Volume 27, Number 9—September 2021
Synopsis
Epidemiology of Coronavirus Disease Outbreak among Crewmembers on Cruise Ship, Nagasaki City, Japan, April 2020
Cite This Article
Citation for Media
Abstract
In April 2020, a coronavirus disease (COVID-19) outbreak occurred on the cruise ship Costa Atlantica in Nagasaki, Japan. Our outbreak investigation included 623 multinational crewmembers onboard on April 20. Median age was 31 years; 84% were men. Each crewmember was isolated or quarantined in a single room inside the ship, and monitoring of health status was supported by a remote health monitoring system. Crewmembers with more severe illness were hospitalized. The investigation found that the outbreak started in late March and peaked in late April, resulting in 149 laboratory-confirmed and 107 probable cases of infection with severe acute respiratory syndrome coronavirus 2. Six case-patients were hospitalized for COVID-19 pneumonia, including 1 in severe condition and 2 who required oxygen administration, but no deaths occurred. Although the virus can spread rapidly on a cruise ship, we describe how prompt isolation and quarantine combined with a sensitive syndromic surveillance system can control a COVID-19 outbreak.
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) was first reported from Wuhan, China (1), and led to outbreaks of coronavirus disease (COVID-19), which was declared a pandemic by the World Health Organization on March 11, 2020. COVID-19 also has been affecting global economies, leading to several recessions (2). Japan experienced an outbreak of COVID-19 on the cruise ship Diamond Princess during the early stages of the epidemic in February 2020 (3–5). The government of Japan prohibited entry into the country at the end of March, declaring a state of emergency in 7 prefectures on April 7, which became a nationwide policy on April 16. Against this backdrop, the Italian cruise ship Costa Atlantica had remained docked at Nagasaki City since January 2020 for full maintenance. In April 2020, we identified an outbreak of COVID-19 on this cruise ship.
COVID-19 spreads easily on cruise ships because of the “3 Cs”: crowded places, close-contact settings, and confined and enclosed spaces (6–9). Given the specialized setting of a cruise ship and its closed population, a cruise ship can offer important insights about infectious disease epidemiology and transmission dynamics (10). How to manage an outbreak of COVID-19 on a cruise ship is a matter of debate, especially in a resource-limited situation. To improve our understanding of COVID-19 and prepare for outbreaks to come, studies of outbreaks on cruise ships are valuable. In this article we describe the epidemiology of the COVID-19 outbreak on Costa Atlantica and approaches taken for managing and responding to this outbreak.
Setting
On April 19, 2020, officials of Costa Atlantica, which had been docked in Nagasaki City since January 2020, reported to Nagasaki City Public Health Center that they had febrile crewmembers (11,12). No passengers were on board the ship. All 623 crewmembers had already completed their quarantine upon entry in Japan, but they had been asked to refrain from leaving the ship unless necessary as part of the public health policy to prevent the spread of COVID-19. Because of cruise ship employment contracts, 56 crewmembers embarked during March 14–April 3. Given the COVID-19 pandemic, the body temperature of all crewmembers had been checked daily since the end of February. Beginning March 22, at the discretion of the cruise ship company, any crewmember with a body temperature >37.1°C was to be isolated in a single-passenger cabin room of the ship; beginning April 19, every nonessential worker was isolated or quarantined in a single-passenger cabin room. Essential workers were defined as crewmembers who were involved in the operation of the ship or in maintaining its operation and functionality, such as the captain, engineers, and food preparation staff.
On April 20, we performed PCR assays for SARS-CoV-2 for 4 crewmembers who had a body temperature >37.1°C, resulting in 1 positive result. During April 21–25, all crewmembers underwent universal screening for infection by using loop-mediated isothermal amplification (LAMP) for SARS-CoV-2. After the universal screening, each nonessential worker remained isolated or quarantined in a single passenger cabin room. Even for those whose test results were positive, crewmembers with mild illness or without signs or symptoms remained on the ship, and the health status of all crewmembers was monitored daily. If clinically indicated, regardless of test results, ill persons were transported and admitted to hospitals in Nagasaki City at the discretion of the ship’s medical doctor.
Data Collection and Definitions
The study population included 623 crewmembers who were on board on April 20, 2020. The cruise ship company provided demographic and body temperature data (ship’s medical record) during March 14–May 27 for all crewmembers on board. Demographic data included sex, date of birth, nationality, and occupation category. Before disembarkation from the ship, crewmembers also provided information regarding their smoking history, presence of any underlying disease, height and weight, daily body temperature, and clinical signs or symptoms during April 28–May 29 by using a smartphone-based remote health monitoring system (13). Obesity, as a risk factor for severe COVID-19, was defined as a body mass index (BMI) >30 (14,15). Clinical signs and symptoms of COVID-19 were fever (body temperature >37.5°C), cough, shortness of breath, nasal congestion, sore throat, nausea or vomiting, conjunctival congestion, headache, fatigue, myalgia or arthralgia, diarrhea, olfactory dysfunction, and taste disorder (loss of taste), which are globally recognized COVID-19 signs and symptoms (1,13,16–18). In managing this outbreak, the threshold value of a body temperature >37.1°C was applied on the basis of the cruise ship’s definition for illness and criteria for isolation precaution.
We defined laboratory-confirmed cases as illness in anyone with a positive test result for SARS-CoV-2 by PCR or LAMP. We defined a probable case was defined as illness in anyone with signs or symptoms indicative of COVID-19 but with a negative test result (19). We divided the severity of COVID-19 into 4 groups (20): severe pneumonia that required intubation or intensive care unit admission, moderate pneumonia that required oxygen administration, mild illness with COVID-19 signs or symptoms that did not require oxygen administration, and an asymptomatic condition without any clinical signs or symptoms. We performed chest radiographs or chest computed tomography scans only for those suspected of having pneumonia, such as prolonged fever or shortness of breath, and those who were hospitalized.
Testing Strategy
We confirmed SARS-CoV-2 infection by using PCR or LAMP. We conducted PCR according to the protocol recommended by Japan’s National Institute of Infectious Diseases (21). LAMP is used for the detection of SARS-CoV-2 because of its fast turnaround time and acceptable levels of sensitivity and specificity (22–24). LAMP was conducted at the Institute of Tropical Medicine at Nagasaki University and Nagasaki University Hospital. Persons who tested positive were allowed to disembark and travel back to their countries after negative test results were confirmed in subsequent tests and their signs or symptoms had resolved.
Data Analysis
We constructed an epidemic curve on the basis of illness onset date, which was based on a body temperature >37.1°C according to the ship’s medical record or the smartphone-based health monitoring system; the onset date of body temperature >37.1°C was defined as the date when body temperature was >37.1°C with a body temperature <37.1°C until the previous day. For the epidemic curve, we used body temperature >37.1°C for 2 reasons: first, it was the cruise ship’s definition for illness and criteria for isolation precaution; second, describing the epidemic curve based on the test results of SARS-CoV-2 from the universal screening would not give an accurate picture of this outbreak because screening was introduced ≈1 month after the beginning of the outbreak and would only detect infections prevalent at the time of screening.
In addition to monitoring such incident events, we monitored the daily prevalent numbers of crewmembers with a body temperature >37.1°C or signs or symptoms. To evaluate the spatial distribution of infection, we plotted on the ship’s map the cabin rooms of crewmembers with a body temperature >37.1°C before isolation. We noted the demographic characteristics of all crewmembers according to their test results and presence of signs or symptoms. We calculated attack rates for both laboratory-confirmed case-patients (laboratory-confirmed case-patients divided by all crewmembers) and with the addition of probable case-patients (laboratory-confirmed case-patients and probable case-patients divided by all crewmembers). We also plotted the clinical course of symptomatic crewmembers individually by calendar date.
We expressed continuous variables as medians and interquartile ranges (IQRs). We summarized categoric variables as numbers and proportions. We conducted statistical analyses by using Stata 16 (StataCorp, https://www.stata.com).
Ethics
The governments of Nagasaki City and Nagasaki Prefecture conducted the surveillance of the COVID-19 outbreak on this cruise ship during April 20–May 29, 2020, under authorization by the Infectious Diseases Control Law. This study was approved by the Institutional Review Board at the Institute of Tropical Medicine at Nagasaki University (approval no. 200619242).
Demographic Characteristics of the Crewmembers
Among the 623 crewmembers, the median age was 31 years (IQR 26–40 years), and 84% (523/623) were men (Table 1). Thirty-six nations were represented by the crewmembers, including (in descending order) the Philippines, India, Indonesia, and China; most (80%) crewmembers were from countries in Asia. Characteristic data were available for 593 crewmembers. Of those, 25% (148/592) had a history of smoking, and 3.7% (22/593) had underlying diseases, including hypertension (2.0% [12/592]), diabetes (1.7% [10/592]), cardiovascular disease (0.2% [1/592]), and asthma (0.2% [1/592]). Median BMI was 24.1 (IQR 21.7–26.7), and 9.4% (49/523) crewmembers had obesity (BMI >30).
Overview of the COVID-19 Outbreak on the Cruise Ship
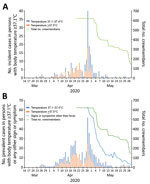
A body temperature >37.1°C was first detected in a crewmember on March 22, and afterwards, 5 other crewmembers had a body temperature >37.1°C during March 24–27 (Figure 1, panel A). Their crew cabin rooms were not concentrated in a single area on the ship (Figure 2, panel A). However, all of these crew members belonged to the entertainment occupation group that boarded the cruise ship from several countries in Europe on March 18 and 19 (Appendix Figure 1). On April 2, another crewmember had a body temperature >37.1°C, and the number of persons with incident fever increased and peaked on April 28, decreasing thereafter (Figure 1, panel A). During March 22–May 29, a total of 211 (34%) had a body temperature >37.1°C. One crewmember who had a body temperature >37.1°C associated with cellulitis was excluded. Apart from the first wave of persons with a body temperature >37.1°C in late March, SARS-CoV-2 infection was distributed similarly across sex, and age group, nationality, and occupation type (Appendix Figure 1). The crew cabin rooms of crewmembers who had a body temperature >37.1°C also were widely distributed throughout the ship (Figure 2, panel B). No information on the ventilation system on the cruise ship was available. We compiled the daily number of crewmembers with a body temperature >37.1°C or with signs or symptoms; a peak occurred on April 28, after which the number gradually decreased until the end of May (Figure 1, panel B).
Among all 623 crewmembers, 149 cases were laboratory-confirmed and 107 probable case-patients who tested negative had clinical signs or symptoms indicative of COVID-19. Restricted to laboratory-confirmed cases, the attack rate for infection was 24%. When probable cases were included, the attack rate was 41%.
Outbreak Control Measures and Management of Disembarkation
An emergency operations center was established in the prefecture office, and an onsite field response center was set up in the harbor near the cruise ship (12). Company staff stayed on board to communicate with both the ship and the public health authorities, and company staff introduced interventions to the ship. Online meetings among company staff on board, the onsite field response center, the emergency operations center, and Nagasaki University Hospital took place almost every morning. In the evening, online meeting between Japan’s Ministry of Health, Labour and Welfare and the emergency operations center took place. Through these communication and coordination mechanisms, we were able to share information, make informed decisions jointly, and implement interventions on the cruise ship.
Every nonessential worker had been separately isolated or quarantined in a single passenger cabin room and not allowed to leave his or her room since April 19. Essential workers who tested negative and had no signs or symptoms served meals or collected laundry for nonessential workers. When medically indicated, a nonessential worker was transported out of the room for medical care. To prevent secondary infection, several interventions were taken. Essential workers were provided with guidance and training for infection prevention on April 26. To ensure that the essential workers did not interact directly with isolated or quarantined crewmembers in their rooms, some interventions were put in place, such as distributing an individual thermometer to each crewmember on April 28 and streaming educational videos on COVID-19 infection prevention in the cabin rooms on April 29. To avoid missing the signs of disease progression and to be able to respond to critical patients in a timely manner, a field clinic was established, along with provision of a vehicle equipped with a computed tomography scanner and a medical transportation system. A remote health monitoring system was developed and introduced to support the cruise ship from outside of the ship (17). After the initial universal screening in April, only essential workers and medical personnel were reexamined when a sign or symptom indicative of COVID-19 was noted; reexaminations were limited in this way to prevent potential spread of the infection.
Starting May 3, those crewmembers who tested negative at universal screening were given priority to disembark; the ship’s medical doctor made the decision on the basis of the crewmember’s body temperature and signs or symptoms. Starting May 14, crewmembers who tested positive were able to disembark and travel back to their countries of origin, provided that they had a subsequent negative test result. Through this predisembarkation testing policy, a total of 495 crewmembers were able to disembark and leave Japan. On May 31, the cruise ship set sail for Manila, the Philippines, with the remaining 126 essential workers, none of whom had a positive test result.
Clinical Outcomes
We compiled the clinical outcomes of all crewmembers and their signs or symptoms during their respective observation periods (Table 2). Among all crewmembers, 0.2% (1/623) had severe pneumonia, 0.3% (2/623) had moderate pneumonia, 32% (200/623) had mild illness, and 67% (420/623) had no signs or symptoms. Among crewmembers with laboratory-confirmed cases, 0.7% (1/149) had severe pneumonia, 1.3% (2/149) had moderate pneumonia, 62% (93/149) had mild illness, and 36% (53/149) had no signs or symptoms. Of the 11 crewmembers admitted to a hospital, 6 had COVID-19 pneumonia.
Clinical Course of Crewmembers Who Had Signs or Symptoms
During the observation period, 96 persons with laboratory-confirmed cases and 107 with probable cases experienced signs or symptoms. The median number of symptomatic days among laboratory-confirmed case-patients was 4 days (IQR 1–8 days) (Appendix Table). Among laboratory-confirmed case-patients who were asymptomatic at the time of universal screening, 58 (52%) subsequently experienced signs or symptoms. Among 38% of the symptomatic crewmembers, symptoms were intermittent, or additional COVID-19 signs or symptoms appeared sporadically over time (Appendix Figure 2).
We have described the key findings from the COVID-19 outbreak that occurred on a cruise ship with multinational crewmembers in Nagasaki City during April 20–May 29, 2020. Six crewmembers were hospitalized for COVID-19 pneumonia, 1 of whom had a severe case, but no deaths occurred. Our retrospective investigation revealed that the outbreak likely started in late March, with the infection introduced into this population from the entertainment occupation group that boarded the ship, which then spread widely inside the ship, irrespective of occupational group, nationality, or crew cabin room location, resulting in 149 laboratory-confirmed cases and 107 probable cases. Because transmission of SARS-CoV-2 from presymptomatic or asymptomatic patients is known to occur (25), certain social activities on the ship could have facilitated transmission which ultimately spread throughout the ship. The epidemic curve (Figure 1, panel A) shows that the number of incident case-patients with a body temperature >37.1°C peaked on April 28. The period between the universal implementation of the quarantine policy (April 19) and the peak of onset (April 28) was longer than the expected incubation period (17,26). This fact might be attributable to several reasons. For instance, before receiving training for infection prevention, essential workers might not have been able to sufficiently prevent infection transmission. Because an essential worker who was measuring body temperatures of isolated or quarantined crewmembers tested positive for SARS-CoV-2 on May 3, we speculate that infection could have spread through any interactions during those measurements or through sharing of the thermometers among the isolated or quarantined crewmembers. These factors might have contributed to further transmissions even after quarantine measures were enforced.
Management of the outbreak on Costa Atlantica was different from that observed on the Diamond Princess or other cruise ship outbreaks. The main difference was that the Costa Atlantica had only crewmembers whereas the Diamond Princess had both passengers and crewmembers. On Costa Atlantica, because passenger cabin rooms inside the ship were empty, crewmembers could be isolated or quarantined inside the ship, which was not possible on the Diamond Princess or other cruise ship outbreaks with passengers. For the outbreak on the Diamond Princess, priority testing was given to the high-risk population. Passengers with positive test results for SARS-CoV-2 were transported to medical facilities, and their clinical courses were followed. For those passengers without positive test results, a 14-day health observation period was set before disembarking (27,28). One study suggested the possibility that evacuating all on board early would have prevented many on the Diamond Princess from becoming infected (29). Early evacuation of all crewmembers was thus initially considered in the Costa Atlantica outbreak. However, there were not enough medical facilities or accommodations to isolate or quarantine all crewmembers in the city, and preparing other isolation facilities would have required installing sewage systems and using communal toilets, which could promote transmission, making such options both impractical and of questionable value. Because we regarded the area inside the ship as contaminated, we developed and introduced a health monitoring system (13), aiming to rapidly detect crewmembers requiring medical attention and to minimize the risk for secondary infection, which was an issue on the Diamond Princess (13,30). Debate is ongoing as to how to manage an outbreak of COVID-19 on a cruise ship, but we should take measures that are best suited for the particular context, especially in resource-limited situations.
As for clinical outcomes, we detected 3 crewmembers with moderate to severe pneumonia (2.0% of laboratory-confirmed cases and 1.2% of laboratory-confirmed and probable cases); this proportion was lower than that noted in a previous report in China, in which 14% of case-patients had severe illness and 5% had critical illness (30). However, the population on the Costa Atlantica included only crewmembers, who were considerably younger and healthier by selection (i.e., healthy worker effect).
Among the laboratory-confirmed cases, we determined 36% (42/149) to be in persons who were asymptomatic (25,31). In the Diamond Princess outbreak, the asymptomatic proportion was reported to be 55% (4), but after transfer to medical facilities, ≈20% of asymptomatic subjects had onset of signs or symptoms (32,33). We were able to follow the clinical courses of all laboratory-confirmed case-patients for >20 days, which prevented misclassification of presymptomatic cases as asymptomatic cases. We also obtained detailed clinical information after introducing the health monitoring system, which had a high usage rate, enabling individual crewmembers to report their signs or symptoms easily on a daily basis. These differences resulted in a lower proportion of asymptomatic cases in our study, which we think to be a more valid picture of the COVID-19 severity spectrum.
Of note, we did not repeat LAMP and PCR tests for SARS-CoV-2 for nonessential workers in our testing strategy. The main goal for our outbreak management was to prevent the spread of infection and to rapidly detect those persons who required medical attention (to provide them with appropriate and timely treatment); thus, repeat testing was not considered necessary as long as nonessential workers who were asymptomatic or had mild illness were isolated or quarantined. On the other hand, essential workers were repeatedly tested because of the potential to spread the infection. Before the ship’s departure, 107 probable cases were reported, which accounted for 23% of crewmembers with negative test results. With limited frequency of testing, some interval-censored infections might have been missed, but with a sensitive health monitoring system and an isolation and quarantine policy in place, we believe our operations were justifiable and effective.
Our study’s first limitation is that we might have underestimated the number of laboratory-confirmed cases because most crewmembers were only tested once. Second, the clinical signs or symptoms of the crewmembers before the introduction of the health monitoring system or after disembarkation could not be tracked, meaning additional symptomatic cases might have occurred.
In conclusion, we have described the epidemiology, along with our management approach, of a COVID-19 outbreak on a cruise ship with crewmembers isolated or quarantined inside the ship. Although SARS-CoV-2 can spread rapidly in closed settings, prompt isolation and quarantine and a sensitive surveillance system using a remote health monitoring approach could successfully control a COVID-19 outbreak on a cruise ship and result in timely medical care for affected persons.
Dr. Maeda is a researcher at the Institute of Tropical Medicine at Nagasaki University and the Nagasaki University Graduate School of Biomedical Science. Her primary research interests include infectious disease epidemiology and public health.
Acknowledgments
We thank all team members, including members from Nagasaki University; National Institute of Infectious Diseases; Nagasaki University Hospital; Nagasaki Prefecture Government; Nagasaki City Public Health Center; Northern Nagasaki Public Health Center; Disaster Medical Assistance Team; Ministry of Health, Labour and Welfare; Japan Self-Defense Forces; National Center for Global Health and Medicine; Disaster Psychiatric Assistance Team; Doctors Without Borders; Japan Heart; and Peace Winds Japan. We also thank all staff and crewmembers of Costa Atlantica.
This work was supported by the Nagasaki Prefecture Government.
References
- Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020;395:497–506. DOIPubMedGoogle Scholar
- World Bank. Global economic prospects. pandemic, recession: the global economy in crisis [cited 2021 Apr 28]. https://www.worldbank.org/en/publication/global-economic-prospects
- Expert Taskforce for the COVID-19 Cruise Ship Outbreak. Epidemiology of COVID-19 outbreak on cruise ship quarantined at Yokohama, Japan, February 2020. Emerg Infect Dis. 2020;26:2591–7. DOIPubMedGoogle Scholar
- Ministry of Health. Labour and Welfare. Official report on the cruise ship Diamond Princess, May 1, 2020 [cited 2021 Apr 28]. https://www.mhlw.go.jp/stf/newpage_11146.html
- Yamagishi T, Kamiya H, Kakimoto K, Suzuki M, Wakita T. Descriptive study of COVID-19 outbreak among passengers and crew on Diamond Princess cruise ship, Yokohama Port, Japan, 20 January to 9 February 2020. Euro Surveill. 2020;25:
2000272 . DOIPubMedGoogle Scholar - Furuse Y, Sando E, Tsuchiya N, Miyahara R, Yasuda I, Ko YK, et al. Clusters of coronavirus disease in communities, Japan, January–April 2020. Emerg Infect Dis. 2020;26:2176–9. DOIPubMedGoogle Scholar
- Moriarty LF, Plucinski MM, Marston BJ, Kurbatova EV, Knust B, Murray EL, et al.; CDC Cruise Ship Response Team; California Department of Public Health COVID-19 Team; Solano County COVID-19 Team. California Department of Public Health COVID-19 Team; Solano County COVID-19 Team. Public health responses to COVID-19 outbreaks on cruise ships—worldwide, February–March 2020. MMWR Morb Mortal Wkly Rep. 2020;69:347–52. DOIPubMedGoogle Scholar
- World Health Organization. COVID-19. Avoid the three Cs. 2020 [cited 2021 Apr 28]. https://www.who.int/brunei/news/infographics---english
- Oshitani H; Expert Members of The National COVID-19 Cluster Taskforce at The Ministry of Health, Labour and Welfare, Japan. Cluster-based approach to coronavirus disease 2019 (COVID-19) response in Japan, from February to April 2020. Jpn J Infect Dis. 2020;73:491–3. DOIPubMedGoogle Scholar
- Mallapaty S. What the cruise-ship outbreaks reveal about COVID-19. Nature. 2020;580:18. DOIPubMedGoogle Scholar
- National Institute of Infectious Diseases. Outbreak of novel coronavirus disease (COVID-19) on a cruise ship docked in Nagasaki City: preliminary interim report. 2020 [cited 2021 Apr 28]. https://www.niid.go.jp/niid/en/2019-ncov-e/2484-idsc/9650-covid19-14-200323-e-2.html
- Nagasaki Prefecture. Investigation report on the outbreak of novel coronavirus cluster aboard the cruise ship “Costa Atlantica” 2020 [cited 2021 Apr 20]. https://www.pref.nagasaki.jp/shared/uploads/2021/02/1613627203.pdf
- Sando E, Morimoto K, Narukawa S, Nakata K. COVID-19 outbreak on the Costa Atlantica cruise ship: use of a remote health monitoring system. J Travel Med. 2021;28:taaa163.
- Petrakis D, Margină D, Tsarouhas K, Tekos F, Stan M, Nikitovic D, et al. Obesity ‑ a risk factor for increased COVID‑19 prevalence, severity and lethality (Review). [review]. Mol Med Rep. 2020;22:9–19. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Defining adult overweight and obesity [cited 2021 Apr 28]. https://www.cdc.gov/obesity/adult/defining.html
- Giacomelli A, Pezzati L, Conti F, Bernacchia D, Siano M, Oreni L, et al. Self-reported olfactory and taste disorders in SARS-CoV-2 patients: a cross-sectional study. Clin Infect Dis. 2020;71:889–90. DOIPubMedGoogle Scholar
- Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, et al.; China Medical Treatment Expert Group for Covid-19. Clinical Characteristics of Coronavirus Disease 2019 in China. N Engl J Med. 2020;382:1708–20. DOIPubMedGoogle Scholar
- Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J, et al. Clinical Characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020;323:1061–9. DOIPubMedGoogle Scholar
- European Centre for Disease Prevention and Control. Case definition for coronavirus disease 2019 (COVID-19) [cited 2021 Apr 28]. https://www.ecdc.europa.eu/en/covid-19/surveillance/case-definition
- Ministry of Health. Labour and Welfare. Clinical management of patients with COVID-19. A guide for front-line healthcare workers. Version 2.1 [cited 2021 Apr 28]. https://www.mhlw.go.jp/content/000646531.pdf
- National Institute of Infectious Diseases. Manual for the detection of pathogen 2019-nCoVver.2.6. [cited 2021 Apr 28]. https://www.niid.go.jp/niid/images/lab-manual/2019-nCoV20200319.pdf
- Park G-S, Ku K, Baek S-H, Kim S-J, Kim SI, Kim B-T, et al. Development of reverse transcription loop-mediated isothermal amplification assays targeting severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). J Mol Diagn. 2020;22:729–35. DOIPubMedGoogle Scholar
- Yan C, Cui J, Huang L, Du B, Chen L, Xue G, et al. Rapid and visual detection of 2019 novel coronavirus (SARS-CoV-2) by a reverse transcription loop-mediated isothermal amplification assay. Clin Microbiol Infect. 2020;26:773–9. DOIPubMedGoogle Scholar
- Yoshikawa R, Abe H, Igasaki Y, Negishi S, Goto H, Yasuda J. Development and evaluation of a rapid and simple diagnostic assay for COVID-19 based on loop-mediated isothermal amplification. PLoS Negl Trop Dis. 2020;14:
e0008855 . DOIPubMedGoogle Scholar - Furukawa NW, Brooks JT, Sobel J. Evidence supporting transmission of severe acute respiratory syndrome coronavirus 2 while presymptomatic or asymptomatic. Emerg Infect Dis. 2020;26:e1–6. DOIPubMedGoogle Scholar
- Lauer SA, Grantz KH, Bi Q, Jones FK, Zheng Q, Meredith HR, et al. The incubation period of coronavirus disease 2019 (COVID-19) from publicly reported confirmed cases: estimation and application. Ann Intern Med. 2020;172:577–82. DOIPubMedGoogle Scholar
- Nakazawa E, Ino H, Akabayashi A. Chronology of COVID-19 cases on the Diamond Princess cruise ship and ethical considerations: a report from Japan. Disaster Med Public Health Prep. 2020;14:506–13. DOIPubMedGoogle Scholar
- Takeuchi I. COVID-19 first stage in Japan - how we treat ‘Diamond Princess Cruise Ship’ with 3700 passengers? Acute Med Surg. 2020;7:
e506 . DOIPubMedGoogle Scholar - Rocklöv J, Sjödin H, Wilder-Smith A. COVID-19 outbreak on the Diamond Princess cruise ship: estimating the epidemic potential and effectiveness of public health countermeasures. J Travel Med. 2020;27:taaa030.
- Ministry of Health. Labour and Welfare. To all medical aid workers on board the cruise ship [cited 2021 Apr 28]. https://www.mhlw.go.jp/content/10900000/000596279.pdf
- Bai Y, Yao L, Wei T, Tian F, Jin DY, Chen L, et al. Presumed asymptomatic carrier transmission of COVID-19. JAMA. 2020;323:1406–7. DOIPubMedGoogle Scholar
- Sakurai A, Sasaki T, Kato S, Hayashi M, Tsuzuki SI, Ishihara T, et al. Natural history of asymptomatic SARS-CoV-2 infection. N Engl J Med. 2020;383:885–6. DOIPubMedGoogle Scholar
- Tabata S, Imai K, Kawano S, Ikeda M, Kodama T, Miyoshi K, et al. Clinical characteristics of COVID-19 in 104 people with SARS-CoV-2 infection on the Diamond Princess cruise ship: a retrospective analysis. Lancet Infect Dis. 2020;20:1043–50. DOIPubMedGoogle Scholar
Figures
Tables
Cite This ArticleOriginal Publication Date: August 05, 2021
1These authors contributed equally to this article.
2These authors were co–principal investigators.
Table of Contents – Volume 27, Number 9—September 2021
| EID Search Options |
|---|
|
|
|
|
|
|

Please use the form below to submit correspondence to the authors or contact them at the following address:
Konosuke Morimoto, Department of Respiratory Infections, Institute of Tropical Medicine, Nagasaki University, 1-12-4 Sakamoto, Nagasaki, 852-8523, Japan
Top