Volume 15, Number 2—February 2009
CME ACTIVITY - Research
Face Mask Use and Control of Respiratory Virus Transmission in Households
Cite This Article
Citation for Media
Introduction

Medscape, LLC is pleased to provide online continuing medical education (CME) for this journal article, allowing clinicians the opportunity to earn CME credit. Medscape, LLC is accredited by the Accreditation Council for Continuing Medical Education (ACCME) to provide CME for physicians. Medscape, LLC designates this educational activity for a maximum of 0.75 AMA PRA Category 1 Credits™. Physicians should only claim credit commensurate with the extent of their participation in the activity. All other clinicians completing this activity will be issued a certificate of participation. To participate in this journal CME activity: (1) review the learning objectives and author disclosures; (2) study the education content; (3) take the post-test and/or complete the evaluation at http://www.medscape.com/cme/eid; (4) view/print certificate.
Learning Objectives
Upon completion of this activity, participants will be able to:
• List the nonpharmaceutical strategies that have been examined for respiratory infection control.
• Describe the type of study used to compare the use of face masks with no face masks for respiratory infection control.
• Identify the most frequent viral cause of influenza-like respiratory infection in children.
• Describe adherence to face mask use by adult household contacts of children with viral respiratory infection.
• Describe the efficacy of face mask use for preventing spread of influenza-like infection.
Editor
Beverly Merritt, Technical Writer-Editor, Emerging Infectious Diseases. Disclosure: Beverly Merritt has disclosed no relevant financial relationships.
CME AUTHOR
Désirée Lie, MD, MSEd, Clinical Professor, Family Medicine, University of California, Orange; Director, Division of Faculty Development, UCI Medical Center, Orange, California. Disclosure: Désirée Lie, MD, MSEd, has disclosed no relevant financial relationships.
AUTHORS
Disclosure: Simon Cauchemez, PhD; Dominic E. Dwyer, BSc(Med), MBBS, FRACP, FRCPA, MD; Holly Seale, BSc, PhD; Pamela Cheung, RN; Gary Browne, MBBS; James Wood, BSc, PhD; and Zhanhai Gao, BSc, MSc, PhD, have disclosed no relevant financial relationships. C. Raina MacIntyre, MBBS, FRACP, FAFPHM, M App Epid, PhD, has disclosed that she has received grants for clinical research from 3M. Michael Fasher, MBBS, PhD, has disclosed that he has received grants for educational activities from and has served as an advisor or consultant to GlaxoSmithKline. Robert Booy, MBBS, FRACP, FRCPCH, MSc, MD, has disclosed that he has received grants for clinical research and educational activities from, and has served as an advisor or consultant to, CSL, Roche, Sanofi, GlaxoSmithKline, and Wyeth. All funding received is directed to a research account at The Children’s Hospital at Westmead, Sydney, Australia, and is not personally accepted by Dr. Booy. Neil Ferguson, FmedSci, DPhi, has disclosed that he has served as an advisor or consultant to Crucell Inc.
Abstract
Many countries are stockpiling face masks for use as a nonpharmaceutical intervention to control virus transmission during an influenza pandemic. We conducted a prospective cluster-randomized trial comparing surgical masks, non–fit-tested P2 masks, and no masks in prevention of influenza-like illness (ILI) in households. Mask use adherence was self-reported. During the 2006 and 2007 winter seasons, 286 exposed adults from 143 households who had been exposed to a child with clinical respiratory illness were recruited. We found that adherence to mask use significantly reduced the risk for ILI-associated infection, but <50% of participants wore masks most of the time. We concluded that household use of face masks is associated with low adherence and is ineffective for controlling seasonal respiratory disease. However, during a severe pandemic when use of face masks might be greater, pandemic transmission in households could be reduced. Many countries are stockpiling face masks for use as nonpharmaceutical interventions to reduce viral transmission during an influenza pandemic. We conducted a prospective cluster-randomized trial comparing surgical masks, non–fit-tested P2 masks, and no masks in prevention of influenza-like illness (ILI) in households. During the 2006 and 2007 winter seasons, 286 exposed adults from 143 households who had been exposed to a child with clinical respiratory illness were recruited. Intent-to-treat analysis showed no significant difference in the relative risk of ILI in the mask use groups compared with the control group; however, <50% of those in the mask use groups reported wearing masks most of the time. Adherence to mask use was associated with a significantly reduced risk of ILI-associated infection. We concluded that household use of masks is associated with low adherence and is ineffective in controlling seasonal ILI. If adherence were greater, mask use might reduce transmission during a severe influenza pandemic.
Highly pathogenic avian influenza virus A (H5N1) continues to spread globally, posing a serious human pandemic threat. In the event of an influenza pandemic or other emerging respiratory disease such as severe acute respiratory syndrome (SARS), it is likely that antiviral drugs and vaccines will be in short supply or that delivery could be delayed. Therefore, nonpharmaceutical interventions such as mask use, handwashing, and other hygiene measures or school closure might be effective early control strategies. In contrast to pharmaceutical interventions, little is known about the effectiveness of nonpharmaceutical interventions in the community. A recent analysis gives estimates of the effect of school closure (1), and several prospective, randomized controlled trials of handwashing have been published (2–11). However, clinical trial data on the ability of face masks to reduce respiratory virus transmission in the community are limited to 1 published prospective trial, which showed lack of efficacy (12). In addition, adverse effects of wearing masks (particularly respirators) may affect compliance and effectiveness (13–15). Despite the lack of quantitative evidence, many countries have included recommendations in their pandemic plans on the use of face masks (16–18). We present the results of a cluster-randomized household study of the effectiveness of using face masks to prevent or reduce transmission of influenza-like illness (ILI).
A prospective, cluster-randomized trial of mask use in households was conducted during the 2 winter seasons of 2006 and 2007 (August to the end of October 2006 and June to the end of October 2007) in Sydney, Australia. Enrollment in the study was restricted to households with >2 healthy adults >16 years of age; the adults had known exposure within the household to a child with fever and respiratory symptoms. Suitable households were identified at a pediatric health service comprising the emergency department of a pediatric hospital and a pediatric primary care practice in Sydney, New South Wales, Australia. The study protocol was approved by the local institutional review board.
Randomization and Intervention
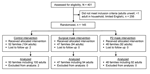
Participating households were randomized to 1 of 3 arms by a secure computerized randomization process: 1) surgical masks (3M surgical mask, catalogue no. 1820; St. Paul, MN, USA) for 2 adults, to be worn at all times when in the same room as the index child, regardless of the distance from the child; 2) P2 masks (3M flat-fold P2 mask, catalogue no. 9320; Bracknell, Berkshire, UK), for 2 adults, to be worn at all times when in the same room as the index child, regardless of the distance from the child; and 3) a control group (no masks used). The P2 masks used have an almost identical specification as N95 masks used in the United States (19). According to New South Wales Health guidelines, pamphlets about infection control were provided to participants in all arms. Study participants and trial staff were not blinded, as it is not technically possible to blind the mask type to which participants were randomized. However, laboratory staff were blinded to the arm of randomization. Figure 1 shows the flow diagram for the trial as suggested by CONSORT guidelines (20).
Recruitment and Follow-up
Children 0–15 years of age seeking treatment at pediatric health services with fever (temperature >37.8oC) and either cough or sore throat were identified by an electronic triage system. Parents or primary caregivers were approached in the waiting room, and that household was invited to join the study if all of the following criteria were satisfied: 1) the household contained >2 adults >16 years of age and 1 child 0–15 years of age; 2) the index child had fever (temperature >37.8oC) and either a cough or sore throat; 3) the child was the first and only person to become ill in the family in the previous 2 weeks; 4) adult caregivers consented to participate in the study; and 5) the index child was not admitted to the hospital.
If eligibility criteria were satisfied, adults from the household were enrolled in the study. Enrolled adults and any siblings of the index child were then evaluated for respiratory symptoms and signs (fever, history of fever or feeling feverish in the past week, myalgia, arthralgia, sore throat, cough, sneezing, runny nose, nasal congestion, headache). If any of these symptoms were present, the family and household were excluded. Sociodemographic and medical information including influenza vaccination history (both the index child and participating adults) was obtained using a researcher-administered questionnaire. Medication use was also recorded. The index case-patient had combined nasal (each nostril) and throat swabs collected for multiplex reverse transcription–PCR (RT-PCR) testing. The household was randomized to 1 of the 3 arms, allocated the appropriate mask type, and educated about infection prevention. Formal fit testing of the P2 masks was not performed, but information pertaining to the correct method for fitting and disposing of the masks was provided. Over the next week, participants were contacted by telephone daily to determine if symptoms had developed and to record adherence to mask use throughout the day.
Each household was supplied with a thermometer to measure the temperature of symptomatic adult participants twice daily. If study staff determined that a participant had developed respiratory disease symptoms at follow-up, a home visit was conducted on the same day and the participant was swabbed and tested for respiratory viruses (see methods described below). Symptomatic participants were then followed up daily for 2 weeks.
Because all respiratory pathogens share similar transmission mechanisms—aerosol, droplet, and fomite spread (although the relative role of these factors may vary among different viruses and in different clinical situations)—we deliberately considered a broad definition of clinical cases consistent with a wide range of common respiratory viruses. Respiratory viruses detected in the study included influenza A and B, respiratory syncytial virus (RSV), adenovirus, parainfluenza viruses (PIV) types 1–3, coronaviruses 229E and OC43, human metapneumovirus (hMPV), enteroviruses, and rhinoviruses.
Adherence to face mask use was specifically monitored during each household follow-up. Measuring adherence and reasons for nonadherence is critical for evaluating the efficacy of mask use for reducing treatment and for providing practical advice on future use of face masks. Exit interviews with participants in the surgical mask and the P2 mask arms were conducted to gain further insights into adherence.
Sample Collection and Laboratory Testing
Rayon-tipped, plastic-shafted swabs were inserted separately into each participant’s nostrils and pharynx, placed into viral transport media, and transported immediately to the laboratory or stored at 4oC if transport was delayed. Nose and throat swabs of index children and adult participants with symptoms of respiratory illness were tested by using nucleic acid and a series of multiplex RT-PCR tests (21) to detect influenza A and B and RSV, PIV types 1–3, picornaviruses (enteroviruses or rhinoviruses), adenoviruses, coronaviruses 229E and OC43, and hMPV.
Case Definition
To include the broadest possible spectrum of clinical syndromes occurring among enrolled adults (22), during follow-up we defined ILI by the presence of fever (temperature >37.8°C), feeling feverish or a history of fever, >2 symptoms (sore throat, cough, sneezing, runny nose, nasal congestion, headache), or 1 of the symptoms listed plus laboratory confirmation of respiratory viral infection. The choice of a relatively broad clinical case definition was dictated by our interest in interrupting transmission of a broad range of respiratory viruses. Laboratory-confirmed cases during the follow-up were defined by the presence of >1 of the symptoms listed above plus laboratory detection of a respiratory virus.
Study Outcomes and Analysis
The primary study outcomes in enrolled adults were the presence of ILI or a laboratory diagnosis of respiratory virus infection within 1 week of enrollment. Given that we demonstrated some dual infections and that there may be a variable sensitivity of RT-PCR for different respiratory viruses, we included all incident infections in adults (by clinical case definition and laboratory testing) in the analysis. We also measured the time from recruitment to infection. Causal linking of the outcomes of ILI and adherence to use of face masks required consideration of the timing of both.
Analysis of primary outcomes was by intention to treat. We performed a multivariate Cox proportional-hazards survival analysis to study secondary outcomes and determine how time lag from recruitment to infection of a secondary case-patient was affected by explanatory covariates (23). Gaussian random effects were incorporated in the model to account for the natural clustering of persons in households (24). The day of infection was reconstructed from the day of symptom onset under the assumption that the incubation period was 1–2 days. To account for exposures that occurred before recruitment, the time when survival analysis started was defined as the maximum value between the day of recruitment minus the incubation period and the start of illness in the index case. (For example, assume a household recruited on day 0 and an incubation period of 2 days. If illness in the index case began on day –3, then the survival analysis began on day –2; if illness in the index case began on day –1, then the survival analysis began the same day.)
The following variables were included in the models: daily adherence to use of P2 or surgical masks, number of adults in the household, number of siblings in the household, and index case <5 years of age. This analysis was performed using the survival package of the statistical software R (www.r-project.org). Comparisons among groups were made with the Fisher exact test for categorical variables. A 2-sided p value <0.05 was considered significant.
Power Analysis
Assuming a secondary attack rate in exposed adults of 20% and an intraclass correlation coefficient of 30%, we estimated that 94 adults would be needed in each arm of the study to show efficacy of >75% of P2 or surgical masks at 80% power and with a p value of 0.05. Our efficacy estimate was a conservative assumption based on observational data for the combined effects of all mask types during the SARS epidemic in Hong Kong (25).
Study Population
We recruited 290 adults from 145 families; 47 households (94 enrolled adults and 180 children) were randomized to the surgical mask group, 46 (92 enrolled adults and 172 children) to the P2 mask group, and 52 (104 enrolled adults and 192 children) to the no-mask (control) group. Two families in the control group were lost to follow-up during the study. Characteristics of the families who participated are shown in Table 1, with no significant differences noted among the 3 arms.
Samples were collected from 141 children; respiratory viruses were detected in 90 (63.8%) children. In 79 (56.0%) of 141 cases, a single pathogen was detected: influenza A in 19/141 (13.5%); influenza B in 7/141 (4.9%); adenoviruses in 7/141 (4.9%); RSV in 5/141 (3.5%); PIV in 8/141 (5.5%) (PIV-1 in 1/141 [0.70%]; PIV-2 in 2/141 [1.4%]; PIV-3 in 5/141 [3.5%]); hMPV in 8/141 (5.7%); and coronavirus OC43 in 3/141 (2.1%). Other viruses detected included picornaviruses in 22/141 (15.6%): rhinoviruses in 11/22 (50.0%); enteroviruses in 5/22 (22.7%) (enterovirus 68 in 1/5 [20.0%] and others in 4/5 [80.0%]); and uncharacterized nonsequenced picornaviruses in 6/22 (27.0%). An additional 11 children (7.8%) had dual or co-infection: 4 (2.8%) with adenovirus and rhinovirus, 2 (1.4%) with rhinovirus and coronavirus; and 1 each with influenza A and enterovirus, influenza A and PIV-2, influenza A and rhinovirus, RSV and enterovirus, and adenovirus and hMPV.
Adherence
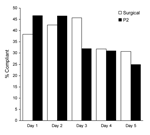
Characteristics of the adherent versus nonadherent participants who were recruited are shown in Table 2; no significant differences were noted between the 2 groups except for the presence of >3 adults in the household. On day 1 of mask use, 36 (38%) of the 94 surgical mask users and 42 (46%) of the 92 P2 mask users stated that they were wearing the mask “most or all” of the time. Other participants were wearing face masks rarely or never. The difference between the groups was not significant (p = 0.37). Adherence dropped to 29/94 (31%) and 23/92 (25%), respectively, by day 5 of mask use (Figure 2).
Table 3 shows reported problems with mask use. There were no significant differences in difficulties with mask use between the P2 and surgical mask groups, but >50% reported concerns, the main one being that wearing a face mask was uncomfortable. Other concerns were that the child did not want the parent wearing a mask and the parent forgot to wear the mask. Additional comments made by some included that the mask did not fit well and that it was not practical to wear at meal time or while asleep. Some adults wore the mask during the day but not at night, even though the sick child was sleeping beside them in their bed.
Intention-to-Treat Analysis
ILI was reported in 21/94 (22.3%) in the surgical group, 14/92 (15.2%) in the P2 group, and 16/100 (16.0%) in the control group, respectively. Samples were collected from 43/51 (84%) sick adults, with respiratory viruses isolated in 17/43 (40%) sick adults. Viral pathogens were isolated from 6/94 (6.4%) in the surgical mask group, 8/92 (8.7%) in the P2 group, and 3/100 (3.0%) in the control group. In 10/17 laboratory-positive cases, the same respiratory virus was isolated in the adult and the child (surgical, 3/94; P2 group, 5/92; and control, 2/100). In 2 cases, the adult was the only person with a laboratory-confirmed virus (1 each from the P2 and surgical groups); in the remaining 5 adults, the virus detected in the child differed from that in the adult (surgical, 2; P2 group, 2; and control group, 1). No dual infections were detected in the adults. Intention-to-treat analysis by households and by participants showed no significant difference between the groups (Table 4).
Risk Factors for ILI
Under the assumption that the incubation period is equal to 1 day (the most probable value for the 2 most common viruses isolated, influenza [21] and rhinovirus [26]), adherent use of P2 or surgical masks significantly reduces the risk for ILI infection, with a hazard ratio equal to 0.26 (95% CI [confidence interval] 0.09–0.77; p = 0.015). No other covariate was significant. Under the less likely assumption that the incubation period is equal to 2 days, the quantified effect of complying with P2 or surgical mask use remains strong, although borderline significant; hazard ratio was 0.32 (95% CI 0.11–0.98; p = 0.046). The study was underpowered to determine if there was a difference in efficacy between P2 and surgical masks (Table 5).
We present the results of a prospective clinical trial of face mask use conducted in response to an urgent need to clarify the clinical benefit of using masks. The key findings are that <50% of participants were adherent with mask use and that the intention-to-treat analysis showed no difference between arms. Although our study suggests that community use of face masks is unlikely to be an effective control policy for seasonal respiratory diseases, adherent mask users had a significant reduction in the risk for clinical infection. Another recent study that examined the use of surgical masks and handwashing for the prevention of influenza transmission also found no significant difference between the intervention arms (12).
Our study found that only 21% of household contacts in the face mask arms reported wearing the mask often or always during the follow-up period. Adherence with treatments and preventive measures is well known to vary depending on perception of risk (27) and would be expected to increase during an influenza pandemic. During the height of the SARS epidemic of April and May 2003 in Hong Kong, adherence to infection control measures was high; 76% of the population wore a face mask, 65% washed their hands after relevant contact, and 78% covered their mouths when sneezing or coughing (28). In addition, adherence may vary depending on cultural context; Asian cultures are more accepting of mask use (29). Therefore, although we found that distributing masks during seasonal winter influenza outbreaks is an ineffective control measure characterized by low adherence, results indicate the potential efficacy of masks in contexts where a larger adherence may be expected, such as during a severe influenza pandemic or other emerging infection.
We estimated that, irrespective of the assumed value for the incubation period (1 or 2 days), the relative reduction in the daily risk of acquiring a respiratory infection associated with adherent mask use (P2 or surgical) was in the range of 60%–80%. Those results are consistent with those of a simpler analysis in which persons were stratified according to adherence (Technical Appendix). We emphasize that this level of risk reduction is dependent on the context, namely, adults in the household caring for a sick child after exposure to a single index case. We urge caution in extrapolating our results to school, workplace, or community contexts, or where multiple, repeated exposures may occur, such as in healthcare settings. The exact mechanism of potential clinical effectiveness of face mask use may be the prevention of inhalation of respiratory pathogens but may also be a reduction in hand-to-face contact. Our study could not determine the relative contributions of these mechanisms. In this study, it is only possible to talk about a statistical association between adherent mask use and reduction in the risk of ILI-infection. The causal link cannot be demonstrated because adherence was not randomized in the trial. Although we found no significant difference in handwashing practices between adherent and non-adherent mask users, it is possible that adherent mask use is correlated with other, unobserved variables that reduce the risk of infection. Further work will therefore be needed to definitively demonstrate that adherent mask use reduces the risk of ILI-infection.
In our study, fit testing for P2 masks was not conducted because this is unlikely to be feasible in the general community during a pandemic. As such, we felt it was more appropriate to determine the efficacy of non–fit-tested masks. We found no difference in adherence between P2 and surgical masks, an important finding, as there is a common belief among healthcare workers that P2 masks are less comfortable. The size of the study did not permit conclusive comparison of the relative efficacy of P2 masks and surgical masks. Given the 5- to 10-fold cost difference between the 2 mask types, quantifying any difference in efficacy between surgical masks and particulate respirators remains a priority that needs to be addressed by a larger trial.
A possible limitation of the study is that some adults may have been incubating infection at the time of enrollment. However, this effect would have biased the results toward the null in the intention-to-treat analysis. The survival analysis explicitly accounted for the existence of a fixed incubation period and incubating infections at the time of enrollment. A potential alternative study design would be to enroll participants from asymptomatic households, do follow-up for development of infection, and then immediately intervene with masks. For such a design, given that only 15%–20% of closely exposed adults will develop illness after exposure to an ill child, thousands of households (rather than hundreds) would be required to afford the same study power. In addition, such a design would have been fraught with underascertainment of incident infections and delayed implementation of mask intervention. We believe ours is a more efficient design. A further limitation is that some parents may have acquired infection outside the home. We identified 5 child–parent pairs with discordant viral infections. The randomization process should have ensured that outside exposure was equally distributed between arms, and this effect would have biased the results toward the null.
In retrospect, relying on laboratory-confirmed cases as the primary outcome may have been unrealistic for a study of this size. ILI in enrolled adults was 17.1%, but laboratory confirmation was modest; the virus was identified in only 34.7% of adult ILI cases (the rate of laboratory diagnosis in children was high at 63.8%). However, even intention-to-treat analysis using ILI outcome shows no significant difference between the groups. We used self-reporting to determine adherence; previous research indicates that patient self-reporting is more reliable than judgments by doctors or nurses when compared against urine drug levels (30). In addition, the significant association between adherence and clinical protection provides internal validation of self-reporting as a measure.
An important aspect of this study is that we included respiratory viruses other than influenza. Although these viruses may differ in their relative dependence (accurate quantitation of this relativity is uncertain for the various viruses) on different transmission mechanisms (i.e., large droplet, aerosol, or fomite), all are transmitted by the respiratory route. Therefore, face mask use should have some effect on virus transmission (e.g., interference with hand-nose contact), given that participants in all arms of the study received the same infection control advice. In addition, we argue that assessing multiple respiratory viruses allows our results to be generalized more broadly to other infections, including new respiratory viruses that may emerge in the future. Conversely, the low rate of confirmed influenza A or B infection (18.4%) in the study could mean that our findings are not directly applicable to a scenario in which influenza predominates. If influenza is more likely than the other viruses in our study to be transmitted by the respiratory route, the prevalence of mixed infections would tend to bias our results toward the null. However, it is possible that a pandemic strain may have different transmission characteristics than seasonal strains as demonstrated by attack rates in different age groups in pandemics compared with seasonal outbreaks and by the detection of influenza virus in different clinical samples in human influenza virus A (H5N1) cases.
Results of our study have global relevance to respiratory disease control planning, especially with regard to home care. During an influenza pandemic, supplies of antiviral drugs may be limited, and there will be unavoidable delays in the production of a matched pandemic vaccine (31). For new or emerging respiratory virus infections, no pharmaceutical interventions may be available. Even with seasonal influenza, widespread oseltamivir resistance in influenza virus A (H1N1) strains have recently been reported (32). Masks may therefore play an important role in reducing transmission.
Dr MacIntyre is head of the School of Public Health and Community Medicine at the University of New South Wales, Australia, and professor of Infectious Diseases Epidemiology. Her research interests include the detailed understanding of the transmission dynamics and prevention of infectious diseases, particularly respiratory pathogens such as influenza, tuberculosis, and other vaccine-preventable infections.
Acknowledgments
We thank John Horvath, Chief Medical Officer of Australia, for providing us with the opportunity to respond to an urgent policy need for obtaining evidence on the efficacy of using face masks. Thanks also to Noemie Ovdin, Linda Donovan, Sophie Branch, Ken McPhie, and Mala Ratnamohan for laboratory testing; Terence Campbell for comments on the manuscript; and the staff of the Emergency Department at the Children’s Hospital Westmead and of the primary care practice of Michael Fasher for assisting with the recruitment of study participants.
The Office of Health Protection, Department of Health and Ageing, Australia, 3M Australia, and Medical Research Council (UK) provided funding for this trial. The National Health and Medical Research Council and the School of Pediatrics and Child Health, University of Sydney provided salary support.
References
- Cauchemez S, Valleron A-J, Boelle P-Y, Flahault A, Ferguson NM. Estimating the impact of school closure on influenza transmission from sentinel data. Nature. 2008;452:750–4. DOIPubMedGoogle Scholar
- Rabie T, Curtis V. Handwashing and risk of respiratory infections: a quantitative systematic review. Trop Med Int Health. 2006;11:258–67. DOIPubMedGoogle Scholar
- Larson E, Aiello A, Lee LV, Della-Latta P, Gomez-Duarte C, Lin S. Short- and long-term effects of handwashing with antimicrobial or plain soap in the community. J Community Health. 2003;28:139–50. DOIPubMedGoogle Scholar
- Larson EL, Lin SX, Gomez-Pichardo C, Della-Latta P. Effect of antibacterial home cleaning and handwashing products on infectious disease symptoms: a randomized, double-blind trial. Ann Intern Med. 2004;140:321–9.PubMedGoogle Scholar
- Luby SP, Agboatwalla M, Feikin DR, Painter J, Billhimer W, Altaf A, Effect of handwashing on child health: a randomized controlled trial. Lancet. 2005;366:225–33. DOIPubMedGoogle Scholar
- Luby SP, Agboatwalla M, Painter J, Altaf A, Billhimer WL, Hoekstra RM. Effect of intensive handwashing promotion on childhood diarrhea in high-risk communities in Pakistan: a randomized controlled trial. JAMA. 2004;291:2547–54. DOIPubMedGoogle Scholar
- Black RE, Dykes AC, Anderson KE, Wells JG, Sinclair SP, Gary GW Jr, Handwashing to prevent diarrhea in day-care centers. Am J Epidemiol. 1981;113:445–51.PubMedGoogle Scholar
- Girou E, Loyeau S, Legrand P, Oppein F, Brun-Buisson C. Efficacy of handrubbing with alcohol-based solution versus standard handwashing with antiseptic soap: randomized clinical trial. BMJ. 2002;325:362. DOIPubMedGoogle Scholar
- Le CT. Statistical comparison of two handwashing protocols. Stat Med. 1986;5:393–6. DOIPubMedGoogle Scholar
- Pereira LJ, Lee GM, Wade KJ. An evaluation of five protocols for surgical handwashing in relation to skin condition and microbial counts. J Hosp Infect. 1997;36:49–65. DOIPubMedGoogle Scholar
- Slota M, Green M, Farley A, Janosky J, Carcillo J. The role of gown and glove isolation and strict handwashing in the reduction of nosocomial infection in children with solid organ transplantation. Crit Care Med. 2001;29:405–12. DOIPubMedGoogle Scholar
- Cowling BJ, Fung ROP, Cheng CKY, Fang VJ, Chan KH, Seto WH, Preliminary findings of a randomized trial of non-pharmaceutical interventions to prevent influenza transmission in households. PLoS One. 2008;3:e2101. DOIPubMedGoogle Scholar
- Kao T-W, Huang K-C, Huang Y-L, Tsai T-J, Hsieh B-S, Wu M-S. The physiological impact of wearing an N95 mask during hemodialysis as a precaution against SARS in patients with end-stage renal disease. J Formos Med Assoc. 2004;103:624–8.PubMedGoogle Scholar
- Lim ECH, Seet RCS, Lee KH, Wilder-Smith EPV, Chuah BYS, Ong BKC. Headaches and the N95 face-mask amongst healthcare providers. Acta Neurol Scand. 2006;113:199–202. DOIPubMedGoogle Scholar
- Mardimae A, Slessarev M, Han J, Sasano H, Sasano N, Azami T, Modified N95 mask delivers high inspired oxygen concentrations while effectively filtering aerosolized microparticles. Ann Emerg Med. 2006;48:391–9. DOIPubMedGoogle Scholar
- Department of Health and Human Services. HHS pandemic influenza plan. Washington: The Department; 2005.
- Australian health management plan for pandemic influenza: important information for all Australians. Canberra: Department of Health and Ageing, Commonwealth of Australia; 2006.
- National plan for the prevention and control of influenza pandemic. Paris: General Secretariat for National Defence; 2007.
- 3M technical update: P2 respirators vs. N95 respirators. 3M Australia; 2005 [cited 2008 Dec 29]. Available from http://multimedia.mmm.com/mws/mediawebserver.dyn?6666660Zjcf6IVs66S4wScOrrrrQ
- Campbell MK, Elbourne DR, Altman DG. CONSORT statement: extension to cluster randomized trials. BMJ. 2004;328:702–8. DOIPubMedGoogle Scholar
- Druce J, Tran T, Kelly H, Kaye M, Chibo D, Kostecki R, Laboratory diagnosis and surveillance of human respiratory viruses by PCR in Victoria, Australia, 2002–2003. J Med Virol. 2005;75:122–9. DOIPubMedGoogle Scholar
- Carrat F, Sahler C, Rogez S, Leruez-Ville M, Freymuth F, Le Gales C, Influenza burden of illness: estimates from a national prospective survey of household contacts in France. Arch Intern Med. 2002;162:1842–8. DOIPubMedGoogle Scholar
- Viboud C, Boelle P-Y, Cauchemez S, Lavenu A, Valleron A-J, Flahault A, Risk factors of influenza transmission in households. Br J Gen Pract. 2004;54:684–9.PubMedGoogle Scholar
- Therneau TM, Grambsch P. Statistics for biology and health: modelling survival data—extending the Cox model. New York: Springer; 2006.
- Seto WH, Tsang D, Yung RWH, Ching TY, Ng TK, Ho M, Effectiveness of precautions against droplets and contact in prevention of nosocomial transmission of severe acute respiratory syndrome (SARS). Lancet. 2003;361:1519–20. DOIPubMedGoogle Scholar
- Harris JM II, Gwaltney JM Jr. Incubation periods of experimental rhinovirus infection and illness. Clin Infect Dis. 1996;23:1287–90. DOIPubMedGoogle Scholar
- Cava MA, Fay KE, Beanlands HJ, McCay EA, Wignall R. Risk perception and compliance with quarantine during the SARS outbreak. J Nurs Scholarsh. 2005;37:343–7. DOIPubMedGoogle Scholar
- Lo JYC, Tsang THF, Leung Y-H, Yeung EYH, Wu T, Lim WWL. Respiratory infections during SARS outbreak, Hong Kong, 2003. Emerg Infect Dis. 2005;11:1738–41. DOIPubMedGoogle Scholar
- Syed Q, Sopwith W, Regan M, Bellis MA. Behind the mask. Journey through an epidemic: some observations of contrasting public health responses to SARS. J Epi Comm Health. 2003;2003:855–6. DOIGoogle Scholar
- Macintyre CR, Goebel K, Brown GV. Patient knows best: blinded assessment of nonadherence with antituberculous therapy by physicians, nurses, and patients compared with urine drug levels. Prev Med. 2005;40:41–5. DOIPubMedGoogle Scholar
- Booy R, Brown LE, Grohmann GS, Macintyre CR. Pandemic vaccines: promises and pitfalls. Med J Aust. 2006;185(Suppl):S62–5.PubMedGoogle Scholar
- World Health Organization. Influenza A (H1N1) virus resistance to oseltamivir—last quarter 2007 to 2 June 2008 [cited 2008 Aug 29]. Available from http://www.who.int/csr/disease/influenza/oseltamivir_summary/en/index.html
Figures
Tables
Follow Up
Earning CME Credit
To obtain credit, you should first read the journal article. After reading the article, you should be able to answer the following, related, multiple-choice questions. To complete the questions and earn continuing medical education (CME) credit, please go to http://www.medscape.com/cme/eid. Credit cannot be obtained for tests completed on paper, although you may use the worksheet below to keep a record of your answers. You must be a registered user on Medscape.com. If you are not registered on Medscape.com, please click on the New Users: Free Registration link on the left hand side of the website to register. Only one answer is correct for each question. Once you successfully answer all post-test questions you will be able to view and/or print your certificate. For questions regarding the content of this activity, contact the accredited provider, CME@medscape.net. For technical assistance, contact CME@webmd.net. American Medical Association’s Physician’s Recognition Award (AMA PRA) credits are accepted in the US as evidence of participation in CME activities. For further information on this award, please refer to http://www.ama-assn.org/ama/pub/category/2922.html. The AMA has determined that physicians not licensed in the US who participate in this CME activity are eligible for AMA PRA Category 1 Credits™. Through agreements that the AMA has made with agencies in some countries, AMA PRA credit is acceptable as evidence of participation in CME activities. If you are not licensed in the US and want to obtain an AMA PRA CME credit, please complete the questions online, print the certificate and present it to your national medical association.
Title: Face Mask Use and Control of Respiratory Virus Transmission in Households
CME Questions
1. Which of the following is least likely to be a nonpharmaceutical strategy examined and reported for the prevention of influenza-like infection (ILI) during an influenza pandemic?
A. School closure
B. Use of face masks
C. Handwashing
D. Quarantine at home
2. Which of the following best describes the type of study used to examine the efficacy of face masks in respiratory infection control at home?
A. Retrospective case-control study
B. Prospective cluster-randomized study
C. Prospective case-control study
D. Observational case series
3. Which of the following is the most common single viral respiratory pathogen to be isolated from 141 children with respiratory viral illness in the study reported?
A. Influenza B
B. Influenza A
C. Adenovirus
D. Respiratory syncytial virus
4. Which of the following best describes the adherence rate for P2 face masks on day 5, after beginning the use of face masks by household adult contacts for household infection control?
A. 25%
B. 31%
C. 36%
D. 46%
5. Which of the following best describes the hazard ratio for risk for transmission of ILI if adherence to face mask use was 100%?
A. 1.00
B. 0.85
C. 0.47
D. 0.26
Activity Evaluation
|
1. The activity supported the learning objectives. |
||||
|
Strongly Disagree |
|
|
|
Strongly Agree |
|
1 |
2 |
3 |
4 |
5 |
|
2. The material was organized clearly for learning to occur. |
||||
|
Strongly Disagree |
|
|
|
Strongly Agree |
|
1 |
2 |
3 |
4 |
5 |
|
3. The content learned from this activity will impact my practice. |
||||
|
Strongly Disagree |
|
|
|
Strongly Agree |
|
1 |
2 |
3 |
4 |
5 |
|
4. The activity was presented objectively and free of commercial bias. |
||||
|
Strongly Disagree |
|
|
|
Strongly Agree |
|
1 |
2 |
3 |
4 |
5 |
Related Links
Table of Contents – Volume 15, Number 2—February 2009
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
C. Raina MacIntyre, School of Public Health and Community Medicine, Faculty of Medicine, The University of New South Wales, Sydney, NSW, 2052 Australia
Top