Volume 26, Number 4—April 2020
Research Letter
Trombiculiasis in a Dog with Severe Neurologic Disorders, Spain
Cite This Article
Citation for Media
Abstract
Chiggers, the larvae of trombiculid mites, parasitize a wide variety of terrestrial vertebrates worldwide. Their bites cause seasonal trombiculiasis in humans and animals. Affected canines can have a variety of digestive and systemic clinical signs. We describe a case of canine trombiculiasis in a dog exhibiting severe neurologic symptoms.
Larvae of trombiculid mites (Acari: Trombiculidae), commonly known as chiggers, are widespread ectoparasites of vertebrates. More than 3,000 trombiculid species are known, and small mammals and birds are their main hosts (1). In Asia, chiggers transmit scrub typhus, a life-threatening human infection caused by Orientia tsutsugamushi (2). In Europe, chiggers are associated with a seasonal trombiculiasis, a dermatitis that affects humans and animals, mostly dogs and cats (3). Infected animals can have signs of skin lesions, pruritus, asthenia, fatigue, pyrexia, digestive disorders, or neurologic dysfunction (3–5). We describe a case of a dog in Spain heavily infested by chiggers and exhibiting severe neurologic symptoms.
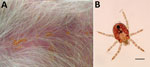
On October 14, 2013, a 2-year-old male basset hound in poor health was admitted to Vetersalud Asís Hospital in Logroño, Spain. The owner reported that the dog had been vomiting and having trouble breathing for 12 hours before he was brought to the veterinary hospital. The dog was drooling, torpid and confused, vocalizing, and barely able to stand. His symptoms started the evening before with a lack of appetite, lethargy, and licking and biting his paws. The symptoms progressed to convulsions and ataxia so severe that the dog could no longer scratch itself. At initial evaluation, he had ataxia and loss of balance. Further clinical examination revealed an elevated body temperature of 39.6°C (normal 38°C–39°C), tachypnea with hyperventilation, and mucosal congestion. Skin examination revealed focal areas of erythema and papules on the abdomen, above the eyes, and in the interdigital areas. We performed skin scrapings on several lesions and needed tweezers to remove many mites that were attached to the dog’s skin (Figure, panel A). Microscopic examination of skin scrapings revealed numerous live mites, which we morphologically identified as Neotrombicula inopinata (6,7) (Figure, panel B).
We treated the dog with phenylpyrazole, a broad-spectrum topical insecticide, and most of the mites detached within 12 hours. We treated the dog’s allergic reaction with methyl prednisolone at an initial dose of 10 mg/kg/day, which was gradually tapered to 0.5 mg/kg/day over 15 days. Complete blood count and chemical tests at admission, 24 h, and 48 h showed no changes except an increase in the number of neutrophils from 21.2 × 103 cells/µL at admission to 35.4 × 103 cells/µL at 48 h (upper limit 16.9 × 103 cells/µL). The dog was hospitalized for 4 days, but ataxia was still evident after discharge (Video). Clinical signs went into remission 7 days after treatment began.
The dog had been walking and playing with its owners through grassy and brushy areas in a pine forest in Sierra Cebollera National Park, La Rioja, Spain (42°6′Ν, 2°33′Ε), ≈8 hours before the onset of symptoms. One owner had an itchy dermatitis that was diagnosed as trombiculiasis and treated at the Infectious Diseases Department at the Hospital Universitario San Pedro, Logroño, 4 days after the outdoor activities (8). We previously reported on trombiculid mites in the vegetation of certain areas of Sierra Cebollera National Park, their causality in human cases of seasonal dermatitis, and co-occurrence with canine cases (4,6,8–10). However, canine trombiculiasis associated with severe neurologic signs had not been described in Spain.
In dogs, massive infestations with chiggers have been related to death, especially when left untreated (10). Orange spots, especially on the lacrimal areas, can assist in the diagnosis of suspected cases of trombiculiasis and should prompt owners to seek immediate veterinary advice. A severe allergic host response, hypersensitivity to mites or their products, or pathogen transmission have been speculated causes of clinical signs in canids (3). The role of N. inopinata mites collected in La Rioja as vectors of arthropodborne bacteria has not been demonstrated (10), and the clinical signs do not suggest an infectious disease process. We hypothesize that severe cases are attributed to the inflammatory response secondary to infestation, but the mechanism is unknown. However, we cannot disregard the implication of a neurotoxic process.
Successful management of symptoms is dependent on early treatment to remove chiggers. Topical insecticides, especially pyrethroids, are considered effective against chigger infestations in canids (3). Our experience has shown efficacy of isoxazolines, although not label indicated, at eliminating chiggers on dogs within 6–8 hours. As noted in this case, a short course of glucocorticoids at an antiinflammatory dose might be necessary to relieve pruritus and to reduce inflammation (3). Currently, no products are specifically licensed for preventing chigger bites. Sprays containing phenylpyrazole, which is licensed for use in dogs and cats against fleas and ticks, also are thought to be effective against mites. Because trombiculiasis is a seasonal threat, the most useful approach to prevent infestations, if feasible, consists of keeping pets away from areas where exposure can occur whenever chiggers are known to be active. Local veterinarians should be aware of the occurrence of canine trombiculiasis and its clinical signs to properly diagnose and manage this potentially fatal condition.
Dr. Santibáñez is a researcher in the Center of Rickettsiosis and Arthropod-Borne Diseases (CRETAV), Infectious Diseases Department, Hospital Universitario San Pedro–Center for Biomedical Research from La Rioja (CIBIR), Logroño, Spain.
References
- Mullen GR, O’Connor BM. Mites (Acari). In: Mullen GR and Durden LA, editors. Medical and veterinary entomology, 3rd ed. London: Academic Press; 2019. p. 533–602.
- Paris D, Day N. Tropical rickettsial infections. In: Farrar J, Hotez PJ, Junghanss T, Kang G, Lalloo D, White NJ, editors. Manson’s tropical infectious diseases, 23rd ed. Philadelphia: WB Saunders; 2014. p. 273–91.
- Santibáñez P, Palomar AM, Portillo A, Santibáñez S, Oteo JA. The role of chiggers as human pathogens. In: Samie A, editor. An overview of tropical diseases. London: Intech; 2015. p.173–202.
- Oteo JA, Portillo A, Santibáñez S, Blanco JR, Pérez-Martínez L, Ibarra V. Cluster of cases of human Rickettsia felis infection from Southern Europe (Spain) diagnosed by PCR. J Clin Microbiol. 2006;44:2669–71. DOIPubMedGoogle Scholar
- Guarneri C, Chokoeva AA, Wollina U, Lotti T, Tchernev G. Trombiculiasis: not only a matter of animals! [in German]. Wien Med Wochenschr. 2017;167:70–3. DOIPubMedGoogle Scholar
- Stekolnikov AA, Santibáñez P, Palomar AM, Oteo JA. Neotrombicula inopinata (Acari: Trombiculidae) - a possible causative agent of trombiculiasis in Europe. Parasit Vectors. 2014;7:90. DOIPubMedGoogle Scholar
- Kudryashova NI. Chigger mites (Acariformes, Trombiculidae) of East Palaearctics [in Russian]. Moscow: KMK Scientific Press; 1998.
- Santibañez-Sáenz P, Palomar-Urbina AM, Imaña-Rodríguez E, Oteo-Revuelta JA. [Pruritic dermatitis after hiking in the mountains] [in Spanish]. Enferm Infecc Microbiol Clin. 2014;32:610–1.PubMedGoogle Scholar
- Jiménez S, Gastón I, Pérez A, Oteo J. A seasonal outbreak of human parasitation by chiggers in La Rioja (Northern Spain). Clin Microbiol Infect. 2001;7(s1):348.
- Santibáñez P. Trombiculidae and trombiculiasis in La Rioja [dissertation] [in Spanish]. Logroño (Spain): Universidad de La Rioja; 2015.
Figures
Cite This ArticleOriginal Publication Date: March 09, 2020
Table of Contents – Volume 26, Number 4—April 2020
| EID Search Options |
|---|
|
|
|
|
|
|

Please use the form below to submit correspondence to the authors or contact them at the following address:
José A. Oteo, Departamento de Enfermedades Infecciosas, Hospital U. San Pedro–CIBIR, C/Piqueras 98-7ª NE, 26006 Logroño, La Rioja, Spain
Top