Volume 26, Number 12—December 2020
Research Letter
Transmission Electron Microscopy Confirmation of Orientia tsutsugamushi in Human Bile
Cite This Article
Citation for Media
Abstract
Scrub typhus, the third most frequently reported infectious disease in South Korea, causes serious public health problems. In 2019, we collected a bile specimen from a patient with scrub typhus through percutaneous transhepatic gallbladder drainage and performed transmission electron microscopy to confirm the ultrastructure of Orientia tsutsugamushi.
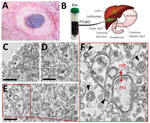
Orientia tsutsugamushi is a gram-negative obligately intracellular coccobacillus and a causative pathogen of scrub typhus, which is transmitted to humans by bites from trombiculid (chigger) mites (1). Scrub typhus is a prevalent acute febrile disease that mainly occurs in the Asia-Pacific region, infecting »1 million persons worldwide each year. In South Korea, infections have increased rapidly since 2014 because of climate change, increased outdoor activities, and numbers of elderly farmers (2). The most typical clinical manifestation of scrub typhus is an eschar at the site of the bite (Figure, panel A); symptoms include fever, headache, muscle pain, nausea, and vomiting (3). Without proper diagnosis and antimicrobial drug treatment, severe illness with multiple organ system involvement can occur; the death rate is »10% (4). Immunohistochemical staining for O. tsutsugamushi antigens have revealed extensive endothelial cell infection in the heart, lung, kidney, pancreas, skin, and brain (5). Bacteria also have been detected in cardiac muscle cells and in macrophages in the liver and spleen (5,6).
In humans, the liver secretes »1 L of bile daily into the intestinal tract. However, little information is available about the presence of gram-negative bacteria in bile (7). Pathogenic microorganisms must endure potential impediments, such as variations in pH, low oxygen levels, nutrient limitation, and elevated osmolarity, to survive in this harsh environment (7). We collected bile from a patient with scrub typhus in South Korea (Figure, panel B) and visualized the ultrastructure of O. tsutsugamushi in the clinical sample using transmission electron microscopy.
In 2019, a 68-year-old woman reported fever, drowsy mental state, abdominal pain, and reduced oral intake. These symptoms had begun 7 days earlier. Her vital signs were blood pressure 100/60 mm Hg and body temperature 38.9°C. Laboratory analysis revealed a leukocyte count 10,350/mL (reference range 4,800–10,800/mL), platelet count 45,000/mL (reference 130,000–450,000/mL), serum creatinine 0.4 mg/dL (reference 0.7–1.7 mg/dL), aspartate aminotransferase 31 IU/L (reference 12–33 IU/L), alanine aminotransferase 41 IU/L (reference 5–35 IU/L), total bilirubin 1.72 mg/dL (reference 0.2–1.2 mg/dL), and C-reactive protein 196.86 mg/L (reference <5 mg/L). Abdominal computed tomography scan detected acute cholecystitis, and percutaneous transhepatic gallbladder drainage was performed. The presence of acute cholecystitis in scrub typhus cases is rare (5 [1.1%] instances of 442 cases) (8). O. tsutsugamushi can also cause liver injury in some patients, but the patient reported here did not have any such signs (9). We confirmed scrub typhus using indirect immunofluorescence assay (IgG 5,120) and nested PCR selective for the 56-kDa gene of O. tsutsugamushi (Appendix). The O. tsutsugamushi identified belonged to the Boryong strain (the most common strain in South Korea). We also detected an eschar in the right inguinal area (Figure, panel A). The patient completely recovered after doxycycline treatment.
A drainage tube was placed in the patient’s gallbladder, and the bile was directly discharged and collected through the tube (Figure, panel B). We tested the bile specimen for pathogens using nested quantitative reverse transcription PCR and DNA sequencing to detect a specific O. tsutsugamushi gene encoding a 56-kDa protein (Appendix) (10). After chemical fixation, the sample was embedded in 100% Epon 812 resin and ultrathin (»80-nm thick) sections were stained with 2% uranyl acetate and 1% lead citrate (Appendix) (10). This sample preparation method might not preserve the ultrastructure of live bacteria, but structural features of the bacteria can be clearly observed. The ultrastructural details were acquired using transmission electron microscopy at 120 kV. Despite the presence of a wide variety of components, we detected O. tsutsugamushi in the bile (asterisks in Figure, panels C–E). The bacteria showed a coccobacillus shape and were 0.5–0.7-μm in diameter and 1.2–2.5-μm long, all typical features of O. tsutsugamushi (5,10). The bacterial cytoplasm was surrounded by an outer membrane, an internal plasma membrane, and a peptidoglycan layer (Figure, panel F). Moreover, the periplasmic space appeared as an electron-lucent gap between the 2 membranes. We also observed a thicker outer leaflet of the cell wall membrane, which is a typical and diagnostic sign of Orientia (5). We also detected multilamellar bodies, which are cholesterol-carrying particles, in the bile sample (black arrowheads in Figure, panel F).
Previously, human scrub typhus disease was studied using a mouse model mimicking the disease and examining clinical samples postmortem (5,6). However, the host cell of O. tsutsugamushi in humans has not been completely defined. In this study, we confirmed detection of O. tsutsugamushi in human bile, an environment in which bacterial survival is challenging. This observation (i.e., the presence of O. tsutsugamushi in human bile) might be useful for diagnosing scrub typhus in patients who do not show clear eschars or skin rash, broadening the potential routes for diagnosing the disease.
Ms. Y. Lee is a researcher at the Korea Basic Science Institute. Her primary interests are electron microscopy of infectious viral and bacterial diseases. Dr. Kim is a senior researcher at the Korea Basic Science Institute. His research interests are in the proteomics of infectious diseases.
Acknowledgment
This work was supported by the Basic Science Research Programs (NRF-2015R1D1A1A01060251 and 2018R1D1A3B07049557) of the National Research Foundation of Korea, which is funded by the Ministry of Education; the Korea Basic Science Institute grant (C030221), and National Research Council of Science & Technology grant by the Korea government (CRC-16-01-KRICT).
References
- Liu YX, Cao WC, Gao Y, Zhang JL, Yang ZQ, Zhao ZT, et al. Orientia tsutsugamushi in eschars from scrub typhus patients. Emerg Infect Dis. 2006;12:1109–12. DOIPubMedGoogle Scholar
- Kim DM. Clinical features and diagnosis of scrub typhus. Infect Chemother. 2009;41:315–22. DOIGoogle Scholar
- Lee CS, Hwang JH. IMAGES IN CLINICAL MEDICINE. Scrub Typhus. N Engl J Med. 2015;373:2455. DOIPubMedGoogle Scholar
- VieBrock L, Evans SM, Beyer AR, Larson CL, Beare PA, Ge H, et al. Orientia tsutsugamushi ankyrin repeat-containing protein family members are Type 1 secretion system substrates that traffic to the host cell endoplasmic reticulum. Front Cell Infect Microbiol. 2015;4:186. DOIPubMedGoogle Scholar
- Moron CG, Popov VL, Feng HM, Wear D, Walker DH. Identification of the target cells of Orientia tsutsugamushi in human cases of scrub typhus. Mod Pathol. 2001;14:752–9. DOIPubMedGoogle Scholar
- Shelite TR, Saito TB, Mendell NL, Gong B, Xu G, Soong L, et al. Hematogenously disseminated Orientia tsutsugamushi–infected murine model of scrub typhus [corrected]. Erratum in: PLoS Negl Trop Dis. 2014;8:e3175. PLoS Negl Trop Dis. 2014;8:e2966.
- Begley M, Gahan CG, Hill C. The interaction between bacteria and bile. FEMS Microbiol Rev. 2005;29:625–51. DOIPubMedGoogle Scholar
- Lee H, Ji M, Hwang JH, Lee JY, Lee JH, Chung KM, et al. Acute cholecystitis in patients with scrub typhus. J Korean Med Sci. 2015;30:1698–700. DOIPubMedGoogle Scholar
- Chung JH, Lim SC, Yun NR, Shin SH, Kim CM, Kim DM. Scrub typhus hepatitis confirmed by immunohistochemical staining. World J Gastroenterol. 2012;18:5138–41. DOIPubMedGoogle Scholar
- Ro HJ, Lee H, Park EC, Lee CS, Il Kim S, Jun S. Ultrastructural visualization of Orientia tsutsugamushi in biopsied eschars and monocytes from scrub typhus patients in South Korea. Sci Rep. 2018;8:17373. DOIPubMedGoogle Scholar
Figure
Cite This ArticleOriginal Publication Date: November 11, 2020
1These authors contributed equally to this article.
2These authors were co-principal investigators.
Table of Contents – Volume 26, Number 12—December 2020
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Sangmi Jun, Center for Research Equipment, Korea Basic Science Institute, 162 Yeongudanji-ro, Ochang-eup, Cheongwon-gu, Cheongju-si, Chungcheongbuk-do, 28119, South Korea
Top