Volume 17, Number 11—November 2011
THEME ISSUE
CHOLERA IN HAITI
Dispatch
Knowledge, Attitudes, and Practices Related to Treatment and Prevention of Cholera, Haiti, 2010
Cite This Article
Citation for Media
Abstract
In response to the recent cholera outbreak, a public health response targeted high-risk communities, including resource-poor communities in Port-au-Prince, Haiti. A survey covering knowledge and practices indicated that hygiene messages were received and induced behavior change, specifically related to water treatment practices. Self-reported household water treatment increased from 30.3% to 73.9%.
Haiti had not experienced an outbreak of cholera for more than half a century. This changed in October 2010 when a large outbreak occurred in Artibonite Department and quickly spread to the remaining departments of Haiti, including the city of Port-au-Prince (1). Given the prevalence of known risk factors for explosive spread of the disease (e.g., low socioeconomic status, high population density), an emergency public health response was initiated. With crowded conditions and limited access to safe water and sanitation, persons living in the capital of Port-au-Prince were especially vulnerable to acquiring cholera (2–5). This risk was exacerbated by the January 12, 2010, earthquake, which led to >1.5 million persons seeking shelter and services at internally displaced persons settlements in and around the capital (6). The first cases were confirmed in Port-au-Prince on November 7, 2010. As of August 8, 2011, Port-au-Prince had reported 112,464 cholera cases and 760 deaths (6).
In response to the cholera outbreak, the Haiti government and partner agencies initiated emergency public health response activities aimed at treating suspected cholera cases and preventing new ones. Response activities included mass media cholera campaigns through radio and hygiene promotion activities by community health workers, distribution of water purification tablets and soap, and limited distribution of oral rehydration solution (ORS) sachets. Prevention efforts focused on internally displaced person settlements in Port-au-Prince and the poorer neighborhoods of the city where information regarding cholera knowledge, dissemination of cholera information, and distribution of treatment and prevention supplies was limited.
During December 6–7 and 14–16, 2010, we conducted a survey to assess the effectiveness of interventions implemented to prevent the spread of cholera and to improve specific response activities in these neighborhoods. Because this investigation was a public health response to an emergency, the Centers for Disease Control and Prevention determined that institutional review board review was not necessary. Informed consent was obtained from all participants.
The survey collected cross-sectional data on household demographics, communications preferences, knowledge of cholera transmission and prevention, water sources and treatment, and hygiene practices. Samples of stored water in the home were tested for chlorine residue by using the Hach Free Chlorine Test (Hach Co., Loveland, CO, USA) to provide an objective measure of water treatment. Microbiological testing for Escherichia coli by using IDEXX Quanti-Tray/2000 (IDEXX Laboratories, Inc., Westbrook, ME, USA) was also conducted on source water. Sampling weights according to the population size were used to improve the overall representativeness of results.
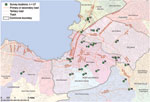
A household questionnaire (Technical Appendix) was pilot tested and administered to 405 households from 27 clusters from resources-limited areas of Cité Soleil, Delmas, Carrefour, and Pétion-Ville (Figure). Clusters were randomly selected by using population proportional to size sampling, with the exception of Cité Soleil, which was undersampled to provide more geographic representation in the sample. In each of the 27 selected clusters, 15 households were selected randomly along a radius from the edge to the center of the cluster.
Persons interviewed were primarily female heads of households (81%). Average household size was 5 persons, and median age of respondents was 35 years (range 17–80 years). Most respondents had access to a cellular telephone (88.1%), radio (67.1%), and television (66.3%). The preferred forms of communication for receiving cholera messages were television (71.1%), radio (68.8%), and trucks with megaphones (44.0%). Knowledge of common signs of cholera was high; the 2 most common signs described were diarrhea (89.1%) and vomiting (83.4%). Respondents also showed high knowledge of transmission modes; 71.9% indicated consumption of contaminated water and 61.4% indicated consumption of contaminated food. The most common prevention method cited was handwashing (86.0%).
Before the outbreak, the most common drinking water sources were piped water to tap stands and public kiosks (Table 1). These water sources were chlorinated irregularly, and only 6.2% of respondents believed that drinking water from the piped supplies was safe. Microbiological testing of 11 unchlorinated piped water sources indicated that 7 were positive for an indicator of fecal contamination (E. coli). Collection of tap water decreased during the cholera outbreak, whereas collection of drinking water from private kiosks nearly doubled (47.6%). Public health messages on the health benefits of water treatment showed diffusion in these neighborhoods; water treatment practices increased from 30.3% before the cholera outbreak to 73.9% after the outbreak (p<0.05), and the 2 most common methods used were water purification tablets (66.6%) and bleach (57.7%) (Table 1). Water purification tablets were considered palatable by most respondents (87.7%), and 70.2% reported purchasing them in the past month (Table 2).
Among 403 (99.5%) households, ≈60% of samples from stored drinking water tested positive for residual chlorine (range 0–3.5 mg/L). Additionally, during the survey administration, nearly all (94.4%) water storage containers had a cover on them that could reduce the chance of contamination.
Hygienic practices (e.g., handwashing and latrine use) are critical for preventing the spread of diarrheal diseases (7–10). Active acceptance of these practices and use of soap was high among respondents. Approximately 94.1% reported washing their hands with soap; 84.1% reported having access to soap, 95.7% reported purchasing soap, and 16.5% reported receiving soap from a distribution location since the outbreak started (Table 2). Use of improved latrines was also reported by most respondents (74.0%).
ORS is a lifesaving therapy for diarrheal diseases, including cholera (11). Nearly 90% of respondents stated that they knew the method of ORS preparation, although only 76.0% of respondents indicated the correct volume of water needed to prepare an ORS sachet as recommended by the World Health Organization (12). One fourth of respondents had ORS in their home when the survey was conducted.
This investigation had several limitations. Because of security restrictions, independent enumerators could not be used. Therefore, some of the enumerators were persons who participated in the implementation of the cholera prevention activities in these communities. Their presence might have biased certain respondent answers. Additionally, sampling was based on available population data from the 2003 census. Migration is likely to have occurred after the earthquake and might have resulted in nonproportional sampling. Finally, sanitation is a sensitive subject within Haitian culture; thus, self-reported access to latrines might be exaggerated. Despite these limitations, the survey provided valuable information reflecting the impact of the public health response to the outbreak and identified areas for improvement.
Overall, the knowledge of cholera symptoms, prevention, treatment, and modes of transmission indicated that public health messages had been effective. Cholera messaging was successful in promoting behavior changes to address the threat of cholera, especially in increasing acceptance of drinking chlorinated water. Recommendations include additional education campaigns to improve knowledge of correct dosing of water with water purification tablets, ORS preparation, and cholera-prevention methods. Additional follow-up is needed to ensure wide-scale availability of household water treatment products and instruction on proper dosing. Public health officials should take advantage of the substantial interest in and acceptance of chemical water treatment and develop sustainable household water treatment programs. More importantly, a concerted effort should be made to improve the safety of water sources through infrastructure upgrades and improved treatment practices. These upgrades would spur timely sanitary reform and improvements to the public health system of Haiti, which occurred over a century ago in Europe, North America, and most recently in Latin America after the introduction of cholera in the 1990s (13,14).
Dr Beau De Rochars is an Epidemic Intelligence Service (EIS) officer at the Centers for Disease Control and Prevention in the EIS Field Assignments Branch stationed in the Florida Department of Health. His major research interests include emerging and zoonotic infectious diseases and vector-borne pathogens.
Acknowledgment
We thank Thomas Bender, Randall Young, Emmanuel Rossignol, Patrice Joseph, Anna Newton, and Group de Recherche et d’Echanges Technologiques staff for their contributions to this project.
References
- Centers for Disease Control and Prevention. Update: cholera outbreak—Haiti, 2010. MMWR Morb Mortal Wkly Rep. 2010;59:1473–9.PubMedGoogle Scholar
- Weber JT, Mintz ED, Canizares R, Semiglia A, Gomez I, Sempertegui R, Epidemic cholera in Ecuador: multidrug-resistance and transmission by water and seafood. Epidemiol Infect. 1994;112:1–11. DOIPubMedGoogle Scholar
- Swerdlow DL, Malenga G, Begkoyian G, Nyangulu D, Toole M, Waldman RJ, Epidemic cholera among refugees in Malawi, Africa: treatment and transmission. Epidemiol Infect. 1997;118:207–14. DOIPubMedGoogle Scholar
- Swerdlow DL, Mintz ED, Rodriguez M, Tejada E, Ocampo C, Espeje L, Waterborne transmission of epidemic cholera in Trujillo, Peru: lessons for a continent at risk. Lancet. 1992;340:28–33. DOIPubMedGoogle Scholar
- Ries AA, Vugia DJ, Beingolea L, Palacios AM, Vasquez E, Wells JG, Cholera in Piura, Peru: a modern urban epidemic. J Infect Dis. 1992;166:1429–33. DOIPubMedGoogle Scholar
- Haitian Ministry of Public Health and Population [cited 2011 Jul 28]. http://www.mspp.gouv.ht/site/index.php?option=com_content&view=article&id=57&Itemid=1
- DuBois AE, Sinkala M, Kalluri P, Makasa-Chikoya M, Quick RE. Epidemic cholera in urban Zambia: hand soap and dried fish as protective factors. Epidemiol Infect. 2006;134:1226–30. DOIPubMedGoogle Scholar
- Hutin Y, Luby S, Paquet C. A large cholera outbreak in Kano City, Nigeria: the importance of hand washing with soap and the danger of street-vended water. J Water Health. 2003;1:45–52. PubMedGoogle Scholar
- Curtis V, Cairncross S. Effect of washing hands with soap on diarrhoea risk in the community: a systematic review. Lancet Infect Dis. 2003;3:275–81. DOIPubMedGoogle Scholar
- Ejemot RI, Ehiri JE, Meremikwu MM, Critchley JA. Hand washing for preventing diarrhoea. Cochrane Database Syst Rev. 2008;CD004265. PubMedGoogle Scholar
- Victora CG, Bryce J, Fontaine O, Monasch R. Reducing deaths from diarrhoea through oral rehydration therapy. Bull World Health Organ. 2000;78:1246–55.PubMedGoogle Scholar
- World Health Organization. Guidelines for cholera control. Geneva. Organization. 1993;▪▪▪:20–2.
- Sepúlveda J, Valdespino JL, Lourdes García-García L. Cholera in Mexico: the paradoxical benefits of the last pandemic. Int J Infect Dis. 2006;10:4–13. DOIPubMedGoogle Scholar
- Harris JB, LaRocque RC, Charles RC, Muazumder RN, Khann AI, Bardhan PK. Cholera’s western front. Lancet. 2010;376:1961–5. DOIPubMedGoogle Scholar
Figure
Tables
Cite This ArticleTable of Contents – Volume 17, Number 11—November 2011
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Valery E.M. Beau De Rochars, 4052 Bald Cypress Way, Bin #A-12, Tallahassee, FL 32399, USA
Top