Volume 20, Number 4—April 2014
Letter
Serologic Evidence of Leptospirosis in Humans, Union of the Comoros, 2011
Cite This Article
Citation for Media
To the Editor: Leptospirosis is a worldwide bacterial zoonosis caused by infection with pathogenic Leptospira spp. (Spirochaetales, Leptospiraceae). Most mammals can be infected, but rats are considered the main reservoir, maintaining Leptospira spirochetes in the lumen of renal tubules and contaminating the environment with bacteria-infected urine. Transmission to humans is accidental, occurring through contact with animal secretions or with contaminated environmental materials.
In temperate countries, human leptospirosis is a sporadic disease; incidence is much higher in the tropics because climate and environmental conditions are conducive to the survival of bacteria, resulting in increased exposure of humans to leptospirosis-causing pathogens (1). Among islands in the southwestern Indian Ocean, human leptospirosis is endemic to Mayotte, France, and La Réunion (2–4) and to the Seychelles, where the incidence of leptospirosis is one of the highest worldwide (5). Leptospirosis is poorly documented in other islands in the region, including Mauritius, Madagascar, and the Union of the Comoros (2,6–8). Whether the scant documentation indicates underdiagnosis or reflects local epidemiologic specificities is unknown. To improve knowledge of Leptospira infection in the region, we conducted a study in the Union of the Comoros to serologically assess the presence or absence of leptospirosis in humans. The Union of the Comoros consists of 3 islands: Grande-Comore, Mohéli, and Anjouan. Together with a fourth, southern island, Mayotte, these islands form the Comoros Archipelago.
For feasibility reasons, we used excess serum samples. Seventy-six samples were from healthy volunteers who gave informed consent; 318 clinical blood samples from patients had been obtained by private laboratories and by the surveillance laboratory of the National Malaria Control Programme (PNLP) during August 1–October 8, 2011. The Ministère de la Santé, de la Solidarité et de la Promotion du Genre of the Union of the Comoros, authorized the serologic investigation (authorization no. 1175/MSSPG/DNS).
We used the microscopic agglutination test (MAT) to test serum samples; the MAT was based on a panel of 15 Leptospira strains, enabling the screening of all recently reported serogroups for human and animal cases on neighboring Mayotte (2,4,9). A list of the tested strains follows, shown as Genus species Serogroup/Serovar (type strain): L. borgpetersenii Ballum/Castellonis (Castellon 3), L. borgpetersenii Sejroe/Hardjobovis (Sponselee), L. borgpetersenii Sejroe/Sejroe (M 84), L. borgpetersenii Tarassovi/Tarassovi (Perepelicin), L. interrogans Australis/Australis (Ballico), L. interrogans Autumnalis/Autumnalis (Akiyami A), L. interrogans Bataviae/Bataviae (Van Tienen), L. interrogans Canicola/Canicola (Hond Utrecht IV), L. interrogans Hebdomadis/Hebdomadis (Hebdomadis), L. interrogans Icterohaemorrhagiae/Copenhageni (Wijnberg), L. interrogans Pyrogenes/Pyrogenes (Salinem), L. kirschneri Cynopteri/Cynopteri (3522C), L. kirschneri Grippotyphosa/Grippotyphosa (Moskva V), L. kirschneri Mini/Undetermined serovar (200803703) (9), L. noguchii Panama/Panama (CZ214K). Each serum sample was tested at dilutions ranging from 1:50 to 1:3,200 and considered positive when the MAT titer was >100.
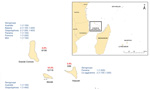
Our serologic findings showed evidence of Leptospira infection in humans on the 3 islands of the Union of the Comoros (MAT titers 100–1,600, geometric mean titer [GMT] 194). The positivity rate was 10.3% (95% CI 4.8–15.9) for samples from Mohéli, 4.2% (95% CI 1.4–7.0) for samples from Grande-Comore, and 3.4% (95% CI 0.1–6.7) for samples from Anjouan; no significant difference was found between islands or by the age or sex of residents (p>0.05, Fisher exact test). Leptospira infection was more prevalent and MAT titers were higher among serum samples from the patient group than the healthy donor group (20 positive samples/318 total vs. 3 positive samples/76 total; GMT 207 vs. GMT 126), but the difference was not significant (p>0.05, Fisher exact test). In 78% of seropositive serum samples, antibodies reacted with serogroups Australis, Bataviae, Grippotyphosa, Panama, Pomona, Pyrogenes, Mini, and/or Sejroe. MAT titers >100, which are suggestive of more specific antibodies to Leptospira, were observed for all serogroups except Australis and Sejroe. Pyrogenes serogroup was identified in one third of positive samples from Mohéli and was associated with the highest agglutination titers (Figure).
Our data indicate that Leptospira infections do occur in humans in the Union of the Comoros; this finding is consistent with those in studies reporting leptospirosis in persons returning from travel in the Union of the Comoros (2,8) and with the detection of pathogenic Leptospira spp. in bats sampled on these islands (10). The human leptospirosis–related serologic findings in Union of Comoros are most comparable to those from neighboring Mayotte, where leptospirosis is mainly caused by serogroups Mini/Sejroe/Hebdomadis complex, Pyrogenes, Grippotyphosa, and Pomona and where serogroup Icterohaemorraghiae is not detectable (2). These findings contrast with human leptospirosis findings from La Réunion and the Seychelles, where the Icterohaemorraghiae serogroup is most common (3).
Our MAT-derived data cannot discriminate between recent and past Leptospira infections, nor can these data be used to determine the severity of the disease in the Union of the Comoros. Nonetheless, the data strongly support the presence of human leptospirosis on the 3 islands of the Union of the Comoros and emphasize the need for a proper diagnosis to ascertain the number of leptospirosis cases among the acute febrile illnesses in this country.
Acknowledgments
We thank Lisa Cavalerie and Marina Béral for their help with statistical analysis and with preparing the figure.
This work was supported by European Regional Development Funds ERDF- POCT; Réunion, LeptOI project.
References
- Bourhy P, Collet L, Lernout T, Zinini F, Hartskeerl RA, van der Linden H, Human Leptospira isolates circulating in Mayotte (Indian Ocean) have unique serological and molecular features. J Clin Microbiol. 2012;50:307–11. DOIPubMedGoogle Scholar
- Picardeau M. Diagnosis and epidemiology of leptospirosis. Med Mal Infect. 2013;43:1–9. DOIPubMedGoogle Scholar
- Bourhy P, Collet L, Clément S, Huerre M, Ave P, Giry C, Isolation and characterization of new Leptospira genotypes from patients in Mayotte (Indian Ocean). PLoS Negl Trop Dis. 2010;4:e724. DOIPubMedGoogle Scholar
- Pappas G, Papadimitriou P, Siozopoulou V, Christou L, Akritidis N. The globalization of leptospirosis: worldwide incidence trends. Int J Infect Dis. 2008;12:351–7. DOIPubMedGoogle Scholar
- Simon F, Morand G, Roche C, Coton T, Kraemer P, Fournier P-E, Leptospirosis in a French traveler returning from Mauritius. J Travel Med. 2012;19:69–71. DOIPubMedGoogle Scholar
- Rahelinirina S, Léon A, Harstskeerl RA, Sertour N, Ahmed A, Raharimanana C, First isolation and direct evidence for the existence of large small-mammal reservoirs of Leptospira sp. in Madagascar. PLoS ONE. 2010;5:e14111. DOIPubMedGoogle Scholar
- Socolovschi C, Angelakis E, Renvoisé A, Fournier P-E, Marié JL, Davoust B, Strikes, flooding, rats, and leptospirosis in Marseille, France. Int J Infect Dis. 2011;15:e710–5. DOIPubMedGoogle Scholar
- Desvars A, Naze F, Vourc’h G, Cardinale E, Picardeau M, Michault A, Similarities in Leptospira serogroup and species distribution in animals and humans in the Indian Ocean island of Mayotte. Am J Trop Med Hyg. 2012;87:134–40. DOIPubMedGoogle Scholar
- Lagadec E, Gomard Y, Guernier V, Dietrich M, Pascalis H, Temmam S, Pathogenic Leptospira spp. in bats, Madagascar and Union of the Comoros. Emerg Infect Dis. 2012;18:1696–8. DOIPubMedGoogle Scholar
Figure
Cite This ArticleRelated Links
Table of Contents – Volume 20, Number 4—April 2014
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Pablo Tortosa, CRVOI, Plateforme de recherche CYROI, 2 rue Maxime Rivière, 97490 Ste Clotilde, FrancePablo Tortosa, CRVOI, Plateforme de recherche CYROI, 2 rue Maxime Rivière, 97490 Ste Clotilde, France
Top