Volume 12, Number 7—July 2006
Dispatch
Leptospirosis in Squirrels Imported from United States to Japan
Cite This Article
Citation for Media
Abstract
We diagnosed leptospirosis in 2 patients exposed to southern flying squirrels imported from the United States to Japan. Patients worked with exotic animals in their company. Leptospira isolates from 1 patient and 5 of 10 squirrels at the company were genetically and serologically identical and were identified as Leptospira kirschneri.
Leptospirosis is a worldwide zoonosis caused by infection with Leptospira interrogans sensu lato species. Leptospira is mostly transmitted to humans through contaminated water or soil and by direct contact with a variety of infected animals (1–3). To date, a variety of wild animals have been imported from foreign countries to Japan. In this study, 2 men working at an animal trading company were infected with Leptospira spp. To determine the source of infection, Leptospira spp. were isolated from animals in their company and sequenced.
An animal trading company in Shizuoka, Japan, imported 106 southern flying squirrels from Miami, Florida, on March 27, 2005. Three workers handled these animals, which were housed 10 animals to a cage. Before patient 1 became ill, the workers dressed casually and touched the animals with bare hands in their routine work. Wild rats (such as Rattus norvegicus or R. rattus) had not invaded the animal house.
On April 22, 2005, patient 1, a 29-year-old man who handled a variety of exotic animals at the company, was hospitalized in Shizuoka Saisei-kai General Hospital with fever (temperature 40°C), headache, chills, nausea, vomiting, jaundice, and uremia, symptoms similar to those of locally acquired leptospirosis. Leptospirosis was diagnosed by polymerase chain reaction (PCR) targeted to the flagellin gene (flaB) and confirmed serologically with convalescent-phase serum by microscopic agglutination test. The patient was seronegative and PCR-negative for hantavirus, which causes symptoms similar to those observed in the patient. He was treated with an intramuscular injection of streptomycin (2 mg/day) for 7 days, which is the recommended treatment for leptospirosis in Japan (4); he consequently recovered.
On June 1, 2005, patient 2, a 28-year-old man who worked at the same company, was hospitalized in Shizuoka Saisei-kai General Hospital with fever (temperature 39°C), headache, chills, nausea, vomiting, jaundice, and uremia. The patient had been in contact with imported animals. He recovered with intramuscular injections of streptomycin (2 mg/day) for 3 days, followed by treatment with oral amoxicillin for 3 days.
Leptospira DNA was detected in serum samples from patient 1 and whole blood from patient 2 by flaB PCR (5). Sequences were determined by Prism 3130-avant DNA Genetic Analyzer (Applied Biosystems, Foster City, CA, USA). Sequences of flaB detected from both patients were identical and showed a high degree of similarity to L. kirschneri.
Diagnosis was performed serologically by microscopic agglutination test with a panel of Leptospira reference strains (3). Convalescent-phase serum samples from both patients reacted to L. kirschneri strain Moskva V and strains isolated from southern flying squirrels, although serum collected on the day of hospitalization was negative in both patients (Table 1). To cultivate Leptospira, a few drops of blood from patient 2 were placed in several tubes of Ellinghausen-McCullough-Johnson-Harris medium supplemented with 2.5% rabbit serum. After 7 days of incubation at 30°C, Leptospira was detected from the culture (isolates P5.4, P10.1, P10.2).
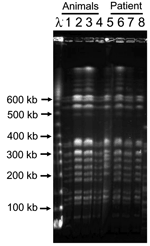
To determine the validity of the association between animals held by the company and the illness, exotic animals (75 animals, 7 species) housed in the company were tested. Leptospira was isolated from 5 of 10 kidney cultures (isolates AM1, AM2, AM3, AM7, AM8) from southern flying squirrels. DNA from the urinary bladders, including the animals' urine, was extracted by using proprietary DNA extraction kits (Quick gene, Fuji Film Co., Tokyo, Japan). Five of 10 southern flying squirrels were flaB PCR-positive (Table 2). Species of the isolates were identified by using flaB and DNA gyrase B subunit gene (gyrB) sequencing analysis. We amplified 1.2-kb partial sequences of gyrB by using primers UP1TL (5´-CAyGCnGGnGGnAArTTyGA-3´; n: A, G, T, or C; r: A or G; y: C or T) and UP2rTL (5´-TCnACrTCnGCrTCnGTCAT-3´; n: A, G, T, or C; r: A or G) (6). The isolates obtained from patient 2 and southern flying squirrels had identical flaB (data not shown) and gyrB (Figure 1) DNA sequences and were identified as L. kirschneri. The flaB sequences from the serum of patient 1 and whole blood of patient 2 were identical to those of isolates from patient 2 and animals. Additionally, restriction fragment length polymorphism (RFLP) analysis based on pulse-field gel electrophoresis was conducted (7). These isolates showed identical RFLP patterns (Figure 2), which suggests that patients were infected with L. kirschneri from southern flying squirrels.
To determine serovar of the isolates, a cross-agglutination test was performed with a panel of hyperimmune rabbit serum raised to representative serovars Icterohemorrhagiae, Copenhageni, Autumnalis, Hebdomadis, Australia, Grippotyphosa, Javanica, and Castellonis, which are present in Japan. These isolates reacted with anti-Grippotyphosa serum but not with the others (data not shown). Convalescent-phase sera from patients reacted with Leptospira isolates from the squirrels and also with serovar Grippotyphosa strain Moskva V (Table 1).
On April 24, the local health government prohibited the company from trading animals and directed them to use protection, such as latex gloves and disinfection of the floor with sodium hypochlorite, against infection. On June 2, all southern flying squirrels were euthanized by carbon dioxide, and the animal house was disinfected by the local health government. PCR detected flaB DNA on the surface of the squirrels' bodies and in urine on the soaked paper in the cages; the sequences were identical to those of the isolates. Before the first case was detected, 27 southern flying squirrels had been distributed to retail pet shops. Sixteen were returned, 2 died, 7 remained at pet shops, and 2 had been sold. The 2 sold animals and 7 remaining at the pet shops were recovered and euthanized. No illness was reported among persons in contact with these animals.
Serovar Grippotyphosa commonly causes canine leptospirosis (8,9) and infects a variety of domestic and wild animals in the United States (10–13). In Japan, serovar Grippotyphosa is distributed in the southernmost islands, the Okinawa archipelago (14), but not on Honshu Island, the main island. Patients did not travel to Okinawa or foreign countries before disease onset. Our findings support the conclusion that the patients were infected with L. kirschneri serovar Grippotyphosa by contact with southern flying squirrels. Similarly, in the United States, humans have acquired monkeypox infection from pet prairie dogs, which had themselves been infected by exotic African rodents (15); these findings show that exotic pets represent a substantial hazard. The outbreak demonstrated how new infectious diseases could be emerging because of importation from overseas. If, during shipping and housing of the animals, the infection were to have expanded among southern flying squirrels, the infection rates and risk for humans would have increased. The leptospirosis cases reported here warn against importing exotic animals.
Dr Masuzawa is a professor at the Faculty of Pharmaceutical Sciences, Chiba Institute of Science, Choshi, Japan. His primary research interests are molecular epidemiology and the ecology of zoonotic and tickborne pathogens, such as Leptospira, Borrelia, and Anaplasma.
Acknowledgment
This work was supported in part by grant H15-Shinkou-14 and H15-Shinkou-12 for Research on Emerging and Reemerging Infectious Disease from the Ministry of Health, Labour and Welfare.
References
- Faine S. Leptospira and leptospirosis. Boca Raton (FL): CRC Press; 1994.
- Terpstra WJ. Human leptospirosis: guidance for diagnosis, surveillance and control. Geneva: World Health Organization and International Leptospirosis Society; 2003.
- Kobayashi Y. Human leptospirosis: management and prognosis. J Postgrad Med. 2005;51:201–4.PubMedGoogle Scholar
- Kawabata H, Dancel LA, Villanueva SY, Yanagihara Y, Koizumi N, Watanabe H. flaB-polymerase chain reaction (flaB-PCR) and its restriction fragment length polymorphism (RFLP) analysis are an efficient tool for detection and identification of Leptospira spp. Microbiol Immunol. 2001;45:491–6.PubMedGoogle Scholar
- Yamamoto S, Harayama S. PCR amplification and direct sequencing of gyrB genes with universal primers and their application to the detection and taxonomic analysis of Pseudomonas putida strains. Appl Environ Microbiol. 1995;61:1104–9.PubMedGoogle Scholar
- Taylor KA, Barbour AG, Thomas DD. Pulsed-field gel electrophoretic analysis of leptospiral DNA. Infect Immun. 1991;59:323–9.PubMedGoogle Scholar
- Ward MP, Guptill LF, Prahl A, Wu CC. Serovar-specific prevalence and risk factors for leptospirosis among dogs: 90 cases (1997–2002). J Am Vet Med Assoc. 2004;224:1958–63. DOIPubMedGoogle Scholar
- Harkin KR, Roshto YM, Sullivan JT, Purvis TJ, Chengappa MM. Comparison of polymerase chain reaction assay, bacteriologic culture, and serologic testing in assessment of prevalence of urinary shedding of leptospires in dogs. J Am Vet Med Assoc. 2003;222:1230–3. DOIPubMedGoogle Scholar
- Richardson DJ, Gauthier JL. A serosurvey of leptospirosis in Connecticut peridomestic wildlife. Vector Borne Zoonotic Dis. 2003;3:187–93. DOIPubMedGoogle Scholar
- Stamper MA, Gulland FM, Spraker T. Leptospirosis in rehabilitated Pacific harbor seals from California. J Wildl Dis. 1998;34:407–10.PubMedGoogle Scholar
- Gese EM, Schultz RD, Johnson MR, Williams ES, Crabtree RL, Ruff RL. Serological survey for diseases in free-ranging coyotes (Canis latrans) in Yellowstone National Park, Wyoming. J Wildl Dis. 1997;33:47–56.PubMedGoogle Scholar
- Williams DM, Smith BJ, Donahue JM, Poonacha KB. Serological and microbiological findings on 3 farms with equine leptospiral abortions. Equine Vet J. 1994;26:105–8. DOIPubMedGoogle Scholar
- Narita M, Fujitani S, Haake DA, Paterson DL. Leptospirosis after recreational exposure to water in the Yaeyama Islands, Japan. Am J Trop Med Hyg. 2005;73:652–6.PubMedGoogle Scholar
- Guarner J, Johnson BJ, Paddock CD, Shieh WJ, Goldsmith CS, Reynolds MG, Monkeypox transmission and pathogenesis in prairie dogs. Emerg Infect Dis. 2004;10:426–31.PubMedGoogle Scholar
Figures
Tables
Cite This ArticleTable of Contents – Volume 12, Number 7—July 2006
| EID Search Options |
|---|
|
|
|
|
|
|

Please use the form below to submit correspondence to the authors or contact them at the following address:
Toshiyuki Masuzawa, Laboratory of Microbiology and Immunology, Faculty of Pharmaceutical Sciences, Chiba Institute of Science, Shiomi-cho 3, Choshi 288-0025, Japan
Top