Volume 31, Number 11—November 2025
Dispatch
Spiroplasma ixodetis in Ticks Removed from Humans, Sweden and Åland Islands, Finland
Cite This Article
Citation for Media
Abstract
The prevalence of Spiroplasma ixodetis in ticks that have bitten humans in Sweden and in the Åland Islands, Finland, was 2.6%, with observed significant geographic differences between regions. The pathogen was not detected in blood samples from participants bitten by S. ixodetis–positive ticks, indicating low risk for transmission to humans.
Spiroplasma ixodetis, an emerging tickborne bacterium transmitted by Ixodes ricinus ticks, shows a prevalence range of 0.4%–3.0% in questing ticks (1,2) to 13.5% in ticks removed from humans in Europe (3). Human cases of S. ixodetis infection, spiroplasmosis, have been reported from Europe, including Sweden (4,5), in both immunocompetent and immunosuppressed patients; symptoms were more severe in immunosuppressed patients (4,6).
Low awareness, nonspecific symptoms similar to other tickborne infections, and potential co-infection with other tickborne pathogens contribute to misdiagnosis or underdiagnosis (7,8). Because S. ixodetis is an intracellular bacterium, culturing is difficult, and no serologic assays are available; the primary detection tool is PCR. We assessed the risk for human exposure to this pathogen by investigating the prevalence, geographic distribution, and potential coexistence with other tickborne pathogens in feeding ticks removed from humans in Sweden and in the Åland Islands, Finland.
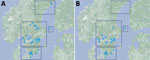
This study is a part of the Tick-Borne Diseases (TBD) STING study, a prospective multicenter study in Sweden and in the Åland Islands, Finland. The study enrolled 2,327 healthy tick-bitten participants (>18 years of age) at primary healthcare centers (PHCs) in 4 geographic regions (9) (Figure) through public advertisements during 2008–2010. The Regional Ethics Review Board in Linköping, Sweden, and the Åland Health Care Ethics Committee approved the study.
We homogenized tick specimens, extracted total nucleic acids, and reverse-transcribed them to cDNA (9) (Appendix). We also extracted DNA from blood plasma collected at inclusion (at the time of the tick bite) and at follow-up 3 months later from participants bitten by a S. ixodetis–positive tick. We detected S. ixodetis in ticks and plasma using a species-specific TaqMan real-time PCR targeting a 170-bp fragment of the RNA polymerase β subunit (10), then performed nucleotide sequencing and verification with BLAST (https://blast.ncbi.nlm.nih.gov/Blast.cgi). We analyzed all S. ixodetis–positive ticks for the presence of nucleic acid from Borrelia burgdorferi sensu lato, B. miyamotoi, tick-borne encephalitis virus, Anaplasma phagocytophilum, Neoehrlichia mikurensis, Babesia spp., and Rickettsia spp. by real-time PCR (11) (Appendix Table 1).
The study consisted of 2,735 I. ricinus ticks: 1,823 nymphs, 689 adults, 118 larvae, and 105 ticks for which we could not determine developmental stage (Table 1). The blood feeding time range was <24 to >72 hours (Appendix Table 2). Most (n = 1,156) ticks were collected in southcentral Sweden, followed by the Åland Islands (n = 950), southernmost Sweden (n = 605), and northern Sweden (n = 24) (Table 2). In total, 72 ticks (2.6%) were positive for S. ixodetis; of those, 60 showed >99.42% sequence identity with S. ixodetis strain sHm (GenBank accession no. AP026933.1). All plasma samples from study participants bitten by a S. ixodetis–containing tick yielded negative PCR results.
We found no statistical differences in the prevalence of S. ixodetis among the different developmental stages of the ticks (Table 1); however, we found a statistically significant difference in geographic distribution of S. ixodetis–positive ticks between southcentral Sweden and southernmost Sweden (p = 0.0004), southcentral Sweden and the Åland Islands (p = 0.00005), and southernmost Sweden and the Åland Islands (p<0.00001). No ticks collected in northern Sweden were positive for S. ixodetis.
In total, 26 (36%) of the S. ixodetis–positive ticks contained >1 additional pathogens, mainly species in the B. burgdorferi s.l. complex (n = 14), of which most were B. afzelii. Coexistence of S. ixodetis and other tickborne pathogens was less common. Fifteen of the ticks with coexisting pathogens were nymphs, and 11 were adult females. Three ticks carried 3 pathogens: S. ixodetis, B. burgdorferi s.l., and N. mikurensis (Appendix Table 2). We found no statistically significant difference between observed frequency (17%) and expected frequency (19%) for coexistence between S. ixodetis and B. burgdorferi s.l. bacteria, suggesting that coexistence does not appear more often than expected by chance based on the prevalences of the individual pathogens (p = 0.738). We found statistically significant differences in geographic distribution of ticks with coexistence, regardless of pathogens, between southcentral Sweden and southernmost Sweden (p = 0.0004), southcentral Sweden and the Åland Islands (p = 0.04), and southernmost Sweden and the Åland Islands (p<0.00001).
The overall prevalence of S. ixodetis in I. ricinus ticks removed from humans was 2.6%, with statistically significant differences in distribution between geographic areas. S. ixodetis–positive ticks were found in all developmental stages, including larvae, suggesting transovarial transmission of the bacterium. The prevalence in our study is consistent to previous studies showing a prevalence of 0.4%–3% in questing ticks (1,2). The number of ticks analyzed from northern Sweden was low, which can explain the negative results in this area. However, because of climate changes and raised temperatures, more suitable habitats for ticks and hosts might result in the spread of S. ixodetis–infected ticks into new areas (12). Few S. ixodetis–positive ticks were detected in the Åland Islands, an area with high tick density, highly endemic for B. burgdorferi s.l. and tick-borne encephalitis virus (9,13). That finding indicates that endemic areas for one pathogen may not be endemic for others.
The negative PCR results in plasma from participants who did not necessarily show symptoms related to tickborne diseases were consistent with a previous study (3). In that study, patients with influenza-like symptoms and erythema migrans also showed negative results in blood after being bitten by a tick carrying S. ixodetis. Even though S. ixodetis bacteria have been detected in blood (4), knowledge of the optimal time of sampling or the frequency of the pathogen in blood is limited. The inclusion sample was collected only days after the tick bite, perhaps before a potential bacteremia, and the follow-up sample was collected 3 months after a potential acute infection, which may be the reason for the negative outcome. No time lag for transmission has been established as of November 2025; because S. ixodetis is located in the midgut of the tick, we hypothesize that the time lag could be similar to that of Borrelia spp. transmission, 24–48 hours (9).
Most of the ticks carrying >1 pathogen contained both S. ixodetis and B. burgdorferi s.l. bacteria. That finding was not surprising because Borrelia spp. bacteria, mainly B. afzelii, are the most common pathogens found in questing ticks in Europe (14).
Our study used samples collected >15 years ago; although our findings might not reflect the current situation, they provide relevant epidemiologic insights into the prevalence and geographic distribution of S. ixodetis. Although we were unable to sequence all S. ixodetis–positive ticks, mainly because of high cycle threshold values (>35), we believe the real-time PCR findings are trustworthy because primers and probe are designed for species-specific detection.
Further studies are needed to expand our understanding of prevalence, geographic distribution, and the possibility of co-infection of tickborne S. ixodetis. Our results indicate low risk of being infected by S. ixodetis after a tick bite; however, spiroplasmosis and co-infections should be considered as differential diagnoses in cases of fever after a tick bite (4,8).
Dr. Lager has a PhD in diagnostics of tickborne diseases at Linköping University. Her research interests concern molecular analyses of ticks, molecular and serological diagnostics of tickborne diseases on human samples, and the development of new molecular methods.
Acknowledgments
We thank all participants and co-workers in the Tick-Borne Diseases STING study. We especially thank Victor Bäckman and Emil Ilvered for excellent laboratory work in analyzing the potential coexistence of multiple pathogens in the ticks.
This study was supported by the Medical Research Council of Southeast Sweden (grant nos. 994295 and 1994196); the Division of Laboratory Medicine, Region Jönköping County; and the Foundation for Medical Research of the Åland Cultural Foundation.
References
- Olsthoorn F, Sprong H, Fonville M, Rocchi M, Medlock J, Gilbert L, et al. Occurrence of tick-borne pathogens in questing Ixodes ricinus ticks from Wester Ross, Northwest Scotland. Parasit Vectors. 2021;14:430.PubMedGoogle Scholar
- Subramanian G, Sekeyova Z, Raoult D, Mediannikov O. Multiple tick-associated bacteria in Ixodes ricinus from Slovakia. Ticks Tick Borne Dis. 2012;3:406–10.PubMedGoogle Scholar
- Geebelen L, Lernout T, Tersago K, Terryn S, Hovius JW, Docters van Leeuwen A, et al. No molecular detection of tick-borne pathogens in the blood of patients with erythema migrans in Belgium. Parasit Vectors. 2022;15:27.PubMedGoogle Scholar
- Eimer J, Fernström L, Rohlén L, Grankvist A, Loo K, Nyman E, et al. Spiroplasma ixodetis infections in immunocompetent and immunosuppressed patients after tick exposure, Sweden. Emerg Infect Dis. 2022;28:1681–5.PubMedGoogle Scholar
- Matet A, Le Flèche-Matéos A, Doz F, Dureau P, Cassoux N. Ocular Spiroplasma ixodetis in newborns, France. Emerg Infect Dis. 2020;26:340–4.PubMedGoogle Scholar
- Aquilino A, Masiá M, López P, Galiana AJ, Tovar J, Andrés M, et al. First human systemic infection caused by Spiroplasma. J Clin Microbiol. 2015;53:719–21.PubMedGoogle Scholar
- Lernout T, De Regge N, Tersago K, Fonville M, Suin V, Sprong H. Prevalence of pathogens in ticks collected from humans through citizen science in Belgium. Parasit Vectors. 2019;12:550.PubMedGoogle Scholar
- Madison-Antenucci S, Kramer LD, Gebhardt LL, Kauffman E. Emerging tick-borne diseases. Clin Microbiol Rev. 2020;33:e00083–18.PubMedGoogle Scholar
- Wilhelmsson P, Lindblom P, Fryland L, Ernerudh J, Forsberg P, Lindgren PE. Prevalence, diversity, and load of Borrelia species in ticks that have fed on humans in regions of Sweden and Åland Islands, Finland with different Lyme borreliosis incidences. PLoS One. 2013;8:
e81433 .PubMedGoogle Scholar - Krawczyk AI, Van Duijvendijk GL, Swart A, Heylen D, Jaarsma RI, Jacobs FH, et al. Effect of rodent density on tick and tick-borne pathogen populations: consequences for infectious disease risk. Parasit Vectors. 2020;13:1–17.PubMedGoogle Scholar
- Gyllemark P, Wilhelmsson P, Elm C, Hoornstra D, Hovius JW, Johansson M, et al. Are other tick-borne infections overlooked in patients investigated for Lyme neuroborreliosis? A large retrospective study from South-eastern Sweden. Ticks Tick Borne Dis. 2021;12:
101759 .PubMedGoogle Scholar - Jaenson TG, Jaenson DG, Eisen L, Petersson E, Lindgren E. Changes in the geographical distribution and abundance of the tick Ixodes ricinus during the past 30 years in Sweden. Parasit Vectors. 2012;5:8.PubMedGoogle Scholar
- Carlströmer Berthén N, Tompa E, Olausson S, Nyberg C, Nyman D, Ringbom M, et al. The AxBioTick study: Borrelia species and tick-borne encephalitis virus in ticks, and clinical responses in tick-bitten individuals on the Aland Islands, Finland. Microorganisms. 2023;11:1100.PubMedGoogle Scholar
- Strnad M, Hönig V, Růžek D, Grubhoffer L, Rego ROM. Europe-wide meta-analysis of Borrelia burgdorferi sensu lato prevalence in questing Ixodes ricinus ticks. Appl Environ Microbiol. 2017;83:e00609–17.PubMedGoogle Scholar
Figure
Tables
Cite This ArticleOriginal Publication Date: December 04, 2025
Table of Contents – Volume 31, Number 11—November 2025
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Malin Lager (née Christiansson), Laboratory Medicine, Department of Clinical Microbiology, Ryhov County Hospital, SE-551 85 Jönköping, Sweden
Top