Volume 18, Number 3—March 2012
Research
Using Genotyping and Geospatial Scanning to Estimate Recent Mycobacterium tuberculosis Transmission, United States
Cite This Article
Citation for Media
Abstract
To determine the proportion of reported tuberculosis (TB) cases due to recent transmission in the United States, we conducted a cross-sectional study to examine culture-positive TB cases with complete genotype results (spoligotyping and 12-locus mycobacterial interspersed repetitive unit–variable-number tandem repeat typing) reported during January 2005–December 2009. Recently transmitted cases were defined as cases with matching results reported within statistically significant geospatial zones (identified by a spatial span statistic within a sliding 3-year window). Approximately 1 in 4 TB cases reported in the United States may be attributed to recent transmission. Groups at greatest risk for recent transmission appear to be men, persons born in the United States, members of a minority race or ethnic group, persons who abuse substances, and the homeless. Understanding transmission dynamics and establishing strategies for rapidly detecting recent transmission among these populations are essential for TB elimination in the United States.
Molecular characterization of Mycobacterium tuberculosis complex has been available for >2 decades in the United States. As a tool to enhance programmatic activities, tuberculosis (TB) genotyping is a useful adjunct to epidemiologic field investigations by defining outbreaks (1,2), discerning episodes of reactivation and relapse (3,4), confirming suspected laboratory contamination (5,6), and evaluating and monitoring TB control program performance (7). TB genotyping results, when combined with epidemiologic data, help identify persons with TB disease who are involved in the same chain of recent transmission (8). Previous analytic studies have used TB genotyping data in conjunction with epidemiologic data to assess correlates of recent TB transmission within localized populations (9–15). A basic assumption of this approach is that recent TB transmission is localized in place and time, that is, progression to TB disease from an infection acquired within the past few years and in the same jurisdiction.
Population-based molecular epidemiologic studies are often subject to several biases and methodologic limitations that impede the ability of investigators to make valid statements about recent TB transmission events in the absence of direct data regarding interpersonal contacts (16). Estimating recent TB transmission is often limited by abbreviated study periods, convenience isolate sampling, and ambiguous geographic boundaries defined for jurisdictional or geopolitical reasons (17,18). TB transmission is not likely to be bound by these artifacts, however. Spatial scanning to detect disease clusters has been successfully applied in multiple settings and for various diseases (19). Using this method in a multiyear, nationally representative database of both genotype and routinely collected TB surveillance data may offer a better solution for accurately defining recent TB transmission.
In 2004, the US Centers for Disease Control and Prevention (CDC) offered universal access to TB genotyping through the National Tuberculosis Genotyping Service (NTGS) to routinely characterize at least 1 M. tuberculosis complex isolate from every TB case-patient in the United States (20). Although the intent of this system is to support local TB programs for public health action, data collected from this system offer a unique opportunity to explore and describe the molecular epidemiology of TB and establish comprehensive molecular TB surveillance in the United States. In this analysis, our goals were to estimate the proportion of TB in the United States attributable to recent transmission and to assess clinical, demographic, and epidemiologic factors associated with recent TB transmission.
Study Population
This study includes verified cases of TB reported to the US National Tuberculosis Surveillance System (NTSS) by the 50 states and the District of Columbia. Clinical, demographic, and epidemiologic variables for each case-patient are collected for surveillance purposes and are described elsewhere (21). M. tuberculosis complex isolates were characterized by using a standardized protocol for spacer oligonucleotide typing (spoligotyping) and 12-locus mycobacterial interspersed repetitive unit–variable-number tandem repeats (MIRU-VNTRs) (22). NTGS results for each submitted isolate were linked to NTSS case records by state and local TB control programs; a standardized case identification number and a unique laboratory accession number were used to form discrete individual isolate-case records (20). When multiple isolates were genotyped for the same person in the same surveillance year, case-patients with discordant genotyping results were excluded from analysis for clustering assignment and risk factor analysis. The final study population included all persons with verified culture-positive TB cases reported during January 2005–December 2009 with a complete spoligotype and 12-locus MIRU-VNTR result.
Four major phylogenetic lineages for M. tuberculosis, along with speciation of M. africanum and M. bovis, were identified by using spoligotyping motifs that referred to an international standard (23). Substance abuse was defined by using previously published methods (24). Persons with TB who received a positive HIV test result at the time of TB diagnosis were classified as TB/HIV case-patients. Persons with TB and negative HIV results or unknown HIV status were classified as having non-HIV TB.
Genotype and Geospatial Clustering
Genotype clusters were defined as cases with matching spoligotype and 12-locus MIRU-VNTR results (i.e., exact match on all loci) reported within statistically significant geospatial zones determined by a spatial scan statistic (25). SaTScan version 9.1.0 (26) was employed to identify geographic areas with a larger-than-expected rate of discrete genotype clustering, and all other culture-positive TB cases counted during the study were considered as the background rate. In brief, all cases were aggregated by genotype according to residential ZIP code where they were reported. Each genotype was then scanned separately, applying a purely spatial analysis, in which the number of events in an area was assumed to be Poisson-distributed to generate circular zones of various sizes up to a maximum radius of 50 km. An evaluation of outbreak investigations conducted by CDC demonstrated no difference in cluster membership when 50-km and 100-km SaTScan search radii were used to identify known epidemiologically linked genotype cases (CDC, unpub. data).
A log-likelihood ratio was calculated for each zone in comparison with all possible zones, with the maximum likelihood ratio representing the zone most likely to identify spatial clustering for each genotype. A Monte Carlo simulation with 999 repetitions was used to determine the distribution of the scan statistic under the null hypothesis of spatial randomness; significant spatial clusters were chosen at an α of p<0.05. Three scans comprised of 3-year overlapping intervals (scan A, 2005–2007; scan B, 2006–2008; scan C, 2007–2009) were performed to identify spatial clusters occurring within a 3-year period. If cases were identified as a member of a statistically significant spatial cluster in any of the 3 periods, they were considered clustered. No duplicative case counting occurred. The purpose of this spatial scan was to characterize each case for a dichotomous outcome: clustered or not clustered. Cases that were both genotypically and spatially clustered were considered recent TB transmission for the purposes of this study. All cases that were not genotypically and spatially clustered were considered reactivation of remotely acquired TB infection, or reactivation TB. For comparative purposes, national-, state- and county-level clustering definitions were created. National-level clustering was defined as >2 culture-positive cases with identical genotypes reported anywhere in the United States during 2005–2009. State-level clustering was defined as >2 culture-positive cases with identical genotypes reported from the same state during 2005–2009. County-level clustering was defined as >2 culture-positive cases with identical genotypes reported from same county during 2005–2009.
Statistical Analyses
A predictive logistic regression model was used to determine potential associations between clinical (e.g., sputum-smear status, known HIV positivity, site of disease and cavitation on chest radiograph, and previous TB diagnosis) and demographic and risk characteristic variables (e.g., race/ethnicity, age, country of birth, homelessness, substance abuse, incarceration at time of diagnosis, and residence at long-term care facility at diagnosis) and the outcome of interest: geospatial and genotype clustering as a proxy for recent TB transmission. Univariate analysis of the categorical independent variables was done by using Pearson χ2. Any variable with a significance value of <0.20 was included in a best subset, multivariate logistic regression model. We built our final model using backward elimination of nonsignificant independent variables (p>0.01). The log-likelihood ratio was used to assess the overall significance of the final models, and the Hosmer-Lemeshow statistic was used to evaluate the fit of each of the final models. To test the hypothesis that factors associated with recent TB transmission events varied by geographic region of the United States, an additional 4 independent models were created following the same process but subset to western, midwestern, northeastern, and southern states, respectively (27).
TB Case Population
During 2005–2009, a total 65,529 verified cases of TB were reported to CDC. Of these, 51,015 (77.9%) were culture-positive (Figure 1). During this period, the overall incidence of TB in the United States declined from 4.8 to 3.8 per 100,000 persons, representing a decline of 20.1% in the overall case count (21).
TB Isolates and Genotype Clusters
During 2005–2009, a total of 45,188 isolates were submitted to NTGS for molecular characterization; 39,474 (87.4%) were successfully matched to a case-patient with reported TB. Two hundred seventy isolates (0.7%) had incomplete results on spoligotype, MIRU-VNTR, or both; 344 case-patients (0.9%) had multiple isolates with discordant genotyping results and were excluded from the analysis. The total number of genotyped TB cases available for analysis was 36,860, representing 72.3% of all reported culture-positive cases. The proportion of reported case-patients for whom complete genotype results were available increased over time, with 6,863 (62.7%) of 10,953 in 2005 and 7,845 (88.4%) of 8,876 in 2009. The number of individual genotype strains (i.e., distinct spoligotype and 12-locus MIRU-VNTR combinations) identified over the study period was 11,722. The proportion of new strains identified per year gradually decreased over time. In 2006, 40.7% of strains identified were new; this percentage was reduced to 14.2% in 2009 (data not shown).
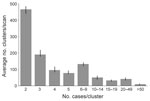
Of the 36,860 cases for which genotyping had been performed, 8,499 (23.1%) were considered clustered by both genotype and spatial concentration and therefore were thought to be members of a putative recent TB transmission event. The average number of spatially concentrated genotype clusters identified per 3-year scanning period was 1,039 (range 970–1,128). Nationally, the overall mean cluster size was 5.7 members (range 2–173 members) (Figure 2). The median cluster size was 3 members, and almost half (46.1%) of the clusters had only 2 members. Other clustering definitions that use geopolitical boundaries had higher average clustering percentages when the same 3-year window periods were used (national-level, 77.3%; state-level, 57.1%; county-level, 38.7%) (Figure 1).
Characteristics of Members with Putative Recent TB Transmission
Cluster members were more likely to be male (66.3% vs. 61.7%), to have been born in the United States (57.4% versus 34.4%), to abuse substances (28.4% versus 14.8%), and to have a history of homelessness (11.1% versus 5.0%) than those thought to have reactivation TB (Table 1). The proportion of cluster members also varied by race compared with those with cases due to reactivation TB: Asian, non-Hispanic (17.6% vs. 29.8%); black, non-Hispanic (39.7% versus 21.6%); Hispanic (25.5% versus 28.5%); and white, non-Hispanic (15.0% versus 17.9%).
Cluster members with recent TB transmission events were also more likely to have reported HIV-positive results (8.7% versus 5.5%), pulmonary disease exclusively (78.4% versus 72.2%), and positive sputum smear results (61.5% versus 55.3%) and to have had a cavitary chest radiograph at time of diagnosis (36.8% versus 32.2%) than those thought to have reactivation TB. Of the 8,499 persons with cases believed to be caused by recent TB transmission, only 2.1% and 4.4% resided in a long-term care or correctional facility at the time of diagnosis, respectively.
Genotype Lineage and Recent TB Transmission Events
The proportions of isolates in each phylogenetic lineage were as follows: Euro-American, 64.2%; Indo-Oceanic, 15.4%; East-Asian, 13.5%; East-African/Indian, 4.3%. M. bovis isolates accounted for 1.6% of reported cases of TB. Seventy-two percent of reported case-patients with M. bovis isolates were non–US-born. M. africanum isolates were identified among 179 patients (0.5%), with 88.6% non–US-born. Among members with recent TB transmission events, 69.2% had TB isolates with Euro-American lineage; 14.9% had isolates with East-Asian lineage, 11.8% had isolates with Indo-Oceanic lineage, 2.3% had isolates of East-African/Indian lineage, 1.5% had M. bovis isolates, and 0.3% had M. africanum isolates.
Factors Associated with Putative Recent TB Transmission Events
In our final adjusted model, the following odds ratios were noted for variables significantly associated with a higher odds of having a case attributed to putative recent TB transmission (Table 1): age (0–4 years of age: adjusted odds ratio [aOR] 3.1, 99% CI 1.4–6.8); black, non-Hispanic (aOR 2.4, 99% CI 2.2–2.7); Hispanic (aOR 1.7, 99% CI 1.5–2.0); Native Hawaiian/Pacific Islander (aOR 2.6, 99% CI 1.5–4.4); US-born (aOR 2.4, 99% CI 2.1–2.7); homeless persons (aOR 1.4, 99% CI 1.2–1.6); persons who abuse substances (aOR 1.4, 99% CI 1.3–1.7); East-Asian lineage (aOR 1.9, 99% CI 1.5–2.6); and Indo-Oceanic lineage (aOR 1.7, 99% CI 1.3–2.3).
Geographic Variation Associated with Recent TB Transmission
Best-fit models to predict those with recent TB transmission were conducted for each of the 4 US geographic regions. Many of the main effects associated with recent TB transmission remained constant (US-born, substance abuse, homeless), although factors varied in both magnitude and risk factor across the United States (Table 2).
Ethnic disparities for recent TB transmission were found among black, non-Hispanic persons living in midwestern and southern states (aOR 2.1, 99% CI 1.7–2.6; aOR 3.6, 99% CI 1.5–8.6), whereas Hispanic persons had the highest odds among those living in northeastern (aOR 2.3, 99% CI 1.7–8.8) and western states (aOR 2.1, 99% CI 1.5–3.0).
Phylogenetic lineage also varied among the different regions. Euro-American lineage (aOR 2.2, 99%,CI 1.1–4.3) had the strongest association for recent transmission in the south, whereas the East-Asian lineage was most strongly associated with recent transmission in western (aOR 2.4, 99% CI 1.4–4.2) and northeastern states (aOR 2.0, 99% CI 1.1–3.6).
According to these findings, ≈1 in 4 TB cases reported in the United States may be attributed to recent TB transmission; this increases to 1 in 3 among US-born persons (Table 1). Our approach to identifying the proportion of reported TB attributable to recent transmission is based on the concept that epidemiologically related organisms share indistinguishable genotypes, whereas unrelated organisms differ at some genetic loci (8). TB cases that occur in spatial clusters and share indistinguishable genotypes are thought to be caused by recently transmitted TB infection; those with nonclustered genotypes are thought to result from progression from an infection acquired >3 years in the past. In the absence of detailed data about interpersonal contact between persons, relying on genotype and on place and time data routinely collected during surveillance activities becomes imperative to assessing recent transmission at a national level. This goal was achieved by using the established infrastructure of NTSS and TB genotyping, universally accessible to TB programs through NTGS, to capture 72% of all cases with culture-positive results over a 5-year period.
Spatial scanning provides a new insight into TB transmission that is independent of jurisdictional or geopolitical boundaries. This nationally representative study incorporated spatial concentration as a core element for defining recent TB transmission. Previous studies were limited to clustering definitions confined to a single jurisdiction (9–11,14,15), state, or province (28,29), or incomplete sampling of an entire nation (13,30). The proportion of cases representing recent TB transmission varied considerably by cluster definitions based on geopolitical borders. If a national clustering definition was used, up to 80% of culture-positive cases would be attributed to recent TB transmission. If a state-based definition or county-based definition was used, up to 57% and 39% of culture-positive cases, respectively, would be attributed to recent TB transmission. Although which definition most accurately represents recent TB transmission is unclear, a clustering definition based on geospatial concentration appears to be the most conservative and is not subject to the potential misclassification of political boundaries. The limitation of using these boundaries can be best exemplified by known inter-jurisdictional TB outbreaks that crossed geopolitical borders (31). Because the proportion of recent TB transmission may be a reflection of the success of control measures, accurately assessing this quantity is of considerable public health importance.
Estimating recent TB transmission also depends on the duration of the study period (16). Other studies have shown increasing clustering proportions as the duration of the study increases, with a plateau effect after 3 years (12,13,17,32,33). The annual proportion of isolates with a new strain identified in the United States during this study period did plateau (data not shown), suggesting a similar phenomenon and potential influencing factor in the long-term estimation of TB genotype clustering nationwide. Using consecutive, overlapping scanning windows that incorporate 3-year intervals maximizes the probability that spatial and temporal clustering represent localized, recent TB transmission within this large and comprehensive dataset. As NTGS continues to mature and grow over time, adjusting for temporal clustering will become essential when estimating recent TB transmission.
Consistent with other published reports from countries with a low incidence of TB, the characteristics of local birth, male sex, minority race, substance abuse, and homelessness were associated with recent TB transmission (17,18,33). These findings highlight the fact that TB may be harder to eliminate among populations characterized by these factors (34). The large proportion of cases attributable to recent TB transmission among minorities, persons who abuse substances, and those who are homeless suggests that limited access to routine health screenings, resulting in delayed diagnoses, may extend infectious periods and rates of TB transmission. Indeed, TB patients who use illicit substances and abuse alcohol have been found to be more contagious (24).
In low-incidence, high-resource countries, efforts to control recent TB transmission are based largely on contact investigation, yet for many reasons, contact investigations may not be sufficiently intensive or comprehensive, even in successful TB control programs (35). Every case of TB began when a person came into contact with a person with contagious TB. Therefore, it follows that clusters of case-patients representing recent TB transmission could be averted through improved contact investigation efforts. Contact investigations are multistep processes in which exposed contacts are systematically evaluated on the basis of the amount of time spent with an infectious person, the environmental conditions of exposure venue, and the contact's intrinsic predisposition for infection or disease (36). Numerous studies have demonstrated that eliciting names of contacts is neither optimally effective nor sufficient to interrupt TB transmission among high-risk groups, such as the homeless and persons who abuse substances (1,24,37,38). The potential for uninterrupted TB transmission is further exacerbated by the poor yield of name-based contact investigations among these populations. Locations are as important as named contacts when investigating recent transmission. A recent study found that 81% of case-patients involved in a multiyear TB outbreak lived in close geographic proximity (38). Spatial scanning methods may assist with identification of specific clusters representing ongoing transmission that could benefit from targeted location-based interventions. Using spatial scanning methods to determine locations with high concentrations of both spatial and genotype clustering may be an effective way to prioritize resources to intervene in populations with high rates of TB transmission.
This study does have limitations. First, isolate submission for TB genotyping is not universal; thus, the database, although large, did not contain all reported case-patients with culture-positive TB during the study period. Clinical, demographic, and epidemiologic characteristics of patients without TB genotyping data did not differ statistically from those with TB genotyping data (data not shown). Second, spatial and genotype clustering serves only as a proxy for recent TB transmission in the absence of detailed data on interpersonal connections between case-patients. Because of dynamic migration patterns within the United States, these methods may fail to ascertain cases that are due to recent transmission when a putative source case-patient moves or if exposure occurred outside the range of spatial scanning. Increased global migration has influenced the epidemiology of TB in the United States as well. Recent immigrants who became infected with a particular genotype elsewhere may resettle in the same neighborhood and, when TB develops after resettlement, it may falsely be considered recent TB transmission. Third, although spoligotyping and 12-locus MIRU-VNTR have good discriminatory power, these methods may not provide the resolution necessary to differentiate evolutionarily close strains (39,40). The introduction of an expanded panel of 24 MIRU-VNTR loci in 2009 to NTGS may reduce this misclassification in the future (40). It is also critical to note that TB transmission dynamics are multifactorial. TB genotype clustering may overestimate transmission. Consideration of patient characteristics, transmission venues, and temporality may better clarify recent transmission.
The integration of NTGS into routine public health practice and surveillance has led to the establishment of molecular surveillance of M. tuberculosis in the United States (20). With improved access to and rapid dissemination of genotyping information, it may be possible to more effectively identify some cases of TB transmission. Yet, TB genotyping, and likely future molecular advancements do not alter real-time public health action. Rather recent transmission can only be prevented by implementing thorough contact investigation and ensuring that subsequent preventive treatment is completed among those identified at highest risk of undergoing a progression from infection to TB disease. If such practices had been successfully followed, as many as one third of all reported TB cases in US-born patients may have been prevented, especially among high-risk populations, such as persons with substance abuse disorders, those experiencing homelessness, or both. Greater attention and resources are needed to develop, implement, and evaluate interventions to control and prevent transmission among these populations. As the United States continues toward TB elimination, understanding transmission dynamics among high-risk populations and establishing new strategies for rapidly detecting and effectively responding to these transmission events will enhance the progress toward achieving this target.
Dr Moonan is a senior epidemiologist with the Division of Tuberculosis Elimination, National Center for HIV/AIDS, Viral Hepatitis, STD, and TB prevention, CDC. His primary research interests include TB transmission dynamics, molecular epidemiology of TB, and enhancing multidrug-resistant TB surveillance in high-prevalence, low-income settings.
Acknowledgment
We gratefully acknowledge the staff from the NTGS contract laboratories, local and state public health laboratories, and local and state health departments who collected data included in these analyses.
References
- Buff AM, Moonan PK, Desai MA, McKenna TL, Harris DA, Rogers BJ, South Carolina tuberculosis genotype cluster investigation: a tale of substance abuse and recurrent disease. Int J Tuberc Lung Dis. 2010;14:1347–9.PubMedGoogle Scholar
- Pevzner ES, Robison S, Donovan J, Allis D, Spitters C, Friedman R, Tuberculosis transmission and use of methamphetamines in Snohomish County, WA, 1991–2006. Am J Public Health. 2010;100:2481–6. DOIPubMedGoogle Scholar
- Burman WJ, Bliven EE, Cowan L, Bozeman L, Nahid P, Diem L, Relapse associated with active disease caused by Beijing strain of Mycobacterium tuberculosis. Emerg Infect Dis. 2009;15:1061–7. DOIPubMedGoogle Scholar
- Jasmer RM, Bozeman L, Schwartzman K, Cave MD, Saukkonen JJ, Metchock B, Recurrent tuberculosis in the United States and Canada: relapse or reinfection? Am J Respir Crit Care Med. 2004;170:1360–6. DOIPubMedGoogle Scholar
- Lai CC, Tan CK, Lin SH, Liao CH, Chou CH, Huang YT, Molecular evidence of false–positive cultures for Mycobacterium tuberculosis in a Taiwanese hospital with a high incidence of TB. Chest. 2010;137:1065–70. DOIPubMedGoogle Scholar
- Cook VJ, Stark G, Roscoe DL, Kwong A, Elwood RK. Investigation of suspected laboratory cross–contamination: interpretation of single smear–negative, positive cultures for Mycobacterium tuberculosis. Clin Microbiol Infect. 2006;12:1042–5. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Monitoring tuberculosis programs–National Tuberculosis Indicator Project, United States, 2002–2008. MMWR Morb Mortal Wkly Rep. 2010;59:295–8.PubMedGoogle Scholar
- Barnes PF, Cave MD. Molecular epidemiology of tuberculosis. N Engl J Med. 2003;349:1149–56. DOIPubMedGoogle Scholar
- Cronin WA, Golub JE, Lathan MJ, Mukasa LN, Hooper N, Razeq JH, Molecular epidemiology of tuberculosis in a low- to moderate-incidence state: are contact investigations enough? Emerg Infect Dis. 2002;8:1271–9.PubMedGoogle Scholar
- Clark CM, Driver CR, Munsiff SS, Driscoll JR, Kreiswirth BN, Zhao B, Universal genotyping in tuberculosis control program, New York City, 2001–2003. Emerg Infect Dis. 2006;12:719–24. DOIPubMedGoogle Scholar
- Serpa JA, Teeter LD, Musser JM, Graviss EA. Tuberculosis disparity between US–born blacks and whites, Houston, Texas, USA. Emerg Infect Dis. 2009;15:899–904. DOIPubMedGoogle Scholar
- Ellis BA, Crawford JT, Braden CR, McNabb SJ, Moore M, Kammerer S, Molecular epidemiology of tuberculosis in a sentinel surveillance population. Emerg Infect Dis. 2002;8:1197–209.PubMedGoogle Scholar
- van Soolingen D, Borgdorff MW, de Haas PE, Sebek MM, Veen J, Dessens M, Molecular epidemiology of tuberculosis in the Netherlands: a nationwide study from 1993 through 1997. J Infect Dis. 1999;180:726–36. DOIPubMedGoogle Scholar
- Barnes PF, Yang Z, Pogoda JM, Preston-Martin S, Jones BE, Otaya M, Foci of tuberculosis transmission in central Los Angeles. Am J Respir Crit Care Med. 1999;159:1081–6.PubMedGoogle Scholar
- Small PM, Hopewell PC, Singh SP, Paz A, Parsonnet J, Ruston DC, The epidemiology of tuberculosis in San Francisco. A population–based study using conventional and molecular methods. N Engl J Med. 1994;330:1703–9. DOIPubMedGoogle Scholar
- Murray M, Alland D. Methodological problems in the molecular epidemiology of tuberculosis. Am J Epidemiol. 2002;155:565–71. DOIPubMedGoogle Scholar
- Houben RM, Glynn JR. A systematic review and meta-analysis of molecular epidemiological studies of tuberculosis: development of a new tool to aid interpretation. Trop Med Int Health. 2009;14:892–909. DOIPubMedGoogle Scholar
- Fok A, Numata Y, Schulzer M, FitzGerald MJ. Risk factors for clustering of tuberculosis cases: a systematic review of population-based molecular epidemiology studies. Int J Tuberc Lung Dis. 2008;12:480–92.PubMedGoogle Scholar
- Kulldorff M, Nagarwalla N. Spatial disease clusters: detection and inference. Stat Med. 1995;14:799–810. DOIPubMedGoogle Scholar
- Ghosh S, Moonan PK, Cowan L, Grant J, Kammerer S, Navin TR. Tuberculosis genotyping information management system: enhancing tuberculosis surveillance in the United States. Infect Genet Evol. 2011 Oct 25; [Epub ahead of print]. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Reported tuberculosis in the United States, 2009. Atlanta: US.Department of Health and Human Services; October 2010 [cited 2012 Jan 12]. http://www.cdc.gov/tb/statistics/reports/2010/default.htm
- Cowan LS, Diem L, Monson T, Wand P, Temporado D, Oemig TV, Evaluation of a two–step approach for large–scale, prospective genotyping of Mycobacterium tuberculosis isolates in the United States. J Clin Microbiol. 2005;43:688–95. DOIPubMedGoogle Scholar
- Click ES, Moonan PK, Winston CA, Cowan LS, Oeltmann JE. Relationship between Mycobacterium tuberculosis phylogenetic lineage and clinical site of disease. Clin Infect Dis. 2012;54:211–9. DOIPubMedGoogle Scholar
- Oeltmann JE, Kammerer JS, Pevzner ES, Moonan PK. Tuberculosis and substance abuse in the United States, 1997–2006. Arch Intern Med. 2009;169:189–97. DOIPubMedGoogle Scholar
- Kulldorff M. A spatial scan statistic. Comm Statist Theory Methods. 1997;26:1481–96. DOIGoogle Scholar
- Kulldorff M; Information Management Services, Inc. SaTScanTM v8.0: Software for the spatial and space-time scan statistics [cited 10 Jan 2012]. http://www.satscan.org/
- United States Census Bureau. Census geographic regions.[cited 2011 Oct 18]. http://www.census.gov/geo/www/geo_defn.html#CensusRegion
- Miller AC, Sharnprapai S, Suruki R, Corkren E, Nardell EA, Driscoll JR, Impact of genotyping of Mycobacterium tuberculosis on public health practice in Massachusetts. Emerg Infect Dis. 2002;8:1285–9.PubMedGoogle Scholar
- Vanhomwegen J, Kwara A, Martin M, Gillani FS, Fontanet A, Mutungi P, Impact of immigration on the molecular epidemiology of tuberculosis in Rhode Island. J Clin Microbiol. 2011;49:834–44. DOIPubMedGoogle Scholar
- Glynn JR, Crampin AC, Yates MD, Traore H, Mwaungulu FD, Ngwira BM, The importance of recent infection with Mycobacterium tuberculosis in an area with high HIV prevalence: a long-term molecular epidemiological study in Northern Malawi. J Infect Dis. 2005;192:480–7. DOIPubMedGoogle Scholar
- Lathan M, Mukasa LN, Hooper N, Golub J, Baruch N, Mulcahy D, Cross-jurisdictional transmission of Mycobacterium tuberculosis in Maryland and Washington, DC, 1996–2000, linked to the homeless. Emerg Infect Dis. 2002;8:1249–51.PubMedGoogle Scholar
- Geng E, Kreiswirth B, Driver C, Li J, Burzynski J, DellaLatta P, Changes in the transmission of tuberculosis in New York City from 1990 to 1999. N Engl J Med. 2002;346:1453–8. DOIPubMedGoogle Scholar
- Nava-Aguilera E, Andersson N, Harris E, Mitchell S, Hamel C, Shea B, Risk factors associated with recent transmission of tuberculosis: systematic review and meta-analysis. Int J Tuberc Lung Dis. 2009;13:17–26.PubMedGoogle Scholar
- Story A, Murad S, Roberts W, Verheyen M, Hayward AC; London Tuberculosis Nurses Network. Tuberculosis in London: the importance of homelessness, problem drug use and prison. Thorax. 2007;62:667–71. DOIPubMedGoogle Scholar
- Weis S. Contact investigations: how do they need to be designed for the 21st century? Am J Respir Crit Care Med. 2002;166:1016–7. DOIPubMedGoogle Scholar
- Taylor Z. Guidelines for the investigation of contacts of persons with infectious tuberculosis. Recommendations from the National Tuberculosis Controllers Association and CDC. MMWR Recomm Rep. 2005;54(RR-15):1–81.PubMedGoogle Scholar
- Asghar RJ, Patlan DE, Miner MC, Rhodes HD, Solages A, Katz DJ, Limited utility of name-based tuberculosis contact investigations among persons using illicit drugs: results of an outbreak investigation. J Urban Health. 2009;86:776–80. DOIPubMedGoogle Scholar
- Perri BR, Proops D, Moonan PK, Munsiff SS, Kreiswirth BN, Kurepina N, Mycobacterium tuberculosis cluster with developing drug resistance, New York, New York, USA, 2003–2009. Emerg Infect Dis. 2011;17:372–8.PubMedGoogle Scholar
- Schürch AC, Kremer K, Kiers A, Daviena O, Boeree MJ, Siezen RJ, The tempo and mode of molecular evolution of Mycobacterium tuberculosis at patient-to-patient scale. Infect Genet Evol. 2010;10:108–14. DOIPubMedGoogle Scholar
- Supply P, Allix C, Lesjean S, Cardoso-Oelemann M, Rusch-Gerdes S, Willery E, Proposal for standardization of optimized mycobacterial interspersed repetitive unit–variable-number tandem repeat typing of Mycobacterium tuberculosis. J Clin Microbiol. 2006;44:4498–510. DOIPubMedGoogle Scholar
Figures
Tables
Cite This ArticleTable of Contents – Volume 18, Number 3—March 2012
| EID Search Options |
|---|
|
|
|
|
|
|

Please use the form below to submit correspondence to the authors or contact them at the following address:
Patrick K. Moonan, Centers for Disease Control and Prevention, 1600 Clifton Rd NE, Mailstop E10, Atlanta, GA 30333, USA
Top