Volume 26, Number 5—May 2020
Policy Review
Nonpharmaceutical Measures for Pandemic Influenza in Nonhealthcare Settings—Social Distancing Measures
Figure
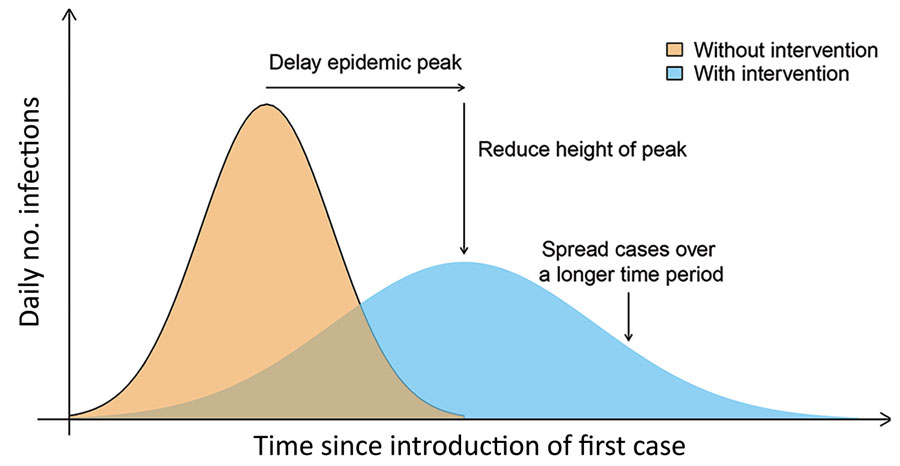
References
- Centers for Disease Control and Prevention. Pandemic influenza, 2019 [cited 2019 Jul 7]. https://www.cdc.gov/flu/pandemic-resources/index.htm
- Ahmed F, Zviedrite N, Uzicanin A. Effectiveness of workplace social distancing measures in reducing influenza transmission: a systematic review. BMC Public Health. 2018;18:518. DOIPubMedGoogle Scholar
- European Centre for Disease Prevention and Control. Guide to public health measures to reduce the impact of influenza pandemics in Europe: The ECDC Menu. Stockholm: The Centre; 2009.
- Qualls N, Levitt A, Kanade N, Wright-Jegede N, Dopson S, Biggerstaff M, et al.; CDC Community Mitigation Guidelines Work Group. Community mitigation guidelines to prevent pandemic influenza—United States, 2017. MMWR Recomm Rep. 2017;66:1–34. DOIPubMedGoogle Scholar
- Bell D, Nicoll A, Fukuda K, Horby P, Monto A, Hayden F, et al.; World Health Organization Writing Group. Non-pharmaceutical interventions for pandemic influenza, international measures. Emerg Infect Dis. 2006;12:81–7. DOIPubMedGoogle Scholar
- Markel H, Lipman HB, Navarro JA, Sloan A, Michalsen JR, Stern AM, et al. Nonpharmaceutical interventions implemented by US cities during the 1918-1919 influenza pandemic. JAMA. 2007;298:644–54. DOIPubMedGoogle Scholar
- Caley P, Philp DJ, McCracken K. Quantifying social distancing arising from pandemic influenza. J R Soc Interface. 2008;5:631–9. DOIPubMedGoogle Scholar
- Chu CY, de Silva UC, Guo JP, Wang Y, Wen L, Lee VJ, et al. Combined interventions for mitigation of an influenza A (H1N1) 2009 outbreak in a physical training camp in Beijing, China. Int J Infect Dis. 2017;60:77–82. DOIPubMedGoogle Scholar
- Gaillat J, Dennetière G, Raffin-Bru E, Valette M, Blanc MC. Summer influenza outbreak in a home for the elderly: application of preventive measures. J Hosp Infect. 2008;70:272–7. DOIPubMedGoogle Scholar
- Vera DM, Hora RA, Murillo A, Wong JF, Torre AJ, Wang D, et al. Assessing the impact of public health interventions on the transmission of pandemic H1N1 influenza a virus aboard a Peruvian navy ship. Influenza Other Respir Viruses. 2014;8:353–9. DOIPubMedGoogle Scholar
- Fraser C, Riley S, Anderson RM, Ferguson NM. Factors that make an infectious disease outbreak controllable. Proc Natl Acad Sci U S A. 2004;101:6146–51. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Influenza (flu) preventive steps, 2018 [cited 2019 Jul 7]. https://www.cdc.gov/flu/prevent/prevention.htm
- Cowling BJ, Chan KH, Fang VJ, Lau LLH, So HC, Fung ROP, et al. Comparative epidemiology of pandemic and seasonal influenza A in households. N Engl J Med. 2010;362:2175–84. DOIPubMedGoogle Scholar
- Patrozou E, Mermel LA. Does influenza transmission occur from asymptomatic infection or prior to symptom onset? Public Health Rep. 2009;124:193–6. DOIPubMedGoogle Scholar
- Wu JT, Riley S, Fraser C, Leung GM. Reducing the impact of the next influenza pandemic using household-based public health interventions. PLoS Med. 2006;3:
e361 . DOIPubMedGoogle Scholar - Peak CM, Childs LM, Grad YH, Buckee CO. Comparing nonpharmaceutical interventions for containing emerging epidemics. Proc Natl Acad Sci U S A. 2017;114:4023–8. DOIPubMedGoogle Scholar
- An der Heiden M, Buchholz U, Krause G, Kirchner G, Claus H, Haas WH. Breaking the waves: modelling the potential impact of public health measures to defer the epidemic peak of novel influenza A/H1N1. PLoS One. 2009;4:
e8356 . DOIPubMedGoogle Scholar - Miyaki K, Sakurazawa H, Mikurube H, Nishizaka M, Ando H, Song Y, et al. An effective quarantine measure reduced the total incidence of influenza A H1N1 in the workplace: another way to control the H1N1 flu pandemic. J Occup Health. 2011;53:287–92. DOIPubMedGoogle Scholar
- Fujita M, Sato H, Kaku K, Tokuno S, Kanatani Y, Suzuki S, et al. Airport quarantine inspection, follow-up observation, and the prevention of pandemic influenza. Aviat Space Environ Med. 2011;82:782–9. DOIPubMedGoogle Scholar
- Li X, Geng W, Tian H, Lai D. Was mandatory quarantine necessary in China for controlling the 2009 H1N1 pandemic? Int J Environ Res Public Health. 2013;10:4690–700. DOIPubMedGoogle Scholar
- van Gemert C, Hellard M, McBryde ES, Fielding J, Spelman T, Higgins N, et al. Intrahousehold transmission of pandemic (H1N1) 2009 virus, Victoria, Australia. Emerg Infect Dis. 2011;17:1599–607. DOIPubMedGoogle Scholar
- McLeod MA, Baker M, Wilson N, Kelly H, Kiedrzynski T, Kool JL. Protective effect of maritime quarantine in South Pacific jurisdictions, 1918-19 influenza pandemic. Emerg Infect Dis. 2008;14:468–70. DOIPubMedGoogle Scholar
- Ferguson NM, Cummings DA, Fraser C, Cajka JC, Cooley PC, Burke DS. Strategies for mitigating an influenza pandemic. Nature. 2006;442:448–52. DOIPubMedGoogle Scholar
- World Health Organization. Ethical considerations in developing a public health response to pandemic influenza. Report no. WHO/CDS/EPR/GIP/2007.2. Geneva: The Organization; 2007.
- Lessler J, Reich NG, Brookmeyer R, Perl TM, Nelson KE, Cummings DA. Incubation periods of acute respiratory viral infections: a systematic review. Lancet Infect Dis. 2009;9:291–300. DOIPubMedGoogle Scholar
- Rothstein MA, Talbott MK. Encouraging compliance with quarantine: a proposal to provide job security and income replacement. Am J Public Health. 2007;97(Suppl 1):S49–56. DOIPubMedGoogle Scholar
- Jackson C, Vynnycky E, Hawker J, Olowokure B, Mangtani P. School closures and influenza: systematic review of epidemiological studies. BMJ Open. 2013;3:
e002149 . DOIPubMedGoogle Scholar - Cauchemez S, Ferguson NM, Wachtel C, Tegnell A, Saour G, Duncan B, et al. Closure of schools during an influenza pandemic. Lancet Infect Dis. 2009;9:473–81. DOIPubMedGoogle Scholar
- Bootsma MC, Ferguson NM. The effect of public health measures on the 1918 influenza pandemic in U.S. cities. Proc Natl Acad Sci U S A. 2007;104:7588–93. DOIPubMedGoogle Scholar
- Cowling BJ, Lau MS, Ho LM, Chuang SK, Tsang T, Liu SH, et al. The effective reproduction number of pandemic influenza: prospective estimation. Epidemiology. 2010;21:842–6. DOIPubMedGoogle Scholar
- Wu JT, Cowling BJ, Lau EH, Ip DK, Ho LM, Tsang T, et al. School closure and mitigation of pandemic (H1N1) 2009, Hong Kong. Emerg Infect Dis. 2010;16:538–41. DOIPubMedGoogle Scholar
- Kawano S, Kakehashi M. Substantial impact of school closure on the transmission dynamics during the pandemic flu H1N1–2009 in Oita, Japan. PLoS One. 2015;10:
e0144839 . DOIPubMedGoogle Scholar - Sato T, Akita T, Tanaka J. Evaluation of strategies for control and prevention of pandemic influenza (H1N1pdm) in Japanese children attending school in a rural town. Simulation using mathematical models. Nihon Koshu Eisei Zasshi. 2013;60:204–11.PubMedGoogle Scholar
- Chen T, Huang Y, Liu R, Xie Z, Chen S, Hu G. Evaluating the effects of common control measures for influenza A (H1N1) outbreak at school in China: A modeling study. PLoS One. 2017;12:
e0177672 . DOIPubMedGoogle Scholar - Chen T, Zhao B, Liu R, Zhang X, Xie Z, Chen S. Simulation of key interventions for seasonal influenza outbreak control at school in Changsha, China. J Int Med Res. 2020;48:
300060518764268 . DOIPubMedGoogle Scholar - Cauchemez S, Bhattarai A, Marchbanks TL, Fagan RP, Ostroff S, Ferguson NM, et al.; Pennsylvania H1N1 working group. Role of social networks in shaping disease transmission during a community outbreak of 2009 H1N1 pandemic influenza. Proc Natl Acad Sci U S A. 2011;108:2825–30. DOIPubMedGoogle Scholar
- Luca G, Kerckhove KV, Coletti P, Poletto C, Bossuyt N, Hens N, et al. The impact of regular school closure on seasonal influenza epidemics: a data-driven spatial transmission model for Belgium. BMC Infect Dis. 2018;18:29. DOIPubMedGoogle Scholar
- Te Beest DE, Birrell PJ, Wallinga J, De Angelis D, van Boven M. Joint modelling of serological and hospitalization data reveals that high levels of pre-existing immunity and school holidays shaped the influenza A pandemic of 2009 in the Netherlands. J R Soc Interface. 2015;12:
20141244 . DOIPubMedGoogle Scholar - Birrell PJ, Ketsetzis G, Gay NJ, Cooper BS, Presanis AM, Harris RJ, et al. Bayesian modeling to unmask and predict influenza A/H1N1pdm dynamics in London. Proc Natl Acad Sci U S A. 2011;108:18238–43. DOIPubMedGoogle Scholar
- Chowell G, Towers S, Viboud C, Fuentes R, Sotomayor V. Rates of influenza-like illness and winter school breaks, Chile, 2004-2010. Emerg Infect Dis. 2014;20:1203–7. DOIPubMedGoogle Scholar
- Chu Y, Wu Z, Ji J, Sun J, Sun X, Qin G, et al. Effects of school breaks on influenza-like illness incidence in a temperate Chinese region: an ecological study from 2008 to 2015. BMJ Open. 2017;7:
e013159 . DOIPubMedGoogle Scholar - Germann TC, Gao H, Gambhir M, Plummer A, Biggerstaff M, Reed C, et al. School dismissal as a pandemic influenza response: When, where and for how long? Epidemics. 2019;28:
100348 . DOIPubMedGoogle Scholar - Reich NG, Brooks LC, Fox SJ, Kandula S, McGowan CJ, Moore E, et al. A collaborative multiyear, multimodel assessment of seasonal influenza forecasting in the United States. Proc Natl Acad Sci U S A. 2019;116:3146–54. DOIPubMedGoogle Scholar
- Asfaw A, Rosa R, Pana-Cryan R. Potential economic benefits of paid sick leave in reducing absenteeism related to the spread of influenza-like illness. J Occup Environ Med. 2017;59:822–9. DOIPubMedGoogle Scholar
- Piper K, Youk A, James AE III, Kumar S. Paid sick days and stay-at-home behavior for influenza. PLoS One. 2017;12:
e0170698 . DOIPubMedGoogle Scholar - Zhai Y, Santibanez TA, Kahn KE, Black CL, de Perio MA. Paid sick leave benefits, influenza vaccination, and taking sick days due to influenza-like illness among U.S. workers. Vaccine. 2018;36:7316–23. DOIPubMedGoogle Scholar
- Ahmed F, Kim S, Nowalk MP, King JP, VanWormer JJ, Gaglani M, et al. Paid leave and access to telework as work attendance determinants during acute respiratory illness, United States, 2017–2018. Emerg Infect Dis. 2020;26:26. DOIPubMedGoogle Scholar
- Hatchett RJ, Mecher CE, Lipsitch M. Public health interventions and epidemic intensity during the 1918 influenza pandemic. Proc Natl Acad Sci U S A. 2007;104:7582–7. DOIPubMedGoogle Scholar
- Staff M, Torres MI. An influenza outbreak among pilgrims sleeping at a school without purpose built overnight accommodation facilities. Commun Dis Intell Q Rep. 2011;35:10–5.PubMedGoogle Scholar
- Leung NH, Xu C, Ip DK, Cowling BJ. The fraction of influenza virus infections that are asymptomatic: a systematic review and meta-analysis. Epidemiology. 2015;26:862–72. DOIPubMedGoogle Scholar
1These first authors contributed equally to this article.
Page created: April 16, 2020
Page updated: April 16, 2020
Page reviewed: April 16, 2020
The conclusions, findings, and opinions expressed by authors contributing to this journal do not necessarily reflect the official position of the U.S. Department of Health and Human Services, the Public Health Service, the Centers for Disease Control and Prevention, or the authors' affiliated institutions. Use of trade names is for identification only and does not imply endorsement by any of the groups named above.