Volume 6, Number 1—February 2000
Perspective
Japanese Encephalitis Immunization in South Korea: Past, Present, and Future
Cite This Article
Citation for Media
Abstract
Japanese encephalitis (JE), once a major public health problem in South Korea, has declined since the 1980s, as a result of improved living conditions, a mosquito eradication program, and a national JE vaccination program, which includes annual booster vaccine for all children < 15 years of age. Increased immunity has greatly reduced illness and death; however, vaccine adverse effects are increasing, and a National Compensation Program for Vaccine Injury was begun in 1995. This article reviews past successes, current problems, and future direction of the JE vaccination program in South Korea.
Historically, JE occurred seasonally in South Korea, causing high rates of illness and death. Although public health records concerning the incidence of the disease before 1933 are not available, outbreaks of "summer encephalitis" were recognized. During summer 1934-35, an outbreak was reported of suspected encephalitis, with acute onset of spiking fever and headache, as well as neurologic abnormalities and mental changes. Although these outbreaks were described as meningococcal meningitis by Korean health authorities, some Japanese workers reported that many of the cases were encephalitis (1,2). In 1946, Sabin et al. (3) isolated JE virus from an American soldier stationed in South Korea. Deuel et al. (4) conducted the first extensive serologic survey by neutralizing test in four areas of South Korea and reported that JE virus was widely disseminated. In 1947, JE was added to the list of first-class emergency diseases in South Korea.
In 1949, when JE became notifiable, 5,548 cases of clinically suspected disease were reported with 2,429 deaths (49% case-fatality rate). The criteria for reporting were high spiking fever, headache, and mental changes with any symptom of central nervous system involvement. Hullinghorst et al. (1), who described the 1949 epidemic in South Korea, reviewed >600 hospital records. Results of bacterial cultures of cerebrospinal fluid (CSF) were reviewed for 567 cases, and the complement fixation and neutralization tests were performed in selected cases. Pathology findings and JE virus isolation from a case, negative results of CSF bacterial cultures, and a relatively uniform clinical picture, including acute high fever, headache, and various neurologic abnormalities, suggested that the outbreak in 1949 was JE (1,5). Thereafter, several outbreaks of thousands of JE cases were reported every 2 to 3 years, and JE was recognized as a recurring public health problem in South Korea (6,7).
In 1954, when the Communicable Disease Control Act (Reg. 308) was enacted, JE was classified as a first-class notifiable communicable disease. The largest recorded JE epidemic, involving 6,897 reported cases, occurred in 1958 (7). In 1963, JE was reclassified as a second-class notifiable disease, along with polio, pertussis, measles, mumps, and other childhood diseases. Since 1964, seroepidemiologic studies with the hemagglutination inhibition test (HI) have been conducted routinely for clinically suspected cases. In 1964, 108 paired and 1,636 acute-phase sera were tested (8). The results indicated that 86.7% of acute-phase sera were negative by the HI test and 54% of paired sera were positive in their second sample. Several thousand cases were reported annually until 1968, with the exception of 1963, when only 19 cases were reported; Chang et al. (9) provide evidence for underreporting in that year (Figure 1). Case reports sharply declined to <100 cases in 1969; <1,000 cases were reported annually until 1973. The last large epidemic was recorded in 1982, when 1,197 cases and 40 deaths were reported. This rapid decline in reported cases may be related to the extensive use of insecticides in rice farming, which led to a marked decrease of Culex tritaeniorhynchus in rural habitats (10,11).
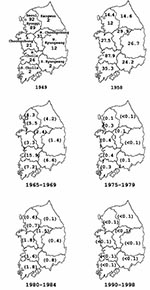
The highest incidence of JE was recorded in Seoul and Kyonggi Province during the first officially reported outbreak in 1949 (Figure 2A). In the epidemics during 1965 to 1984, a higher incidence was recorded in the southwestern than in the northeastern provinces (Figure 2B). The southwestern provinces are mainly under rice cultivation with large flooded rice paddies, while the northeastern provinces are mountainous. Vector mosquito populations were more prevalent in the southwest than in the northeast (8), leading to greater risk for enzootic viral transmission in the southwestern provinces. The high incidence in Seoul in the 1949 outbreak may be accounted for by the rapidly increasing susceptible population in the capital and its suburbs since 1945 (7). Approximately 90% of the cases occurred from mid-August to mid-September; more than 80% were among children 3 to 15 years of age (9,10).
Factors affecting the size of JE epidemics include the risk for being infected by the virus when bitten by a vector mosquito and the JE seropositive rate in the population. In 1965, before the national vaccination program was implemented, Chang et al. (9) estimated the natural seroconversion rate of HI antibody in children <15 years of age at approximately 9%, indicating that the estimated incidence of JE cases during epidemics would have been higher without intervention. Several studies comparing seroprevalence rates before and after the epidemic season indicated that the seropositivity rate was higher in South Choongchung Province (86.4% before the epidemic season vs ~100% after the epidemic season in 1984) than in Seoul (56% before the epidemic season vs ~72% after the epidemic season in 1987) (Figure 3) (12-15).
From 1985 to 1998, only 21 cases of JE were serologically confirmed. Factors leading to this decrease include the National Immunization Program (NIP), initiated in 1983, which has conferred protective immunity on children at risk. The national socioeconomic growth for the past 3 decades has allowed improved standards of living and environmental conditions. The modernization of agricultural practices led to changes in the epidemiology of JE.
Since 1975, an epidemic forecast program to alert the public against JE has been implemented by the health authorities every year before the epidemic season (16) (Table 1). To predict the possibility of an outbreak, the health authorities have attempted to isolate the virus from the vector mosquito, C. tritaeniorhynchus; estimate population density of C. tritaeniorhynchus among captured mosquitoes; and determine JE antibody levels in pigs. Monitoring for C. tritaeniorhynchus begins in early May. The population density of C. tritaeniorhynchus in mosquitos captured in seven urban and rural areas was 76.1% in 1982, when the most recent epidemic occurred (11). Because outbreaks in humans seem closely related to a rapid rise of HI antibody titers in pigs, the blood of young pigs (<6 months old) is screened weekly at slaughterhouses for immunoglobulin (Ig) M antibody. In areas where epidemics have occurred, vector mosquitos collected are homogenized and injected into suckling mice; JE virus is identified by HI and, recently, by polymerase chain reaction in the brains of mice manifesting JE symptoms.
When the JE vector mosquito is first detected, health authorities issue an alert that encourages JE vaccination (Table 1). If JE IgM antibody titers increase in pigs or JE virus is isolated, aggressive mosquito control is implemented.
A small amount of the mouse brain-derived formalin-inactivated Nakayama vaccine from Japan was imported in 1967 (17,18). In the early 1970s, the Nakayama vaccine began to be produced locally. Despite an active campaign with the Nakayama vaccine, the annual number of doses distributed remained under 500,000 in the 1970s, for a vaccine coverage rate of <5% (11). However, the vaccine coverage rate increased to 16.8% in 1981. The most recent epidemics—1,197 reported cases in 1982 and 139 in 1983—prompted a mass immunization program for children at risk. Children 3 to 15 years of age were vaccinated at state public health centers, and simultaneous vaccination in the private sector was encouraged; as a result, the immunization rate increased to 60% in 1983, when a JE epidemic occurred. In 1986, 12 million doses were distributed in the public and private sectors, which was more than the estimated number of children <15 years of age. From 1985 to 1992, almost 10 million doses of Nakayama vaccine were distributed each year, enough to vaccinate 97% of the nation's children (Figure 1).
In 1983, the age of initial dose of JE vaccine was recommended by the health authorities at 3 years of age, except for areas in which the disease had recently become endemic, where it could be given earlier. The series consisted of three doses of primary vaccination, with annual boosters until 15 years of age. Because the vaccination rate could not be maintained above 90% by individual immunization during the spring campaign (May to July), mass immunization at schools and public health centers was used.
Since 1984, when JE vaccine coverage reached almost 90%, only a few sporadic cases occurred in young adults or the elderly. The incidence of JE was reduced from >18.5/105 in 1964 to <0.02/105 over the past 3 decades. Several factors contributed to the rapid decline. In addition to improved living conditions, public health, the widespread use of agricultural herbicides and insecticides, a decrease in the population density of vector mosquitos by the removal of mosquito habitats, and the modernization of agricultural practices, such as improved sanitary conditions on pig farms in rural areas, may have decreased the risk for human infection. In South Korea, C. tritaeniorhyncus usually appears in May and multiplies rapidly in July and August. From 1982 to 1985, mosquitos were collected in seven areas from May to late October. The number of mosquitos gradually decreased, from 11,278 per day (76% C. tritaeniorhyncus) in 1982; to 4,334 (59.2%) in 1983; 2,150 (40.3%) in 1984; and 1,212 (34.4%) in 1985 (11). The virus infestation rate of the vector mosquito has been consistently <1% since 1990. Consequently, the risk of being exposed to the vector mosquito and infected by JE virus has decreased.
Another contributing factor is the policy of maintaining high levels of immunity through the expansion of the routine childhood immunization program. An immunization coverage rate >97% has significantly contributed to the prevention of JE. In 1969, a JE vaccine efficacy trial was performed among schoolchildren in southwestern provinces in South Korea; approximately 45,000 children were vaccinated and another 45,000 were controls. Although no epidemic occurred during this period (19,20) because of vaccination, the HI seropositive rate of 11.6% in prevaccination sera increased to 75% in postvaccination sera after two doses of mouse brain-derived Nakayama vaccine. The seropositivity rate by neutralizing antibody test was 99% postvaccination.
At present, visitors to South Korea on business or vacation are considered at low risk for JE; routine vaccination with Nakayama vaccine may not be necessary for these travelers. However, JE immunization is recommended for visitors to disease-endemic areas during transmission season. Vaccine is advised especially for travelers who stay for an extended time (>30 days) or are at high risk for exposure to vector mosquitos through activities or housing.
In 1972, the manufacture of Nakayama JE vaccine was privatized and transferred to the South Korea Green Cross Company. Currently, seven pharmaceutical companies manufacture JE vaccine. Before 1995, when boosters were given annually, the total amount of vaccine needed for the population at risk was 8,500 to 9,000 liters per year. Vaccine production is projected more than 1 year in advance; the amount to be used the next year is usually determined in February. Then the injection of JE virus into mice, recovery of the virus from mouse brain tissue, and production of bulk vaccine begin. Vaccine is ready in October, and after a thorough testing in January of the following year, is distributed in March.
Although the mass immunization campaign was successful in attaining high rates of vaccination coverage, JE vaccine-related adverse effects may have been overlooked. A reporting system was not available until 1995, so the incidence of JE vaccine-related adverse effects among South Korean children is not known. However, in 1994, six cases of severe systemic illness after JE vaccination were reported (21) (Table 2). Two sudden deaths were attributed to anaphylactic reaction to the vaccine, and four cases of severe neurologic illness, including encephalopathy and acute disseminated encephalomyelitis, were reported. Since 1994, seven cases have been filed with the Advisory Committee of the National Immunization Program, according to the National Compensation Program for Vaccine Injury (Table 2).
Although the cost-effectiveness of the JE immunization program, including annual boosters, has not been evaluated, JE has been successfully controlled in South Korea for the past 2 decades. Questions remain about the optimum immunization schedule, including appropriate ages for initial vaccination and boosters. The state health authority recommends two doses 4 weeks apart with a booster 1 year later as a primary immunization, and annual boosters thereafter up to 15 years of age. Since the longevity of neutralizing antibody after primary vaccination was not known and seemed short lived, frequent boosters appeared necessary. However, without sound evidence, the total of 14 doses of vaccine until 15 years of age led to concerns about excessive vaccination and increased risk for vaccine adverse effects.
The 1994 report of the cluster of severe adverse systemic effects after JE vaccination prompted medical and social debate (22,23). A causal association between JE vaccine and the cluster of severe adverse effects has not been clearly established; however, empiric evidence, including the timing of events, characteristics of the adverse reactions, susceptibility, and lack of alternative etiologic agents, indicates a causal relationship. Public concern over adverse reactions led to refusal of the vaccination and a consequent decrease in coverage rate. In response, the National Compensation Program for Vaccine Injury was begun in 1995.
During public debate about the JE immunization schedule, the safety and quality of the domestically produced JE vaccines were questioned. The Advisory Committee of the National Immunization Program announced that the annual booster immunization schedule had become impractical because of the inappropriate administration of the vaccine during the mass immunization in the spring, the need to define the long-term immunity in the elderly (> 65 years of age), poor recognition of adverse effects, the need to guarantee the quality of the vaccine manufactured in South Korea, and public reluctance to receive JE vaccination. The committee agreed that the JE immunization program should be improved with regard to the schedule, age of initial vaccination, booster schedule, and vaccine strain. The annual booster schedule was changed to once every 2 years, and single-dose rather than multidose vials were used, as recommended by the South Korean Society of Pediatricians.
In 1996, a seroprevalence study for plaque-reduction neutralizing antibody (PRNT) was carried out to indirectly evaluate the efficacy of booster vaccination in 311 schoolchildren (24). The neutralizing antibody titers were found to decrease gradually as the interval between boosters increased (Figure 4A). The seropositivity rate of 98.1%, 99%, and 95.6% at 6, 18, and 30 months, respectively, had declined to 71.4% by 42 months (Figure 4B). To replace the inactivated mouse brain-derived vaccine, a clinical trial with a live attenuated SA14-14-2 vaccine, which has been used safely and effectively in >100 million children in China since 1988 (25), was conducted in South Korean children in 1997. A preliminary immunogenicity study among South Korean children 1 to 3 years of age indicated a 96% rate of seroconversion in PRNT antibody, with a geometric mean titer (GMT) of 188 after a single primary immunization dose. In children who had been immunized with two or three doses of inactivated Nakayama vaccine, the booster administration of SA14-14-2 vaccine produced an anamnestic response with a GMT of 3,378 in all cases without virus-specific IgM response (Figure 5) (26).
During the last 10 years, JE has occurred more frequently in adults than in childrentwo-thirds of Korean JE patients were middle-aged adults. Adults are not protected by the current immunization program, probably because of waning immunity. Long-term immunity must be maintained to prevent secondary vaccine failure. A single booster with the live-attenuated SA14-14-2 vaccine might confer long-term immunity for adults and decrease the frequency of vaccination, as well as the risk for vaccine adverse effects.
The national immunization program against JE in children should be continued according to established schedules in South Korea; however, the booster schedule should be adjusted. Surveillance for JE and vaccine adverse reactions should be strengthened to better assess the number of cases and reactions associated with immunization. A new, more advanced vaccine, such as the live attenuated SA14-14-2 vaccine, should be adopted and integrated into the pediatric immunization schedule.
Dr. Sohn is professor of pediatric infectious disease at Yonsei University and a member of the Advisory Committee of the National Immunization Program. He was a member of a working group for the improvement of the national immunization program and of an ad hoc committee for assessing JE vaccine adverse effects. He also participated in the clinical trial of SA14-14-2 vaccine in South Korea.
Acknowledgment
This work was supported in part by grants from the Advisory Committee of the National Immunization Program, Department of Health and Welfare Grant no. HMP-98-P-0008.
References
- Hullinghorst RL, Burns KF, Choi YT, Whatley LR. Japanese B encephalitis in Korea. The epidemic of 1949. JAMA. 1951;145:460–6.
- Shiba Y, Chun CH. On epidemic encephalitis or so-called summer encephalitis occurring in Seoul last summer. Journal of Mansen No Ikai. 1935;180:1.
- Sabin AB, Schlesinger RW, Ginder WR, Matsumoto M. Japanese B encephalitis in an American soldier in Korea. Am J Hyg. 1947;46:356–75.PubMedGoogle Scholar
- Deuel RE, Bawell MB, Matumoto M, Sabin AB. Status and significance of inapparent infection with virus of Japanese B encephalitis in Korea and Okinawa in 1946. Am J Hyg. 1950;51:13–20.PubMedGoogle Scholar
- Lee SY, Kim UY. Studies on the epidemic of Japanese B encephalitis in Korea 1949. Part 1: Studies on the virus isolation. Bulletin of National Institute for Prevention of Infectious Disease. 1950;2:54–69.
- Chang KS, Han JS, Lee BH. Epidemiological observation of Japanese B encephalitis in Korea, 1958. The New Medical Journal. 1959;2:75–82.
- Chang IJ. Epidemiology of Japanese encephalitis in Korea. Korean Medical Journal. 1959;4:35–50.
- Kim KH, Paik SB, Whang CH, Kim HD. Seroepidemiology of Japanese encephalitis in Korea, 1964. Report of National Institute of Health, Korea 1965;2:63-9.
- Chang IC, Hong KW, Whang KS. Japanese encephalitis in Korea, 1963. Human serology. Korean Medical Journal. 1965;10:77–92.
- Kim KH. Epidemiological features of Japanese encephalitis in the Republic of Korea. Korean Journal of Virology. 1979;9:43–55.
- Lee CW, Oh DK. Epidemiological trend of Japanese encephalitis in Korea. Korean Journal of Preventive Medicine. 1987;20:137–46.
- Lee YT, Youm BJ. A hemagglutination inhibition antibody test for Japanese encephalitis virus among the Koreans, 1984-1985. Journal of Korean Society of Virology. 1986;15:1–9.
- Lee YT, Cho KB, Kang PW, Hong SH, Park CH, Youm BJ. Distribution of hemagglutination inhibition antibody to Japanese encephalitis virus in Koreans 1987. Journal of Korean Society of Virology. 1989;19:41–7.
- Lee CH, Lee YT, Ko KK, Moon KS, Kim OJ. The distribution of hemagglutination inhibition antibody for Japanese encephalitis virus in Koreans, 1979. Korean Journal of Virology. 1980;10:65–9.
- Lee YT, Lee CH. The distribution of hemagglutination inhibition antibody for Japanese encephalitis virus in Koreans, 1976. Journal of Korean Society of Microbiology. 1977;10:65–9.
- Kim KH, Shin HK, Ree HI. Survey for the prediction of the occurrence of Japanese encephalitis epidemic in Korea, 1978. Journal of the Korean Society of Virology. 1978;8:37–43.
- Kim KH, Paik SB, Chang KS. Epidemiology of Japanese encephalitis in the Republic of Korea, 1967. Annual Report of National Institute of Health, Korea 1967;1:55-72.
- Kim KH, Paik SB. Studies on the preparation of JE vaccine with mouse brain. Annual Report of National Institute of Health, Korea 1968;1:31-6.
- Kim KH. Japanese encephalitis vaccination. Journal of Korean Medical Association. 1982;25:812–7.
- Kim KH. Japanese encephalitis vaccine and its efficacy. Postgraduate Medical Digest. 1979;7:148–55.
- Sohn YM, Lee DH, Choi KW, Sohn KC, Lee JB, Sshin HK, Cluster of adverse events after Japanese encephalitis vaccination in Korea. In: Program and Abstract of the 1994 Annual Meeting of Korean Society of Infectious Disease; Seoul, Korea; 1994 Nov 25 [abstract 14]. Korean Journal of Infectious Disease. 1994;26:449.
- Sohn YM, Pyen BY, Hong YJ, Kang JW, Lee WJ, Oh SH, Antibody response to Japanese encephalitis virus after immunization. Journal of Korean Pediatrics. 1995;38:730–1.
- Sohn YM. Standards for immunization practices and vaccine injury compensation. Korean Journal of Infectious Disease. 1995;27:247–53.
- Sohn YM, Choi BY, Kim CW, Kang JH, Kim JA, Evaluation for the improvement of efficiency of immunization program in Korea; Japanese encephalitis. Report of Evaluation of National Vaccination Program. Washigton: National Institute of Health; 1999, p. 205-6.
- Tsai TF, Chan GJ, Yu YX. Japanese encephalitis vaccines. In: Plotkin SE, Orenstein E, editors. Vaccines. 3rd ed. Philadeplhia: W.B. Saunders Company; 1999. p. 672-710.
- Sohn YM, Park MS, Rho HO, Chandler LJ, Shope RE, Primary and booster immune response to SA14-14-2 Japanese encephalitis vaccine in Korean infants. Vaccine. 1999;17:2259–64. DOIPubMedGoogle Scholar
Figures
Tables
Cite This ArticleTable of Contents – Volume 6, Number 1—February 2000
| EID Search Options |
|---|
|
|
|
|
|
|




Please use the form below to submit correspondence to the authors or contact them at the following address:
Young Mo Sohn, Department of Pediatrics, Yongdong Severnace Hospital, Yonsei University College of Medicine, Youngdong P.O. Box 1217, Seoul, 135-270 South Korea; fax: 82-2-3461-9473
Top