Volume 2, Number 4—October 1996
Dispatch
Assessing the Costs and Benefits of an Oral Vaccine for Raccoon Rabies: A Possible Model
Cite This Article
Citation for Media
Abstract
Any cost-benefit analysis of the use of an oral vaccine to control raccoon rabies should include calculating both costs and benefits in terms of $/unit area. Further, cost savings must be adjusted to match the stages of an epizootic: pre-epizootic, epizootic, and post-epizootic. A generic model, which can be adapted to different sites, illustrates the use of threshold analysis to link distribution costs, cost savings, bait density, and vaccine price. Initial results indicate the need to lower the cost of the vaccine, continue research to determine optimal bait densities, and examine distribution plans that do not require continued protection of areas in which raccoon rabies was eliminated through previous vaccination programs.
Over the past 30 years, reported cases of animal rabies in the United States have increased, from fewer than 5,000 per year in the early 1960s to almost 10,000 per year in the mid-1990s (1,2). Most of the increase is attributable to the spread of raccoon rabies from Florida to the northeastern states (1). The impact of this epizootic has been considerable. For example, hospitals in Connecticut reported a 2,000% increase in the annual number of postexposure rabies prophylaxis treatments after raccoon rabies was first detected in the state in 1991 (3). Postexposure prophylaxis costs $2,000 to $3,000, or more, per person (3,4). In addition, a raccoon rabies epizootic increases other costs, including those associated with animal control and laboratory diagnosis (5; Tysmans, J., Costs of rabies in Cumberland County, NC: 1993 and 7/1/94-6/30/95 [MPH thesis], Chapel Hill (NC): Dept. of Health Policy and Admin., Univ. of North Carolina, Chapel Hill, 1996).
Oral vaccines offer a potential solution to rabies in wildlife populations (6,7). The spread of rabies in foxes in an area of Switzerland was halted when an oral vaccine was used to vaccinate 60% of the fox population (8). An oral vaccine to control raccoon rabies (9) is undergoing evaluation in New York and Massachusetts (10,11). Also, large-scale programs are using an oral vaccine against rabies in coyote and gray fox populations in Texas (12).
Uhaa et al. (5) examined the economics of using an oral vaccine in Hunterdon and Warren Counties, New Jersey. However, their study was limited to a 5-year period and only to costs borne by the two counties. To aid the collection of data needed to conduct a cost-benefit analysis of the use of an oral vaccine in large areas (e.g., an entire state) and over prolonged periods (e.g., 30 years), this article outlines some basic premises required for such an analysis and a generic cost-benefit model, which can be modified to fit specific geographic areas. Since many of the necessary data for the model are still being collected, the data used in the model are illustrative rather than definitive.
Any evaluation of the costs and benefits of using an oral vaccine to protect wild raccoon populations must be based on three premises: 1) Oral vaccine is distributed on a per unit area basis, calculated by using estimates of raccoon population density (i.e., a predetermined number of baits per raccoon times the number of raccoons per unit area). Costs of an oral vaccine program, therefore, are expressed in $/unit area. 2) To compare costs and benefits, all benefits that might accrue because of oral vaccine use must also be converted into $/unit area. 3) The cost savings (benefits) must be adjusted to match three broad, time-based categories describing different stages of an epizootic: pre-epizootic, epizootic, and post-epizootic (rabies still present in the population). The greatest cost savings is likely to occur during the epizootic since this stage is typically associated with the highest cost of raccoon rabies control (5; Tysmans, J., MPH thesis, 1996). In New Hampshire, for example, the annual number of requests for Animal Damage Control services involving raccoons went from 250 per year in pre-epizootic years (1988-1991), to 667 during an epizootic year (1993), and then declined to 165 in the post-epizootic years (13).
A cost-benefit model with a societal perspective was constructed (on Excel 5.0, Microsoft, Inc.) by using a discount rate of 3% (14) over 30 years to provide a Net Present Value (NPV) ( Technical Appendix). The costs of a raccoon rabies vaccination program include purchasing and distributing the oral vaccine in bait form. The benefits of such a program are the direct and indirect cost savings obtained by successfully halting or preventing a raccoon rabies epizootic and subsequent enzooticity. Since the vaccine technology is new, and no data exist on how the technology might change over the 30 years, it is assumed that the real costs and benefits are constant over the 30 years. Parameters and values used in the model are presented in Table 1.
Since what constitutes an "ideal" plan for large-scale oral vaccine bait distribution is not known, two scenarios were constructed. The area covered and the rate of barrier movement were chosen merely for illustration. Once actual proposals are made, the area covered and the time line may be modified to suit specific geographic areas. The first scenario assumes that bait is distributed in ever-expanding circles, starting with an area covered by a radius of 20 mi (area: 1,257 sq. mi). This area would be baited for 2 years. In the third year, the radius of the circle would be increased to 25 mi. The area between the 20-mi and 25-mi radius would then be baited for 2 years, at which time the radius defining the outer boundary would be increased by another 5 mi. This process would continue for 20 years, at the end of which the radius of the circle would be 65 mi, encompassing 13,273 sq. mi, which is approximately equal to one-third the area of New York State. At the end of the 20 years, a 10-year period would follow during which a 5-mi wide barrier zone would be baited every year. The yearly and cumulative total areas baited are shown in Figure 1. The barrier zone is necessary because the described plan cannot guarantee elimination, and the area covered by a vaccine program is vulnerable to the reintroduction of rabid animals. The second scenario considers the entire 13,273 sq. mi baited during the first 2 years, followed by 28 years of baiting a 5-mi-wide barrier zone.
In an economic analysis, opportunity costs should be used (15). However, the vaccine is still experimental, and data concerning discount prices could not be obtained. Therefore, the cost of oral vaccine in bait form was calculated at $1.50 per unit. This is the cost reported for trials of the oral vaccine in New York State (C. Hanlon, unpublished report, New York State Department of Health, 1995). In lieu of accurate opportunity costs, a sensitivity analysis evaluates the threshold price (i.e., NPV = $0) of the vaccine. This threshold value can then be compared with actual opportunity costs when more data become available.
The bait density required to successfully halt or stop raccoon rabies has not been definitively determined (10,11,16,17). Raccoon density can vary enormously with local ecology and weather (16,18-20). On the basis of densities currently under trial, for each of the two scenarios it is assumed that bait is distributed at 250 units per sq. mi, with an assumed raccoon density of approximately 50 per sq. mi (i.e., five baits per raccoon). Bait density is also the subject of sensitivity analysis.
Distribution costs for oral rabies vaccine have yet to be comprehensively documented. In current trials in New York and Massachusetts, bait was dropped by people walking and from aircraft, helicopters, and cars, depending on the terrain and available resources. The use of some vehicles has been donated, as have large amounts of personnel time; therefore, their cost is difficult to determine (an economic analysis must contain such costs). To illustrate the generic model, total distribution costs were assumed to be $100 per sq. mi. This cost is also the subject of a sensitivity analysis.
In the model described here, the benefits from using the oral vaccine are assumed to be the cost savings derived directly from preventing a raccoon-related rabies epizootic and post-epizootic. These cost savings are, therefore, the difference between the pre-epizootic costs of controlling rabies and the costs incurred during the epizootic and post-epizootic periods. It was assumed that a rabies epizootic lasts 2 years (1) and that the years following were defined as post-epizootic. The direct costs associated with the control of animal rabies have been listed (5) and can be broken down into four categories. These categories, with the estimated proportional contribution to the entire cost savings, are animal control costs (41%); laboratory diagnosis costs (13%); education and administration costs (9%); and human costs, such as pre- and post-exposure prophylaxis treatments (37%). Just as opportunity costs should be used for input costs, so potential cost savings should be valued at costs and not charges (15). For example, the average operating cost-to-charge ratio for urban hospitals in New York is 0.635:1 (15).
To illustrate the generic model, data from New York (Harris-Valente et al., unpublished report, 1995) were used to provide a preliminary estimate of cost savings ($1.52 per person), which will occur during the epizootic phase. The same data source yielded a figure of $0.30 per person during the post-epizootic phase. These savings per person are converted to savings per unit area as follows: On the basis of population estimates (21) from 53 counties in New York State, the median population density was estimated at 103 persons per sq. mi (25th percentile = 67; 75th = 204). Thus, for the areas baited, the savings were calculated at $156.56 per sq. mi for the first 2 epizootic years ($1.52 per person x 103 persons per sq. mi), and $30.90 per sq. mi for the post-epizootic years ($0.30 per person x 103 persons per sq. mi). Cost-savings data from New Jersey (5) are used in the sensitivity analysis.
The relative importance of distribution costs (excluding costs of vaccine) with respect to the amount of cost savings can be examined by constructing a distribution costs:cost savings ratio on a per-unit-area basis. Thus, the baseline case of $100 per sq. mi distribution costs and maximum cost savings during epizootic years of $156.56 per sq. mi ($1.52 per person x 103 persons per sq. mi) gives a ratio of 1:1.57. This ratio can be altered for sensitivity analyses.
The proportion of household pets and domesticated animals vaccinated before an epizootic can be quite low. For example, in Cumberland County, North Carolina, it was estimated that only 20% of dogs and cats were vaccinated against rabies before the epizootic (Tysmans, J., MPH thesis, 1996). During an epizootic, public health officials often encourage or enforce pet vaccinations, and vaccination rates often increase (5; Tysmans, J., MPH thesis, 1996). Successful elimination of raccoon rabies from an area could be considered a good reason for allowing vaccination rates to remain at lower levels, thus avoiding the costs associated with increased vaccinations. However debatable this proposition is, the economic impact of considering reduced pet vaccinations as a benefit is demonstrated by rerunning the two distribution scenarios and including the potential cost savings associated with reduced pet vaccination levels.
An example of the savings estimate follows: In 1991, there were 52.5 million dogs and 57 million cats in the United States (22), an average of 0.41 pets per person. During pre-epizootic periods, 0.14 pets per person (32% of average pets per person) are vaccinated each year against rabies (5). In the epizootic year this rate increased to 0.24 pets per person (55% of average pets per person) (5). Thus, during an epizootic period, there is an increase of approximately 11 extra pet vaccinations per sq. mi (0.24 - 0.14 pets per person x 103 persons per sq. mi). Pet vaccinations are costed at $16 per pet (Tysmans, J., MPH thesis, 1996). When baseline figures are used for distribution costs and cost savings (Table 1), a total distribution cost:cost savings ratio of 1:3.33 is calculated. No data are available concerning post-epizootic pet vaccination rates, and it is arbitrarily assumed that there are 2.75 extra pet vaccinations in post-epizootic stages (25% of the epizootic increase).
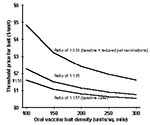
The impact of two alternate discount rates (0% and 5%) was evaluated, and the impact of higher distribution costs was assessed. In New Jersey (5), the costs of distribution were calculated at approximately $260 per sq. mi, while cost savings during the epizootic period were calculated at $2.60 per person (without reduced pet vaccinations considered as a benefit). This gives a distribution costs: cost savings ratio of 1:1.03 (compared with 1:1.57 in the baseline scenario) increasing the costs of distribution relative to cost-savings. The impact of removing the cost of having to continuously bait a barrier zone around areas covered by previous vaccination programs was then considered. In the first distribution scenario, costs associated with baiting a barrier for years 21 through 30 were removed from the model. In the second distribution scenario, it was assumed that the barrier need only be maintained for 2 years after the first 2 years of baiting (i.e., no baiting for years 5 through 30). The final sensitivity analysis used the first distribution scenario to examine the threshold price of oral vaccine for levels of bait density ranging from 100 sq. mi to 300 sq. mi, and using three different distribution costs:cost savings ratios. Threshold price was determined by altering the price of the vaccine until the NPV for a given bait density equaled $0 (see footnote) The first two price ratios were 1:1.57 (baseline, Table 1) and 1:1.96. The latter represents an arbitrary increase of +25% in cost-savings relative to distribution costs. The last price ratio used for the threshold analyses was constructed by assuming that reduced rates of pet vaccination resulted in additional cost-savings of $176 per sq. mi ($16 per pet x 11 extra vaccinations per sq. mi), giving a ratio of 1:3.33.
The first distribution scenario (expanding circles) provides smaller losses than the second distribution scenario (baiting the entire area in 2 years, followed by 28 years of baiting a 5-mi boundary) (Table 2). Considering the avoidance of increased pet rabies vaccinations as a benefit improves the NPVs of both scenarios and changes the NPV of the expanding circles distribution scenario from negative to positive. For the baseline case, using different discount rates changes the absolute values but not the signs.
The smaller distribution costs:cost saving ratio of 1:1.03 increased the losses (larger negative NPVs) and reduced the sole positive NPV to +$0.9 million (3% discount rate). Eliminating the need for baiting a protective barrier saves $4.8 million in the expanding circles scenario ($7.9-$3.1 million, 3% discount rate) and $14.8 million in the entire area scenario ($13.7 million + $1.1 million, 3% discount rate) (Table 2). Figure 2 shows the threshold prices for the oral vaccine in the expanding circles scenario, given different levels of bait density used and three different distribution costs:cost-savings ratios. At the baseline distribution costs:cost-savings ratio of 1:1.57, and at bait density of 250 baits per sq. mi, the threshold price for the oral vaccine is $0.63 per unit. When the distribution costs:cost-savings ratio is increased to 1:1.96, the threshold price for 250 baits per sq. mi is $0.91 per unit (+44% from baseline threshold). When reduced pet vaccinations are considered a benefit and the distribution costs:cost-savings ratio increases to 1:3.33, the threshold prices are always greater than the $1.50 cost of the vaccine (Figure 2).
Many of the data used in the generic model are assumed for illustrative purposes. The results presented here, therefore, should not be used to decide if a large-scale oral vaccine program is economically worthwhile. These results identify at least two priorities: the need to continue research that will determine the optimal level of bait density and the importance of better defining the distribution costs:cost-savings ratio. Both of these priorities are the focus of research efforts in New York and Massachusetts.
The results of the generic model (Table 2) clearly identify the importance of pet vaccinations when considering the costs and benefits of a raccoon vaccination program. It can be argued that avoidance of increased pet vaccinations is a benefit only if the laws requiring small animal vaccinations were passed solely as a result of the raccoon epizootic. It could be counterargued that, because past rabies control programs were so successful, the current laws are unnecessary and an economic burden to society. However, this would suggest that public health officials would accept a repeal of mandatory vaccination requirements except under extenuating circumstances (e.g., a rabies epizootic). Further, there are other sources of rabies exposure (e.g., bats), and the risk for pet exposure from these will most likely not be altered by a raccoon rabies vaccination program.
In evaluating an actual proposed rabies vaccine program, the use of expanding circles, although more economical than baiting entire areas at once (Table 2), may be unrealistic because of natural terrain or political boundaries. The sensitivity analyses demonstrated the costs of having to maintain a barrier (Table 2). The only way to avoid having to maintain a barrier over a long time may be to conduct a large-scale program, involving many contiguous states. However, such a program would pose a financial burden on governments and, at its conclusion, would still not stop rabies from being reintroduced in a manner similar to that which caused the current epizootic.
In addition to the issues related to distribution, two important implicit assumptions in the model affect costs: 1) the vaccine is 100% effective in stopping rabies in baited areas in 2 years; and, 2) rabies is not reintroduced. Removal of these assumptions would effectively increase the cost of the program by requiring increased bait densities, longer baiting periods, or both. Any of these situations would move the optimal bait density in Figure 2 (X-axis) to the right, further reducing the threshold value of the vaccine. Obviously, increased costs would merely increase the negative value of the NPVs presented in Table 2. The threshold analysis used here (Figure 2) provides a basis, even when some data are uncertain, for discussing discount pricing of the vaccine with the manufacturers when bulk purchases for large-scale programs are being planned.
References
- Rupprecht CE, Smith JS. Raccoon rabies—the re-emergence of an epizootic in a densely populated area. Semin Virol. 1994;5:155–64. DOIGoogle Scholar
- Krebs JW, Strine TW, Smith JS, Rupprecht CE, Childs JE. Rabies surveillance in the United States during 1993. J Am Vet Med Assoc. 1994;205:1695–709.PubMedGoogle Scholar
- Centers for Disease Control and Prevention. Rabies postexposure prophylaxis—Connecticut, 1990-1994. MMWR Morb Mortal Wkly Rep. 1996;45:232–4.PubMedGoogle Scholar
- Centers for Disease Control and Prevention. Animal rabies—South Dakota, 1995. MMWR Morb Mortal Wkly Rep. 1996;45:164–6.PubMedGoogle Scholar
- Uhaa IJ, Dato VM, Sorhage FE, Beckly JW, Roscoe DE, Gorsky RD, Benefits and costs of using an orally absorbed vaccine to control rabies in raccoons. J Am Vet Med Assoc. 1992;201:1873–82.PubMedGoogle Scholar
- Winkler WG, Bogel K. Control of rabies in wildlife. Sci Am. 1992; (
June ):86–92. DOIPubMedGoogle Scholar - Rupprecht CE, Smith JS, Fekadu M, Childs JE. The ascension of wildlife rabies: A cause for public health concern or intervention? Emerg Infect Dis. 1995;1:107–14. DOIPubMedGoogle Scholar
- Steck F, Wandler A, Bischel P, Capt S, Hafliger U, Schneider L. Oral immunization of foxes against rabies. Laboratory and field studies. Comp Immunol Microbiol Infect Dis. 1982;5:165–79. DOIPubMedGoogle Scholar
- Rupprecht CE, Wiktor TJ, Johnson DH, Hamir AN, Dietzschold B, Wunner Wh, et al. Oral immunization and protection of raccoons (Procyon lotor) with a vaccinia-rabies glycoprotein recombinant virus vaccine. Proc Natl Acad Sci U S A. 1986;83:7947–50. DOIPubMedGoogle Scholar
- Robbins AH, Niezgoda M, Levine S, Windmiller BS, McGuill MW, Rowell SL, Oral rabies vaccination of raccoons (Procyon lotor) on the Cape Cod isthmus, Massachusetts. Presented at the 5th Annual International Meeting of Rabies in the Americas, Niagara Falls, Ontario, Canada, 1994; Conference Abstracts, p.29.
- Hanlon CA, Trimarchi CE, Rupprecht CE, Debbie JG. Oral wildlife rabies vaccination in New York state: First field evaluation in an enzootic raccoon rabies area. Presented at the 6th Annual International Meeting on Research Advances and Rabies Control in the Americas, Merida, Mexico, 1995; Program and Abstracts, p.29.
- Manning A. Texas officials take battle against rabies to the air. USA Today January 11, 1996:27.
- Slate D, Calvert RT, Chipman RB, Barden ME. Raccoon pest management patterns before, during and after a rabies epizootic in northern New England: What do they mean? Presented at the 6th Annual International Meeting on Research Advances and Rabies Control in the Americas, Merida, Mexico; 1995; Program and Abstracts, p.20.
- Gold MR, Siegel JE, Russell LB, Weinstein MC, eds. Cost effectiveness in health and medicine. New York: Oxford University Press, 1996.
- Haddix AC, Teutsch SM, Shaffer PA, Dunet DO, eds. Prevention effectiveness: A guide to decision analysis and economic evaluation. New York: Oxford University Press, 1996.
- Perry BD, Garner N, Jenkins SR, McCloskey K, Johnston DH. A study of techniques for the distribution of oral rabies vaccine to wild raccoon populations. J Wildl Dis. 1989;25:206–17.PubMedGoogle Scholar
- Linhart SB, Blom FS, Engeman RM, Hill HL, Hon T, Hall DI, A field evaluation of baits for delivering oral rabies vaccines to raccoons (Procyon lotor). J Wildl Dis. 1994;30:185–94.PubMedGoogle Scholar
- Hanlon CL, Hayes DE, Hamir AN, Snyder DE, Jenkins S, Hable CP, Proposed field evaluation of a rabies recombinant vaccine for raccoons (Procyon lotor): sites election, target species characteristics, and placebo baiting trials. J Wildl Dis. 1989;25:555–67.PubMedGoogle Scholar
- Hoffmann CO, Gottschang JL. Numbers, distribution, and movements of a raccoon population in a suburban residential community. J Mammal. 1977;58:623–36. DOIGoogle Scholar
- Hudson EM. The raccoon (Procyon lotor) on St. Catherines Island, Georgia: Part 2: Relative abundance in different forest types as a function of population density. American Musgum Novitates 1978;1-16.
- Population Estimates and Population Distribution Branches, Division of Population, U.S. Bureau of the Census. Estimates of the resident population of states and counties, and percent change 4/1/90 to 7/1/94. Posted on the Internet: 1995 Jan 18.
- American Veterinary Medical Association. US pet ownership and demographics source book. Schaumburg, IL: American Veterinary Medical Association, 1995.
Figures
Tables
Cite This ArticleTable of Contents – Volume 2, Number 4—October 1996
| EID Search Options |
|---|
|
|
|
|
|
|