Volume 19, Number 7—July 2013
Dispatch
Clinical Findings for Early Human Cases of Influenza A(H7N9) Virus Infection, Shanghai, China
Cite This Article
Citation for Media
Abstract
A novel strain of influenza A(H7N9) virus has emerged in China and is causing mild to severe clinical symptoms in infected humans. Some case-patients have died. To further knowledge of this virus, we report the characteristics and clinical histories of 4 early case-patients.
Avian influenza A(H7N9) virus normally circulates among birds; however, human infections with this virus were confirmed in China on March 31, 2013 (1,2). To help identify the best treatment strategies for influenza A(H7N9) virus infection, we summarized the clinical characteristics and outcomes for the first 4 patients who were transferred to Shanghai Public Health Clinical Center (SHPHCC) for treatment of influenza A(H7N9) virus infection. For each case, infection was confirmed by the Shanghai Municipal Centers for Disease Control and Prevention.
Clinical features of the 4 case-patients are listed in Table 1. All case-patients were 58- to 73-year-old married men, farmers or retirees, and long-term residents of Shanghai (Fengxian, Baoshan, Songjiang, and Pudong districts, respectively). Case-patient 1 had a history of coronary heart disease and hepatic schistosomiasis; case-patient 2 had no history of chronic disease; case-patient 3 had a history of hypertension and gout; and case-patient 4 had a history of hypertension and repetitive cough for >10 years during spring and autumn.
Case-patient 1 raised chickens at home. Case-patients 2–4 had no clear history of close contact with poultry; however, each had visited various farmers’ markets that sold live poultry. None of the patients raised pigeons or live in or near a heavily pigeon-infested area.
Before being transferred to SHPHCC on April 6, 2013 (patients 1 and 2) and April 7, 2013 (patients 3 and 4), the 4 patients had been treated in local hospitals; infection with influenza A(H7N9) virus had been confirmed by real-time reverse transcription PCR of nasopharyngeal swab samples before transfer. The case-patients had cough and fever and had been expectorating sputum for ≈6–7 days before admittance to SHPHCC. In addition, all had experienced cold-like symptoms and fatigue before influenza-like symptoms developed. Case-patient 4 had cough and fever for 18 and 10 days, respectively, before being transferred to SHPHCC; his case was the most serious of the 4, and the disease progressed rapidly after he was transferred to SHPHCC.
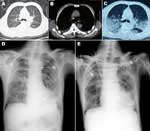
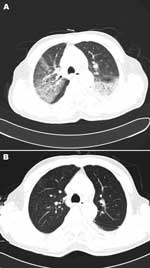
Total leukocyte counts for case-patients 1–4 were within or slightly below reference values: 5.50, 5.95, 3.50, and 4.60 × 109/L, respectively (reference value 4.00–10.00 × 109/L). The proportions of neutrophils were normal or slightly high: 79.6%, 62.6%, 72.4%, and 68.0%, respectively (reference value 50.0%–70.0%). Laboratory test results at admission are shown in Table 2. Radiograph findings mainly included ground-glass opacity and consolidation (Figures 1, 2; Technical Appendix Figures 1, 2). Computed tomography (CT) scans and radiograph findings, along with clinical manifestations and laboratory test results, helped establish early diagnoses.
To ensure proper treatment/management of the patients, an emergency team was established; the team followed the procedures shown in Technical Appendix Figure 3. All 4 case-patients were administered antimicrobial drugs and the antiviral drug oseltamivir. Case-patient 1 began treatment 6 days after the onset of hypoxia, when large areas of lung inflammation were seen on radiographs. Case-patient 2 was treated 4 days after the onset of fever, when CT scan results revealed inflammation in the left upper lung lobe. Case-patient 3 began treatment 4 days after the onset of cough, sputum, and shortness of breath and after CT scan results revealed inflammation in the left lower lung lobe. Case-patient 4 began treatment 16 days after onset of high fever, dyspnea on exertion, and hypoxemia. Additional details for each patient are included below, and results of viral testing done at admission and 5 days later are shown in Technical Appendix Table 1. Disease characteristics for infections caused by influenza virus subtypes H1N1, H5N1, and H7N9 are shown in Technical Appendix Table 2.
Case-patient 1 was receiving noninvasive ventilator-assisted breathing when he arrived at SHPHCC. His oxygen saturation remained at ≈95%, and he was given continuous intravenous dopamine infusion. He had acute respiratory failure, coronary heart disease (stage 2 heart failure), and renal function insufficiency at admission. On April 11, 11 days after the onset of the symptoms and 2 hours after endotracheal intubation and mechanical ventilation began, he died from respiratory failure.
Case-patient 2 arrived at SHPHCC with a nasal cannula inserted to maintain oxygen saturation at 95%. His general condition improved steadily after commencing antiviral drug treatment, and he was discharged 18 days after illness onset.
Case-patient 3 arrived at SHPHCC with a nasal cannula inserted to maintain oxygen saturation at 95%. He had a history of hypertension and gout. He was treated with oseltamivir, antimicrobial drugs, and steroids to suppress lung inflammation. His condition improved substantially, and he was discharged 21 days after illness onset.
Case-patient 4 arrived at SHPHCC in critical condition: oxygen saturation was 88%, and he had shortness of breath (30–35 breaths/min). He was immediately given noninvasive mechanical ventilation. One day after admission, his condition deteriorated; multiple organ dysfunctions in lung and kidney developed. His condition continued to deteriorate despite active treatment with oseltamivir and antimicrobial drugs. Severe hypoxemia developed. Two days after admission, invasive mechanical ventilation and then extracorporeal membrane oxygenation were implemented. The patient was still in critical condition on April 21, 2013.
Clinical manifestations of disease in the 4 case-patients were consistent with those reported for other persons infected with influenza A(H7N9) virus (3). Case-patients 1 and 4 had a more severe disease course than case-patients 2 and 3. All patients sought medical care for unresolved fever, cough, expectoration of sputum, and shortness of breath. The severe cases progressed rapidly: body temperature was mostly sustained >39°C, and breathing was difficult and sometimes accompanied by hemoptysis. A rapid progression of acute respiratory distress syndrome occurred in case-patients 1 and 4, along with mediastinal emphysema, shock, disturbed consciousness, and acute kidney injury. No close contacts of the 4 patients have had signs or symptoms of infection.
The currently available drug treatment for influenza A(H7N9) virus infection is neuraminidase inhibitors (e.g., oseltamivir). Their early use may be recommended (4) but is not always achieved. Case-patient 4 only began neuraminidase inhibitors 16 days after the onset of symptoms, by which time he was in a severe condition. Case-patient 1 was treated with oseltamivir 6 days after the onset of symptoms and, despite treatment, died 6 days after admission to SHPHCC. Earlier, higher doses combined with continuous treatment might improve patient outcomes (5). On the basis of clinical judgment, we now use 150 mg of oseltamivir twice daily for severe cases, monitoring for toxicity.
The benefits of oseltamivir treatment of influenza A(H7N9) virus infections are debatable; for example, case-patients 2 and 3 remained positive for the virus after 9–11 days of oseltamivir treatment (Technical Appendix Table 1). Thus, it is essential to determine whether the virus has developed resistance to oseltamivir. Ineffectiveness of the oral oseltamivir formulations may also have contributed to treatment failure, especially for case-patients 1 and 4: the drug may not have been well absorbed, especially by patients in severe condition. If available in the future, systemic delivery of oseltamivir may be superior.
Of the 4 patients reported here, only case-patient 1 died shortly after admission to SHPHCC. He is also the only patient who had close contact with chickens. However, it is not clear that this contact contributed to the rapid progression of disease in case-patient 1, especially given the fact that case-patient 4, who is still in critical condition, also had rapid progression of disease. The other patients did not raise birds at home, but they visited live poultry markets.
Prompt and early communication of the clinical features of persons infected with avian influenza A(H7N9) virus is crucial to the development of effective treatment strategies (6). Research to understand the transmission pattern and effective control of this virus is urgently needed (7–9).
Dr Lu is director of the Respiratory Department, SHPHCC, and is in charge of treatment and management of influenza A(H7N9) virus–infected patients. His primary interest is infectious diseases, especially tuberculosis in children.
Acknowledgments
We thank Thomas Marcinko for his invaluable help editing the manuscript.
This study was funded in part by the National Institute of Allergy and Infectious Diseases, National Institutes of Health, Department of Health and Human Services (contract no. HHSN272200800014C).
References
- Parry J. H7N9 avian flu kills seven and infects 23 in China. BMJ. 2013;346:f2222.PubMedGoogle Scholar
- Parry J. H7N9 avian flu infects humans for the first time. BMJ. 2013;346:f2151. DOIPubMedGoogle Scholar
- Gao R, Cao B, Hu Y, Feng Z, Wang D, Hu W, Human infection with a novel avian-origin influenza A (H7N9) virus. N Engl J Med. 2013 [Epub ahead of print].
- Domínguez-Cherit G, Lapinsky SE, Macias AE, Pinto R, Espinosa-Perez L, de la Torre A, Critically ill patients with 2009 influenza A(H1N1) in Mexico. JAMA. 2009;302:1880–7. DOIPubMedGoogle Scholar
- White NJ, Webster RG, Govorkova EA, Uyeki TM. What is the optimal therapy for patients with H5N1 influenza? PLoS Med. 2009;6:e1000091. DOIPubMedGoogle Scholar
- Uyeki TM, Cox NJ. Global concerns regarding novel influenza A (H7N9) virus infections. N Engl J Med. 2013 [Epub ahead of print].
- Fauci AS, Collins FS. Benefits and risks of influenza research: lessons learned. Science. 2012;336:1522–3 . DOIPubMedGoogle Scholar
- Patterson AP, Tabak LA, Fauci AS, Collins FS, Howard S. Research funding. A framework for decisions about research with HPAI H5N1 viruses. Science. 2013;339:1036–7 . DOIPubMedGoogle Scholar
- Lurie N, Manolio T, Patterson AP, Collins F, Frieden T. Research as a part of public health emergency response. N Engl J Med. 2013;368:1251–5. DOIPubMedGoogle Scholar
Figures
Tables
Cite This Article1These authors contributed equally to this article.
Table of Contents – Volume 19, Number 7—July 2013
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Shuihua Lu, Shanghai Public Health Clinical Center, 2901 Caolong Rd, Jinshan, Shanghai 201508, Peoples’ Republic of China
Top