Volume 21, Number 1—January 2015
Dispatch
Avian Influenza (H7N9) Virus Infection in Chinese Tourist in Malaysia, 2014
Cite This Article
Citation for Media
Abstract
Of the ≈400 cases of avian influenza (H7N9) diagnosed in China since 2003, the only travel-related cases have been in Hong Kong and Taiwan. Detection of a case in a Chinese tourist in Sabah, Malaysia, highlights the ease with which emerging viral respiratory infections can travel globally.
Human infection with avian influenza (H7N9) virus was first reported from China in 2013 (1). Since then, ≈400 cases have been diagnosed in China and some in Hong Kong and Taiwan. Most patients were older adults with severe community-acquired pneumonia; risk for admission to an intensive care unit is 83%, and risk for death is 27%–36% (2,3). We report avian influenza (H7N9) virus infection outside greater China, in a Chinese tourist visiting Sabah, Malaysia.
The patient was a 66-year-old woman from Guangzhou, Guangdong Province, China. She was not obese and had no relevant medical history. She worked on a household farm that cultivated vegetables but not animals. On January 30, 2014, she purchased from a poultry market 3 live chickens, which she slaughtered and cooked that day. According to the patient, these chickens and those at the market appeared healthy; she reported no contact with other birds. Two days later, she experienced cough, myalgia, and fever and consulted a local doctor who treated her symptomatically without performing laboratory or radiologic investigations. The woman subsequently went on holiday and flew to Peninsular Malaysia on February 4 and to Sabah, Malaysian Borneo, on February 6. She had persistent fever, worsening productive cough, arthralgia, abdominal pain, and diarrhea. On February 7, she sought care at Tuaran District Hospital for acute respiratory distress; she was intubated and transferred to a private specialist hospital in Kota Kinabalu, Sabah, Malaysia. At admission, she was placed in a negative-pressure isolation room with a portable high-efficiency particulate air filter that removes air particles >0.3 μm; staff observed airborne-transmission precautions.
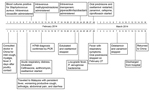
Abnormal findings during initial examination were blood pressure 70/40 mm Hg, heart rate 96 beats/minute, and generalized crackles heard on lung auscultation. Hematologic, biochemical, and arterial blood gas results from samples obtained at admission (while the patient received 100% oxygen by mechanical ventilation) are summarized in the Table. Chest radiographs showed extensive dense pulmonary consolidations. The patient received dopamine, ceftriaxone, azithromycin, and oseltamivir. Culture of blood collected at admission grew methicillin-susceptible Staphylococcus aureus; tracheal aspirate results were negative, and cloxacillin was administered. The patient received ventilatory support with synchronized intermittent mandatory ventilation with a positive end-expiratory pressure of 10 cm H2O. On February 13 she was given methylprednisolone, which was discontinued on February 20 and replaced with oral prednisone on February 21. Ventilatory requirements gradually decreased, and she was extubated on February 22, after blood results normalized and oseltamivir was discontinued. However, on February 23, a low-grade fever and Pseudomonas aeruginosa bacteremia were found, and the patient was given meropenem and piperacillin-tazobactam. On February 28, her respiratory symptoms and fever recrudesced after discontinuation of oral prednisone. On the same day, oseltamivir and prednisone were given along with inhaled zanamivir, intravenous cefepime, and ciprofloxacin; her condition gradually improved. On March 7, oseltamivir and zanmivir were discontinued; on March 13, the patient was considered well and was discharged with a tapering dose of prednisone. She returned to China on March 16. A time line of her travel and hospital course is detailed in the Figure.
According to Malaysian Ministry of Health criteria, infection with influenza (H7N9) virus is suspected in persons with severe respiratory illness and a history of travel from affected areas in China. For this patient, on February 7, clinicians from district and specialist hospitals sent throat swabs in viral transport media (Copan Diagnostics, Inc., Murrieta, CA, USA) to the National Influenza Centre at the Institute of Medical Research in Kuala Lumpur for virus studies. Real-time reverse transcription PCR was used to test for the following viruses, as described (4): influenza A, influenza B, influenza A(H1N1) pdm09, influenza H1 seasonal, influenza H3 seasonal (all by using Centers for Disease Control and Prevention protocols [5]), influenza H7 avian (Centers for Disease Control and Prevention, Chinese National Influenza Centre [1], and local protocols), and influenza N9 (Chinese National Influenza Centre protocol). Results were positive for influenza A and influenza H7 and N9: results remained positive on repeated swab samples collected on February 13 and 22. Sequencing of the hemagglutinin and neuraminidase genes revealed that these strains were closely related to strains from Guangzhou and Guandong (4) but did not reveal the mutation associated with oseltamivir resistance: R294K (N9 numbering) (6). No virus was detected in samples collected on February 26 and 28.
During February 7–16, officials from the Malaysian Public Health Department and Sabah State Health Department identified 191 persons who had had contact with the patient; 6 were symptomatic, but nasopharyngeal swab specimens were negative for influenza. The symptomatic contacts included tour group members and personnel from various hotels, restaurants, airlines, tourist destinations, airports, and hospitals.
The rapid diagnosis of avian influenza (H7N9) virus infection outside China and Taiwan in a Chinese tourist traveling to Sabah, Malaysia, highlights the value of a high index of suspicion by medical staff, awareness and adherence to national guidelines, and good laboratory services (4). The clinical features of the patient were similar to those previously reported from China: median age of affected persons was 61 years, and >80% of patients reported exposure to live poultry and experienced pneumonia or respiratory failure (7). Virus was detected by reverse transcription PCR after the patient had received oseltamivir for 2 weeks, as has been reported (6), although the significance of prolonged detection is unclear because the patient’s clinical condition improved markedly, no oseltamivir resistance mutations were found (4), and virus persistence may have be associated with steroid use. The patient’s condition deteriorated after taking oseltamivir 1 week after symptom onset and ventilatory requirements increased, possibly because of secondary S. aureus infection, a well-known complication of influenza (8). The patient was given methylprednisolone after a week of hospitalization; although she subsequently improved, it was unclear if this was in response to the antimicrobial drugs, the corticosteroids, or the natural course of the infection. Anecdotal reports describe clinical improvement of a patient in Taiwan with influenza (H7N9) pneumonia after receipt of corticosteroids (9), but such improvement has not been supported by larger studies of influenza (H7N9) patients (3) or studies of adults in Vietnam infected with avian influenza (H5N1) virus (10,11).
Of the ≈400 cases of human avian influenza (H7N9) infection diagnosed in China since 2003, the only travel-related cases were in Hong Kong and Taiwan, which have close geographic, economic, and cultural ties to China and extensive bidirectional travel. This case highlights the ease with which emerging viral infections can travel globally. On a map of recent air travel from China, major destinations identified (12) were Taiwan, Hong Kong, Malaysia, and Singapore; dozens of flights went to major cities in Europe and North America, which received hundreds of visitors directly from China weekly. In the first 3 quarters of 2013, an estimated 72.5 million tourists left China (13). To ensure accurate identification and appropriate management of emerging novel respiratory viral infections, clinicians in destination countries need to obtain detailed travel histories from tourists and returning travelers
The influenza (H7N9) virus is not easily transmissible among humans, and our investigations did not find any evidence of spread to the patient’s fellow travelers, medical staff, or other contacts. However, the virus has the potential to adapt to mammalian hosts over time (14,15). Clinicians and public health authorities need to be alert to the latest epidemiologic information on emerging respiratory viruses; local capacity to isolate, diagnose, and treat illness in travelers with unusual respiratory viral infections is also needed.
Dr. William is an infectious diseases physician at the Queen Elizabeth Hospital, Kota Kinabalu, Sabah, Malaysia. His research interests are the epidemiology, clinical features, diagnosis, pathophysiology, and management of malaria caused by Plasmodium knowlesi.
Acknowledgment
We thank the Director General of Health, Malaysia, for permission to publish this report and Makmal Kesihatan Awam for providing and allowing us to publish the results of the investigation of possible contacts. We also thank Anupama Vasudevan for assistance with preparation of the figure.
References
- Gao R, Cao B, Hu Y, Feng Z, Wang D, Hu W, Human infection with a novel avian-origin influenza A (H7N9) virus. N Engl J Med. 2013;368:1888–97. DOIPubMedGoogle Scholar
- Yu H, Cowling BJ, Feng L, Lau EH, Liao Q, Tsang TK, Human infection with avian influenza A H7N9 virus: an assessment of clinical severity. Lancet. 2013;382:138–45. DOIPubMedGoogle Scholar
- Gao HN, Lu HZ, Cao B, Du B, Shang H, Gan JH, Clinical findings in 111 cases of influenza A (H7N9) virus infection. N Engl J Med. 2013;368:2277–85. DOIPubMedGoogle Scholar
- Jeyanthi S, Tengku Rogayah TAR, Thayan R, Az-Ulhusna A, Aruna A, Khebir BV, Molecular characterization of influenza A (H7N9) virus from the first imported H7N9 case in Malaysia. J Gen Mol Virol. 2014;6:19–27 .DOIGoogle Scholar
- Novel Swine-Origin Influenza A (H1N1) Virus Investigation Team; Dawood FS, Jain S, Finelli L, Shaw MW, Lindstrom S, Garten RJ, Emergence of a novel swine-origin influenza A (H1N1) virus in humans. N Engl J Med. 2009;360:2605–15.
- Hu Y, Lu S, Song Z, Wang W, Hao P, Li J, Association between adverse clinical outcome in human disease caused by novel influenza A H7N9 virus and sustained viral shedding and emergence of antiviral resistance. Lancet. 2013;381:2273–9. DOIPubMedGoogle Scholar
- Li Q, Zhou L, Zhou M, Chen Z, Li F, Wu H, Epidemiology of human infections with avian influenza A(H7N9) virus in China. N Engl J Med. 2014;370:520–32. DOIPubMedGoogle Scholar
- Morens DM, Taubenberger JK, Fauci AS. Predominant role of bacterial pneumonia as a cause of death in pandemic influenza: implications for pandemic influenza preparedness. J Infect Dis. 2008;198:962–70. DOIPubMedGoogle Scholar
- Lin PH, Chao TL, Kuo SW, Wang JT, Hung CC, Lin HC, Virological, serological, and antiviral studies in an imported human case of avian influenza A(H7N9) virus in Taiwan. Clin Infect Dis. 2014;58:242–6 .DOIPubMedGoogle Scholar
- Hien ND, Ha NH, Van NT, Ha NT, Lien TT, Thai NQ, Human infection with highly pathogenic avian influenza virus (H5N1) in northern Vietnam, 2004–2005. Emerg Infect Dis. 2009;15:19–23. DOIPubMedGoogle Scholar
- Tran TH, Nguyen TL, Nguyen TD, Luong TS, Pham PM. Nguyen vV, et al. Avian influenza A (H5N1) in 10 patients in Vietnam. N Engl J Med. 2004;350:1179–88.
- Butler D. Mapping the H7N9 avian flu outbreaks. Nature. 2013 Apr 24 [cited 2014 Sep 30]. http://www.nature.com/news/mapping-the-h7n9-avian-flu-outbreaks-1.12863
- Arit WG. China's outbound tourism growing by 18%—and no sign of slowing down. Forbes Asia. 2013 Nov 21 [cited 2014 Sep 30]. http://www.forbes.com/sites/profdrwolfganggarlt/2013/11/21/chinas-outbound-tourism-growing-by-18-and-no-sign-of-slowing-down/
- Morens DM, Taubenberger JK, Fauci AS. H7N9 avian influenza A virus and the perpetual challenge of potential human pandemicity. mBio. 2013;4:e00445–13 9DOIGoogle Scholar
- Morens DM, Taubenberger JK, Fauci AS. Pandemic influenza viruses—hoping for the road not taken. N Engl J Med. 2013;368:2345–8. DOIPubMedGoogle Scholar
Figure
Table
Cite This ArticleTable of Contents – Volume 21, Number 1—January 2015
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Tsin Wen Yeo, Lee Kong Chian School of Medicine, Nanyang Technological University, Singapore School of Biological Sciences, 60 Nanyang Ave #04n-15, 637551, Singapore
Top