Volume 28, Number 10—October 2022
Dispatch
Molecular Detection of Histoplasma capsulatum in Antarctica
Cite This Article
Citation for Media
Abstract
We detected Histoplasma capsulatum in soil and penguin excreta in the Antarctic Peninsula by sequencing after performing species-specific PCR, confirming previous observations that this pathogen occurs more broadly than suspected. This finding highlights the need for surveillance of emerging agents of systemic mycoses and their transmission among regions, animals, and humans in Antarctica.
Histoplasma capsulatum is a dimorphic fungus of the order Onygenales, which can cause systemic mycosis when inhaled (1). The filamentous phase of the fungus usually inhabits environments rich in phosphate and nitrogenous compounds, typically coming primarily from bird or bat droppings. Human intervention and other disturbances to those environments promote dispersion of fungal propagules (spores) in the air, which enables the inhalation of infectious particles (2). This pathogen has a wide variety of hosts in addition to humans, and its close relationship with vertebrates suggests that birds and mammals can play a crucial role in the dispersal of the members of this species complex (3).
Histoplasmosis occurs worldwide; prevalence varies from low in Europe and Oceania to moderate in Africa and South Asia to high in North America, Central America, and South America. Among areas where it is most prevalent, Latin America is the region with the largest number of cases (3).
The genus Histoplasma is composed of multiple genetically distinct clades, which differ in geographic distribution, virulence, and progression of pathology (4). Kasuga et al. (4) evaluated the population genetic diversity of isolates from different countries and continents by using 4 partial protein coding regions and suggested dividing H. capsulatum into 7 phylogenetic species (4). Those results initiated a whole-genome study to evaluate the species complex, proposing 4 genetically different species: H. capsulatum (Panamanian linage), H. mississippiense (NAm1), H. ohiense (NAm2), and H. suramericanum (LAmA) (5).
Antarctica is the most isolated and inhospitable continent on the planet. Over the past 2 decades, however, the intensity of human activity has continued to increase, driven by not just explorers but also scientific researchers, station support personnel, fishers, whalers, and, more recently, tourists. These increased human activities have a substantial effect on all life forms in Antarctica, transporting nonindigenous species to the continent and exporting endemic and autochthones species to other continents, including human, animal and plant pathogenic fungi (6,7). However, pathogenic fungi are rarely explored in the Antarctic setting (8), and their effect on visitors to Antarctica and on the human populations in other continents is underinvestigated. This study describes the molecular detection of H. capsulatum in soil and penguin excreta in the Antarctic Peninsula.
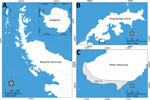
We collected environmental samples in the Potter Peninsula, an Antarctic Special Protected Area located in King George Island, during the summer of 2020 (Figure 1). In total, we collected 9 samples of penguin excreta, 3 samples of fur seal feces, and 8 samples of superficial soil using sterile material and kept them at 2°C–8°C until analysis.
We extracted DNA from the environmental samples and monitored crossover contamination by including 1 sterile water sample at every set (Appendix). We performed nested PCR twice for all samples, using methods specific for the detection and identification of H. capsulatum DNA according to Bialek et al. (9). To check for the presence of PCR inhibitors and to avoid false-negative results, we used H. capsulatum reference strain G217B as positive control. Sequence analysis detected H. capsulatum in 2 of 8 soil samples and in 3 of 9 samples from penguin excreta (Appendix Figure).
We submitted the 5 sequences we detected to GenBank (accession nos. MZ713369–73) and compared them with other H. capsulatum sequences. This comparison generated an identity of >98.56% (100% cover) with the deposited sequences of the 100-kDa-like protein gene from H. capsulatum and 85% similarity with the sequence of a transcription factor of Blastomyces dermatitidis SLH14081 and B. gilchristii SLH14081 (GenBank accession nos. XM_045419905 and XM_002628281.2).
Alignment with GenBank sequences from strains representing the different genetic lineages (Table) demonstrated a difference of up to 14 bp with the 3 haplotypes from Antarctica. The phylogenetic tree formed different groups corresponding to different geographic lineages. Two excreta samples and 1 soil sample grouped with representative strains of the Latin American lineage LAmB1, and 1 soil and 1 excreta sample grouped with a representative strain of LAmA2 lineage. No sample from Antarctica grouped with representative strains of the North America or Panama lineages (Figure 2), indicating a closer association of the newly discovered Histoplasma from Antarctica to the South America lineages.
Moderate temperatures (18°C–28°C), constant humidity (>60%), and a low light environment are thought to characterize suitable ecologic conditions for H. capsulatum growth (10). Despite the average temperature in Antarctica being below that recognized as ideal for the growth of the fungus, the molecular identification of H. capsulatum in 5 of 20 samples collected in Antarctica suggests this species complex could survive at lower temperatures.
Although molecular detection of the fungus does not guarantee its viability, this area of Antarctica is part of an Antarctic Special Protected Area and experiences strong influence of avifauna during the summer period, as well as being host to bird colonies, sea mammal breeding areas, and diverse plant species. Consequently, the soil has high levels of potassium, nitrogen, calcium, and total organic carbon (11), which are good conditions for fungal growth. Ideally, H. capsulatum should be isolated for complete phenotypic and genotypic study, but it is a slow-growth fungus, and its growth is overtaken by fast-growing fungi. Animal inoculation is often used to recover H. capsulatum, but it demands a Biosafety Level 3 facility, which was not available to us.
The molecular detection of H. capsulatum in penguin excreta and ornithogenic soil samples leads us to consider the possibility that the fungus could have been imported from outside the continent by migratory birds. Birds are the only terrestrial vertebrates that share with humans the peculiarity of traveling in a few hours across national and intercontinental borders (12). During migration, birds have the potential to disperse microorganisms that can be dangerous to humans and a threat to animals (13). The fact that high densities of cosmopolitan fungi were found in winter seasonal snow suggests those fungi might be present in air arriving at the Antarctica Peninsula (14). Another possibility could be human intervention in the region. Alien microbes, fungi, plants, and animals have arrived over approximately the previous 2 centuries, coinciding with human activity in Antarctica (6).
The differentiation of the 7 phylogenetic species in the complex could not be performed with the genetic marker used in this study. However, we detected different haplotypes that grouped with some of those geographically distinct phylogenetic species, suggesting dispersion of the fungus on multiple occasions and, perhaps, indicating adaptation on its way to becoming endemic to the Antarctic Peninsula. The detection of H. capsulatum genetically close to representative strains of the Latin American lineages (LAmA2/LAmB1) in Antarctica represents not only the geological history of the continent with South America but the complex dynamics of soil formation and presence of fauna and flora that enable adequate conditions for its maintenance.
This study evaluated a small geographic area of the peninsula, but it has already demonstrated that H. capsulatum occurs more broadly than previously suspected (15). Considering the capacity of the species to cause life-threatening epidemics and the intensifying human presence on the continent, identifying and monitoring fungi in various Antarctic habitats and animals becomes a fundamental strategy for surveilling emerging systemic mycoses and the flow of these agents between regions, animals, and humans.
Mr. Machado Moreira is a PhD student in the postgraduate program in Tropical Medicine at Instituto Oswaldo Cruz, Fiocruz. His primary research interests are polyphasic taxonomy, phylogeny, and diagnosis of invasive fungal infections.
Acknowledgments
This project was partially funded by CNPQ/MCTIC/CAPES/FNDCT Nº 21/2018–PROANTAR (442646/2018-6) and Inova Fiocruz/Fundação Oswaldo Cruz (project no. 4720463444). The funders had no role in study design, data collection and interpretation, or the decision to submit the work for publication.
We are eternally grateful to the late Dr. Bodo Wanke for the opportunity to start this project, for his help on designing the study, and mentoring. He will be missed.
References
- Deepe GS Jr. Outbreaks of histoplasmosis: The spores set sail. PLoS Pathog. 2018;14:
e1007213 . DOIPubMedGoogle Scholar - Teixeira MM, Patané JS, Taylor ML, Gómez BL, Theodoro RC, de Hoog S, et al. Worldwide phylogenetic distributions and population dynamics of the genus Histoplasma. PLoS Negl Trop Dis. 2016;10:
e0004732 . DOIPubMedGoogle Scholar - Kasuga T, White TJ, Koenig G, McEwen J, Restrepo A, Castañeda E, et al. Phylogeography of the fungal pathogen Histoplasma capsulatum. Mol Ecol. 2003;12:3383–401. DOIPubMedGoogle Scholar
- Sepúlveda VE, Márquez R, Turissini DA, Goldman WE, Matute DR. Genome sequences reveal cryptic speciation in the human pathogen Histoplasma capsulatum. MBio. 2017;8:8. DOIPubMedGoogle Scholar
- Frenot Y, Chown SL, Whinam J, Selkirk PM, Convey P, Skotnicki M, et al. Biological invasions in the Antarctic: extent, impacts and implications. Biol Rev Camb Philos Soc. 2005;80:45–72. DOIPubMedGoogle Scholar
- Tin T, Fleming ZL, Hughes KA, Ainley DG, Convey P, Moreno CA, et al. Impacts of local human activities on the Antarctic environment. Antarct Sci. 2009;21:3–33. DOIGoogle Scholar
- de Sousa JRP, Gonçalves VN, de Holanda RA, Santos DA, Bueloni CFLG, Costa AO, et al. Pathogenic potential of environmental resident fungi from ornithogenic soils of Antarctica. Fungal Biol. 2017;121:991–1000. DOIPubMedGoogle Scholar
- Bialek R, Feucht A, Aepinus C, Just-Nübling G, Robertson VJ, Knobloch J, et al. Evaluation of two nested PCR assays for detection of Histoplasma capsulatum DNA in human tissue. J Clin Microbiol. 2002;40:1644–7. DOIPubMedGoogle Scholar
- Kwon-Chung KJ, Bennett JE. Medical mycology. 2nd ed. Philadelphia: Lea & Febiger; 1992.
- Poelking EL. Solos, ambiente e dinâmica climática da camada na Península Potter, Antártica Marítima [dissertation]. Viçosa, Brazil: Federal University of Viçosa; 1978.
- Jourdain E, Gauthier-Clerc M, Bicout DJ, Sabatier P. Bird migration routes and risk for pathogen dispersion into western Mediterranean wetlands. Emerg Infect Dis. 2007;13:365–72. DOIPubMedGoogle Scholar
- Reed KD, Meece JK, Henkel JS, Shukla SK. Birds, migration and emerging zoonoses: west nile virus, lyme disease, influenza A and enteropathogens. Clin Med Res. 2003;1:5–12. DOIPubMedGoogle Scholar
- de Menezes GCA, Amorim SS, Gonçalves VN, Godinho VM, Simões JC, Rosa CA, et al. Diversity, distribution, and ecology of fungi in the seasonal snow of Antarctica. Microorganisms. 2019;7:445. DOIPubMedGoogle Scholar
- Ashraf N, Kubat RC, Poplin V, Adenis AA, Denning DW, Wright L, et al. Re-drawing the maps for endemic mycoses. Mycopathologia. 2020;185:843–65. DOIPubMedGoogle Scholar
Figures
Table
Cite This ArticleOriginal Publication Date: September 14, 2022
Table of Contents – Volume 28, Number 10—October 2022
| EID Search Options |
|---|
|
|
|
|
|
|

Please use the form below to submit correspondence to the authors or contact them at the following address:
Luciana Trilles, Instituto Nacional de Infectologia Evandro Chagas–INI/FIOCRUZ, Pavilhão Maria Deane Av. Brasil, 4365, 21040-900 Rio de Janeiro, Brazil
Top