Volume 18, Number 2—February 2012
Letter
Hand, Foot, and Mouth Disease Caused by Coxsackievirus A6, Japan, 2011
Cite This Article
Citation for Media
To the Editor: Coxsackievirus A6 (CVA6) belongs to human enterovirus species A of the genus Enterovirus. According to a Japanese Infectious Agents Surveillance Report, this virus is one of the major causes of herpangina, an acute febrile disease characterized by vesicles, ulcers, and redness around the uvula, which occurs mainly in young children and infants (1).
In June 2011, a sudden increase in cases of hand, foot, and mouth disease (HFMD) at pediatric sentinel sites (≈3,000 pediatric hospitals and clinics) was reported to the National Epidemiologic Surveillance of Infectious Diseases System in Japan. Compared with past numbers of cases over 30 years of surveillance, the number of cases of HFMD per sentinel site peaked in week 28 (July) of 2011 (10.97 cases per sentinel), particularly in western Japan (2). According to the Infectious Agents Surveillance Report (as of September, 18, 2011), CVA6 was detected in 709 HFMD cases and 156 herpangina cases throughout Japan (1).
Clinical samples (throat swab specimens and feces) obtained from sentinel sites in Shimane, Hyogo, Hiroshima, and Shizuoka, Japan, were screened for enteroviruses by using an enterovirus-specific reverse transcription PCR and sequence analysis of the partial viral protein (VP)4/VP2 or VP1 region (3). Among 93 clinical samples from 108 HFMD case-patients, we identified 74 case-patients as CVA6 positive by sequence analysis.
On the basis of sequence analysis of the entire VP1 region (GenBank accession nos. AB649286–AB649291), the consensus sequence had 82.3%–82.5% nt identity (94.8%–95.4% aa identity) with the prototype CVA6 Gdula strain (GenBank accession no. AY421764). CVA6 was not isolated from clinical samples in a cell culture system. Therefore, most CVA6 strains were identified by molecular detection directly from clinical samples and sequence analysis. Some CVA6 strains were grown and isolated in suckling mice; these strains were antigenically identified as CVA6 by a neutralization test with specific antiserum against CVA6 (4).
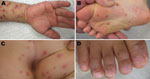
In Japan, HFMD and herpangina are classified as category V infectious diseases. On the basis of clinical diagnosis, suspected infections were reported by pediatric sentinel sites on a weekly basis to the Infectious Disease Surveillance Center of the National Institute of Infectious Diseases (Tokyo, Japan). Typical clinical signs and symptoms of HFMD cases caused by CVA6 were fever, mild vesicles in oral mucosa, and skin blisters on hands, arms, feet, legs, buttocks, and nail matrixes (Figure). Some patients with HFMD had onychomadesis (periodic shedding of the nails) 1–2 months after onset of HFMD. Most cases of HFMD were self-limited. However, additional follow-up may be necessary for patients with onychomadesis who are treated at dermatology clinics.
As in other countries in the Asia–Pacific region, major causes of HFMD in Japan were CVA16 and enterovirus 71. In 2010, enterovirus 71 was identified as a major cause of HFMD (2). In contrast, CVA6 was consistently associated with herpangina, as were CVA2, CVA4, CVA5, and CVA10, but CVA6 was occasionally detected in HFMD case-patients. CVA6 was the major cause of herpangina in 2007, but an increase in the detection rate of CVA6 in HFMD case-patients was reported in Japan in 2009 (2).
HFMD outbreaks caused by CVA6 were reported in Singapore, Finland, and Taiwan in 2007–2009 (5–8). Recent HFMD outbreaks in Finland and Spain were associated with cases of onychomadesis 1–2 months after onset of HFMD (6,8,9). In Japan, cases of onychomadesis after onset of HFMD were reported in 2009 (10). Therefore, changes in clinical outcomes of CVA6-associated diseases should be investigated.
Although most HFMD cases caused by CVA6 in Japan were mild, CVA6 was also detected in other clinical samples, including cerebrospinal fluid from a patient with acute encephalitis in Hiroshima, which reaffirmed possible additional clinical manifestations during an HFMD outbreak caused by CVA6. Careful surveillance of disease and infectious agent activities are crucial in monitoring CVA6-associated HFMD, onychomadesis, and neurologic diseases. Nucleotide identity between CVA6 strains in Finland (2008) (7) and Japan (2011) was ≈95% in the partial VP1 region. More detailed genetic, phenotypic, and epidemiologic analyses of CVA6 are needed to determine the role of CVA6 in HFMD outbreaks with or without onychomadesis.
Acknowledgments
We thank the staff of prefectural and municipal public health institutes in Japan for virus detection, identification and molecular analysis, and Grant Hansman for critical review of the manuscript.
This study was supported in part by grants-in-aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan, and for research on emerging and re-emerging infectious diseases from the Ministry of Health, Labour and Welfare, Japan.
References
- Infectious Disease Surveillance Center. Virus isolation/detection from hand, foot and mouth disease cases, 2007–2011. Infectious Agents Surveillance Report [cited 2011 Nov 7]. http://hasseidoko.mhlw.go.jp/Byogentai/Pdf/data37e.pdf
- Infectious Disease Surveillance Center. Infectious Disease Weekly Report, Hand-foot-mouth disease cases reported per sentinel weekly [cited 2011 Nov 7]. http://idsc.nih.go.jp/idwr/kanja/weeklygraph/06HFMD-e.html
- Perera D, Shimizu H, Yoshida H, Tu PV, Ishiko H, McMinn PC, A comparison of the VP1, VP2, and VP4 regions for molecular typing of human enteroviruses. J Med Virol. 2010;82:649–57.PubMedGoogle Scholar
- Konno M, Yoshioka M, Sugie M, Maguchi T, Nakamura T, Kizawa M, Fourteen years’ surveillance of coxsackievirus group A in Kyoto 1996‒2009 using mouse, RD-18S, and Vero cells. Jpn J Infect Dis. 2011;64:167–8.PubMedGoogle Scholar
- Wu Y, Yeo A, Phoon MC, Tan EL, Poh CL, Quak SH, The largest outbreak of hand; foot and mouth disease in Singapore in 2008: the role of enterovirus 71 and coxsackievirus A strains. Int J Infect Dis. 2010;14:e1076–81.PubMedGoogle Scholar
- Österback R, Vuorinen T, Linna M, Susi P, Hyypia T. Waris M. Coxsackievirus A6 and hand, foot, and mouth disease, Finland. Emerg Infect Dis. 2009;15:1485–8.PubMedGoogle Scholar
- Lo SH, Huang YC, Huang CG, Tsao KC, Li WC, Hsieh YC, Clinical and epidemiologic features of coxsackievirus A6 infection in children in northern Taiwan between 2004 and 2009. J Microbiol Immunol Infect. 2011;44:252–7.PubMedGoogle Scholar
- Blomqvist S, Klemola P, Kaijalainen S, Paananen A, Simonen ML, Vuorinen T, Co-circulation of coxsackieviruses A6 and A10 in hand, foot and mouth disease outbreak in Finland. J Clin Virol. 2010;48:49–54.PubMedGoogle Scholar
- Guimbao J, Rodrigo P, Alberto MJ, Omenaca M. Onychomadesis outbreak linked to hand, foot, and mouth disease, Spain, July 2008. Euro Surveill. 2010;15:19663.PubMedGoogle Scholar
- Watanabe Y, Nanba C, Tohyama M, Machino H, Hashimoto K. Outbreak of nail matrix arrest following hand-foot-mouth disease [in Japanese]. Japanese Journal of Dermatology. 2011;121:863–7.
Figure
Cite This ArticleRelated Links
Table of Contents – Volume 18, Number 2—February 2012
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Hiroyuki Shimizu, Department of Virology II, National Institute of Infectious Diseases, Gakuen 4-7-1, Musashimurayama-shi, Tokyo 208-0011, Japan
Top