Volume 13, Number 6—June 2007
Dispatch
Full Recovery from Baylisascaris procyonis Eosinophilic Meningitis
Cite This Article
Citation for Media
Abstract
Infection by Baylisascaris procyonis is an uncommon but devastating cause of eosinophilic meningitis. We report the first case-patient, to our knowledge, who recovered from B. procyonis eosinophilic meningitis without any recognizable neurologic deficits. The spectrum of illness for this organism may be wider than previously recognized.
Eosinophilic meningitis is defined by >10 eosinophils/mm3 in the cerebrospinal fluid (CSF) or >10% eosinophils of the total CSF leukocyte count. In the United States, the most common cause of eosinophilic meningitis is the presence of a ventriculoperitoneal shunt, but worldwide it is infection by Angiostrongylus cantonensis (1). Other infectious causes of eosinophilic meningitis include Toxocara spp., Gnathostoma spinigerum, neurocysticercosis, and Baylisascaris procyonis. The latter is an intestinal roundworm endemic to the US raccoon population (2). B. procyonis has not been described in New Orleans but is known to occur in raccoons in northern Louisiana (D. Bowman, pers. comm.) and in the nearby states of Texas, Georgia, Oklahoma (2,3), and Mississippi (C. Panuska, unpub. data).
Previously, all reported human cases of B. procyonis eosinophilic meningitis have resulted in death or severe neurologic sequelae. We describe a patient with clinically apparent B. procyonis eosinophilic meningitis, who appears to have completely recovered. This patient’s recovery supports the notion that a wide spectrum of clinical disease exists for this parasite and that it may be a more common human infection than previously recognized.
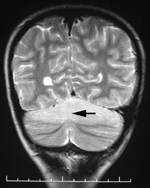
A 4-year-old boy from New Orleans, Louisiana, who had sickle cell disease and a history of a splenectomy, was admitted to our hospital with 1 day of headache, right arm pain, and emesis. He was alert and oriented; his oral temperature was 38°C; and physical examination found only mild upper extremity tremors, dysmetria, and bilateral extensor plantar response. His blood leukocyte count was 16,000/mm3, with 12% eosinophils; blood cultures yielded no growth. During the next 3 days, his headache and vomiting worsened and ataxia developed. Magnetic resonance imaging of the brain, performed on day 5 of illness, demonstrated cerebellar edema (Figure). CSF analysis showed the following: 5 erythrocytes, 1,734 leukocytes/mm3 (55% of which were eosinophils), protein 290 mg/dL, and glucose 53 mg/dL. The boy was given 1 dose of mannitol (0.25 g/kg) and a loading dose of dexamethasone (1 mg/kg), followed by 0.25 mg/kg dexamethasone every 6 hours for 2 weeks. On day 9, a parasitic infection was suspected, and albendazole (10 mg/kg every 12 hours for 5 days) was begun. The boy’s history was negative for travel outside the United States, raw food consumption, household pets, developmental disability, or pica. His mother reported household rodent infestation and fecal droppings on the patient’s bed; raccoons had been seen in the neighborhood, but the boy had not been directly exposed to them. Three days after corticosteroid therapy began, headache and vomiting stopped and only mild ataxia remained. Repeat magnetic resonance imaging and lumbar puncture on day 12 showed improvement in cerebellar edema and CSF eosinophilia (107 leukocytes/mm3 with 6% eosinophils). Upon discharge (day 16), the patient’s only abnormal finding was mild dysmetria of the right hand. One month later he was asymptomatic, and results of a neurologic examination were within normal limits; 24 months later he remained well.
Serologic test results for Toxocara canis (Centers for Disease Control and Prevention, Atlanta, GA, USA), Treponema pallidum, Mycoplasma, Epstein-Barr virus, and lymphocytic choriomeningitis virus were all negative. Acute-phase and convalescent-phase serum specimens (obtained 10 days and 7 weeks after illness onset, respectively) were negative for A. cantonensis (Western blot performed at Mahidol University, Bangkok, Thailand) (4); both were positive for B. procyonis (ELISA performed at Purdue University, West Lafayette, IN, USA) with optical density (OD) values of 0.547 and 0.976, respectively (positive cut-off OD >0.250; K. Kazacos, pers. comm.). CSF (acute specimen only) was negative for A. cantonensis and B. procyonis (OD = 0.006). A stool sample was negative for ova and parasites.
Comprehensive reviews of the epidemiology and clinical features of B. procyonis infection have been recently published (2,3,5,6). The definitive host for this roundworm is the raccoon (Procyon lotor), which each day sheds millions of eggs in feces, which heavily contaminate parks and neighborhoods (7). Humans are infected by ingesting the eggs; the median age of infected humans is 13 months, reflecting the propensity of young children to explore the environment orally (2,3). Subclinical infection has been suggested by a study in Chicago, which found 30 (8%) of 389 children 1–4 years of age were seropositive for B. procyonis, although none had experienced symptoms (8). After B. procyonis larvae hatch, they penetrate the intestinal wall and disseminate; the ensuing manifestations depend on infecting dose, location of migrating larvae, and degree of inflammation produced (2,3). The larvae are not neurotropic, but some may reach the central nervous system and, because of their large size (1.5–2.0 mm), cause major tissue damage (2,3). All previously described 13 patients who had clinically apparent B. procyonis eosinophilic meningitis died or were left with severe neurologic sequelae (Table); to our knowledge, our patient represents the first to fully recover. B. procyonis could cause low-level infections with mild and nonspecific clinical manifestations, similar to covert toxocariasis (9,10), that can go unrecognized. Our patient underwent an extensive evaluation because of his underlying sickle cell disease and the suspicion for a cerebrovascular event; otherwise, his eosinophilic meningitis may have been missed.
Confirmation of B. procyonis infection requires identification of the larvae in tissues. A biopsy specimen was not obtained from our patient because of his benign clinical course; his case thus remains probable, rather than confirmed. Probable cases can be ascertained by a rise in serum or CSF antibody, as detected by an ELISA (11) performed at the Department of Comparative Pathobiology, Purdue University. Our patient’s acute-phase serum sample was moderately positive and the convalescent-phase titer increased, which supports B. procyonis infection. Stool testing, however, is not useful because in humans the parasite does not complete its life cycle and thus does not produce eggs (3).
Treatment with albendazole after egg ingestion but before the onset of symptoms can prevent development of clinical baylisascariasis (2,10). However, after central nervous system symptoms appear, whether albendazole confers clinical benefit or instead worsens outcome due to parasite death and the resultant inflammatory response is unclear. Because of the latter possibility, corticosteroids should be used (3). Whether our patient’s favorable outcome was due to a low burden of infection (as suggested by mild symptoms and modest serum antibody levels), host factors, or prompt initiation of therapy (mannitol, corticosteroids, and albendazole) is not known.
In conclusion, eosinophilic meningitis is a syndrome with many causes; in the United States, an important cause to consider is B. procyonis. All previously reported cases of eosinophilic meningitis resulted in death or severe neurologic disability. We report the likely first case-patient who fully recovered from B. procyonis eosinophilic meningitis. Although the potential for long-term sequelae in this patient is unknown, his short-term recovery has been excellent, and clinical and radiologic improvements suggest resolution of the disease process. This case demonstrates that milder presentations of B. procyonis infection are possible and suggests that infection by this parasite may be more frequent than previously recognized.
Dr Pai is a fellow in pediatric hematology-oncology at Duke University in Durham, North Carolina, USA. Her main research interest is infections in immunocompromised persons.
Acknowledgment
We thank Jennifer Robichaud and Paron Dekumyoy for testing and input in the interpretation of the serologic results for B. procyonis and A. cantonensis, respectively.
References
- Michaels MG. Eosinophilic meningitis. In: Long SS, Pickering LK, Prober CG, editors. Principles and practice of pediatric infectious diseases. 2nd ed. Philadelphia: Churchill Livingston; 2003:312–5.
- Kazacos KR. Baylisascaris procyonis and related species. In: Samuel WM, Pybus MJ, Kocan AA, editors. Parasitic diseases of wild mammals. 2nd ed. Ames (IA): Iowa State University Press; 2001:301–41.
- Murray WJ, Kazacos KR. Raccoon roundworm encephalitis. Clin Infect Dis. 2004;39:1484–92. DOIPubMedGoogle Scholar
- Nuamtanong S. The evaluation of the 29 and 31 kDa antigens in female Angiostrongylus cantonensis for serodiagnosis of human angiostrongyliasis. Southeast Asian J Trop Med Public Health. 1996;27:291–6.PubMedGoogle Scholar
- Sorvillo F, Ash LR, Berlin OG, Morse SA. Baylisascaris procyonis: an emerging helminthic zoonosis. Emerg Infect Dis. 2002;8:355–9. DOIPubMedGoogle Scholar
- Gavin PJ, Kazacos KR, Shulman ST. Baylisascariasis. Clin Microbiol Rev. 2005;18:703–18. DOIPubMedGoogle Scholar
- Roussere GP, Murray WJ, Raudenbush CB, Kutilek MJ, Levee DJ, Kazacos KR. Raccoon roundworm eggs near homes and risk for larva migrans disease, California communities. Emerg Infect Dis. 2003;9:1516–22.PubMedGoogle Scholar
- Brinkman WB, Kazacos KR, Gavin PJ, Binns HJ, Robichaud JD, O’Gorman M, Seroprevalence of Baylisascaris procyonis (raccoon roundworm) in Chicago area children. In: Program and abstracts of the 2003 Annual Meeting of the Pediatric Academic Societies, Seattle, Washington; 2003 May 3–6. Abstract 1872 [cited 2007 Mar 29]. Available from http://www.abstracts2view.com/pasall/authorindex.php)
- Taylor MR, Keane CT, O’Connor P, Mulvihill E, Holland C. The expanded spectrum of toxocaral disease. Lancet. 1988;1:692–4. DOIPubMedGoogle Scholar
- Kazacos KR. Protecting children from helminthic zoonoses. Contemp Pediatr. 2000;17(Suppl):1–24.
- Boyce WM, Asai DJ, Wilder JK, Kazacos KR. Physicochemical characterization and monoclonal and polyclonal antibody recognition of Baylisascaris procyonis larval excretory-secretory antigens. J Parasitol. 1989;75:540–8. DOIPubMedGoogle Scholar
Figure
Table
Cite This ArticleTable of Contents – Volume 13, Number 6—June 2007
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Rodolfo E. Bégué, Children’s Hospital, Infectious Diseases, 200 Henry Clay Ave, New Orleans, LA 70118, USA
Top