Volume 32, Number 4—April 2026
Research
Dengue Incidence, Seroprevalence, and Expansion Factors from Active Surveillance, Brazil, 2016–2021
Cite This Article
Citation for Media
Abstract
Dengue is hyperendemic in Brazil and is underestimated by passive surveillance. To better understand dengue incidence, we conducted epidemiologic analyses among participants, 2–59 years of age, from the placebo arm of a phase 3 dengue vaccine trial. During 2016–2021, a total of 5,947 participants contributed to 22,028 person-years of follow-up. We identified and virologically confirmed dengue (VCD), Zika, and chikungunya infections. We observed VCD and chikungunya incidence heterogeneity by age, geographic location, and study year. Children 2–6 years of age experienced the highest VCD (2.33/100 person-years) and chikungunya (1.02/100 person-years) incidence. VCD peaked in 2019 (n = 148) whereas chikungunya peaked in 2017 (n = 51). VCD incidence rates from active surveillance were generally higher than those reported to the national passive surveillance system; expansion factor range was <1–9.5 by municipality. Active surveillance is critical to better understand and characterize dengue epidemiology.
Dengue, caused by infection with one of 4 dengue virus (DENV) serotypes, is endemic in over 100 countries (1–4). Clinical manifestations of dengue range from asymptomatic to severe illness that can be fatal. Dengue is the most rapidly spreading mosquitoborne viral disease, increasing faster than any other communicable disease (5). Dengue mainly circulates in tropical and subtropical climates; most cases occur in Southeast Asia and Latin America (2,4). However, cases outside endemic areas are becoming more frequent because of increases in urbanization, travel to endemic regions, and the expansion of the primary vector (6,7).
More than 50% of the dengue cases in Latin America are reported in Brazil (8,9). In a 2024 outbreak, >10 million cases and >6,000 deaths were reported across Brazil (10,11). All 4 DENV serotypes have been reported in Brazil since 2010; typically, 2 serotypes cocirculate with variations in the dominant serotype over time (10). In addition to DENV, chikungunya virus (CHIKV) and Zika virus (ZIKV), which are transmitted by the same Aedes spp. mosquito vector, circulate in Brazil (12). CHIKV was first identified in Brazil in 2014 and causes annual epidemics (13,14). In 2015, a major outbreak of Zika led the Brazil Ministry of Health to declare a national health emergency (15,16).
The epidemiology of dengue in Brazil has previously been described using data collected through passive surveillance (17). Dengue, chikungunya, and Zika are notifiable diseases in Brazil; healthcare institutions report suspected, probable, and laboratory-confirmed cases, along with basic demographic information, to the national passive surveillance system, Sistema de Informação de Agravos de Notificação (SINAN) (17). However, because of the subclinical manifestation of dengue, many patients do not seek medical care. In addition, the nonspecific clinical presentation that overlaps with other arboviral diseases, including chikungunya and Zika, can cause misclassification. Those factors, along with reporting biases, can result in an underestimation of dengue burden by passive surveillance systems (18). Instead, active surveillance of prospective longitudinal cohorts can better estimate the burden of dengue with generally higher incidence rates than those reported by the national surveillance system (19,20).
To better understand dengue in Brazil, we conducted epidemiologic analyses among participants enrolled in a large phase 3 efficacy trial of a live attenuated tetravalent dengue vaccine, Butantan-DV (21,22). We described dengue serostatus by demographic characteristics before receipt of vaccine or placebo. We used the active surveillance of participants in the placebo arm of the trial to estimate incidence rates of dengue during 2016–2021 and determine the degree of underreporting compared with the national passive surveillance system.
Dengue Vaccine Efficacy Trial Design and Participants
DEN-03-IB (clinical trials identifier NCT02406729) is a double-blind, randomized, placebo-controlled, phase 3 trial to assess the safety and efficacy of a single dose of Butantan-dengue vaccine (Butantan-DV) for the prevention of symptomatic virologically confirmed dengue (VCD) (21,22). Participants included healthy persons 2–59 years of age who were enrolled and randomized 2:1 (Butantan-DV:placebo), stratified by age group (2–6, 7–17, and 18–59 years), at 16 sites in 15 municipalities across the 5 geographic regions of Brazil; 3 sites in the North, 4 sites in the Northeast, 3 sites in the Center-West, 5 sites in the Southeast, and 1 site in the South region. National Commission for Research Ethics (approval no. CAAE 44462915.8.1001.0068) and local ethics committees approved the study; it was conducted in accordance with the principles of good clinical practice.
Seropositivity Measurements
We determined baseline dengue serostatus retrospectively using blood samples collected on day 0 from enrolled participants, before receipt of vaccine or placebo. Samples were tested in a validated virus reduction neutralization test (VRNT), as previously described (21–24). In brief, serially diluted serum samples were mixed with wild-type DENV representing each of the 4 serotypes (DENV-1–4) before incubation with Vero cells. Cells were then fixed, stained with custom DENV-specific primary antibodies (GenScript, https://genscript.com) followed by Alexa Fluor 448-conjugated secondary antibodies (Invitrogen, https://invitrogen.com), and counted. The results were reported as a 60% VRNT (VRNT60) titer, the reciprocal of the serum dilution that reduced the number of infected cells by 60% compared with the virus control. We defined prior exposure to any DENV serotype (i.e., dengue seropositive at baseline) as having a VRNT60 titer against any of the 4 DENV serotypes above the lower limit of quantification (i.e., a VRNT60 titer of DENV-1 >18 or DENV-2 >15 or DENV-3 >12 or DENV-4 >13) at baseline (21–24).
Active Surveillance of Participants in the DEN-03-IB Placebo Arm
We conducted active surveillance of the 5,947 participants who received placebo and were in the per-protocol population of DEN-03-IB over 64 months from start through the data cutoff for the primary analysis, February 22, 2016–July 13, 2021. We defined the data cutoff as the date at which all enrolled participants in either treatment group had completed >2 years of follow-up (22). We analyzed deidentified data to assess the epidemiology and natural history of dengue in Brazil.
Site staff contacted participants by email, text message, or telephone at least monthly in the first 2 years and every 3 months afterwards to identify postvaccination adverse events and potential dengue cases. The sites could increase the frequency of follow-up contacts during times of localized outbreaks. In addition, we instructed participants in both treatment arms to seek out the trial team if they experienced a febrile illness or illness suspected to be dengue on the basis of clinical symptoms. We evaluated the presence and intensity of clinical symptoms during each unscheduled visit to assess suspected cases.
In cases of suspected dengue, a blood sample was collected, preferably within 9 days of symptom onset, for virologic confirmation. We extracted total RNA using QIAamp Viral RNA Mini Kit (QIAGEN, https://qiagen.com) before conducting reverse transcription PCR (RT-PCR) assays in a central laboratory. We made virologic confirmation of wild-type DENV and serotype determinations using a validated fourplex RT-PCR assay as previously described (25). In brief, we reversed transcribed and amplified total isolated RNA using DENV serotype–specific primer/probe sets targeting each of the 4 DENV serotypes (DENV-1–4). In addition, we tested samples separately for the presence of CHIKV and ZIKV viral RNA using previously described singleplex RT-PCRs with primer/probe sets targeting CHIKV or ZIKV (26, 27).
National Data
SINAN is a passive surveillance system that collects information from healthcare providers and institutions throughout Brazil on nationally notifiable diseases (17). Dengue cases in SINAN were defined by 2009 WHO diagnostic criteria (28) and confirmed through laboratory testing. In addition, healthcare providers reported basic demographic data (sex, age, race/ethnicity, and geographic location) from each dengue case (suspected, probable or confirmed) to SINAN. We pulled laboratory-confirmed dengue cases (confirmed by RT-PCR or IgM) from SINAN for the municipalities and time that DEN-03-IB took place. We disaggregated census data from the Instituto Brasileiro de Geografia e Estatística for the 15 municipalities that contained >1 of the 16 study sites.
Expansion Factors
We determined expansion factors (EF) as the ratio of VCD incidence from active surveillance of the placebo arm of DEN-03-IB per 100,000 person-years divided by laboratory-confirmed dengue incidence from the national passive surveillance system, SINAN, per 100,000 population, as described previously (19). We defined VCD incidence from active surveillance as the number of virologically confirmed cases over person-years of follow-up, determined weekly as the cumulative time that each participant contributed during active surveillance over the duration of the study, and in 2019 during an epidemic year. Given the large age groups (2–59 years of age) included in DEN-03-IB, we calculated EF for the entire population of the 15 municipalities for interpretation feasibility. We calculated laboratory-confirmed dengue incidence from passive surveillance by dividing laboratory-confirmed dengue cases using RT-PCR or IgM by the municipality population based on census data (19). An EF >1 indicates potential underreporting by SINAN; an EF <1 indicates potential underreporting by active follow-up.
Statistical Analyses
We summarized baseline demographics of all participants enrolled in the phase 3 trial (n=16,235) (Table 1). Covariates included age group at enrollment (2–6, 7–17, and 18–59 years of age), biologic sex (M/F), race (Pardo [multiracial Brazilian], White, Black, Asian, and Indigenous or Other), geographic region in Brazil (North, Northeast, Central-West, South, Southeast), prior exposure to any DENV serotype (yes/no) and a self-reported history of yellow fever vaccination before study enrollment (yes/no).
We calculated estimates of incidence of virologically confirmed dengue, chikungunya, or Zika only among placebo recipients in the per-protocol population (n = 5,947) using a person-time approach. We defined incidence rate as cases per 100 person-years. We counted participants who experienced recurrent infections by >1 DENV serotype once in the total incidence and separately by serotype for the serotype-specific incidence. We determined incidence by age group according to participant age at the time of the event. We summarized incidence rates by demographic subgroup, baseline dengue serostatus for those with a known serostatus, and by study year. We calculated 95% CI for incidence rates using Poisson exact (29).
We estimated EFs for each municipality to understand the degree of underreporting of dengue illness in the national passive surveillance system (30). We calculated 95% CI for EFs using Clopper-Pearson exact method (31). We calculated EFs and 95% CI during the entire follow-up study period (2016–2021) and during an outbreak year (2019).
We summarized the frequency and distribution of clinical signs and symptoms associated with virologically confirmed dengue-associated or chikungunya-associated illness among placebo recipients and calculated 95% CIs using Clopper-Pearson exact method (31). We performed statistical analyses using SAS software version 9.4 (SAS Institute, Inc., https://www.sas.com).
Participant Demographics and Baseline Serostatus
A total of 16,235 participants underwent randomization and received Butantan-DV (n = 10,259) or placebo (n = 5,976) during February 2016–July 2019. The baseline characteristics were comparable between the 2 arms; all participants had a history of previous yellow fever vaccination and approximately half of participants did not have evidence of prior dengue exposure before vaccination (Table 1). Of the 16,235 participants, 15,605 (96.1%) had a known dengue serostatus at baseline; 9,864 in the Butantan-DV arm and 5,741 in the placebo arm (Table 2). At baseline, most children ages 2–6 years of age (81.0%) and participants in the South region (91.8%) were DENV-naive. Although DENV seropositivity increased with age, 26.9% of adults (18–59 years old) were seronegative at baseline (Table 2).
Incidence of VCD
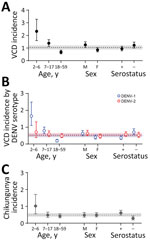
Participants had completed >2 years of follow-up by the data cutoff (July 13, 2021). In total, 5,947 participants in the placebo arm had contributed to 22,028 person-years of follow-up. During follow-up, 228 cases of VCD from any DENV serotype were reported after Day 28 (incidence rate = 1.04/100 person-years), accounting for 1.71% of fever episodes (Appendix Table 1). Children 2–6 years of age had the highest rate of VCD (2.33/100 person-years) compared with older age groups (1.38/100 person-years for the 7–17 group and 0.68/100 person-years for the 18–59 group) (Figure 1). The Center-West region had the highest incidence (1.64/100 person-years); VCD was not observed in the South (Figure 2). VCD incidence peaked in 2019 (148 cases; 2.56/100 person-years).
We observed VCD cases resulting from DENV-1 (n = 111; 0.50/100 person-years) and DENV-2 (n = 119; 0.54/100 person-years) among participants in the placebo arm (Appendix Table 2); we did not observe cases of VCD resulting from DENV-3 or DENV-4 in the trial by the cutoff date. Two participants had dual infections of DENV-1 and DENV-2; in 1 participant they were concurrent and in the other, sequential. The Center-West and Southeast regions had a higher rate of DENV-2 (1.3/100 person-years in Center-West and 0.80/100 person-years in Southeast) compared with the North and Northeast, which were dominated by DENV-1 (0.58/100 person-years in the North region and 0.77/100 person-years in Northeast). We also observed differences in DENV serotype-specific incidence by age groups; DENV-1 incidence was higher in the 2–6 age group, DENV-2 was higher in the 18–59 age group, and both DENV serotypes had comparable incidence rates in the 7–17 age group.
Estimating the Degree of Passive Surveillance System Underreporting for Dengue
Underreporting in the national passive surveillance system, SINAN, varied by municipality and over time (Figure 3). By municipality, considering the entire study period (2016–2021), EF range was <1 to 9.5 (Table 3). When considering only 2019, the year in which a major dengue outbreak occurred in Brazil (10, 32, 33), the EF range by municipality was 0–492.9 (Table 4).
Incidence of Other Laboratory-Confirmed Arboviral-Associated Illness
During the study period, 3 laboratory-confirmed Zika episodes (incidence rate 0.01/100 person-years) and 106 laboratory-confirmed chikungunya cases (incidence rate 0.48/100 person-years) were captured. We observed the highest incidence of laboratory-confirmed chikungunya in the 2–6 age group (1.02/100 person-years) spread out across the geographic locations; the Northeast region had the highest rates (0.70/100 person-years). Furthermore, we observed most laboratory-confirmed chikungunya cases (n = 54) in 2016 (0.99/100 person-years) and 2017 (1.68/100 person-years), the 2 years with the lowest rates of VCD during the study (Figure 2).
The clinical manifestations of VCD and chikungunya cases during the follow-up were generally comparable; arthralgia, pyrexia, and headache were the most commonly reported symptoms among either VCD or chikungunya cases (Figure 4). Arthritis was more commonly reported among chikungunya cases (11%) than VCD cases (1%).
We used active surveillance from a phase 3 dengue vaccine efficacy trial (DEN-03-IB) to better understand dengue incidence in Brazil during 2016–2021. Dengue incidence was generally higher in our study than estimates reported in the national passive surveillance system but varied by municipality and study year. Nonspecific clinical manifestations overlapping with other circulating arboviruses, as we observed with laboratory-confirmed chikungunya in this study, may further contribute to underreporting of dengue.
We used data from ≈6,000 participants 2–59 years of age who were enrolled in the placebo arm of the study to assess the incidence of dengue. Nearly a third of the participants in DEN-03-IB were adults (18–59 years of age); a large proportion of whom (26.9%) were dengue seronegative at baseline. Furthermore, active surveillance ensured that even mild cases of dengue were detected and distinguished from other arboviruses (ZIKV and CHIKV). Although the follow-up spanned multiple seasons (2016–2021), we detected only DENV-1 and DENV-2 in the study; we did not observe cases of VCD caused by DENV-3 or DENV-4. The absence of DENV-3 and DENV-4 reflects the reported circulation of DENV in Brazil during the period in which the trial was conducted (10). We observed regional and age differences in serotype-specific incidence for DENV-1 and DENV-2, suggesting previous population exposure histories may affect DENV serotype circulation. Consistent with previous reports that used passive surveillance (34–41), we found that the highest burden of dengue occurred in the Central-West region. Furthermore, in our study, children 2–6 years of age had the highest incidence of laboratory-confirmed dengue and chikungunya compared with the older age subgroups.
Placebo cohorts from phase 3 efficacy trials are a valuable data source to characterize dengue epidemiology within a country. Our findings add to previous results from other dengue vaccine phase 3 trials conducted in Brazil and provide report of active surveillance among adults (>18 years of age). Although those datasets are complementary, between-study comparisons are challenging because of differences in participant demographics, study site locations, and the period of follow-up. CYD15 was a phase 3 trial of the tetravalent dengue vaccine CYD-TDV (Dengvaxia; Sanofi, https://www.sanofi.com) conducted in 5 countries across 22 sites, including 5 sites in Brazil, during June 2011–April 2014 (42). In CYD15, overall VCD incidence was 3.5/100 person-years among 1,177 placebo recipients 9–16 years of age in Brazil (43), higher than what we observed in the DEN-03-IB trial from 2016–2021 (1.04/100 person-years). TIDES was a phase 3 trial of the tetravalent dengue vaccine TAK-003 (Qdenga; Takeda, https://www.takeda.com) conducted at 26 sites in 8 countries, including 4 sites in Brazil during September 2016–December 2021 (44, 45, 46). In this similar timeframe, VCD incidence among 560 participants 4–16 years of age in Brazil (0.9/100 person-years) was generally comparable to rates observed in DEN-03-IB; incidence peaked in 2016 (caused by DENV-1) and 2019 (caused by DENV-2), consistent with DEN-03-IB. Still, the differences between incidence rates across trials could be attributed to differences by age or underlying serostatus of the study population and emphasize the variability and unpredictability of dengue epidemiology.
Previous studies of dengue epidemiology in Brazil have relied on data from SINAN, the national passive surveillance system. However, incidence rates from passive surveillance are likely underestimating the true burden of dengue because of the subclinical nature of dengue, particularly with the first infection, and because the clinical manifestation of dengue is similar to that of other arboviral diseases, including chikungunya and Zika. In addition, laboratory confirmation practices vary across healthcare institutions. We observed a large degree of underreporting in the national passive surveillance system (ratio of DEN-03-IB/SINAN>1), particularly during the dengue outbreak in 2019 (10,32,33). The increased underreporting in 2019 was likely caused by differences in surveillance practices during an outbreak, when the volume of cases overwhelmed testing and reporting systems; it is more challenging to conduct laboratory confirmation on suspected cases in those conditions (47). We also observed underreporting in the active surveillance (ratio of DEN-03-IB/SINAN<1) in some sites, particularly across the full study period of 2016–2021. A possible cause of the underreporting in active surveillance could be our limited ability to calculate EF from only a subset of the population, because clinical sites do not necessarily represent the entire municipality. EFs estimated from CYD15 using similar methods indicated that dengue was underreported in Brazil during 2011–2014 at a national (EF = 26.7), state (EF = 16.9), and local level (EF = 19.4) (19). Although it is difficult to compare EF estimates that are highly dependent on data availability, including age stratification, case definitions, and temporospatial factors, those data support the finding that underreporting of dengue in passive surveillance systems remains an important issue (19).
Two other arboviruses, ZIKV and CHIKV, co-circulate with DENV in Brazil (12). ZIKV was first identified in Brazil in 2015, before the initiation of the DEN-03-IB vaccine trial (16); ZIKV caused a major outbreak that peaked in February 2016, just as trial enrollment began, and subsequently circulated at low levels. In our study, 3 episodes of ZIKV were confirmed in participants under active surveillance. A possible explanation for the rarity of Zika cases in DEN-03-IB is the limited number of participants under active surveillance during the Zika outbreak; the last study participant enrolled in 2019 (22). An outbreak of chikungunya peaked in 2017; we captured many cases in our study. The overall low specificity of symptoms between chikungunya and dengue among participants in this study represents a misclassification risk that could contribute to underreporting to SINAN. The detection of both CHIKV and ZIKV infections, albeit at lower rates than VCD, illustrates the co-circulation of arboviruses in Brazil and the potential for misclassification in syndromic surveillance systems. Those observations confirm the need to reinforce laboratory confirmation practices.
DEN-03-IB enrolled participants 2–59 years of age in predefined urban centers; generalizability to older adults, rural populations, or other geographic regions may be limited. Few participants were enrolled in the single clinical site located in the South region of Brazil, limiting the interpretation of dengue circulation in that region. Several factors can affect incidence estimations including follow-up, withdrawal, or differential healthcare seeking across time and sites, although we minimized those factors in the randomized controlled trial. Nevertheless, the rigorous and standardized surveillance we conducted across all sites strengthens the internal validity and comparability of our findings.
EF calculations have inherent limitations, such as the comparison of active surveillance in healthy participants with passive surveillance data from the municipalities’ general population. Furthermore, given the limited number of observations at the geographic level in this study, we did not stratify EFs by age. Although EF methodology is not perfect, EF estimates can provide a sense of the magnitude of dengue underreporting.
In sum, dengue epidemiology is unpredictable and varies over time by geography, serotype and age, even within a country. A better understanding of its epidemiology would inform public health interventions aimed at the prevention and control of dengue worldwide. Clinical manifestations are nonspecific, and surveillance remains an important tool to monitor arbovirus epidemiology. Furthermore, the differences in national surveillance systems, their reporting and laboratory-confirmation practices, and variable clinical definitions limit the extrapolation of surveillance data between countries. Our findings have direct implications for public health decision making, including the implementation of vaccination strategies and the interpretation of surveillance systems data. Longitudinal active surveillance embedded within vaccine trials represents a valuable approach to refining estimates of disease burden and informing control strategies in endemic settings.
Ms. Barros is an epidemiologist manager leading epidemiologic and post-marketing studies on immunopreventable diseases and vaccines at Instituto Butantan, São Paulo, Brazil. Her area of interest includes developing epidemiologic studies on immunopreventable diseases and vaccine outcomes in the public health context.
Acknowledgments
We thank the participants (and their parents) who enrolled in the study, Monica Cintra (Instituto Butantan, São Paulo, Brazil) for her leadership and contributions to the study; Bo Zheng and Fansen Kong (Merck Sharp & Dohme LLC, a subsidiary of Merck & Co., Inc., Rahway, NJ, USA [MSD]) and Amit Bhaniani (MSD [UK] Limited, London, UK) for programming support. Editorial assistance was provided by Karyn Davis (MSD).
Data sharing: Data and code will be made to qualified scientific researchers with a specific purpose outlined in a proposal approved by Instituto Butantan. Requests will be evaluated for scientific validity within 6 months. Underlying code and complete deidentified patient data set will be shared after the researcher enters into standard data sharing agreement and the proposal is approved. Researchers must commit to transparency in publication. Requests for data must be sent to
Instituto Butantan, São Paulo, Brazil sponsored the phase 3 trial with statistical analyses, data management, and assay support from MSD.
M.M., E.M.A, A.E-J., and G.A. are employees of MSD, and M.L.J. is an employee of MSD (UK) Limited, London, UK, all of whom may own stock or hold stock options in Merck & Co., Inc., Rahway, NJ, USA. E.N.C.B., M.A.R., J.A.M., and F.C.B. are employees of Instituto Butantan, a nonprofit public health institution of the State of São Paulo, Brazil. F.C.B. reports owning stock from Novartis.
References
- Bhatt S, Gething PW, Brady OJ, Messina JP, Farlow AW, Moyes CL, et al. The global distribution and burden of dengue. Nature. 2013;496:504–7. DOIPubMedGoogle Scholar
- Stanaway JD, Shepard DS, Undurraga EA, Halasa YA, Coffeng LE, Brady OJ, et al. The global burden of dengue: an analysis from the Global Burden of Disease Study 2013. Lancet Infect Dis. 2016;16:712–23. DOIPubMedGoogle Scholar
- Yang X, Quam MBM, Zhang T, Sang S. Global burden for dengue and the evolving pattern in the past 30 years. J Travel Med. 2021;28:
taab146 . DOIPubMedGoogle Scholar - Deng J, Zhang H, Wang Y, Liu Q, Du M, Yan W, et al. Global, regional, and national burden of dengue infection in children and adolescents: an analysis of the Global Burden of Disease Study 2021. EClinicalMedicine. 2024;78:
102943 . DOIPubMedGoogle Scholar - Pan American Health Organization (PAHO). Dengue [cited 2025 Mar 28]. https://www3.paho.org/data/index.php/en/mnu-topics/indicadores-dengue-en.html
- Paz-Bailey G, Adams LE, Deen J, Anderson KB, Katzelnick LC. Dengue. Lancet. 2024;403:667–82. DOIPubMedGoogle Scholar
- Xu Z, Bambrick H, Frentiu FD, Devine G, Yakob L, Williams G, et al. Projecting the future of dengue under climate change scenarios: progress, uncertainties and research needs. PLoS Negl Trop Dis. 2020;14:
e0008118 . DOIPubMedGoogle Scholar - Sansone NMS, Boschiero MN, Marson FAL. Dengue outbreaks in Brazil and Latin America: the new and continuing challenges. Int J Infect Dis. 2024;147:
107192 . DOIPubMedGoogle Scholar - Tapia-Conyer R, Betancourt-Cravioto M, Mendez-Galvan J. Dengue: an escalating public health problem in Latin America. Paediatr Int Child Health. 2012;32(Suppl 1):14–7. DOIGoogle Scholar
- Brasil, Ministério da Saúde, Secretaria de Vigilância em Saúde. Monitoring of arboviruses and closing report of the Emergency Operations Committee (COE) Dengue and other Arboviruses 2024 [in Portuguese]. Bol Epidemiol (Porto Alegre). 2024;55:••• https://www.gov.br/saude/pt-br/centrais-de-conteudo/publicacoes/boletins/epidemiologicos/edicoes/2024/boletim-epidemiologico-volume-55-no-11.pdf cited 2026 Mar 12.
- Pan American Health Organization. Dengue: analysis by country. 2024 [cited 2026 Mar 12]. https://www.paho.org/en/arbo-portal/dengue-data-and-analysis/dengue-analysis-country
- Cardoso CW, Paploski IA, Kikuti M, Rodrigues MS, Silva MM, Campos GS, et al. Outbreak of exanthematous illness associated with Zika, chikungunya, and dengue viruses, Salvador, Brazil. Emerg Infect Dis. 2015;21:2274–6. DOIPubMedGoogle Scholar
- Nunes MR, Faria NR, de Vasconcelos JM, Golding N, Kraemer MU, de Oliveira LF, et al. Emergence and potential for spread of chikungunya virus in Brazil. BMC Med. 2015;13:102. DOIPubMedGoogle Scholar
- de Souza WM, Ribeiro GS, de Lima STS, de Jesus R, Moreira FRR, Whittaker C, et al. Chikungunya: a decade of burden in the Americas. Lancet Reg Health Am. 2024;30:
100673 . DOIPubMedGoogle Scholar - Faria NR, Azevedo RDSDS, Kraemer MUG, Souza R, Cunha MS, Hill SC, et al. Zika virus in the Americas: early epidemiological and genetic findings. Science. 2016;352:345–9. DOIPubMedGoogle Scholar
- Campos GS, Bandeira AC, Sardi SI. Zika virus outbreak, Bahia, Brazil. Emerg Infect Dis. 2015;21:1885–6. DOIPubMedGoogle Scholar
- Ministry of Health (Brazil). Brazil information system for notifiable diseases [cited 2026 Mar 12]. https://portalsinan.saude.gov.br
- Silva MM, Rodrigues MS, Paploski IA, Kikuti M, Kasper AM, Cruz JS, et al. Accuracy of dengue reporting by national surveillance system, Brazil. Emerg Infect Dis. 2016;22:336–9. DOIPubMedGoogle Scholar
- Sarti E, L’Azou M, Mercado M, Kuri P, Siqueira JB Jr, Solis E, et al. A comparative study on active and passive epidemiological surveillance for dengue in five countries of Latin America. Int J Infect Dis. 2016;44:44–9. DOIPubMedGoogle Scholar
- Gurgel-Gonçalves R, Oliveira WK, Croda J. The greatest dengue epidemic in Brazil: surveillance, prevention, and control. Rev Soc Bras Med Trop. 2024;57:
e002032024 . DOIPubMedGoogle Scholar - Kallás EG, Cintra MAT, Moreira JA, Patiño EG, Braga PE, Tenório JCV, et al. Live, attenuated, tetravalent Butantan-Dengue vaccine in children and adults. N Engl J Med. 2024;390:397–408. DOIPubMedGoogle Scholar
- Nogueira ML, Cintra MAT, Moreira JA, Patiño EG, Braga PE, Tenório JCV, et al. Phase 3 Butantan-DV Working Group. Efficacy and safety of Butantan-DV in participants aged 2–59 years through an extended follow-up: results from a double-blind, randomised, placebo-controlled, phase 3, multicentre trial in Brazil. Lancet Infect Dis. 2024;24:1234–44. DOIPubMedGoogle Scholar
- Russell KL, Rupp RE, Morales-Ramirez JO, Diaz-Perez C, Andrews CP, Lee AW, et al. A phase I randomized, double-blind, placebo-controlled study to evaluate the safety, tolerability, and immunogenicity of a live-attenuated quadrivalent dengue vaccine in flavivirus-naïve and flavivirus-experienced healthy adults. Hum Vaccin Immunother. 2022;18:
2046960 . DOIPubMedGoogle Scholar - Whiteman MC, Bogardus L, Giacone DG, Rubinstein LJ, Antonello JM, Sun D, et al. Virus reduction neutralization test: a single-cell imaging high-throughput virus neutralization assay for dengue. Am J Trop Med Hyg. 2018;99:1430–9. DOIPubMedGoogle Scholar
- Johnson BW, Russell BJ, Lanciotti RS. Serotype-specific detection of dengue viruses in a fourplex real-time reverse transcriptase PCR assay. J Clin Microbiol. 2005;43:4977–83. DOIPubMedGoogle Scholar
- Lanciotti RS, Kosoy OL, Laven JJ, Panella AJ, Velez JO, Lambert AJ, et al. Chikungunya virus in US travelers returning from India, 2006. Emerg Infect Dis. 2007;13:764–7. DOIPubMedGoogle Scholar
- Lanciotti RS, Kosoy OL, Laven JJ, Velez JO, Lambert AJ, Johnson AJ, et al. Genetic and serologic properties of Zika virus associated with an epidemic, Yap State, Micronesia, 2007. Emerg Infect Dis. 2008;14:1232–9. DOIPubMedGoogle Scholar
- Brasil. Ministério da Saúde. Secretaria de Vigilância em Saúde. Diretoria Técnica de Gestão. Dengue: diagnosis and clinical management: adult and child [in Portuguese]. Ministério da Saúde, Secretaria de Vigilância em Saúde, Diretoria Técnica de Gestão. 4th ed. Brasília (Brazil): Ministério da Saúde; 2013.
- Ulm K. A simple method to calculate the confidence interval of a standardized mortality ratio (SMR). Am J Epidemiol. 1990;131:373–5. DOIPubMedGoogle Scholar
- Toan NT, Rossi S, Prisco G, Nante N, Viviani S. Dengue epidemiology in selected endemic countries: factors influencing expansion factors as estimates of underreporting. Trop Med Int Health. 2015;20:840–63. DOIPubMedGoogle Scholar
- Newcombe RG. Two-sided confidence intervals for the single proportion: comparison of seven methods. Stat Med. 1998;17:857–72. DOIPubMedGoogle Scholar
- Brasil, Ministério da Saúde, Secretaria de Vigilância em Saúde. Death due to arboviruses in Brazil, 2008 to 2019 [in Portuguese]. Bol Epidemiol (Porto Alegre). 2020;51:1–28.
- Brasil, Ministério da Saúde, Secretaria de Vigilância em Saúde. Monitoring of urban arbovirus cases transmitted by Aedes (dengue, chikungunya, and Zika), epidemiological weeks 01 to 50 [in Portuguese]. Bol Epidemiol (Porto Alegre). 2020;51:1–33.
- Junior JBS, Massad E, Lobao-Neto A, Kastner R, Oliver L, Gallagher E. Epidemiology and costs of dengue in Brazil: a systematic literature review. Int J Infect Dis. 2022;122:521–8. DOIPubMedGoogle Scholar
- Hökerberg YHM, Kohn F, Souza TS, Passos SRL. Clinical profile of dengue in the elderly using surveillance data from two epidemics. Rev Soc Bras Med Trop. 2022;55:
e0290 . DOIPubMedGoogle Scholar - Macias AE, Werneck GL, Castro R, Mascareñas C, Coudeville L, Morley D, et al. Mortality among hospitalized dengue patients with comorbidities in Mexico, Brazil, and Colombia. Am J Trop Med Hyg. 2021;105:102–9. DOIPubMedGoogle Scholar
- Santana LMR, Baquero OS, Maeda AY, Nogueira JS, Chiaravalloti Neto F. Spatio-temporal dynamics of dengue-related deaths and associated factors. Rev Inst Med Trop São Paulo. 2022;64:
e30 . DOIPubMedGoogle Scholar - Sousa SC, Silva TAMD, Soares AN, Carneiro M, Barbosa DS, Bezerra JMT. Factors associated with deaths from dengue in a city in a metropolitan region in southeastern Brazil: a case-control study. Rev Soc Bras Med Trop. 2022;55:e0043–2022. DOIPubMedGoogle Scholar
- Werneck GL, Macias AE, Mascarenas C, Coudeville L, Morley D, Recamier V, et al. Comorbidities increase in-hospital mortality in dengue patients in Brazil. Mem Inst Oswaldo Cruz. 2018;113:
e180082 . DOIPubMedGoogle Scholar - Queiroga AS, Barbosa DAM, Campos TL, Schwarzbold AV, Siqueira AM, Salvato RS, et al. Severe dengue-related deaths in the elderly population soared in Southern Brazil in 2024. IJID Reg. 2025;14:
100577 . DOIPubMedGoogle Scholar - Burattini MN, Lopez LF, Coutinho FA, Siqueira JB Jr, Homsani S, Sarti E, et al. Age and regional differences in clinical presentation and risk of hospitalization for dengue in Brazil, 2000–2014. Clinics (Sao Paulo). 2016;71:455–63. DOIPubMedGoogle Scholar
- Villar L, Dayan GH, Arredondo-García JL, Rivera DM, Cunha R, Deseda C, et al.; CYD15 Study Group. Efficacy of a tetravalent dengue vaccine in children in Latin America. N Engl J Med. 2015;372:113–23. DOIPubMedGoogle Scholar
- L’Azou M, Moureau A, Sarti E, Nealon J, Zambrano B, Wartel TA, et al.; CYD14 Primary Study Group. CYD15 Primary Study Group. Symptomatic dengue in children in 10 Asian and Latin American countries. N Engl J Med. 2016;374:1155–66. DOIPubMedGoogle Scholar
- Biswal S, Reynales H, Saez-Llorens X, Lopez P, Borja-Tabora C, Kosalaraksa P, et al.; TIDES Study Group. Efficacy of a tetravalent dengue vaccine in healthy children and adolescents. N Engl J Med. 2019;381:2009–19. DOIPubMedGoogle Scholar
- Kastner R, López-Medina E, Sirivichayakul C, Biswal S, Escudero I, Folschweiller N, et al. The burden of dengue in Latin America and Asia: Epidemiological data over 57 months of follow-up in a phase 3 trial. Poster presented at: The American Society of Tropical Medicine and Hygiene Annual Meeting; November 13–17, 2024; New Orleans, Louisiana, USA.
- Tricou V, Yu D, Reynales H, Biswal S, Saez-Llorens X, Sirivichayakul C, et al. Long-term efficacy and safety of a tetravalent dengue vaccine (TAK-003): 4.5-year results from a phase 3, randomised, double-blind, placebo-controlled trial. Lancet Glob Health. 2024;12:e257–70. DOIPubMedGoogle Scholar
- Brasil. Ministério da Saúde. Health surveillance guide. 4th edition. Brasília: Ministério da Saúde; 2019.
Figures
Tables
Cite This ArticleOriginal Publication Date: April 06, 2026
1Preliminary results from this study were presented at the American Society for Tropical Medicine and Hygiene annual meeting; November 13–17, 2024; New Orleans, Louisiana, USA.
Table of Contents – Volume 32, Number 4—April 2026
| EID Search Options |
|---|
|
|
|
|
|
|



Please use the form below to submit correspondence to the authors or contact them at the following address:
Maïna L’Azou Jackson, Epidemiology, MSD (UK) Ltd, 120 Moorgate, London EC2M 6UR, UK
Top