Volume 13, Number 10—October 2007
THEME ISSUE
Global Poverty and Human Development
Research
Cost-effectiveness of Algorithms for Confirmation Test of Human African Trypanosomiasis
Cite This Article
Citation for Media
Abstract
The control of Trypanosoma brucei gambiense human African trypanosomiasis (HAT) is compromised by low sensitivity of the routinely used parasitologic confirmation tests. More sensitive alternatives, such as mini-anion exchange centrifugation technique (mAECT) or capillary tube centrifugation (CTC), are more expensive. We used formal decision analysis to assess the cost-effectiveness of alternative HAT confirmation algorithms in terms of cost per life saved. The effectiveness of the standard method, a combination of lymph node puncture (LNP), fresh blood examination (FBE), and thick blood film (TBF), was 36.8%; the LNP-FBE-CTC-mAECT sequence reached almost 80%. The cost per person examined ranged from €1.56 for LNP-FBE-TBF to €2.99 for LNP-TBF-CTC-mAECT-CATT (card agglutination test for trypanosomiasis) titration. LNP-TBF-CTC-mAECT was the most cost-effective in terms of cost per life saved. HAT confirmation algorithms that incorporate concentration techniques are more effective and efficient than the algorithms that are currently and routinely used by several T.b. gambiense control programs.
Human African trypanosomiasis (HAT) is a parasitic disease that affects 36 countries in sub-Saharan Africa. The most recent World Health Organization (WHO) prevalence estimates are 50,000–70,000 cases worldwide, based on a total number of 17,500 new HAT cases per year worldwide (1). Trypanosoma brucei gambiense HAT control activities are based principally on the active detection of cases by population screening and subsequent treatment of infected patients. Because of the relative toxicity of HAT drugs, a correct diagnosis is essential before the treatment can begin (2).
The specificity of the card agglutination test for trypanosomiasis (CATT) used in screening is not 100% accurate, so HAT control programs use a variable sequence of parasitologic tests as confirmation tests. In the Democratic Republic of Congo (DRC), this sequence, called the standard algorithm, comprises lymph node puncture (LNP), followed by fresh blood examination (FBE) and thick blood film (TBF). Several authors have reported on the low sensitivity levels of HAT confirmation tests (3,4). Paquet et al. reported that mobile HAT screening teams in Uganda detected only 39% of all HAT cases (5). HAT cases missed by population screening will later be diagnosed by fixed health services operating in the same areas as the mobile teams, but almost invariably not until the late stages of the disease. HAT confirmation is more straightforward (6). Late-stage detection is problematic because it carries a much poorer prognosis for the patient and forgoes the principal public health objective of HAT control, which is a rapid reduction in transmission. \Technical solutions to increase the sensitivity of screening algorithms do exist. Several concentration tests have been proposed, notably the mini-anion exchange centrifugation technique (mAECT) (7), capillary tube centrifugation (CTC) (8), and the quantitative buffy coat (QBC) (9). A recent study of 436 case-patients conducted in Kwamouth, DRC, showed that 154 had parasitologic-confirmed HAT cases. Although good sensitivity was reported, and mAECT and CTC were relatively simple to implement, it is not economically feasible to use these innovative tools in the field.
Other authors have proposed recourse to serology using higher cut-offs of the CATT test to increase specificity (referred to as CATT titration, in contrast with CATT whole blood, which is the test used in the first screening step) as part of the algorithm for use in screening, or as a test to decide whether to treat. The present study is an analysis of the cost-effectiveness and value for HAT control policy of different HAT confirmation algorithms, including serologic algorithms.
A decision-analysis model was used to estimate the effectiveness and cost-effectiveness of a number of HAT screening-treatment algorithms; different HAT confirmation test sequences were compared, including concentration techniques and CATT titration. Decision analysis is a method that quantifies the value of several alternative options in a complex choice. This technique requires the construction of a decision tree, which shows detailed options, estimation of the node probabilities, and an evaluation of the economic or public health consequences of each option (John M, unpub. data) (10,11). A health service perspective was taken for this analysis, which includes all screening and treatment costs generated by the choice of HAT test algorithms.
Decision Tree
Fourteen HAT control experts were asked to identify all relevant test sequences that would confirm HAT in a given person (i.e., positive in the initial screening test, CATT). The availability of these tests was an important factor in the expert poll. At the time of this study, QBC was no longer manufactured, and for this reason, it was not included in our analysis. We analyzed 7 algorithms as shown in Table 1. All algorithms imply that only parasitologic positives will be put on stage-dependent treatment except for the fourth group (serologic algorithm), which implies stage-dependent treatment of persons who are negative for parasites but positive by CATT titration.
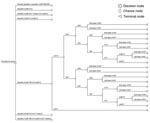
We constructed a decision tree comparing the algorithms mentioned above (Figure 1); the entry point is a person who participates in HAT population screening conducted by a mobile team. There are 4 possible outcomes for such a person: a true HAT case-patient is treated, a true HAT case-patient remains untreated, a non-HAT case-patient receives HAT treatment, or a non-HAT case-patient remains untreated. These 4 outcomes were evaluated in terms of lives saved.
Probabilities
Table 2 shows the probabilities used in this decision analysis. The baseline values were generated in a study carried out in Kwamouth between February and May 2004 (4) or were retrieved from the literature. In the baseline scenario, we assumed HAT prevalence in the community to be 1%. This value is a limit used by HAT-control programs to distinguish between severe and nonsevere HAT foci. A literature search was performed by using the Medline database to find information reported between 1950 and 2005 to identify baseline values of parameters with a plausible range. A sensitivity analysis was performed to test consistency of our conclusions over the range of plausible values.
Effectiveness
The effectiveness of each HAT screening-treatment algorithm was estimated, taking into account all steps, including screening, confirmation, and treatment. The results were quantified in terms of the number of lives saved (confirmed case, treated, and cured) by each algorithm. HAT treatment decision depends on disease staging (12). A diagnostic algorithm can theoretically generate 4 different outcomes: true positive, false positive, true negative, and false negative.
Effectiveness values were assigned to each of the alternatives. A true HAT case-patient who is treated is equal to 0.9 lives saved because the efficacy of HAT treatment is estimated at 90%, according to data from the Programme National de Lutte contre la Trypanosomiase Humaine Africaine (PNLTHA) between 1996 and 2002. For a few persons, treatment of non-HAT case-patients with toxic drugs will lead to iatrogenic death. Therefore, an effectiveness value was assigned to this endpoint of –0.001 lives saved for first-stage drugs and –0.020 lives saved for second-stage drugs. A non-HAT case-patient and a true HAT case-patient who was untreated were each assigned an effectiveness value of 0 lives saved. Effectiveness was expressed as the percentage of HAT deaths averted by a strategy. To obtain the actual number of lives saved by the strategy, this value must be multiplied by HAT prevalence.
Costs
While assessing the different algorithms, we distinguished between 3 steps in the process: 1) screening, 2) confirmation, and 3) treatment. Using the ingredient approach, we estimated the cost of screening by the mobile team for HAT on the basis of observations made in 2003. A detailed overview of cost items is given in Table 3. The cost of the screening step includes all equipment required to set up a mobile team: vehicles, depreciation, operating costs, and CATT reagents.
For the second step (HAT confirmation), each confirmation test was assessed in terms of resources consumed, equipment depreciation, and time taken by a mobile team to realize each test. Data on costs and time were collected during a validation study conducted in Kwamouth in 2004 (4). The time for each diagnostic test was estimated by using a stopwatch for a sample of 50 procedures, and the results were measured in terms of minutes elapsed. The cost of LNP has been estimated as €0.19, FBE at €0.21, TBF at €0.54, CTC at €0.76, and mAECT at €2.82 (4).
The third step, treatment, includes the cost of hospitalization care (fixed cost) as well as the cost of drugs and medical supplies. Preferential drug prices that are currently applicable were used in the calculations (pentamidine €1.54/vial, melarsoprol €5.3/vial), and the number of doses was 8 for pentamidine and 9 for melarsoprol. We assumed that 50% of case-patients were in stage 1 (needing pentamidine) and 50% were in stage 2 (needing melarsoprol).
Analysis
The efficiency of each algorithm was evaluated on the basis of the cost-effectiveness ratio expressed in terms of €/life saved. This ratio was obtained by dividing the cost (in €) per person examined for each algorithm by the strategy’s effectiveness (in % HAT deaths averted per person examined), multiplied by HAT prevalence.
We used the following equations:
Probability of treatment of a true-positive person was calculated per stage z (1,2) as follows:
Probability of treatment of a false-positive person was generally defined as:
However, for algorithms including CATT titration without subsequent confirmation, the probability of treatment of a false-positive person was defined as:
Finally, we calculated the incremental cost-effectiveness ratio (ICER) of saving 1 additional HAT patient by comparing each alternative algorithm to the strategy immediately above it after ranking the order of effectiveness. The ICER was calculated as:
HAT prevalence, sensitivity, and specificity of different tests were the subject of a sensitivity analysis. A series of 1-way sensitivity analyses were conducted to examine the effect of changes in those parameters over the plausible range mentioned in Table 2 on the efficiency ranking of strategies. DATA Pro 2004 software (TreeAge, Williamstown, MA, USA) was used for this analysis.
We estimated the cost of population screening for HAT conducted by a mobile team in 2003 (excluding the cost related to confirmation and treatment) at €1.17/per person examined (Table 4). The treatment cost was estimated at €51.32/person treated with pentamidine and €129.92/person treated with melarsoprol.
Table 4 shows the cost and effectiveness per person examined for the complete screening-treatment process. Furthermore, it presents the incremental cost, the incremental effectiveness, and the incremental cost-effectiveness ratio of each algorithm compared to the next least-effective. Table 4 shows that algorithm 5 is the most cost-effective algorithm (€264.02/life saved), with algorithm 4 a close second-best option (€265.98/life saved). Although the cost per person examined for the 2 algorithms does not differ substantially, algorithm 5 is slightly more efficacious, saving 79.60% of avoidable deaths versus 77.60% for algorithm 4.
The standard algorithm (algorithm 1) had an effectiveness of 36.80% with a €/person examined of €1.56 and an efficiency of €424.94/life saved. From column 7 in Table 4, the incremental cost-effectiveness ratio to save 1 additional life ranged between €76.34 and €200/life saved for the concentration technique algorithms and €2,617.65/life saved if the decision to treat was based on serologic evidence. Algorithm 6 was dominated by algorithm 5 because algorithm 6 costs more and is less effective.
The sensitivity analysis showed that our conclusion remained robust to variation over the range of uncertainty in all parameters included in the model (Figure 2). Changes in the specificity of CATT and CATT titration, cost of pentamidine, and HAT prevalence decreased the difference in the cost-effectiveness ratio with the next most efficient algorithm. Figure 3 shows the variation of the cost-effectiveness ratio in function of the prevalence.
Current observations suggest that parasitologic confirmation tests of inadequate sensitivity lead to suboptimal effectiveness of HAT active case-finding programs (4). Our analysis shows that concentration techniques, and to a lesser extent, serologic tests can substantially improve the efficiency of HAT confirmation algorithms. The currently used algorithm (standard algorithm) was the least cost-effective of all those compared, mainly because its sensitivity is so low. Low effectiveness of the standard algorithm was also reported by Paquet et al. (5), Pépin et al. (6), and recently by Robays et al. (13) who put it respectively at 39.5%, 20–30%, and 50%. The greater effectiveness of concentration techniques (currently €2.82/test for mAECT) more than compensates for the higher cost. Serologic algorithms were not more cost-effective than the algorithms that included concentration techniques, but the difference in efficiency decreased at a higher prevalence (Figure 3). Algorithms combining CATT titration with subsequent confirmation by concentration techniques were not competitive in this analysis; efficiency always remained lower than that of algorithms based exclusively on concentration techniques. This is due to the loss of patients caused by the suboptimal sensitivity of CATT titration.
Our study could shed some light on the controversial issue of treating for HAT on the basis of serologic evidence. In a similar discussion in the field of kala-azar case management, Boelaert et al. (14) argued that a serologic algorithm was more cost-effective, and therefore a better choice, than a parasitologic algorithm with poor sensitivity.
In this study, we also find that treating patients suspected by serologic tests to have HAT is a better option than using the current algorithm without concentration techniques. This may be a valuable strategy when introduction of mAECT or CTC is not yet feasible. A limitation of the study is that the specificity values of CATT and CATT dilution are based on data from 1 region and might be underestimated given findings from routine data from the national program (4). However, this regional variation remains poorly documented, and better estimations of the specificity of CATT in different regions are needed. The use of CATT titration has primarily been evaluated in the group of CATT whole blood–positive persons who were negative for parasites. Chappuis et al. (15), Simarro et al. (16), Van Nieuwenhove and Declercq (17), Frézil et al. (18), and Bruneel et al. (19) evaluated the strategy of treating persons who had positive serologic test results (indirect immunofluorescent antibody test or CATT) and who were negative for parasites and found this strategy more effective than that based on parasitologic confirmation.
Our model did not give different weights to iatrogenic deaths of noninfected persons compared with infected persons. This point should be carefully considered because the serologic algorithm will expose some noninfected persons to toxic drugs. However, as no treatment with second-stage HAT drugs will be given unless a lumbar puncture and parasitologic confirmation in cerebrospinal fluid are obtained, the exposure of noninfected persons to the highly toxic second-stage HAT drugs will be minimal, even under a serologic algorithm.
Our decision analysis is based on a model that depends on certain assumptions made for the purpose of simplification. An important assumption is that a true HAT case missed by the mobile teams will eventually die; in practice, if treatment is sought, this patient’s condition might be diagnosed and cured, or alternatively, HAT could be detected later by the mobile team on a second visit. We examined whether this assumption would change our conclusions by hypothesizing that 40% of such HAT case-patients would be detected and treated at a later stage. In this scenario, the differences between algorithms in terms of cost-effectiveness are reduced without altering the relative order (data not shown).
Second, confirmation tests in the sequence were used as if they were independent, but in reality, this is unlikely. For example, mAECT sensitivity could be different in a group of TBF-positive persons compared to a group of TBF-negative persons. We have examined the effect of this conditional relationship on the findings of our study by means of sensitivity analysis (data not shown). Once again, these variations did not affect the ranking of the results.
The cost of the mobile team per person screened was estimated on the basis of 40,000 examinations per year (20). Even if the program could screen 60,000 persons per mobile team per year, it would not change the rank order of efficiency. Finally, better confirmation algorithms for HAT may also have a beneficial effect on transmission because there will be fewer undetected cases to spread the disease in the community. If such an effect is considered, it might favor the efficiency of treatment based on serologic markers, which may lead to a faster reduction of the human reservoir similar to the chemoprophylaxis campaigns of the 1950s. Unfortunately, no sufficiently validated models for T. b. gambiense sleeping sickness transmission allow for the estimation of this potential benefit at population level. Our analysis disregarded this potential future benefit.
A policy change in HAT population screening seems definitely needed, and there is ample scope for improving the sensitivity of the confirmation stage. Introducing algorithm 5 has an incremental cost-effectiveness ratio of €200.00/(additional) life saved. This ratio represents the cost to HAT control programs of shifting to algorithm 5 (the most cost-effective) to save an additional life. This choice seems very rational. The incremental cost-effectiveness ratio was €76.34 if HAT control programs chose algorithm 4. TBF is a lengthy procedure, and dropping it from the sequence has logistic and organizational advantages. Our calculations were based on an estimate of 47 minutes of staff time required for TBF, obtained in a previous study (4). However, because labor costs are so low in the DRC and TBF does not require expensive reagents or equipment, it remains a very affordable test, whenever there are no time constraints for staff.
In conclusion, the standard HAT screening algorithm has low sensitivity and is inefficient. Inclusion of concentration techniques in HAT screening algorithms can be recommended as cost-effective alternatives. The use of serologic algorithms should be studied further before being recommended for HAT population screening.
Dr Lutumba is head of the research unit of the national sleeping sickness control program of the Democratic Republic of Congo. He has extensive experience in sleeping sickness control in the DRC and participates in clinical research programs on diagnosis and treatment of HAT.
Acknowledgment
We offer thanks to all HAT experts who have contributed to this study.
References
- World Health Organization. Human African trypanosomiasis (sleeping sickness): epidemiological update. Wkly Epidemiol Rec. 2006;81:69–80.PubMedGoogle Scholar
- Blum J, Nkunku S, Burri C. Clinical description of encephalopathic syndromes and risk factors for their occurrence and outcome during melarsoprol treatment of human African trypanosomiasis. Trop Med Int Health. 2001;6:390–400. DOIPubMedGoogle Scholar
- Miezan TW, Meda AH, Doua F, Cattand P. Evaluation of the parasitologic technics used in the diagnosis of human Trypanosoma gambiense trypanosomiasis in the Ivory Coast. Bull Soc Pathol Exot Filiales. 1994;87:101–4.
- Lutumba P, Robays J, Miaka C, Kande V, Simarro PP, Shaw AP, The efficiency of different detection strategies of human African trypanosomiasis by T.b. gambiense. Trop Med Int Health. 2005;10:347–56. DOIPubMedGoogle Scholar
- Paquet C, Castilla J, Mbulamberi D, Beaulieu MF, Gastellu Etchegorry MG, Moren A. Trypanosomiasis from Trypanosoma brucei gambiense in the center of north-west Uganda: evaluation of 5 years of control (1987–1991). Bull Soc Pathol Exot. 1995;88:38–41.PubMedGoogle Scholar
- Pépin J, Guern C, Mercier P, Moore A. Utilisation du Testryp CATT pour le dépistage de la trypanosomiase à Nioki, Zaïre. Ann Soc Belg Med Trop. 1986;66:213–24.PubMedGoogle Scholar
- Lumsden WHR, Kimber CD, Evans DA, Doig SJ. Trypanosoma brucei: miniature anion-exchange centrifugation technique for detection of low parasitaemias: adaptation for field use. Trans R Soc Trop Med Hyg. 1979;73:312–7. DOIPubMedGoogle Scholar
- Woo PTK, Kauffmann M. The haematocrit centrifuge technique for the detection of low virulent strains of trypanosomes of the Trypanosoma congolense sub-group. Acta Trop. 1971;28:304–8.PubMedGoogle Scholar
- Bailey JW, Smith DH. The quantitative buffy coat for the diagnosis of trypanosomes. Trop Doct. 1994;24:54–6.PubMedGoogle Scholar
- Weinstein MC, Fineberg HV. Clinical decision analysis. Philadelphia: WB Saunders; 1980. p. 1–351.
- Drummond MF, O'Brien BJ, Stoddart GL, Torrance GW. Methods for the economic evaluation of health care programs, 2nd ed. Oxford: Oxford University Press; 1997. p. 305.
- Stich A, Abel PM, Krishna S. Human African trypanosomiasis. BMJ. 2002;325:203–6. DOIPubMedGoogle Scholar
- Robays J, Bilengue MM, Van der Stuyft P, Boelaert M. The effectiveness of active population screening and treatment for sleeping sickness control in the Democratic Republic of Congo. Trop Med Int Health. 2004;9:542–50. DOIPubMedGoogle Scholar
- Boelaert M, Lynen L, Desjeux P, Van der Stuyft P. Cost-effectiveness of competing diagnostic-therapeutic strategies for visceral leishmaniasis. Bull World Health Organ. 1999;77:667–74.PubMedGoogle Scholar
- Chappuis F, Stivanello E, Adams K, Kidane S, Pittet A, Bouvier P. Card agglutination test for trypanosomiasis (CATT) end-dilution titer and cerebrospinal fluid cell count as predictors of human African Trypanosomiasis (Trypanosoma brucei gambiense) among serologically suspected individuals in southern Sudan. Am J Trop Med Hyg. 2004;71:313–7.PubMedGoogle Scholar
- Simarro PP, Ruiz JA, Franco JR, Josenando T. Attitude towards CATT-positive individuals without parasitological confirmation in the African Trypanosomiasis (T.b. gambiense) focus of Quicama (Angola). Trop Med Int Health. 1999;4:858–61. DOIPubMedGoogle Scholar
- Van Nieuwenhove S, Declercq J. Mass serodiagnosis and treatment of serological positives as a control strategy in Trypanosoma gambiensis. In: Crooy PG, editor. Symposium on the diagnosis of African Sleeping Sickness due to T. gambiense. Rixensart: Smith Kline-RIT; 1984. p. 71–5.
- Frézil JL, Coulm J, Alary JC. Post-therapeutic evolution of patients presenting an immunological suspicion of trypanosomiasis without parasitological proof. Med Trop (Mars). 1979;39:53–6.PubMedGoogle Scholar
- Bruneel H, Van den Eeckhout A, Molisho D, Burke J, Degroof D, Pépin J. Control of Trypanosoma Gambiense trypanosomiasis. Evaluation of a strategy based on the treatment of serologically suspected cases with a single dose of diminazene. Ann Soc Belg Med Trop. 1994;74:203–15.PubMedGoogle Scholar
- Lutumba P, Robays J, Miaka C, Mesu VK, Molisho D, Declercq J, Trypanosomiasis control, Democratic Republic of Congo, 1993–2003. Emerg Infect Dis. 2005;11:1382–8.PubMedGoogle Scholar
- Noireau F, Gouteux JP, Duteurtre JP. Diagnostic value of a card agglutination test (Testryp CATT) in the mass screening of human trypanosomiasis in the Congo. Bull Soc Pathol Exot Filiales. 1987;80:797–803.PubMedGoogle Scholar
- Noireau F, Lemesre JL, Nzoukoudi MY, Louembet MT, Gouteux JP, Frezil JL. Serodiagnosis of sleeping sickness in the Republic of the Congo: comparison of indirect immunofluorescent antibody test and card agglutination test. Trans R Soc Trop Med Hyg. 1988;82:237–40. DOIPubMedGoogle Scholar
- Magnus E, Lejon V, Bayon D, Buyse D, Simarro P, Verloo D, Evaluation of EDTA version of CATT/Trypanosoma brucei gambiense for serological screening of human blood samples. Acta Trop. 2002;81:7–12. DOIPubMedGoogle Scholar
- World Health Organization Expert Committee. Control and surveillance of African trypanosomiasis. Report No. 881. Geneva: The Organization; 1998.
- Doua F, Boa FY. Human trypanosomiasis in the Ivory Coast: therapy and problems. Acta Trop. 1993;54:163–8. DOIPubMedGoogle Scholar
- Legros D, Evans S, Maiso F, Enyaru JC, Mbulamberi D. Risk factors for treatment failure after melarsoprol for Trypanosoma brucei gambiense trypanosomiasis in Uganda. Trans R Soc Trop Med Hyg. 1999;93:439–42. DOIPubMedGoogle Scholar
- Pépin J, Milord F, Khonde A, Niyonsenga T, Loko L, Mpia B. Gambiense trypanosomiasis: frequency of, and risk factors for, failure of melarsoprol therapy. Trans R Soc Trop Med Hyg. 1994;88:447–52. DOIPubMedGoogle Scholar
Figures
Tables
Cite This ArticleTable of Contents – Volume 13, Number 10—October 2007
| EID Search Options |
|---|
|
|
|
|
|
|


Please use the form below to submit correspondence to the authors or contact them at the following address:
Marleen Boelaert, Institute of Tropical Medicine, Nationalestraat 155, 2000, Antwerp, Belgium;
Top