Volume 11, Number 8—August 2005
Letter
Real-time Polymerase Chain Reaction To Diagnose Lymphogranuloma Venereum
Cite This Article
Citation for Media
To the Editor: An outbreak of rectal lymphogranuloma venereum (LGV) has been detected in the Netherlands among men who have sex with men (1–4). More cases of LGV in other European countries such as Belgium, France, and the United Kingdom have been reported, and the first cases have been detected in the United States as well. This infection is encountered not only by clinicians who treat sexually transmitted diseases but also by gastroenterologists. Both the European Surveillance of Sexually Transmitted Infections (http://www.essti.org) and the Centers for Disease Control and Prevention (http://www.cdc.gov) are working on outbreak warning and response systems to increase the awareness and the direct management of the LGV outbreak (5,6).
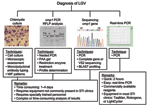
Different approaches have been described to diagnose LGV infections (Figure). The first 3 approaches have serious disadvantages: cell culture is rarely available in routine diagnostic settings, polymerase chain reaction (PCR)-based restriction fragment length polymorphism (RFLP) analysis (usually nested PCR approaches are used) needs post-PCR restriction enzyme profiling, and sequencing requires additional analyses of sequence data to identify the Chlamydia trachomatis serovar responsible for infection. In addition, all 3 techniques are time consuming (at least 1–4 days to get a result), laborious, and require specially trained personnel in a sophisticated laboratory setting. Therefore, we developed a real-time PCR approach (TaqMan and Rotorgene) that can easily identify LGV strains in 2 hours with equipment that is available in almost all diagnostic settings.
We used the polymorphic membrane protein H gene (pmp gene) as a PCR target because it has a unique gap in LGV strains of C. trachomatis, compared to other serovars, which makes it highly specific. The following primers and probes were selected: LGV-F 5´ CTG TGC CAA CCT CAT CAT CAA 3´, LGV-R 5´ AGA CCC TTT CCG AGC ATC ACT 3´, and LGV MGB-probe 6-FAM-CCT GCT CCA ACA GT. Real-time PCR conditions (20-μL format) for TaqMan were as follows: 2× TaqMan Universal Mastermix (Applied Biosystems, Foster City, CA, USA), 18 pmol each primer, 0.2 μmol/L probe, and 2 μL (LGV L2) DNA or clinical sample; 2 min at 50°C, 10 min at 95°C, and 40 cycles of 15 sec at 95°C and 1 min at 60°C. Conditions for Rotorgene were as follows: 10× buffer (Hoffman-La Roche Ltd, Basel, Switzerland), 10 pmol each primer, 0.04 μmol/L probe, 2 μL (LGV L2) DNA or clinical sample; 2 min at 50°C, 10 min at 95°C, and 45 cycles of 15 sec at 95°C and 1 min at 60°C. By using a previously described serial dilution of LGV L2 (7), sensitivity was assessed as 0.01 inclusion-forming units for both real-time PCR assays.
To determine specificity, we tested different C. trachomatis serovars and serovariants A, B, Ba, C, D, Da, D-, E, F, G, Ga, H, I, Ia, I-, J, Jv, K, L1, L2, L2b, L3, C. muridarum (MoPn), C. pneumoniae, C. pecorum, C. psittaci, and 32 other microorganisms that normally reside in the human perianal and urogenital region and in the oropharynx. These organisms included gram-positive and gram-negative bacteria and yeast: Acinetobacter baumannii, Campylobacter jejuni, Candida albicans, other yeast, Enterobacter agglomerans, Enterococcus faecalis, Escherichia coli, Streptococcus spp., Haemophilus influenzae, Klebsiella pneumoniae, Mycoplasma spp., Neisseria meningitidis, Pasteurella spp., Pseudomonas aeruginosa, Salmonella enteritidis, Shigella sonnei, Staphylococcus aureus, and others. Only LGV strains L1, L2, L2b, and L3 tested positive in both the TaqMan and Rotorgene assays, which shows the analytical specificity of real-time PCR.
Subsequently, we determined in a blinded setting the presence of LGV in a selected group of patients (clinical spectrum and epidemiology described elsewhere [8]) according to C. trachomatis–positive rectal swab (Chlamydia 2SP Collection & Transport Kit [Quelab] by commercially available PCR (COBAS AMPLICOR, Hoffman-La Roche Ltd). By using the 2 reference standard techniques to type C. trachomatis serovars (PCR-based RFLP of the omp1 gene or sequencing the variable segment 2 [VS-2] of the omp1 gene) (9,10) with DNA isolated from rectal swab specimens (standard isopropanol DNA isolation method), we identified 28 of 125 men as LGV-positive. These 28 samples were also positive in both the TaqMan and Rotorgene assays. We also identified 2 additional LGV infections, which were initially typed and then retested as single-strain infections with serovars E and D by both PCR-based RFLP analysis and VS-2 sequencing. This discrepancy is most likely due to a double infection, which will, in most cases, result in the preferential amplification of 1 strain in the omp1 PCR and PCR-based sequencing methods; in the TaqMan and Rotorgene assays, only LGV strains can be amplified. Whether this outbreak is partially technically driven must be assessed in the future by retrospectively investigating the presence of these LGV infections in men who have sex with men and the presence of the L2b strain in the past, since at present only LGV infections from 2003 to 2005 have been investigated.
References
- Nieuwenhuis RF, Ossewaarde JM, van der Meijden WI, Neumann HA. Unusual presentation of early lymphogranuloma venereum in an HIV-1 infected patient: effective treatment with 1 g azithromycin. Sex Transm Infect. 2003;79:453–5. DOIPubMedGoogle Scholar
- Nieuwenhuis RF, Ossewaarde JM, Götz HM, Dees J, Thio HB, Thomeer MG, Resurgence of lymphogranuloma venereum in Western Europe: an outbreak of Chlamydia trachomatis serovar L2 proctitis in the Netherlands among men who have sex with men. Clin Infect Dis. 2004;39:996–1003. DOIPubMedGoogle Scholar
- Den Hollander JG, Ossewaarde JM, de Marie S. Anorectal ulcer in HIV patients, don't forget lymphogranuloma venereum! AIDS. 2004;18:1484–5. DOIPubMedGoogle Scholar
- French P, Ison CA, Macdonald N. Lymphogranuloma venereum in the United Kingdom. Sex Transm Infect. 2005;81:97–8. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Lymphogranuloma venereum among men who have sex with men—Netherlands, 2003–2004. MMWR Morb Mortal Wkly Rep. 2004;53:985–8.PubMedGoogle Scholar
- van Weel J. Rare sexually transmitted disease hits Europe. Lancet Infect Dis. 2004;4:720. DOIPubMedGoogle Scholar
- Morré SA, Sillekens P, Jacobs MV, van Aarle P, de Blok S, van Gemen B, RNA amplification by nucleic acid sequence–based amplification with an internal standard enables reliable detection of Chlamydia trachomatis in cervical scrapings and urine samples. J Clin Microbiol. 1996;34:3108–14.PubMedGoogle Scholar
- Spaargaren J, Fennema HSA, Morré SA, de Vries HJC, Coutinho RA. New Lymphogranuloma venereum Chlamydia trachomatis variant, Amsterdam. Emerg Infect Dis. 2005;11:1090–2.PubMedGoogle Scholar
- Morré SA, Ossewaarde JM, Lan J, van Doornum GJ, Walboomers JM, MacLaren DM, Serotyping and genotyping of genital Chlamydia trachomatis isolates reveal variants of serovars Ba, G, and J as confirmed by omp1 nucleotide sequence analysis. J Clin Microbiol. 1998;36:345–51.PubMedGoogle Scholar
- Molano M, Meijer CJLM, Morré SA, Pol R, van den Brule AJ. Combination of PCR targeting the VD2 of omp1 and reverse line blot analysis for typing of urogenital Chlamydia trachomatis serovars in cervical scrape specimens. J Clin Microbiol. 2004;42:2935–9. DOIPubMedGoogle Scholar
Figure
Cite This Article1These authors contributed equally to this study.
Related Links
Table of Contents – Volume 11, Number 8—August 2005
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Servaas A. Morré, VU University Medical Center, Faculty of Medicine, Laboratory of Immunogenetics, Van der Boechorststraat 7, 1081 BT, Amsterdam, the Netherlands; fax: 31-20-44-48418
Top