Volume 28, Number 7—July 2022
Research Letter
Hodgkin Lymphoma after Disseminated Mycobacterium genavense Infection, Germany
Cite This Article
Citation for Media
Abstract
Mycobacterium genavense infection, a rare nontuberculous mycobacteria infection, occurs in heavily immunocompromised patients (i.e., those with advanced HIV disease, genetic disorders, or acquired immunologic disorders and those undergoing immunosuppressive therapy). We report a case of disseminated M. genavense infection preceding Hodgkin lymphoma in a patient without obvious risk factors for this infection.
Mycobacterium genavense was first described in 1992 in HIV-positive patients with low CD4 counts and disseminated mycobacterial disease (1). Since the 2000s, additional risk factors for this bacterial infection became known (e.g., solid organ transplantation, hematopoietic stem cell transplantation, Epstein-Barr virus–associated lymphoproliferative disorder, neutralizing anti–interferon γ autoantibodies, adenosine deaminase deficiency, nuclear factor κB1 deficiency) (2,3). Clinical manifestations of M. genavense commonly involve blood and lymph nodes but can include the gastrointestinal tract, spleen, liver, and bone marrow; pneumonia, prosthetic joint infection, endobronchial mass, and brain mass have also been described.
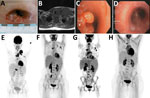
A previously healthy 23-year-old woman sought medical treatment at University Hospital Gießen (Gießen, Germany) for progressive cervical lymphadenopathy (Figure, panel A) and fever originating 4 months prior. A professional animal keeper, she had no history of previous infections or autoimmune disease, an unremarkable family history, and no travel outside of Europe; her tattoos showed no signs of irritation. She experienced gender dysphoria and used masculinizing hormone therapy (testosterone). We excluded common causes of cervical lymphadenopathy (e.g., HIV, tuberculosis, bacterial abscess, Epstein-Barr virus, lymphoma, toxoplasmosis, bartonellosis, and syphilis), but the extensive lymphadenopathy pointed to a severe disease (Figure, panel B, E). Multiple conglomerate, necrotizing mediastinal lymph nodes resulted in a tracheo-esophageal fistula (Figure, panel C), which required esophageal stenting.
Cervical lymph nodes showed a necrotizing, giant cell–containing inflammatory reaction. We detected acid-fast bacteria on microscopic examination and subsequently identified it as M. genavense by using broad-range 16S-rDNA PCR and Sanger sequencing of the resulting amplicon (Appendix). In blood and bone marrow, we detected no mycobacteria. From culture on solid medium and mycobacteria growth indicator tube, we were unable to recover outgrowth. M. genavense cannot be cultivated in routine liquid and solid media (Löwenstein–Jensen and Stonebrink) but requires special supplementation for recovery on culture (Middlebrook 7H11 agar [ThermoFisher, https://www.thermofisher.com] supplemented with mycobactin J) and an incubation period >100 days. Standardized susceptibility testing is not available (4).
For this nontuberculous mycobacteria (NTM) disease, diagnostic criteria are ill defined and no treatment guidelines are established. Reported case-patients are treated with a 2- to 4-drug regimen, including mostly macrolides, rifampin, ethambutol, and amikacin or fluroquinolones. The regimen for this patient consisted of clarithromycin, rifabutin, ethambutol, and temporary add-on doses of levofloxacin, amikacin, clofazimine, or bedaquiline. During the ensuing months, the wounds and tracheo-esophageal fistula slowly healed (Figure, panel D), and imaging showed decreased uptake (Figure, panel F).
As a professional pet keeper, the patient had close contact with domestic animals, including birds. Zoonotic transmission of M. genavense has not been well described (5), but it does pose a potential risk for susceptible hosts. Because a predisposing risk factor for the patient’s NTM disease had not been identified, we ruled out several conditions: acquired immunodeficiency, idiopathic CD4 lymphocytopenia, Mendelian susceptibility to mycobacterial disease, and neutralizing anti–interferon γ autoantibodies or a defect in the (proximal) interferon γ receptor signaling pathway (data not shown). A targeted gene panel with a focused analysis on 810 genes associated with immune and blood disorders did not identify a genetic variant that could alone explain the phenotype; however, we detected several rare variants (Appendix).
After 11 months of antibiotic therapy, an 18F-FDG-PET scan revealed new lymphadenopathy and splenomegaly (Figure, panel G). CD4-to-CD8 ratio dropped from 1.7 to 1.0, and we found new low-level EBV viremia (350 copies/mL). On the basis of new tissue samples from mediastinal lymph nodes, we diagnosed classical Hodgkin lymphoma (HL [mixed type]) stage IV. Mycobacterial PCR was negative in all these samples and, retrospectively, all previous samples were tumor-free. Six cycles of chemotherapy (brentuximab combined with doxorubicin, vinblastine, dacarbazine) were followed by 4 doses of nivolumab because of histologically confirmed mixed response. One year after treatment completion and cessation of antimycobacterial therapy, liquid biopsy and an 18F-FDG-PET scan showed complete remission and no signs of NTM infection (Figure, panel H).
In other reports of M. genavense infections related to lymphomas, patients acquired the infection during immunosuppressive therapy; however, in this patient, infection preceded HL. Genetic and environmental factors are relevant in the pathogenesis of HL (6) and in pathogenic pathways triggered by virus infections (e.g., HIV and Epstein-Barr virus) (7); bacterial antigen triggering has been implicated recently in early developmental stages of the disease (8). Other reports have discussed an increased risk for HL after tuberculosis infection (9) and HL associated with concomitant tuberculosis, leprosy, and Mycobacterium avium complex disease (10).
M. genavense remains a diagnostic challenge because standard media and incubation times do not yield bacterial growth, which can result in missed diagnoses. Research is needed to gain a clear understanding of the interplay of NTM and HL, specifically in regard to how mycobacterial antigens trigger pathogenic pathways during HL development and the role of HL in causing local immune escape mechanisms and immunologic imbalance resulting in susceptibility to infections.
In conclusion, we report a patient with disseminated M. genavense infection preceding HL who recovered after antimycobacterial therapy and first- and second-line chemotherapy. A zoonotic source of M. genavense infection is likely. Furthermore, because sex hormones affect immunity and testosterone is a susceptibility factor for mycobacterial disease, masculinizing hormone therapy could have contributed to susceptibility.
Dr. Trauth is attending physician at University Hospital Gießen, Germany. Her primary interests include pulmonary infections and antibiotic stewardship.
References
- Böttger EC, Teske A, Kirschner P, Bost S, Chang HR, Beer V, et al. Disseminated “Mycobacterium genavense” infection in patients with AIDS. Lancet. 1992;340:76–80. DOIPubMedGoogle Scholar
- Bustamante J, Boisson-Dupuis S, Abel L, Casanova J-L. Mendelian susceptibility to mycobacterial disease: genetic, immunological, and clinical features of inborn errors of IFN-γ immunity. Semin Immunol. 2014;26:454–70. DOIPubMedGoogle Scholar
- Mahmood M, Ajmal S, Abu Saleh OM, Bryson A, Marcelin JR, Wilson JW. Mycobacterium genavense infections in non-HIV immunocompromised hosts: a systematic review. Infect Dis (Lond). 2018;50:329–39. DOIPubMedGoogle Scholar
- Griffith DE, Aksamit T, Brown-Elliott BA, Catanzaro A, Daley C, Gordin F, et al.; ATS Mycobacterial Diseases Subcommittee; American Thoracic Society; Infectious Disease Society of America. An official ATS/IDSA statement: diagnosis, treatment, and prevention of nontuberculous mycobacterial diseases. Am J Respir Crit Care Med. 2007;175:367–416. DOIPubMedGoogle Scholar
- Schmitz A, Korbel R, Thiel S, Wörle B, Gohl C, Rinder M. High prevalence of Mycobacterium genavense within flocks of pet birds. Vet Microbiol. 2018;218:40–4. DOIPubMedGoogle Scholar
- Cartwright RA, Watkins G. Epidemiology of Hodgkin’s disease: a review. Hematol Oncol. 2004;22:11–26. DOIPubMedGoogle Scholar
- Carbone A, Gloghini A, Caruso A, De Paoli P, Dolcetti R. The impact of EBV and HIV infection on the microenvironmental niche underlying Hodgkin lymphoma pathogenesis. Int J Cancer. 2017;140:1233–45. DOIPubMedGoogle Scholar
- Weniger MA, Küppers R. Molecular biology of Hodgkin lymphoma. Leukemia. 2021;35:968–81. DOIPubMedGoogle Scholar
- Li G, Chen G-L, Zhou Y, Yao G-Q, Yang S, Ji D-M. Increased risk of lymphoma in men or the elderly infected with tuberculosis. Mediterr J Hematol Infect Dis. 2021;13:
e2021053 . DOIPubMedGoogle Scholar - Varkey MR, Ali J, Lapinel NC. The chicken and the egg dilemma: A case of disseminated MAC with Hodgkin’s lymphoma. Respir Med Case Rep. 2020;31:
101253 . DOIPubMedGoogle Scholar
Figure
Cite This ArticleOriginal Publication Date: June 09, 2022
Table of Contents – Volume 28, Number 7—July 2022
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Janina Trauth, University Hospital Gießen and Marburg GmbH, Section of Infectious Diseases, Klinikstr 33, 35392 Gießen, Germany
Top