Volume 27, Number 7—July 2021
Research
Shiga Toxin–Associated Hemolytic Uremic Syndrome in Adults, France, 2009–2017
Cite This Article
Citation for Media
Abstract
We conducted a retrospective study on hemolytic uremic syndrome caused by Shiga toxin–producing Escherichia coli (STEC) in 96 adults enrolled in the cohort of the National Reference Center for Thrombotic Microangiopathies network in France during 2009–2017. Most infections were caused by STEC strains not belonging to the O157 or O104 serogroups. Thirty (31.3%) patients had multiple risk factors for thrombotic microangiopathy. In total, 61 (63.5%) patients required dialysis, 50 (52.1%) had a serious neurologic complication, 34 (35.4%) required mechanical ventilation, and 19 (19.8%) died during hospitalization. We used multivariate analysis to determine that the greatest risk factors for death were underlying immunodeficiency (hazard ratio 3.54) and severe neurologic events (hazard ratio 3.40). According to multivariate analysis and propensity score-matching, eculizumab treatment was not associated with survival. We found that underlying conditions, especially immunodeficiency, are strongly associated with decreased survival in adults who have hemolytic uremic syndrome caused by STEC.
Shiga toxin–producing Escherichia coli (STEC) infection is an environmental foodborne or waterborne disease that causes bloody diarrhea. Approximately 5%–20% of cases are complicated by hemolytic uremic syndrome (HUS) (1,2). Shiga toxins (Stx) can cause acute microvascular injury, leading to thrombotic microangiopathy (TMA), which is characterized by hemolytic anemia and thrombocytopenia, and in the scenario of HUS, associated with acute kidney injury (3). Researchers estimate that the global prevalence of STEC infection is ≈43.1 acute illnesses/100,000 person-years, causing ≈3,890 annual cases of STEC-associated HUS (4). STEC-associated HUS occurs mostly in children; sporadic cases are rare in adults.
Among children, STEC-associated HUS is the most frequent form of TMA and the leading cause of acute renal failure (3). In France, surveillance for STEC-associated HUS in children <15 years of age has existed since 1996. This surveillance system comprises 32 pediatric healthcare centers, including all 21 university hospital units specializing in pediatric nephrology. These centers notify public health authorities of cases of STEC-associated HUS. The National Reference Center for Escherichia coli, Shigella and Salmonella at the Institut Pasteur (NRC-Ec; Paris, France) and its associated laboratory at the Robert Debré University Hospital (Paris, France) confirm and characterize STEC infections in children and adults. This surveillance network estimated the annual incidence of HUS in France to be 1.00 case/100,000 child-years, causing a ≈1% death rate during 2007–2016 (5).
Despite the much lower incidence of HUS among adults than children, most deaths caused by STEC-associated HUS occur among persons >60 years of age (2,6). The French national health authorities do not have a dedicated surveillance system for STEC-associated HUS in adults. In 2011, a large STEC outbreak in Europe sickened 3,816 persons in Germany, causing 845 cases of HUS and 54 deaths; 24 persons were affected in the Bordeaux region of France, including 9 who had HUS, 8 of whom were adults (7,8). The outbreak was linked to an atypical hybrid pathotype E. coli O104:H4 strain characterized by enteroaggregative and enterohemorrhagic virulence; the strain also produced an extended spectrum β-lactamase. Most (88%) patients involved in this outbreak, which was associated with consumption of organic fenugreek sprouts, were adults, and the median age was 42 years. Publicity surrounding this outbreak raised awareness of STEC-associated HUS in adults. However, cases of STEC-associated HUS in adults remain rare (9,10). Hence, the clinical characteristics of adult STEC-associated HUS and the effects of therapeutic strategies on outcome remain uncertain. We describe the epidemiologic and clinical features of adults with STEC-associated HUS, identify predictors of patient outcomes, and assess the effectiveness of therapeutic interventions in this population.
Study Design, Settings, and Data Sources
We conducted a retrospective cohort study of STEC-associated HUS cases in adults registered during January 2009–December 2017 in France by the Centre National de Référence des Microangiopathies Thrombotiques (CNR-MAT; https://www.cnr-mat.fr). We reviewed all medical files from the CNR-MAT database. This work was part of the TMA study approved by our institutional review board (Comité pour la protection des personnes Ile-de-France; approval no. CPP04807) in accordance with the Declaration of Helsinki and the French Data Protection Authority.
Diagnostic Criteria
The diagnosis of HUS required the coexistence of TMA (i.e., thrombocytopenia [platelet levels <150,000 cells/μL] and microangiopathic hemolytic anemia [hemoglobin levels <12 g/dL]) and an acute kidney injury (AKI). We included all TMA patients >18 years of age in the CNR-MAT cohort who had an AKI and a positive PCR result for the Stx genes stx1, stx2, or both. We considered patients to have fever if they had a temperature of >38°C within 24 hours after admission.
Microbiological Data
Participating laboratories conducted PCR specific for stx1 and stx2 on E. coli strains isolated from stool, blood, and urine samples. Laboratory technicians also cultured samples from stx-positive stools. To characterize the isolated STEC strains, technicians used an O-serogroup multiplex PCR selective for the 10 most frequent serogroups affecting humans in France: O157, O26, O145, O55, O103, O104, O111, O91, O121, and O80 (11). Strains belonging to other serogroups were characterized by PCR of the restriction fragment length polymorphism of the O operon, rfb (rfb-RFLP) (12). In April 2017, NRC-Ec and local laboratories also began to characterize strains using whole-genome sequencing, when available. If a strain was stx-positive but its serogroup was not identified by culture, we classified that strain as not isolated.
Variables
Participating laboratories and physicians submitted data on each patient’s medical history, clinical and biological features, microbiological findings, and treatment at admission and during hospitalization (13). We retrospectively calculated each patient’s age-weighted Charlson Comorbidity Index (CCI) (14) and classified AKI according to the Kidney Disease: Improving Global Outcomes (KDIGO) criteria published by the International Society of Nephrology (15). We investigated ADAMTS13 and complement alternative pathway (CAP) activity as previously described (16).
Treatments and Outcomes
Treatment consisted mainly of therapeutic plasma exchange (TPE) or best supportive care (BSC) according to the discretion of the treating physician. The C5 complement blocker eculizumab (Soliris; Alexion Pharmaceuticals, Inc., https://alexion.com) also was given at the discretion of the treating physician; however, physicians were encouraged to discuss eculizumab use with a member of the CNR-MAT team. The primary outcome of this study was patient survival at the time of most recent follow-up.
Statistics
We reported qualitative variables as frequencies and percentages; we reported quantitative discrete and continuous variables as medians and interquartile ranges (IQRs). We estimated survival using the Kaplan-Meier method. We used Cox proportional hazards regression to identify factors independently associated with survival. The proportional hazard assumption was supported by a nonsignificant relationship between scaled Schoenfeld residuals and time and refuted by a significant relationship using an alpha (α) risk set at 5%. We reported the results using hazard ratios (HRs) and 95% CIs, using an α risk set at 5% statistical significance. To quantify the effect of eculizumab on survival, we calculated and compared the propensity scores of patients who did and did not use eculizumab (Appendix). We used R software version 3.6.1 (The R Project for Statistical Computing, https://www.r-project.org) for statistical analysis. For propensity score analysis, we used MatchIt package (17).
Of the 4,048 patients in the CNR-MAT cohort, we first identified 61 adult STEC-associated HUS patients with complete data during January 2009–December 2017. After comparing the NRC-Ec and CNR-MAT surveillance data, we identified 35 additional patients to be included in the study cohort. In total, the study cohort comprised 96 patients (Appendix Figure 1). This cohort included patients from hospitals throughout France, most of which were part of the CNR-MAT network (Figure 1, panel A). The women-to-men ratio was 1.7 and median age was 60.5 years (IQR 47.0–71.0 years) (Figure 1, panel B). Geographic, temporal, and microbiological characteristics of the cases suggested an outbreak among 13 patients (Figure 1). The cohort also included 8 patients affected by the 2011 O104:H4 outbreak in France described previously (8). We found a patient in our cohort who was infected in a family cluster of STEC-associated HUS in 2014, but the strain could not be identified. We also found 4 patients (2 in Marne, 1 in Nord, 1 in Paris) who tested positive for STEC O91 in summer 2013 but did not share a known infection source.
In total, 69 (71.9%) patients had underlying conditions; the median CCI was 2.00 (IQR 1.00–4.25) (Table 1). Of the 96 patients, 27 (28.1%) had an underlying immunodeficiency and 30 (31.3%) had >1 condition that might contribute to TMA.
Most (83.3%) patients had diarrhea and nearly half (49.0%) had bloody diarrhea; 11 patients had severe colitis, including 4 who required emergency surgery (Table 2). All patients had renal impairment. In 2011, 2 patients with STEC O104:H4 infection had proteinuria (i.e., >1 g/L) but not serum creatinine elevation; these patients also had microangiopathic hemolytic anemia and peripheral thrombocytopenia (8). The other 94 patients all had AKI stage 1 or higher according to KDIGO criteria, of which 61 (63.5%) required dialysis. Of 12 patients who underwent kidney biopsy, 11 showed signs of TMA. Most (76%) patients had neurologic symptoms, mainly confusion (56.3%) and headache (18.8%). Approximately half (52.1%) of patients had a serious neurologic complication such as seizure, coma, or focal deficiency. In addition, 34 (35.4%) patients required mechanical ventilation. In total, 42 patients had high blood pressure (>150/90 mm Hg) at admission; severe hypertension (>170/110 mm Hg) subsequently developed in 11 patients and hypertensive retinopathy developed in 6 patients. Only 2 patients had hypotension (<90/60 mm Hg) at admission. In total, 41 (42.7%) patients had cardiac events; in 26 of 43 cases with available data, patients had troponin levels above the defined threshold of their respective laboratory (Table 2).
CAP measurements during the acute phase of illness were recorded in 69 patients. Of these patients, 36 (52.2%) had values within the reference range (Table 2). Less than 10% of patients had low levels of C3, C4, factor H, or factor I, whereas 26 (38.8%) patients had low levels of CH50. CD46 levels were low in 65.7% (23/35) patients. Two patients had low levels of anti-factor H antibodies (242 and 800 arbitrary units) (Table 2). ADAMTS13 activity was detectable (>10%) in all 69 patients in whom it was tested.
Among the 84 cases in which stx type was detected, stx1–/stx2+ was the most common genotype (85.7%). The stx1+/stx2– genotype was significantly associated with increased CCI and immunodeficiency (Appendix Table 1). As expected, the most common STEC isolation site was stool (93.8%), whereas only 10 patients had STEC-positive urine or blood samples. Seven (7.3%) patients had STEC-positive urine samples, including 5 who had a urologic infection without associated colitis. Four patients had STEC-positive blood samples, including 1 patient for whom STEC was identified in blood samples only. In total, 5 patients had a multisite infection.
Most (60; 62.5%) had a serogroup typable by the NRC-Ec; 7 (7.3%) patients had an untypable serogroup. The most common serogroups were O91 (12; 17.9%) and O157 (10; 14.9%) (Table 2). The STEC isolates from urine samples belonged to the O104, O91, O106, O126, O174, and O148 serogroups; isolates from blood samples belonged to the O80, O103, and O128 serogroups (Appendix Table 2).
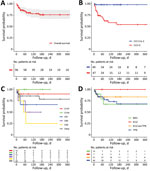
In total, 19 (19.8%) patients died during hospitalization (Figure 2, panel A; Appendix Table 3). Patients died 3–152 days after admission and had a median follow-up period of 112 days (IQR 49–238). After follow-up, 1 patient had HELLP (hemolysis, elevated liver enzymes, low platelets) syndrome; the patient was STEC-negative at the time of the episode. None of the surviving patients had a further episode of TMA during follow-up.
Patients were treated mainly with BSC, TPE, or eculizumab; 3 patients also received immunoadsorption treatment (Appendix Table 4). Of the 61 patients who required dialysis, 17 (25.4%) died. At the end of the follow-up period, 6 (9.8%) patients still required dialysis, including 4 who had a follow-up period of >90 days. Patients who received dialysis were treated for a median duration of 13.5 days (IQR 8–28 days); 38 patients no longer required dialysis at the end of the follow-up period. After a median follow-up period of 34 days (IQR 23–75 days), the median serum creatinine value was 92 μmol/L (IQR 74–124 μmol/L). Of the 50 patients with a severe neurologic complication, 14 (28.0%) died. Of the 25 surviving patients with available data, 8 (32.0%) patients had neurologic sequelae, including persistent sensorimotor deficit (7, 28.0%), epilepsy (2, 8.0%), and cognitive impairment (2, 8.0%).
In total, 26 (27.1%) patients were treated with macrolides, including 3 who received the treatment to prevent infectious meningoencephalitis associated with eculizumab. Fifty-seven (59.4%) patients received β-lactam antimicrobial drugs, aminoglycosides, or quinolones; 22 (22.9%) patients received metronidazole.
After unadjusted analysis, we found that age (HR 1.04, 95% CI 1.01–1.07; p = 0.01), CCI (HR 1.15, 95% CI 1.03–1.28; p = 0.02) (Figure 2, panel B), underlying immunodeficiency (HR 4.36, 95% CI 1.72–11.07; p<0.01), and associated digestive disease (HR 4.07, 95% CI 1.63–10.14; p<0.01) were significantly associated with death of all causes (Table 3). We also found that severe neurologic events (HR 2.90, 95% CI 1.04–8.06; p = 0.04), mechanical ventilation (HR 2.71, 95% CI 1.09–6.74; p = 0.03), and dialysis (HR 5.57, 95% CI 1.29–24.16; p = 0.02) were predictive of death. High troponin levels and stx types were not associated with survival (Table 3). Most patients who died had STEC strains belonging to non-O104 and non-O157 serogroups (Figure 2, panel C; Appendix Table 3). We found that overall survival was comparable among patients treated by different combinations of BSC, TPE, and eculizumab (p = 0.43 by log-rank test) (Table 3; Figure 2, panel D). The use of macrolides was not associated with survival (p = 0.77).
Multivariate analysis showed that underlying immunodeficiency (HR 3.54, 95% CI 1.24–10.14; p = 0.02) and severe neurologic events (HR 3.40, 95% CI 1.05–11.04; p = 0.04) were negatively associated with survival (Table 3). After adjustment of determinants retained for the multivariate analysis, we found that eculizumab was not associated with survival (HR 0.77, 95% 0.25–2.33; p = 0.64). Propensity score-matching also indicated that eculizumab was not associated with survival (p = 0.34) (Appendix Table 5, Figure 2).
We found that 20% of adults who had STEC-associated HUS died during hospitalization, in agreement with previous findings (9,10); however, <1% of children who had STEC-associated HUS died in France during the same years, 2007–2016 (5). In addition, adults had cerebral involvement 3 times more frequently than children (2); 52.1% of adult patients had severe neurologic manifestations, similar to the observations of Karpac et al. (10). Renal recovery was slow and inconsistent; 4 patients still required dialysis 90 days after hospitalization (9). One third of patients required mechanical ventilation. These findings emphasize that, in adults, STEC-associated HUS is a severe systemic disease that can cause multiple organ failure. However, inclusion in the CNR-MAT registry relied on voluntary physician reporting; thus, this case series is not exhaustive and might disproportionately reflect the most severe cases. As previously observed for children (18), most cases in this cohort were sporadic and, for unclear reasons, in women. In regard to age distribution, STEC-associated HUS has a U curve from birth to old age (6,9,10,19). During the study period, 1,095 STEC-associated HUS cases in children were reported to Santé Publique France through the country’s pediatric surveillance network (5). By comparison, this disease appears to be much rarer among adults, although underreporting is probable.
Our findings on underlying conditions and deaths by age group resemble those of the FoodNet registry of elderly adults with STEC-associated HUS (9). The risk for death from STEC-associated HUS increases for persons age >40 years, suggesting that young and middle-aged adults have similar clinical courses to those observed in children. We found a strong association between underlying conditions and decreased survival, especially for patients with immunodeficiency (9,20–23). The prevalence of antibodies against Stx decreases for persons >40 years of age (24), which might account for the more severe forms of STEC-associated HUS in elderly persons. The expression of glomerular globotriaosylceramide (Gb3), the main receptor of Stx, was thought to decrease with age; however, researchers now believe that expression levels remain stable throughout a person’s lifetime (25). Renal and neurologic signs similar to those caused by HUS develop in immunocompromised mice after STEC inoculation or Stx exposure, whereas wild-type mice are naturally resistant to this disease (26,27). Together, these findings highlight the role of the immune system in preventing STEC-associated HUS. Immunodeficiency probably contributes to disease severity.
The 2011 outbreak in Europe illustrated that microbiological characteristics play a key role in STEC-associated HUS (7). The distribution of serotypes among adults in our study was slightly different than in a study on pediatric HUS in France in the same timeframe (5). Non-O157 strains were more prevalent in the pediatric series (5) and in ours, whereas O157 and O26 were more commonly observed among children than adults (23% among children vs. 15% among adults for O157; 11% among children vs. 6% among adults for O26) (5). A similar overall distribution was observed among children and adults with STEC infection in Norway (23% for O157, 10% for O26) (28). By contrast, serogroups O91 and O104 have been mainly found among adults (29,30). The data might have been skewed by the 2011 outbreak caused by a strain belonging to the O104 serogroup; this outbreak caused infections in younger persons who had fewer underlying conditions, which could account for the better outcomes of those patients. Other serogroups, especially O80, O26, and O91, are emerging and might be associated with increased pathogenicity (2,18). STEC O91 was also the most common serogroup among adults with STEC infections in Germany (30), which raises the question of increased pathogenicity in adults and in persons >40 years of age.
In agreement with previous reports of STEC-associated HUS in adults (29,31), we found that stx1+/stx2– strains were more prevalent among adults (14.3%) than had been previously documented among children (2.0%) (5). One possible explanation for this distribution might be that in some patients, HUS was concurrent with but unrelated to infection or colonization by stx1+/stx2– STEC; however, this scenario is unlikely because STEC-positive patients had typical features of HUS in an infectious context. We cannot exclude the possibility that the stx2 gene could have been lost in human hosts during infection or ex vivo during subculture, as already described for STEC O26 (32). In this series, all stx1+/stx2– strains belonged to non-O157 serogroups. These findings are similar to those of Käppeli et al. (29), who found that 15.8% of cases of non-O157 STEC–associated HUS were caused by stx1+/stx2– strains, which could suggest that different serogroups might pose different risks for HUS associated with particular stx genotypes. Last, most (83%) patients with stx1+/stx2– genotypes had underlying immunodeficiency; one explanation could be that immunodeficient patients are more susceptible to Stx1. The alleles stx1 and stx2c have been associated with a lower risk for severe STEC infection and HUS (28). However, stx1a is associated with higher risk for severe STEC infection (33). We did not have data on stx subtypes in our study.
We observed CAP abnormalities similar to those previously reported in a cohort of 113 cases of STEC-associated HUS in children (16). We found that 65.7% of patients had low CD46 and 38.8% had low CH50 levels. However, a decrease in the concentration of complement factors, the interpretation of which remains equivocal, might be attributable to kidney damage and STEC-associated HUS (16). The presence of an inflammatory syndrome further complicates the interpretation of these data. In contrast to atypical HUS, pediatric STEC-associated HUS has not been linked to a constitutional or acquired dysregulation of the CAP. Screening for variants in complement genes is not usually conducted among children with STEC-associated HUS. Similarly, it seems unlikely that STEC infection reveals underlying CAP abnormalities in many adults.
We found that 7% of patients had STEC-positive urine samples, an underrecognized finding documented by Lavrek et al. (34). Although urine samples might be easily contaminated, especially in patients who have diarrhea, these findings encourage systematic STEC-specific PCR screening and culture confirmation of stool or other biological samples (in the event of extraintestinal E. coli infection) from adult TMA patients (2,34).
Because the effectiveness of specific treatments remains unclear, BSC is the cornerstone of STEC-associated HUS treatment (2,35,36). Univariate analysis indicated that TPE was not associated with overall survival improvement, although other studies have concluded differently (37–39). However, considering the substantial overlap between the signs and symptoms of STEC-associated HUS in adults and TMA of other etiologies, some researchers believe that plasma therapy should be given until TTP or atypical HUS are ruled out (13,40). Whether TPE should be continued after the determination of stx status remains unclear. As previously reported, we did not find a clear survival benefit from eculizumab (38,41). However, the small sample size and the strong differences between patients who did and did not receive eculizumab treatment preclude definitive conclusions.
The benefits of antimicrobial drugs in treating STEC-associated HUS are unclear (42,43). Previous studies suggest that the use of antimicrobial drugs during early stages of STEC infection is associated with the development of HUS. However, the effects of antimicrobial drugs administered after HUS diagnosis remain unknown (42). A retrospective study reported that azithromycin administered during STEC infection might reduce the duration of STEC carriage (43). We found that use of macrolides was not associated with survival. This observation might have been confounded by possible unreported administration of antimicrobial drugs before hospitalization, treatment for unstandardized indications at the discretion of the practitioner, or other variables. We also found that the prescription of multiple antimicrobial drugs was a common practice, especially in cases of severe infection.
In conclusion, STEC-associated HUS is rarer among adults than among children but causes more severe disease and death. Underlying conditions, especially immunodeficiency, are strongly associated with decreased survival. The severity of the disease, a probably underestimated prevalence, and the risk for outbreaks of emerging STEC-associated HUS provide strong arguments for active epidemiologic and microbiological surveillance of this disease.
Dr. Travert is a medical intern at Assistance Publique-Hôpitaux de Paris in Paris, France. His research interests include the epidemiology of STEC-associated HUS and environmental factors contributing to autoimmune diseases.
Members of the Reference Center for Thrombotic Microangiopathies team: Jean-François Augusto, Elie Azoulay, Virginie Barbay, Ygal Benhamou, Dominique Bordessoule, Christophe Charasse, Anne Charvet-Rumpler, Dominique Chauveau, Gabriel Choukroun, Jean-Philippe Coindre, Paul Coppo, Elise Corre, Yahsou Delmas, Georges Deschenes, Alain Devidas, Antoine Dossier, Olivier Fain, Fadi Fakhouri, Véronique Frémeaux-Bacchi, Lionel Galicier, Steven Grangé, Bertrand Guidet, Jean-Michel Halimi, Mohamed Hamidou, Raoul Herbrecht, Miguel Hié, Frédéric Jacobs, Bérangère Joly, Tarik Kanouni, Gilles Kaplanski, Alexandre Lautrette, Véronique Le Guern, Bruno Moulin, Christiane Mousson, Mario Ojeda Uribe, Abdelkader Ouchenir, Nathalie Parquet, Frédéric Pène, Pierre Perez, Pascale Poullin, Claire Pouteil-Noble, Claire Presne, François Provôt, Eric Rondeau, Samir Saheb, Amélie Seguin, Aude Servais, Alain Stépanian, Agnès Veyradier, Cécile Vigneau, Alain Wynckel, and Patricia Zunic.
Acknowledgments
We thank Eric Alamartine, Sandrine Bedon Carte, Gilles Bernardin, Severin Cabasson, Vincent Cadiergue, Jean-François Cerfon, Thomas Crepin, Vincent Das, Philippe De Swardt, Geneviève Dumont, Alexandre Hertig, Jean Claude Lacherade, Olivier Leroy, Julie Le Scanff, Didier Perez, Emilie Pinçon, Jean-Pierre Quenot, Felipe Suarez, Rachel Tetaz, Olivier Thaunat, Jean Marc Thouret, and Xavier Valette for their valuable collaboration with the CNR-MAT. These physicians played an active role in care of patients with STEC-associated HUS.
This work was partly funded by grants from the French Ministry of Health (Programme Hospitalier de Recherche Clinique [grant nos. P120118 and AOM12259]). B.T. has received a research grant from CSL Behring (https://www.cslbehring.com). E.R. and C.P. are members of the Advisory Board for Alexion Pharmaceuticals, Inc. (https://alexion.com). Y.D. has received lecture fees from Alexion Pharmaceuticals, Inc. and honorarium as advisory board member for Sanofi (https://www.sanofi.com). F.F. has received consultancy fees and speaker honoraria from F. Hoffmann-La Roche Ltd (https://www.roche.com); Alexion Pharmaceuticals, Inc.; Apellis Pharmaceuticals (https://apellis.com); Achillion Pharmaceuticals; Novartis AG (https://www.novartis.com); and Alnylam Pharmaceuticals, Inc. (https://www.alnylam.com). P.C. is member of the advisory boards of Alexion Pharmaceuticals, Inc.; Sanofi; Shire P.C.C. (http://shirepcc.com); Takeda Pharmaceutical Company Limited (https://www.takeda.com); and Octapharma AG (https://www.octapharma.com); he has received consultancy fees and speaker honoraria from Sanofi; Alexion Pharmaceuticals, Inc.; and Takeda Pharmaceutical Company Limited.
References
- Karmali MA, Steele BT, Petric M, Lim C. Sporadic cases of haemolytic-uraemic syndrome associated with faecal cytotoxin and cytotoxin-producing Escherichia coli in stools. Lancet. 1983;1:619–20. DOIPubMedGoogle Scholar
- Joseph A, Cointe A, Mariani Kurkdjian P, Rafat C, Hertig A. Shiga toxin–associated hemolytic uremic syndrome: a narrative review. Toxins (Basel). 2020;12:67. DOIPubMedGoogle Scholar
- Fakhouri F, Zuber J, Frémeaux-Bacchi V, Loirat C. Haemolytic uraemic syndrome. Lancet. 2017;390:681–96. DOIPubMedGoogle Scholar
- Majowicz SE, Scallan E, Jones-Bitton A, Sargeant JM, Stapleton J, Angulo FJ, et al. Global incidence of human Shiga toxin-producing Escherichia coli infections and deaths: a systematic review and knowledge synthesis. Foodborne Pathog Dis. 2014;11:447–55. DOIPubMedGoogle Scholar
- Bruyand M, Mariani-Kurkdjian P, Le Hello S, King L-A, Van Cauteren D, Lefevre S, et al.; Réseau Français Hospitalier de Surveillance du Shu Pédiatrique. Paediatric haemolytic uraemic syndrome related to Shiga toxin-producing Escherichia coli, an overview of 10 years of surveillance in France, 2007 to 2016. Euro Surveill. 2019;24:24. DOIPubMedGoogle Scholar
- Gould LH, Demma L, Jones TF, Hurd S, Vugia DJ, Smith K, et al. Hemolytic uremic syndrome and death in persons with Escherichia coli O157:H7 infection, foodborne diseases active surveillance network sites, 2000-2006. Clin Infect Dis. 2009;49:1480–5. DOIPubMedGoogle Scholar
- Frank C, Werber D, Cramer JP, Askar M, Faber M, an der Heiden M, et al.; HUS Investigation Team. Epidemic profile of Shiga-toxin-producing Escherichia coli O104:H4 outbreak in Germany. N Engl J Med. 2011;365:1771–80. DOIPubMedGoogle Scholar
- Delmas Y, Vendrely B, Clouzeau B, Bachir H, Bui H-N, Lacraz A, et al. Outbreak of Escherichia coli O104:H4 haemolytic uraemic syndrome in France: outcome with eculizumab. Nephrol Dial Transplant. 2014;29:565–72. DOIPubMedGoogle Scholar
- Gould LH, Jordan JG, Dunn J, Apostol M, Griffin PM; Emerging Infections Program FoodNet Working Group. Postdiarrheal hemolytic uremic syndrome in persons aged 65 and older in foodnet sites, 2000-2006. J Am Geriatr Soc. 2011;59:366–8. DOIPubMedGoogle Scholar
- Karpac CA, Li X, Terrell DR, Kremer Hovinga JA, Lämmle B, Vesely SK, et al. Sporadic bloody diarrhoea-associated thrombotic thrombocytopenic purpura-haemolytic uraemic syndrome: an adult and paediatric comparison. Br J Haematol. 2008;141:696–707. DOIPubMedGoogle Scholar
- Soysal N, Mariani-Kurkdjian P, Smail Y, Liguori S, Gouali M, Loukiadis E, et al. Enterohemorrhagic Escherichia coli hybrid pathotype O80:H2 as a new therapeutic challenge. Emerg Infect Dis. 2016;22:1604–12. DOIPubMedGoogle Scholar
- Coimbra RS, Grimont F, Lenormand P, Burguière P, Beutin L, Grimont PA. Identification of Escherichia coli O-serogroups by restriction of the amplified O-antigen gene cluster (rfb-RFLP). Res Microbiol. 2000;151:639–54. DOIPubMedGoogle Scholar
- Coppo P, Schwarzinger M, Buffet M, Wynckel A, Clabault K, Presne C, et al.; French Reference Center for Thrombotic Microangiopathies. Predictive features of severe acquired ADAMTS13 deficiency in idiopathic thrombotic microangiopathies: the French TMA reference center experience. PLoS One. 2010;5:
e10208 . DOIPubMedGoogle Scholar - Charlson M, Szatrowski TP, Peterson J, Gold J. Validation of a combined comorbidity index. J Clin Epidemiol. 1994;47:1245–51. DOIPubMedGoogle Scholar
- International Society of Nephrology. KDIGO clinical practice guideline for acute kidney injury. 2012 [cited 2020 Jul 31]. https://kdigo.org/wp-content/uploads/2016/10/KDIGO-2012-AKI-Guideline-English.pdf
- Frémeaux-Bacchi V, Sellier-Leclerc A-L, Vieira-Martins P, Limou S, Kwon T, Lahoche A, et al. Complement gene variants and Shiga toxin–producing Escherichia coli-associated hemolytic uremic syndrome. Clin J Am Soc Nephrol. 2019;14:364–77. DOIPubMedGoogle Scholar
- Ho D, Imai K, King G, Stuart EA. MatchIt: nonparametric preprocessing for parametric causal inference. J Stat Softw. 2011;42:1–28. DOIGoogle Scholar
- Karmali MA, Karmali MA. Emerging public health challenges of Shiga toxin–producing Escherichia coli related to changes in the pathogen, the population, and the environment. Clin Infect Dis. 2017;64:371–6. DOIPubMedGoogle Scholar
- Carter AO, Borczyk AA, Carlson JAK, Harvey B, Hockin JC, Karmali MA, et al. A severe outbreak of Escherichia coli O157:H7—associated hemorrhagic colitis in a nursing home. N Engl J Med. 1987;317:1496–500. DOIPubMedGoogle Scholar
- Ville S, Ydee A, Garandeau C, Canet E, Tissot A, Cantarovich D, et al. Shiga toxin-producing Escherichia coli-associated hemolytic uremic syndrome in solid organ transplant recipients. Kidney Int. 2019;96:1423–4. DOIPubMedGoogle Scholar
- Farina C, Gavazzeni G, Caprioli A, Remuzzi G. Hemolytic uremic syndrome associated with verocytotoxin-producing Escherichia coli infection in acquired immunodeficiency syndrome. Blood. 1990;75:2465. DOIPubMedGoogle Scholar
- Vera-Aguilera J, Duma N, Gast K, Alkhateeb H, Tande A, Leung N, et al. Hemolytic uremic syndrome associated with Escherichia coli O157 infection in an allogenic stem cell transplant recipient. Mayo Clin Proc Innov Qual Outcomes. 2018;2:387–91. DOIPubMedGoogle Scholar
- Manière L, Domenger C, Camara B, Giovannini D, Malvezzi P, Rostaing L. An atypical case of Shiga toxin producing–Escherichia coli hemolytic and uremic syndrome (STEC-HUS) in a lung transplant recipient. Case Rep Transplant. 2019;2019:
9465040 . DOIPubMedGoogle Scholar - Karmali MA, Mascarenhas M, Petric M, Dutil L, Rahn K, Ludwig K, et al. Age-specific frequencies of antibodies to Escherichia coli verocytotoxins (Shiga toxins) 1 and 2 among urban and rural populations in southern Ontario. J Infect Dis. 2003;188:1724–9. DOIPubMedGoogle Scholar
- Ergonul Z, Clayton F, Fogo AB, Kohan DE. Shigatoxin-1 binding and receptor expression in human kidneys do not change with age. Pediatr Nephrol. 2003;18:246–53. DOIPubMedGoogle Scholar
- Brando RJF, Miliwebsky E, Bentancor L, Deza N, Baschkier A, Ramos MV, et al. Renal damage and death in weaned mice after oral infection with Shiga toxin 2-producing Escherichia coli strains. Clin Exp Immunol. 2008;153:297–306. DOIPubMedGoogle Scholar
- Karpman D, Connell H, Svensson M, Scheutz F, Alm P, Svanborg C. The role of lipopolysaccharide and Shiga-like toxin in a mouse model of Escherichia coli O157:H7 infection. J Infect Dis. 1997;175:611–20. DOIPubMedGoogle Scholar
- Brandal LT, Wester AL, Lange H, Løbersli I, Lindstedt B-A, Vold L, et al. Shiga toxin-producing escherichia coli infections in Norway, 1992-2012: characterization of isolates and identification of risk factors for haemolytic uremic syndrome. BMC Infect Dis. 2015;15:324. DOIPubMedGoogle Scholar
- Käppeli U, Hächler H, Giezendanner N, Beutin L, Stephan R. Human infections with non-O157 Shiga toxin-producing Escherichia coli, Switzerland, 2000-2009. Emerg Infect Dis. 2011;17:180–5. DOIPubMedGoogle Scholar
- Werber D, Beutin L, Pichner R, Stark K, Fruth A. Shiga toxin-producing Escherichia coli serogroups in food and patients, Germany. Emerg Infect Dis. 2008;14:1803–6. DOIPubMedGoogle Scholar
- Adams NL, Byrne L, Smith GA, Elson R, Harris JP, Salmon R, et al. Shiga toxin–producing Escherichia coli O157, England and Wales, 1983–2012. Emerg Infect Dis. 2016;22:590–7. DOIPubMedGoogle Scholar
- Bielaszewska M, Prager R, Köck R, Mellmann A, Zhang W, Tschäpe H, et al. Shiga toxin gene loss and transfer in vitro and in vivo during enterohemorrhagic Escherichia coli O26 infection in humans. Appl Environ Microbiol. 2007;73:3144–50. DOIPubMedGoogle Scholar
- Byrne L, Adams N, Jenkins C. Association between Shiga toxin–producing Escherichia coli O157:H7 stx gene subtype and disease severity, England, 2009–2019. Emerg Infect Dis. 2020;26:2394–400. DOIPubMedGoogle Scholar
- Lavrek D, Lava SAG, Milani GP, Simonetti GD, Bianchetti MG, Giannini O. Hemolytic-uremic syndrome after Escherichia coli urinary tract infection in humans: systematic review of the literature. J Nephrol. 2018;31:919–24. DOIPubMedGoogle Scholar
- Michael M, Elliott EJ, Ridley GF, Hodson EM, Craig JC. Interventions for haemolytic uraemic syndrome and thrombotic thrombocytopenic purpura. Cochrane Database Syst Rev. 2009;1:
CD003595 . DOIPubMedGoogle Scholar - Grisaru S, Xie J, Samuel S, Hartling L, Tarr PI, Schnadower D, et al.; Alberta Provincial Pediatric Enteric Infection Team. Associations between hydration status, intravenous fluid administration, and outcomes of patients infected with Shiga toxin–producing Escherichia coli: a systematic review and meta-analysis. JAMA Pediatr. 2017;171:68–76. DOIPubMedGoogle Scholar
- Keenswijk W, Raes A, De Clerck M, Vande Walle J. Is plasma exchange efficacious in Shiga toxin–associated hemolytic uremic syndrome? A narrative review of current evidence. Ther Apher Dial. 2019;23:118–25. DOIPubMedGoogle Scholar
- Kielstein JT, Beutel G, Fleig S, Steinhoff J, Meyer TN, Hafer C, et al.; Collaborators of the DGfN STEC-HUS registry. Best supportive care and therapeutic plasma exchange with or without eculizumab in Shiga-toxin-producing E. coli O104:H4 induced haemolytic-uraemic syndrome: an analysis of the German STEC-HUS registry. Nephrol Dial Transplant. 2012;27:3807–15. DOIPubMedGoogle Scholar
- Padmanabhan A, Connelly-Smith L, Aqui N, Balogun RA, Klingel R, Meyer E, et al. Guidelines on the use of therapeutic apheresis in clinical practice—evidence-based approach from the Writing Committee of the American Society for Apheresis: the eighth special issue. J Clin Apher. 2019;34:171–354. DOIPubMedGoogle Scholar
- Joseph A, Rafat C, Zafrani L, Mariani-Kurkdjian P, Veyradier A, Hertig A, et al. Early differentiation of Shiga toxin–associated hemolytic uremic syndrome in critically ill adults with thrombotic microangiopathy syndromes. Crit Care Med. 2018;46:e904–11. DOIPubMedGoogle Scholar
- Lapeyraque A-L, Malina M, Fremeaux-Bacchi V, Boppel T, Kirschfink M, Oualha M, et al. Eculizumab in severe Shiga-toxin-associated HUS. N Engl J Med. 2011;364:2561–3. DOIPubMedGoogle Scholar
- Wong CS, Mooney JC, Brandt JR, Staples AO, Jelacic S, Boster DR, et al. Risk factors for the hemolytic uremic syndrome in children infected with Escherichia coli O157:H7: a multivariable analysis. Clin Infect Dis. 2012;55:33–41. DOIPubMedGoogle Scholar
- Nitschke M, Sayk F, Härtel C, Roseland RT, Hauswaldt S, Steinhoff J, et al. Association between azithromycin therapy and duration of bacterial shedding among patients with Shiga toxin-producing enteroaggregative Escherichia coli O104:H4. JAMA. 2012;307:1046–52. DOIPubMedGoogle Scholar
Figures
Tables
Cite This ArticleOriginal Publication Date: June 11, 2021
1These first authors contributed equally to this article.
2Members of this group are listed at the end of this article.
Table of Contents – Volume 27, Number 7—July 2021
| EID Search Options |
|---|
|
|
|
|
|
|

Please use the form below to submit correspondence to the authors or contact them at the following address:
Paul Coppo, AP-HP.6 and Sorbonne Université, 184 rue du Faubourg Saint-Antoine, Assistance Publique–Hôpitaux de Paris, 75012 Paris, France
Top