and Africans represent 10% of the world population. AIDS is now the leading cause of death in Africa (2.2–2.4 million deaths in 2003) (2). UNAIDS particularly underlined the rapidly rising prevalence in Cameroon, a central African country (4.7% in 1996, 11.8% in 2001) (1,3). As in many countries, these data come from sentinel surveillance of women attending urban and semi-urban antenatal clinics.
Data from rural areas are scarce, and the dynamics of HIV infection are poorly documented. Travel has been linked to an increased risk among rural populations (4). The recent environmental changes related to commercial logging in Equatorial Africa could potentially facilitate HIV dissemination. Commercial logging has led to road construction in remote forested areas, human migration (especially of single men), and develop social and economic networks (including commercial sex work) that support this industry (5). In Cameroon, commercial logging has been growing for at least 4 decades. We have previously shown that these environmental changes might represent a risk to human health through exposure to simian immunodeficiency viruses (6). We investigated the seroprevalence of HIV, the nature of circulating HIV genetic variants, and factors associated with HIV infection in a logging area of southern Cameroon.
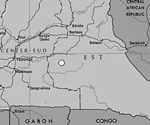
A cross-sectional, community-based survey was performed in September 2001 in a remote village where a sawmill and logging camp have been located since 1973 (Nkonzuh, East Province) and also in two neighboring villages (Mboumo and Kompia, 10 km and 30 km from the logging camp, respectively). The three villages are 250 km from Yaoundé, the capital of Cameroon (Figure). The total population of the three villages has increased since commercial logging began and was estimated at 1,000 inhabitants at the time of the survey (excluding the logging camp). Approximately 200 workers are employed in this industry; approximately half originate from the region. Some workers live in the traditional neighborhoods of Nkonzuh, and a small number live in Mboumo and Kompia; most live in the logging camp. The survey in Nkonzuh was carried out in the traditional neighborhoods but not in the logging camp itself. All inhabitants >15 years of age were asked to participate in the survey during door-to-door visits. After participants gave informed consent, they were interviewed by using a verbal standard questionnaire in French or a local language. The data gathered included the village name, time spent in the village, house number, date of birth or age, sex, ethnic group, marital status, level of education, occupation, and history of blood transfusion, injection, surgery, circumcision or excision, tattoo, and sexually transmitted infections (STI).
Serologic screening for HIV infection was based on an enzyme-linked immunosorbent assay (ELISA) (Murex HIV-1.2.O, Abbott, Rungis, France). All positive samples were confirmed and typed (HIV-1 or -2) by using a line immunoassay (INNO-LIA HIV-1+2, Innogenetics, Ghent, Belgium). All positive samples were further typed (HIV-1 group M, N, O or HIV-2) with an in-house ELISA based on V3 loop peptides. HIV-1–positive samples were genetically characterized in the gag and env genes by sequencing and phylogenetic analysis, as described (7). Syphilis was diagnosed by using the rapid plasma reagin (RPR) (Becton Dickinson, Mountain View, CA) and Treponema pallidum hemagglutination (TPHA) (Sanofi Pasteur, Chaska, MN) tests.
The χ² and Fisher exact tests were used to compare the distribution of categorical variables between men and women. For continuous variables, comparisons were based on the nonparametric Mann-Whitney two-sample test. Multivariate random-effects logistic regressions, including sex-specific analyses, were used to identify factors associated with HIV infection (8). Independent variables associated with HIV infection, identified by using a conservative threshold of p < 0.25 in univariate analysis, were retained for multivariate analysis. Ninety-five percent confidence intervals (CI) of proportions were estimated by using the binomial exact method.
Four hundred eighty-four persons were enrolled (Table 1). Most (77.8%) were Badjoe, a local ethnic group, and 6.4% were Pygmies; 25 other ethnic groups were also represented. The HIV serologic results were available for 476 persons. Seven persons refused venipuncture after interview, and one sample could not be analyzed. These eight persons did not differ from the other persons in term of sex (50.0% women vs. 47.1% women) but were slightly younger (median, 26.8 years vs. 34.9 years). Five (1.1%) of the 476 HIV serologic results were indeterminate, and these persons were excluded from the analysis of risk factors. The overall HIV seroprevalence was 7.4% (CI 5.2%–10.1%). Women had a far higher HIV seroprevalence than men (overall 11.1% vs. 3.1%) (Table 2), which ranged from 4.9% in women at least 50 years of age to 22.5% in the 25- to 34-year age group. In men, the HIV seroprevalence ranged from 1.4% in the 15- to 24-year age group to 6.0% in the 25- to 34-year age group. The HIV seroprevalence was higher for both sexes, although not significantly, in the village in which the logging camp is located than in the two surrounding villages (Table 1).
All 35 seropositive persons were infected by HIV-1, and no one was coinfected by HIV-2. Samples from 28 persons reacted with group M peptides, and two others reacted with both group M and O peptides. Five serum samples did not react with group M, N, or O peptides. Twenty-six of the 35 seropositive samples could be amplified, and all were genetically characterized, in both gag and env (n = 24), gag only (n = 1), or env only (n = 1). The circulating recombinant form (CRF) 02_AG strain predominated (72.0% in gag and 76.0% in env), and several other variants cocirculated (subtypes A, F2, G, and H and CRF06_cpx and CRF11_cpx). A discordant profile was observed between the gag and env genes in three persons (12.5%): Agag/Henv, Ggag/CRF06_cpxenv, Ggag/CRF11_cpxenv, respectively.
In univariate analysis, HIV infection in women was associated with age group (p = 0.03), marital status (p = 0.002), level of education (p = 0.03), history of blood transfusion (p = 0.05), and STI (p = 0.04) (Table 1). In men, no factors were associated with HIV infection. In multivariate analysis, HIV infection remained strongly associated with sex (odds ratio 10.22; CI 3.19–32.80; p < 0.001), after adjustment for marital status, level of education, and history of STI. No specific risk factors were found in men. In contrast, women who are unmarried, educated, or have a history of an STI were more likely to be infected by HIV than women who were married, never-schooled, or did not have a history of an STI (Table 3).
We identified a population with a high seroprevalence of HIV infection; nearly one quarter of women 25–34 years of age were infected. The HIV seroprevalence among women 15–44 years of age (median 26 years) was slightly higher than among women of the same age group (median 22 years) who attended urban and semiurban antenatal clinics in the East Province (14.5% vs. 10.0%) (9). HIV seroprevalence among women was comparable in the 15- to 24-year age groups (10.0% vs. 10.4%) and the 35- to 44-year age groups (11.5% vs. 12.5%), while it was much higher in the 25- to 34-year age group (22.5% vs. 8.3%). Lower seroprevalence rates among women who went to the antenatal clinics than in the general female population have been reported in several African countries, which is attributable to lower fertility among HIV-infected women (10), but the far higher rate observed in our 25- to 34-year age group is particularly striking.
The overall HIV seroprevalence was higher, although not significantly, in our survey (7.4%, CI 5.2%–10.1%) than in another survey conducted in villages of the same province (4.5%, CI 3.3%–6.1%) (11). The villages we surveyed are more readily accessible by car, which favors travels to and from places with higher HIV seroprevalence (towns and other regions). The proportion of Pygmies, who are known to have a low HIV seroprevalence (12), confirmed by our results, is lower in the area we surveyed. Some villages surveyed by Nyambi et al. (11) were located in an area with a more recent history of logging activity where environmental changes had not yet fully affected the epidemic.
The high HIV seroprevalence in women 25–34 years of age living in this rural area could be related to commercial logging. In a context in which workers had relatively high salaries (U.S. $60 to U.S. $530 per month), sexual networks were extensive and complex (13). An estimated 40 female sex workers were permanently living in the logging camp (S. Loul, pers. comm.). In addition, ≈100 women arrived at the logging camp from towns or neighboring villages at the time of salary distribution (twice a month), to trade or offer paid sex (U.S. $1.50 per intercourse). Some men and women had sex with several partners a night. Some workers’ wives also had extramarital sex. Seroprevalence in both sex and odds ratio when men and women are compared are age-specific; seroprevalence in women 25–34 years of age is greater for those in our study than those in the sentinel surveillance. The lack of association with local risk factors, such as blood transfusion and injection, and the results of the multivariate analysis suggest that young, unmarried, and educated local women could be mainly infected by workers during unprotected relationships in exchange for money or goods. The high prevalence of syphilis confirmed high-risk sexual behavior (11.8% in women 15–44 years of age compared to 3.6% among those who attended antenatal clinics) (9).
HIV-1 genetic diversity and its distribution were similar to that observed in towns (7,14), which suggests that the spread of HIV in this rural area results from numerous introductions of the virus. The vulnerability of this rural population, especially young women, to HIV infection could be related to commercial logging and the social and economic networks it creates.
Dr. Laurent is an epidemiologist at Institut de Recherche pour le Développement (IRD), Montpellier, France. His major interests include epidemiology and clinical research on HIV infection in Africa.
Acknowledgments
We thank Géraldine Manirakiza, Marie Bourgeois, Audrey Gleize, Mathurin, and Justin Wadi for their contribution to the field work; Alice Manirakiza for providing information on the East Province and helping to prepare the manuscript; Séverin Loul for information on the East Province and study area; and Philippe Auzel for helping to prepare and execute the study.
This work was supported by Institut de Recherche pour le Développement.
References
- UNAIDS. AIDS epidemic update: December 2002. Geneva: Joint United Nations Programme on HIV/AIDS; 2002
- UNAIDS. AIDS epidemic update: December 2003. Geneva: Joint United Nations Programme on HIV/AIDS; 2002.
- UNAIDS. Report on the global HIV/AIDS epidemic July 2002. Geneva: Joint United Nations Programme on HIV/AIDS; 2002.
- Lagarde E, Schim van der Loeff M, Enel C, Holmgren B, Dray-Spira R, Pison G, Mobility and the spread of human immunodeficiency virus into rural areas of West Africa. Int J Epidemiol. 2003;32:744–52. DOIPubMedGoogle Scholar
- Wilkie D, Shaw E, Rotberg F, Morelli G, Auzel P. Roads, development, and conservation in the Congo Bassin. Conserv Biol. 2000;14:1614–22. DOIGoogle Scholar
- Peeters M, Courgnaud V, Abela B, Auzel P, Pourrut X, Bibollet-Ruche F, Risk to human health from a plethora of simian immunodeficiency viruses in primate bushmeat. Emerg Infect Dis. 2002;8:451–7.PubMedGoogle Scholar
- Vergne L, Bourgeois A, Mpoudi-Ngolé E, Mougnutou R, Mbuagbaw J, Liegeois F, Biological and genetic characteristics of HIV infections in Cameroon reveals dual group M and O infections and a correlation between SI-inducing phenotype of the predominant CRF02_AG variant and disease stage. Virology. 2003;310:254–66.PubMedGoogle Scholar
- Goldstein H. Multilevel statistical models. 2nd ed. London: Arnold; 1995.
- National AIDS Control Committee. National serosurvey on HIV/syphilis. Cameroon: The Committee; 2001.
- Changalucha J, Grosskurth H, Mwita W, Todd J, Ross D, Mayaud P, Comparison of HIV prevalences in community-based and antenatal clinic surveys in rural Mwanza, Tanzania. AIDS. 2002;16:661–5. DOIPubMedGoogle Scholar
- Nyambi P, Zekeng L, Kenfack H, Tongo M, Nanfack A, Nkombe I, HIV infection in rural villages of Cameroon. J Acquir Immune Defic Syndr. 2002;31:506–13.PubMedGoogle Scholar
- Ndembi N, Yumo H, Takehisa J, Takemura T, Kobayashi E, Ngansop C, HIV type 1 infection in Pygmy hunter gatherers is from contact with Bantu rather than from nonhuman primates. AIDS Res Hum Retroviruses. 2003;19:435–9. DOIPubMedGoogle Scholar
- Ryder A. Demographics, health, and education of Bantu women in logging camps and surrounding villages in the forests of south-eastern Cameroon: a comparison of space and time. [cited 2002 Dec 20]. Available from: http://www.yale.edu/sangha/PDF_FILES/RyderAbigailReport.pdf
- Carr JK, Torimiro JN, Wolfe ND, Mpoudi-Ngolé E, Kim B, Sanders-Buell E, The AG recombinant IbNG and novel strains of group M HIV-1 are common in Cameroon. Virology. 2001;286:168–81. DOIPubMedGoogle Scholar
Figure
Tables
Cite This ArticleTable of Contents – Volume 10, Number 11—November 2004
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Christian Laurent, Institut de Recherche pour le Développement–UMR 145, 911, avenue Agropolis, BP 64501, 34394 Montpellier cedex 5, France; fax: 00 33 4 67 41 61 46
Top