Volume 27, Number 11—November 2021
Dispatch
Fatal Multisystem Inflammatory Syndrome in Adult after SARS-CoV-2 Natural Infection and COVID-19 Vaccination
Cite This Article
Citation for Media
Abstract
We describe a fatal case of multisystem inflammatory syndrome in an adult with onset 22 days after a second dose of mRNA coronavirus disease vaccine. Serologic and clinical findings indicated severe acute respiratory syndrome coronavirus 2 infection occurred before vaccination. The immunopathology of this syndrome, regardless of vaccination status, remains poorly understood.
A multisystem inflammatory syndrome in children (MIS-C) and adults (MIS-A) occurring after coronavirus disease (COVID-19) has been identified; onset is ≈4–6 weeks after severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection (1–3). A case definition for MIS-A has been developed by the Centers for Disease Control and Prevention (CDC) (4); MIS-A after vaccination is rare and remains of great clinical and public health interest (5). We report a case study and histopathologic findings from a fatal MIS-A case after SARS-CoV-2 infection and subsequent complete COVID-19 vaccination.
The patient was a healthcare worker in his 30s with no notable medical history. In December 2020, he experienced mild COVID-19–like illness symptoms, including fatigue and loss of taste and smell. He did not undergo testing for SARS-CoV-2 at that time and was unaware of the need for isolation. Six days after onset of COVID-19–like symptoms, and when fully recovered, the patient received the first dose of Pfizer/BioNTech (https://www.pfizer.com) mRNA COVID-19 vaccine. He received the second dose 20 days later. After the second dose, he reported fatigue and malaise, which resolved within 2 days.
Twenty-two days after receiving the second dose of the COVID-19 vaccine, he had onset of new fever, malaise, headache, and odynophagia. He was examined by an outpatient medical provider. Diagnostic testing was notable for a negative COVID-19 test by reverse transcription PCR (RT-PCR), negative rapid influenza antigen, and negative rapid antigen detection for group A Streptococcus. Four days later, the patient visited an emergency department because of worsening symptoms. Assessment of vital signs revealed a temperature of 37.2°C, heart rate 113 beats/min, and blood pressure of 117/66 mmHg. Physical examination identified right-sided cervical lymphadenopathy, marked bilateral conjunctival erythema, and a faint papular rash on the pelvis and left flank. Laboratory testing revealed a peripheral-blood leukocyte count of 11,000 cells/μL, 93.5% segmented neutrophils, and thrombocytopenia with a platelet count of 110,000/μL (Table). Portable chest radiograph results were without notable findings.
On hospital day 2, the patient remained febrile and tachycardic (heart rate 90–135 beats/min) and had a blood pressure of 92/56 mmHg. Diagnostic evaluation revealed a negative SARS-CoV-2 RT-PCR test but a positive serologic test for SARS-CoV-2 nucleocapsid IgG. Additional diagnostic tests were conducted (Table). Inflammatory markers showed elevated C-reactive protein at 284.0 mg/L, serum ferritin at 1434.9 ng/mL, and troponin-I at 18.0 ng/mL. On the evening of hospital day 2, the patient received 75 g of intravenous immune globulin (IVIG).
Early morning on hospital day 3, the patient had an acute change in mental status, including confusion and global aphasia. An emergent computed tomography scan of the head was negative for cerebrovascular accident and showed normal brain parenchyma and no evidence of acute infarction, mass, or hemorrhage. On completion of the scan, the patient was found nonresponsive and without a pulse. He underwent multiple rounds of advanced cardiac life support, resulting in return of spontaneous circulation. A chest radiograph showed an enlarged cardiac silhouette, and an echocardiogram showed severe biventricular dysfunction, severe global hypokinesis of the left ventricle, and left ventricular ejection fraction of 20%. The patient received a second dose of IVIg and intravenous steroids and extracorporeal membrane oxygenation support was initiated. On hospital day 4, severe multisystem organ failure continued to progress. The patient died on hospital day 4.
We reviewed the patient’s medical history and clinical chart. We assessed serum samples collected during the hospital course before and after IVIg, and we determined endpoint titers to SARS-CoV-2 nucleocapsid (IgM and IgG) and spike receptor binding domain with neutralization functions against spike protein (6,7). The endpoint titer was a modified protocol based on Stadlbauer et al. (8). We completed an autopsy and sent formalin-fixed, paraffin-embedded tissues to CDC. Microscopic examination of lung, airways, pulmonary lymph node, liver, heart, spleen, kidneys and stomach tissue samples was performed; LT-Gram stain was performed on lungs and heart. An RT-PCR assay for SARS-CoV-2 was performed on RNA extracted from formalin-fixed, paraffin-embedded tissues from lungs, airways, and heart by methods previously published (9). This activity was reviewed by CDC and was conducted consistent with applicable federal law and CDC policy.
Serum antibody results drawn before IVIg infusion were negative for SARS-CoV-2 IgM but positive for IgG. Serum results had a high titer of anti-spike receptor binding domain antibody both before and after IVIg (1:75,000) compared with a naturally infected SARS-CoV-2–positive control (1:4,000). In addition, the pre-IVIG sample serum results demonstrated neutralizing function.
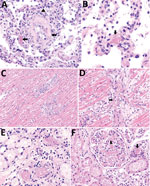
Notable findings on gross internal autopsy examination included a 525-mL pericardial effusion and cardiac enlargement, as well as a 5-L hemoperitoneum and a 20-cm diameter perisplenic hematoma. Microscopic examination of the lungs showed diffuse congestion, increased intra-alveolar macrophages, multifocal hemorrhage, capillaritis, and microthrombi throughout (Figure, panels A, B). We observed no viral inclusions or diffuse alveolar damage. Trachea and bronchi showed mild tracheobronchitis. Sections of the heart showed multifocal myocarditis with mixed inflammatory infiltrate, myocyte necrosis, and numerous microthrombi. We also identified disseminated microvascular thrombosis in the heart, stomach, kidneys, and liver (Figure, panels C–F). Gram stain results were negative on lung and heart tissue. SARS-CoV-2 RT-PCR was negative on lungs, trachea, bronchi, and heart.
This fatal case of MIS-A occurred after full COVID-19 vaccination in a patient with prior natural SARS-CoV-2 infection suspected 6 weeks before MIS-A symptom onset. Serum antibody results before IVIg infusion indicated the patient was previously infected with SARS-CoV-2 and was vaccinated with a COVID-19 vaccine. Antibodies to the nucleocapsid protein are the most sensitive target for serologic diagnosis for natural infection (P.D. Burbelo et al., unpub. data, https://doi.org/10.1101/2020.04.20.20071423), and these antibodies are not present following COVID-19 vaccination alone. In addition, clinical history was compatible with natural infection beginning 6 days before the first mRNA vaccine dose and consistent with negative SARS-CoV-2 nucleocapsid IgM on testing during hospitalization.
The patient demonstrated similar clinical findings to previously reported MIS-A cases, including fever for 3 consecutive days, laboratory evidence of inflammation, neurologic and mucocutaneous clinical findings, and severe cardiac illness that included systemic hypotension progressing to cardiogenic shock (1,5). These criteria meet the CDC case definition for MIS-A, as well as a definitive case at level 1 of diagnostic certainty by the Brighton collaboration case definition for MIS-A and MIS-C (10). In addition, the histopathologic findings of capillaritis and multiorgan microvascular thrombosis in association with clinical symptoms and laboratory findings are compatible with MIS-A (1,11). Substantial blood loss on gross examination may represent a diffuse intravascular coagulation–type picture in which diffuse microthrombosis depleted platelets and clotting factors. The etiology for clinical deterioration was likely multifactorial, although considerable cardiac compromise in the setting of high fluid volumes and intraperitoneal hemorrhage may have contributed to multiorgan failure
Whether mRNA COVID-19 vaccination contributed to MIS-A onset in this case is unclear, and future epidemiologic studies are needed to understand whether an association exists. The immunopathology leading to hyperinflammation causing MIS-A after SARS-CoV-2 infection remains unknown, although postinfection immune dysregulation is consistent among reported cases. Notably, MIS-A has not been reported among adult participants of COVID-19 vaccine trials (10), and no direct evidence exists to support vaccine alone as the primary etiology in this case. This article further emphasizes the importance of COVID-19 prevention, for which infection prevention strategies and vaccination remain our greatest defense.
Dr. Grome is an infectious diseases physician and Epidemic Intelligence Service Officer for the Centers for Disease Control and Prevention, Atlanta, Georgia. She is currently assigned as a field officer at the Tennessee Department of Health in Nashville, Tennessee.
Acknowledgment
This work was supported by the National Institutes of Health (grant nos. R43 AI155211 and R01 AI139267 awarded to M.G.S.).
References
- Morris SB, Schwartz NG, Patel P, Abbo L, Beauchamps L, Balan S, et al. Case series of multisystem inflammatory syndrome in adults associated with SARS-CoV-2 infection—United Kingdom and United States, March–August 2020. MMWR Morb Mortal Wkly Rep. 2020;69:1450–6. DOIPubMedGoogle Scholar
- Tenforde MW, Morris SB. Multisystem inflammatory syndrome in adults: coming into focus. Chest. 2021;159:471–2. DOIPubMedGoogle Scholar
- Godfred-Cato S, Bryant B, Leung J, Oster ME, Conklin L, Abrams J, et al.; California MIS-C Response Team. COVID-19-associated multisystem inflammatory syndrome in children—United States, March–July 2020. MMWR Morb Mortal Wkly Rep. 2020;69:1074–80. DOIPubMedGoogle Scholar
- National Center for Immunization and Respiratory Diseases, Centers for Disease Control and Prevention. Multisystem inflammatory syndrome in adults (MIS-A) case definition information for healthcare providers 2021 [cited 2021 Jul 1]. https://www.cdc.gov/mis/mis-a/hcp.html
- Salzman MB, Huang CW, O’Brien CM, Castillo RD. Multisystem inflammatory syndrome after SARS-CoV-2 infection and COVID-19 vaccination. Emerg Infect Dis. 2021;27:1944–8. DOIPubMedGoogle Scholar
- McAndrews KM, Dowlatshahi DP, Dai J, Becker LM, Hensel J, Snowden LM, et al. Heterogeneous antibodies against SARS-CoV-2 spike receptor binding domain and nucleocapsid with implications for COVID-19 immunity. JCI Insight. 2020;5:
142386 . DOIPubMedGoogle Scholar - Condor Capcha JM, Lambert G, Dykxhoorn DM, Salerno AG, Hare JM, Whitt MA, et al. Generation of SARS-CoV-2 spike pseudotyped virus for viral entry and neutralization assays: a 1-week protocol. Front Cardiovasc Med. 2021;7:
618651 . DOIPubMedGoogle Scholar - Stadlbauer D, Amanat F, Chromikova V, Jiang K, Strohmeier S, Arunkumar GA, et al. SARS-CoV-2 seroconversion in humans: a detailed protocol for a serological assay, antigen production, and test setup. Curr Protoc Microbiol. 2020;57:
e100 . DOIPubMedGoogle Scholar - Bhatnagar J, Gary J, Reagan-Steiner S, Estetter LB, Tong S, Tao Y, et al. Evidence of severe acute respiratory syndrome coronavirus 2 replication and tropism in the lungs, airways, and vascular endothelium of patients with fatal coronavirus disease 2019: an autopsy case series. J Infect Dis. 2021;223:752–64. DOIPubMedGoogle Scholar
- Vogel TP, Top KA, Karatzios C, Hilmers DC, Tapia LI, Moceri P, et al. Multisystem inflammatory syndrome in children and adults (MIS-C/A): Case definition & guidelines for data collection, analysis, and presentation of immunization safety data. Vaccine. 2021;39:3037–49. DOIPubMedGoogle Scholar
- Magro C, Mulvey JJ, Berlin D, Nuovo G, Salvatore S, Harp J, et al. Complement associated microvascular injury and thrombosis in the pathogenesis of severe COVID-19 infection: A report of five cases. Transl Res. 2020;220:1–13. DOIPubMedGoogle Scholar
Figure
Table
Cite This ArticleOriginal Publication Date: September 24, 2021
Table of Contents – Volume 27, Number 11—November 2021
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Heather N. Grome, Tennessee Department of Health, Communicable Diseases and Emergency Preparedness Division, 710 James Robertson Pkwy, Nashville, TN 37243, USA
Top