Volume 29, Number 3—March 2023
Dispatch
Risk Factors for Reinfection with SARS-CoV-2 Omicron Variant among Previously Infected Frontline Workers
Cite This Article
Citation for Media
Abstract
In a cohort of essential workers in the United States previously infected with SARS-CoV-2, risk factors for reinfection included being unvaccinated, infrequent mask use, time since first infection, and being non-Hispanic Black. Protecting workers from reinfection requires a multipronged approach including up-to-date vaccination, mask use as recommended, and reduction in underlying health disparities.
Essential and frontline workers experience repeated occupational exposure to SARS-CoV-2 (1). The variant B.1.1.529 (Omicron) is characterized by unprecedented transmissibility and potential for immune evasion, which led to a surge in first-time infections and reinfections in the United States beginning in December 2021 (2). Before Omicron predominance, previous infection had been highly protective against reinfection, but protection waned as Omicron emerged (3–5). Compared with results for pre-Omicron variants, reports of mRNA vaccine effectiveness against first-time Omicron infections were lower (46% after 2 doses and 60% after 3 doses) (6). Early reports on vaccine effectiveness against hospitalization related to reinfection with Omicron demonstrated 35% risk reduction with 2 doses of mRNA vaccine and 68% with 3 doses (6,7).
Little is known about the constellation factors that put persons who had previous infections at risk for reinfection with Omicron (8). In this study, we examined a prospective cohort of essential and frontline workers who had previous SARS-CoV-2 infections to identify risk factors for reinfection during Omicron predominance.
Beginning in July 2020, frontline workers in 8 US locations were enrolled in the Arizona Healthcare, Emergency Response, and Other Essential Workers Study (AZ-HEROES) and the Research on the Epidemiology of SARS-CoV-2 in Essential Response Personnel (RECOVER) Study (9,10). Participants self-collected weekly mid-turbinate nasal specimens regardless of symptoms and upon the date of onset of any COVID-19–like illness symptoms. All specimens were tested at Marshfield Clinical Research Laboratories (Marshfield, WI, USA) for SARS-CoV-2 RNA by reverse transcription PCR (RT-PCR) testing. Specimens positive by RT-PCR with a cycle threshold (Ct) value <30 underwent whole-genome sequencing to determine SARS-CoV-2 variant. (Ct is defined as the number of cycles required for the fluorescent signal to cross the threshold [i.e., exceeds background level].)
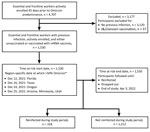
If the specimen was ineligible (Ct >30) for sequencing, the date of incident infection was used to estimate variant predominance by using the state-specific date at which >50% of specimens sequenced were of the Delta or Omicron variants according to Centers for Disease Control and Prevention data (Figure) (11). Only participants who were actively enrolled in the study during site-specific Omicron predominance, and those who had 1 previous infection at least 45 days before Omicron predominance, were included (Figure).
We identified first infections on the basis of participant-reported positive viral test results before enrollment or positive study-based RT-PCR results after enrollment. We defined reinfections as the second incident infection with >90 days between last date of positivity for first infection and first date of positivity for the second infection, or a second infection after 45 days from a distinct SARS-CoV-2 variant. We collected demographic and underlying health information at enrollment. Participants self-reported vaccination at enrollment, quarterly, and more frequently when new vaccines became available; study staff subsequently verified self-reports through vaccine card uploads, state vaccine registries or electronic medical records. We collected exposure variables, including self-reported mask use and number of hours worked per week, monthly and averaged them over the study period (12). All participants provided written consent, and protocols were approved by institutional review boards at all participating sites, including Abt Associates and the Centers for Disease Control and Prevention.
We estimated unadjusted and adjusted hazard ratios for Omicron reinfection with Cox proportional-hazards models by using the Andersen–Gill extension to account for time-varying vaccination status described previously (13). Adjusted models included demographic information, preexisting health conditions, time-varying vaccination status, self-reported mask use in the community, and time since previous infection. All statistical analyses were conducted in R version 4.0.4 (The R Project for Statistical Computing, https://www.r-project.org) and SAS university edition 9.4 (SAS Institute, Inc., https://www.sas.com).
Of 4,707 actively enrolled HEROES-RECOVER participants, 1,587 (33.7%) had a previous SARS-CoV-2 infection >45 days before Omicron predominance. We excluded from the study population persons who had received J&J/Janssen (https://www.jnj.com) vaccination (n = 57) (Figure). From the location-specific date of Omicron predominance through April 3, 2022, a total of 1,530 participants who had previous SARS-CoV-2 infections contributed 124,665 person-days at risk for reinfection (Table). More than half of the participants were from Arizona (59.7%), female (60.5%), and non-Hispanic White (66.9%). In this study sample, 42.5% were healthcare personnel, 26.1% first responders, and 31.4% other essential workers.
Of all mRNA vaccines received, 71.2% were BNT162b2 (Pfizer-BioNTech, https://www.pfizer.com) and 28.8% were mRNA-1273 (Moderna, https://www.modernatx.com). About half (51.0%) of participants experienced their first infection within a year of location-specific Omicron predominance. Reinfections were identified among 318 (20.8%) participants; 27.0% of those reinfected were asymptomatic.
The proportional hazards assumption was met for all models. Participants who had 2 or 3 doses of mRNA vaccine had lower risk for reinfection with Omicron than persons who were unvaccinated (adjusted HR [aHR] 0.57 [95% CI 0.43–0.75] for those with 2 doses; aHR 0.54 [95% CI 0.39–0.75] for those with 3 doses) (Table). Although age and sex did not significantly predict reinfection in this sample, residence in Utah (aHR 1.61, 95% CI 1.09–2.37; referent Tucson, AZ, USA) and self-identification as non-Hispanic Black (aHR 2.14, 95% CI 1.17–3.92; referent non-Hispanic White) were risk factors for reinfection. Participants who wore masks in community settings less frequently, defined as wearing less than the mean reported percentage of time of 47% (interquartile range 8%–83%), had higher risk for reinfection (aHR 1.39, 95% CI 1.07–1.82). Finally, participants for whom >1 year had elapsed since their first infection had increased risk for reinfection compared with persons who had <1 year since their first infection (aHR 1.63, 95% CI 1.28–2.07).
In this prospective cohort of previously infected frontline workers, mRNA vaccination with 2 or 3 doses reduced the risk for reinfection by >40%. Risk for reinfection was increased by low self-reported mask use and for persons who had an initial infection >1 year before the study period. Those findings are consistent with risk factor studies for primary infections and suggest that infection-induced immunity wanes over time (12,14). Given that 27% of reinfections were asymptomatic, our findings suggest that vaccination might have been protective against infections that workers would have acquired unknowingly. Non-Hispanic Black participants had increased risk for reinfection, which underscores the need for addressing health disparities, especially because racial and ethnic minority groups are overrepresented among essential and frontline workers (15).
The first limitation of this study is that sparse data contributed from certain geographic sites and demographic groups reduced the precision of estimates. Second, it is possible that some persons who were reinfected during the early phases of Omicron predominance (when Omicron and Delta were co-circulating) and who also had high Ct values that precluded whole-genome sequencing were misclassified as Omicron reinfections (instead of Delta), although that number is probably negligible, given the rapid acceleration of Omicron dominance. Third, although inclusion of self-reported mask use in community settings was a strength of the study, we were unable to account for venue-specific mask mandates, which might have been variable among participants or changed throughout the study period. Fourth, findings suggesting the need for second and third doses of mRNA vaccines are less relevant as recommendations for additional and variant-specific boosters emerge. Nonetheless, those findings suggest the role of time since immune-modifying events, including most recent mRNA vaccination or previous infection, in reducing risk for reinfection. Overall, our findings underscore the need for maintaining a multipronged approach, including vaccines, nonpharmaceutical interventions, and efforts to reduce disparities, to protect frontline workers as the pandemic enters a period in which reinfections are increasingly common.
Dr. Ellingson is an associate professor of epidemiology at the Mel and Enid Zuckerman College of Public Health at the University of Arizona, Tucson, AZ. Her primary research interest is infectious diseases in high-risk occupational and congregate settings.
Acknowledgments
On behalf of HEROES-RECOVER Network, we thank the cohort participants and the following collaborators: Eduardo Azziz-Baumgartner, Melissa L. Arvay, William Brannen, Stephanie Bialek, Allison Ciesla, Alicia M. Fry, Aron Hall, Adam MacNeil, Clifford McDonald, Sue Reynolds, Robert Slaughter, Matthew J. Stuckey, Rose Wang, Ryan Wiegand, CDC; Danielle R. Hunt, Laura J. Edwards, Robin Bloodworth, Claire Douglas, Jazmin Duque, Jini Etolue, Deanna E. Fleary, Jessica Flores, Isaiah Gerber, Kimberly Groover, Louise Hadden, Jenna Harder, Nancy McGarry, Peenaz Mistry, Tyler C. Morrill, Kelly Patlan, Brandon P. Poe, Khaila Prather, Meghan Shea, John Thacker, Pearl Zheng, Abt Associates; Kayan Dunnigan, Spencer Rose, Nicole Calhoun, Leah Odame-Bamfo, Clare Mathenge, Michael E. Smith, Kempapura Murthy, Tnelda Zunie, Eric Hoffman, Martha Zayed, Ashley Graves, Joel Blais, Jason Ettlinger, Sharla Russell, Natalie Settele, Tiya Searcy, Rupande Patel, Elisa Priest, Jennifer Thomas, Muralidhar Jatla, Madhava Beeram, Javed Butler, Alejandro Arroliga, Baylor Scott and White Health; Holly Groom, Yolanda Prado, Daniel Sapp, Mi Lee, Chris Eddy, Matt Hornbrook, Donna Eubanks, Danielle Millay, Dorothy Kurdyla, Kristin Bialobok, Ambrosia Bass, Kristi Bays, Kimberly Berame, Cathleen Bourdoin, Rashyra Brent, Carlea Buslach, Lantoria Davis, Stephen Fortmann, Jennifer Gluth, Kenni Graham, Tarika Holness, Kelley Jewell, Enedina Luis, Abreeanah Magdaleno, DeShaun Martin, Joyce Smith-McGee, Martha Perley, Sam Peterson, Aaron Peipert, Krystil Phillips, Joanna Price, Ana Reyes, Sperry Robinson, Katrina Schell, Emily Schield, Natosha Shirley, Anna Shivinsky, Valencia Smith, Britta Torgrimson-Ojerio, Brooke Wainwright, Shawn Westaway, Kaiser Permanente NW; Saydee Benz, Adam Bissonnette, Krystal Boese, Emily Botten, Jarod Boyer, Michaela Braun, Julianne Carlson, Caleb Cravillion, Amber Donnerbauer, Tim Dziedzic, Joe Eddy, Heather Edgren, Alex Ermeling, Kelsey Ewert, Connie Fehrenbach, Rachel Fernandez, Wayne Frome, Sherri Guzinski, Mitch Hertel, Garrett Heuer, Erin Higdon, Cressa Huotari, Lynn Ivacic, Lee Jepsen, Steve Kaiser, Bailey Keffer, Tammy Koepel, Sarah Kohn, Alaura Lemieux, Carrie Marcis, Megan Maronde, Isaac McCready, Nidhi Mehta, Dan Miesbauer, Collin Nikolai, Brooke Olson, Jeremy Olstadt, Lisa Ott, Cory Pike, Nicole Price, Chris Reardon, Alex Slenczka, Elisha Stefanski, Lydia Sterzinger, Kendra Stoltz, Melissa Strupp, Lyndsay Watkins, Roxann Weigel, Ben Zimmerman, Marshfield Clinic Research Laboratory; Damena Gallimore-Wilson, Roger Noriega, Cynthia Beaver, Alexandra Cruz, Annabel Reyes, Brigitte Madan, Addison Testoff, John Jones, University of Miami; Jennifer Viergutz, Angela Hunt, Jessica Lundgren, Tyna O’Connor, Daniel Stafki, Jill Dolezilek, Bethany Brunner, Leiah Hoffman, Kate Diluzio O’Connor, Daniel Stafki, Jill Dolezilek, Bethany Brunner, Leiah Hoffman, Kate Diluzio, St. Luke’s; Ariyah Armstrong, Nora Baccam, Shawn Beitel, Tatum Butcher, Shelby Capell, Andrea Carmona, Karysa Carson, Alissa Coleman, Hannah Cowling, Carly Deal, Kiara Earley, Sophie Evans, Julia Fisher, Ashlyn Flangos, Joe K. Gerald, Lynn Gerald, Anna Giudici, Erika Goebert, Taylor Graham, Sofia Grijalva, Hanna Hanson, Olivia Healy, Chloe Hendrix, Katherine Herder, Adrianna Hernandez, Raven Hilyard, Rezwana Islam, Caroline Klinck, Karl Krupp, Karla Ledezma, Sally Littau, Amelia Lobos, Jeremy Makar, Natalya Mayhew, Kristisha Mevises, Cierra Morris, Sarah Murray, Janko Nikolich-Žugich, Assumpta Nsengiyunva, Kennedy Obrien, Mya Pena, Riley Perlman, Celia Pikowski, Ferris A. Ramadan, Jen Scott, Priyanka Sharma, Alison Slocum, Saskia Smidt, Lili Steffen, Jayla Sowell, Danielle Stea, Xiaoxiao Sun, Nicholas Tang, Gianna Taylor, Ta’Nya Tomas, Heena Timsina, Italia Trejo, April Yingst, University of Arizona; Rachel T. Brown, Camie Schaefer, Arlyne Arteaga, Matthew Bruner, Daniel Dawson, Emilee Eden, Jenna Praggastis, Joseph Stanford, Jeanmarie Mayer, Marcus Stucki, Riley Campbell, Kathy Tran, Madeleine Smith, Braydon Black, Christina Pick, Madison Tallman, Chapman Cox, Derrick Wong, Michael Langston, Adriele Fugal, Fiona Tsang, Maya Wheeler, Gretchen Maughan, Megan Wilson, Pasha Stinson, Jesse Williams, Seon Reed, Jinyi Mao, Nikki Gallacher, Kendal Chatard, Jenna Vo, Katie Luong, Ryder Jordin, Grace Stewart, Brock Bourdelle, Timina Powaukee, Max Minoughan, University of Utah. The Florida research team thanks the firefighters, healthcare workers, and frontline and essential workers for participating in this occupational cohort study.
This study was supported by the National Center for Immunization and Respiratory Diseases, Centers for Disease Control and Prevention under contract numbers 75D30120R68013 awarded to the Marshfield Clinic Research Laboratory and 75D30120C08379 to the University of Arizona.
ALN reports receiving support from Pfizer and Vir Biotechnology for unrelated studies.
References
- Michaels D, Wagner GR. Occupational Safety and Health Administration (OSHA) and worker safety during the COVID-19 pandemic. JAMA. 2020;324:1389–90. DOIPubMedGoogle Scholar
- Pulliam JRC, van Schalkwyk C, Govender N, von Gottberg A, Cohen C, Groome MJ, et al. Increased risk of SARS-CoV-2 reinfection associated with emergence of Omicron in South Africa. Science. 2022;376:
eabn4947 . DOIPubMedGoogle Scholar - Altarawneh HN, Chemaitelly H, Hasan MR, Ayoub HH, Qassim S, AlMukdad S, et al. Protection against the Omicron variant from previous SARS-CoV-2 infection. N Engl J Med. 2022;386:1288–90. DOIPubMedGoogle Scholar
- Hall VG, Al-Alahmadi G, Solera JT, Marinelli T, Cardinal H, Prasad GVR, et al. Outcomes of SARS-CoV-2 infection in unvaccinated compared with vaccinated solid organ transplant recipients: a propensity matched cohort study. Transplantation. 2022;106:1622–8. DOIPubMedGoogle Scholar
- Hansen CH, Michlmayr D, Gubbels SM, Mølbak K, Ethelberg S. Assessment of protection against reinfection with SARS-CoV-2 among 4 million PCR-tested individuals in Denmark in 2020: a population-level observational study. Lancet. 2021;397:1204–12. DOIPubMedGoogle Scholar
- Yoon SK, Hegmann KT, Thiese MS, Burgess JL, Ellingson K, Lutrick K, et al.; HEROES-RECOVER Network Investigators; HEROES-RECOVER Network Investigators. HEROES-RECOVER Network Investigators. Protection with a third dose of mRNA vaccine against SARS-CoV-2 variants in frontline workers. N Engl J Med. 2022;386:1855–7. DOIPubMedGoogle Scholar
- Plumb ID, Feldstein LR, Barkley E, Posner AB, Bregman HS, Hagen MB, et al. Effectiveness of COVID-19 mRNA vaccination in preventing COVID-19-associated hospitalization among adults with previous SARS-CoV-2 infection—United States, June 2021‒February 2022. MMWR Morb Mortal Wkly Rep. 2022;71:549–55. DOIPubMedGoogle Scholar
- Helfand M, Fiordalisi C, Wiedrick J, Ramsey KL, Armstrong C, Gean E, et al. Risk for reinfection after SARS-CoV-2: a living, rapid review for American College of Physicians practice points on the role of the antibody response in conferring immunity following SARS-CoV-2 infection. Ann Intern Med. 2022;175:547–55. DOIPubMedGoogle Scholar
- Edwards LJ, Fowlkes AL, Wesley MG, Kuntz JL, Odean MJ, Caban-Martinez AJ, et al. Research on the epidemiology of SARS-CoV-2 in essential response personnel (RECOVER): protocol for a multisite longitudinal cohort study. JMIR Res Protoc. 2021;10:
e31574 . DOIPubMedGoogle Scholar - Lutrick K, Ellingson KD, Baccam Z, Rivers P, Beitel S, Parker J, et al. COVID-19 infection, reinfection, and vaccine effectiveness in a prospective cohort of Arizona frontline/essential workers: the AZ HEROES research protocol. JMIR Res Protoc. 2021;10:
e28925 . DOIPubMedGoogle Scholar - Centers for Disease Control and Prevention. COVID data tracker: variant proportions [cited 2022 Dec 28]. https://covid.cdc.gov/covid-data-tracker/#variant-proportions
- Naleway AL, Grant L, Caban-Martinez AJ, Wesley MG, Burgess JL, Groover K, et al. Incidence of SARS-CoV-2 infection among COVID-19 vaccinated and unvaccinated healthcare personnel, first responders, and other essential and frontline workers: Eight US locations, January-September 2021. Influenza Other Respir Viruses. 2022;16:585–93. DOIPubMedGoogle Scholar
- Thompson MG, Burgess JL, Naleway AL, Tyner H, Yoon SK, Meece J, et al. Prevention and attenuation of COVID-19 with the BNT162b2 and mRNA-1273 vaccines. N Engl J Med. 2021;385:320–9. DOIPubMedGoogle Scholar
- Goldberg Y, Mandel M, Bar-On YM, Bodenheimer O, Freedman LS, Ash N, et al. Protection and waning of natural and hybrid immunity to SARS-CoV-2. N Engl J Med. 2022;386:2201–12. DOIPubMedGoogle Scholar
- Lopez L III, Hart LH III, Katz MH. Racial and ethnic health disparities related to COVID-19. JAMA. 2021;325:719–20. DOIPubMedGoogle Scholar
Figure
Table
Cite This ArticleOriginal Publication Date: January 26, 2023
Table of Contents – Volume 29, Number 3—March 2023
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Katherine D. Ellingson, Department of Epidemiology and Biostatistics, Zuckerman College of Public Health, University of Arizona, Tucson, AZ 85724, USA
Top