Volume 28, Supplement—December 2022
SUPPLEMENT ISSUE
Clinical
Clinical and Economic Impact of COVID-19 on Agricultural Workers, Guatemala1
Cite This Article
Citation for Media
Abstract
We evaluated clinical and socioeconomic burdens of respiratory disease in banana farm workers in Guatemala. We offered all eligible workers enrollment during June 15–December 30, 2020, and annually, then tracked them for influenza-like illnesses (ILI) through self-reporting to study nurses, sentinel surveillance at health posts, and absenteeism. Workers who had ILI submitted nasopharyngeal swab specimens for testing for influenza virus, respiratory syncytial virus, and SARS-CoV-2, then completed surveys at days 0, 7, and 28. Through October 10, 2021, a total of 1,833 workers reported 169 ILIs (12.0 cases/100 person-years), and 43 (25.4%) were laboratory-confirmed infections with SARS-CoV-2 (3.1 cases/100 person-years). Workers who had SARS-CoV-2‒positive ILIs reported more frequent anosmia, dysgeusia, difficulty concentrating, and irritability and worse clinical and well-being severity scores than workers who had test result‒negative ILIs. Workers who had positive results also had greater absenteeism and lost income. These results support prioritization of farm workers in Guatemala for COVID-19 vaccination.
Essential workers have been at greater risk for COVID-19 than for the general population, but little is known about the risk to persons working within the agricultural sector in low- to middle-income countries (LMICs) (1–3). Limited data from the United States have demonstrated a high burden of SARS-CoV-2 in this population (1); many agricultural workers continued working throughout the pandemic (4). In LMICs, agricultural workers play a critical role in food security and represent a major economic force. In Guatemala, these workers are 35% of the overall labor force, and agricultural products account for 45% of all exports and 11.3% of total gross domestic product (5). Guatemala is also a major trading partner of the United States, exporting US $2.1 billion in agricultural products annually, including nearly 50% of the banana supply of the United States (6). Therefore, agricultural workers in Guatemala and similar LMICs are arguably essential not only for local food security but also for the food security of international trading partners, such as the United States.
In addition to increased risk for exposure to SARS-CoV-2, the virus that causes COVID-19, persons working in the agricultural sector might also be at increased risk for poor clinical outcomes from COVID-19 because of a high prevalence of comorbidities associated with environmental stress, such as chronic kidney disease of unknown origin (Mesoamerican nephropathy) (7–9). Economic outcomes, such as work absenteeism and decreased job performance while working (presenteeism), are also critical factors, as is the case with influenza (10–14). Because agricultural workers are often the primary income earners for their households, the consequences may extend to their households and communities. Despite the increased clinical and economic vulnerability of agricultural workers and their critical role in global food security, little is known about the socioeconomic consequences of COVID-19 and other respiratory illnesses among this essential workforce, and the subsequent effects on their households and communities.
The Agricultural Workers and Respiratory Illness Impact (AGRI) Study was designed as an influenza cohort and expanded to include other viral respiratory pathogens, including SARS-CoV-2. The study has 2 primary aims: to characterize the clinical and socioeconomic outcomes of acute respiratory viral infections among farm workers in Guatemala, and to measure the effectiveness of a workplace-based vaccination program in improving these outcomes. Here, we provide a comprehensive description of the AGRI cohort and a summary of clinical and economic outcomes from the first year of virologic surveillance.
Study Setting and Population
This 5-year study was conducted within a large banana farm in the coastal lowlands of southwestern Guatemala. Farm workers are exposed to high temperatures and humidity and are at risk for environment-associated chronic medical conditions, such as chronic kidney disease of unknown origin (7,15). Previous surveys (2015, 2017–2018) found a predominantly young, male, and economically vulnerable workforce. Farmworkers are typically the sole income earners for their households and report high rates of food insecurity, similar to other agribusiness workers in the region and migrant worker populations in the United States (16,17). The regional population experiences high levels of food insecurity, stunting, poverty, and communicable diseases and low access to healthcare (18,19).
As is typical in many agribusinesses, field workers and packaging workers receive baseline pay plus daily bonuses based on productivity recorded by the company. Managers and workers in administrative job categories are paid by day. Workers who become ill and receive excused absences from their managers receive two thirds of baseline pay for the duration of the excused absence, up to a maximum of US $15.60/day. Workers with laboratory-confirmed SARS-CoV-2 are mandated to quarantine at home with excused absences for up to 2 weeks.
All eligible workers within the 9 banana farm worksites were offered enrollment in the study during June 15‒December 30, 2020, and annually thereafter. Inclusion criteria were age >18 years, plans to remain employed by the agribusiness for >1 year, access to a telephone, and agreement to enable use of company-based absenteeism and job performance records. For this analysis, participant follow-up was performed through October 10, 2021; all study procedures (testing and follow-up) performed after that date were considered missing, even if the associated influenza-like illness (ILI) case was previously identified.
After written informed consent was obtained, study nurses collected contact information and demographic, occupational, socioeconomic, and clinical data, including risk factors for severe COVID-19. Workers provided enrollment and annual blood specimens that were screened for markers of chronic kidney disease (e.g., estimated glomerular filtration rate [20]), SARS-CoV-2 nucleocapsid IgG (Elecsys Immunoassay; Roche, https://www.roche.com), and in some instances SARS-CoV-2 neutralizing antibodies (Beckham/Santiago Laboratories, University of Colorado, Aurora, CO, USA). Workers leaving employment had exit interviews and were removed from the study, but data collected during their employment were retained in the study database.
Surveillance for ILI
After enrollment, all workers began prospective active surveillance for ILI, initially defined as a self-reported fever/temperature >38°C and cough in the previous 10 days, to focus on detection of influenza (21). In January 2021, the ILI case definition was expanded to include fever, cough, or shortness of breath in the previous 10 days (COVID-19–like illness [22]), to increase sensitivity of COVID-19 case detection (23).
We used 3 strategies for detecting ILI. The first strategy was symptom screening through workers self-reporting symptoms to a study nurse during weekly worksite visits, work supervisors routinely querying workers for cough and fever at daily team meetings, and telephone contact to a study nurse by workers experiencing symptoms at any time. The second was sentinel surveillance of all workers who had ILI and presented to worker health posts within the farm. The third was active monitoring and ILI screening phone calls to absent workers identified on the company absenteeism registry. During worksite visits, study nurses visited worksites at given times each week, and workers were able to self-report to the nurse at that time. Work supervisors (or nurses at health posts) could also notify the study team on behalf of workers after obtaining their permission. In February 2021, absenteeism calls were discontinued because those ILI case-patients were consistently identified through other surveillance approaches.
Syndromic Illness Characterization
Study nurses interviewed workers who had ILI and collected clinical, epidemiologic, and outcome data for the workers and general epidemiologic and socioeconomic outcome data for their households. Study nurses also collected nasopharyngeal swab specimens, which were placed in viral transport medium and tested within 24 hours for SARS-CoV-2 by using the Q COVID rapid antigen test (Q-NCOV-01G; Biosensor SD, https://www.sdbiosensor.com) (24). Aliquots were also tested for influenza A/B viruses and respiratory syncytial virus (RSV) by using the Cobas Liat Influenza A/B (and RSV) real-time reverse transcription PCR (RT-PCR) instrument (Roche) (25). Patients who had ILI and tested positive for SARS-CoV-2, influenza, or RSV are hereafter referred to as SARS-CoV-2‒positive ILI, influenza-positive ILI, or RSV-positive ILI, respectively. The first 40 available ILI specimens collected through April 2021 and shipped to the University of Colorado were also tested for an additional 15 respiratory pathogens by using the multiplex BioFire FilmArray RP2.1 assay (26). Viral testing results were shared with participants when available (usually within 24 hours) and weekly with the Guatemala Ministry of Health.
Clinical and Socioeconomic Outcome Assessments
The study relied on a case‒cohort study design to measure self-reported clinical and socioeconomic outcomes. All persons in the overall cohort with ILI were considered to be case-patients. Each week, a subcohort of 15 enrolled workers who did not have ILI in the preceding 28 days were selected at random (≈5% of the cohort/month) as controls. Study nurses administered follow-up surveys over the telephone to case-patients at 1 and 4 weeks after their ILI visit. Controls were notified that they had been selected (day 0) and received the same surveys 1 and 4 weeks later; controls did not undergo diagnostic testing, and a control who had ILI develop during the 4-week follow-up was considered to be a case-patient at the time of illness.
Clinical and well-being outcomes were collected by using the Influenza Intensity and Impact Questionnaire (FluiiQ) Inventory (27), which is a validated Spanish-language outcome measure designed for clinical and epidemiologic outpatient studies of influenza and RSV. The inventory consists of 13 items for symptom severity, a combined systemic score (7 items) and respiratory score (6 items). The well-being scores are impact on daily activities score (7 items), impact on emotions score (4 items), and impact on others score (5 items). Each combined score is averaged by the number of individual items such that all scores are 0‒3; a higher score indicated greater severity or negative impact on well-being. The follow-up surveys also collected health-seeking behavior (e.g., hospitalization, medication use).
During follow-up surveys, economic outcomes were assessed by using questions adapted from the 2016 World Health Organization Manual for Estimating the Economic Burden of Seasonal Influenza (28) and supplemented with the World Bank National Survey of Living Conditions (29), which includes a Spanish translation (La Encuesta Nacional de Condiciones de Vida) used in Guatemala (30). The survey collected data on direct medical costs, direct nonmedical costs (i.e., transportation), and indirect costs related to loss of productivity (i.e., absenteeism) for the worker and the household. Results were compared with the basic food basket price in Guatemala, which reflects the minimum kilocalories intake (2,262 kilocalories) for a 4.77-member household for 1 month (US $386.30 in March 2021) (31). Although not included in this analysis, company-reported individual-level data were linked to workers, including absenteeism, productivity metrics (task-specific units of production, such as tons of bananas harvested per day), and wages.
Statistical Analysis
We calculated incidence density (number of cases per person-time of follow-up) of ILI and pathogen-specific ILI. We used descriptive statistics to calculate differences between clinical and socioeconomic outcomes between groups. For normally distributed continuous variables, we calculated means and SDs and used the Student t-test to determine major differences between groups. For non–normally distributed continuous variables, we calculated medians and interquartile ranges and used the Wilcoxon rank-sum test to determine major differences between groups. For categorical variables, we used χ2 and Fischer exact tests to determine major differences in distribution of categories between groups. For all analyses, p<0.05 was considered statistically significant.
Ethics
The study was approved by the Colorado Multiple Institutional Review Board (protocol #19-1836) and the Guatemala Ministry of Health National Ethics Committee (HRMC-560-2020). The local Southwest Trifinio Community Advisory Board for Research agreed to the study. Workers receive no compensation for study participation.
During June 15, 2020‒October 10, 2021, a total of 2,371 workers were screened for enrollment; 160 (6.7%) were ineligible, and 378 (17.1%) declined participation (Figure 1). Of the 1,833 enrolled participants (Table 1), 1,590 (86.7%) remained active in the study as of October 10, 2021, representing 1,402.9 person-years of surveillance. Workers who declined participation were slightly younger than participants (29.6 vs. 30.9 years; p<0.01) but had similar sex distribution and ethnicity.
Most workers were male (84.1%) and worked in the fields (69.0%). Self-reported chronic medical conditions were uncommon except for obesity (body mass index >30 kg/m2, 11.3%) and kidney disease (3.2%); 12.8% of workers (n = 234) took medications, most of whom (n = 122, 52%) took vitamins, followed by pain relievers/anti-inflammatory drugs (14%), antimicrobial drugs (7%), diabetes-related medications (7%), and proton pump inhibitors (6%). Only 5.9% reported ever having received an influenza vaccination, including 17 (6.4%) of 267 workers who self-reported chronic diseases. Workers began to receive COVID-19 vaccination through the workplace in August 2021 (ChAdOx1, AstraZeneca, https://www.astrazeneca.com; and mRNA-1273, Moderna, https://www.modernatx.com). Of 1,334 workers enrolled during June‒December 2020 who had samples available, 616 (46.2%) were reactive for SARS-CoV-2 nucleocapsid IgG.
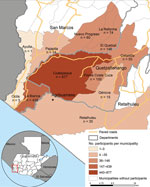
Household size averaged 5.7 persons (3.3 adults, 2.3 children), and half the workers (n = 877; 48.2%) lived the urban municipality of Coatepeque; the study catchment area was ≈2,600 km2 (Figure 2). Median self-reported monthly income for the individual worker was US $337.20 (interquartile range $311.30‒$389.10) and for the household was US $363.20 (interquartile range $324.30‒$505.80); 58.0% of workers reported being worried about the inability to purchase food in the preceding 12 months.
Asymptomatic Control Subjects
Of the 915 asymptomatic randomly selected controls (August 10, 2020–October 10, 2021), the study team was able to contact 696 (76.0%) by telephone. There were no significant differences in enrollment characteristics between those contacted and those not contacted. Of the 696 controls who were contacted initially, 623 (89.5%) were successfully contacted at 1 week and 588 (84.4%) at 4 weeks.
Absenteeism
During August 31, 2020‒February 19, 2021, a total of 36 workers (51.4%) had >1 day of work absence. Study personnel contacted 504 (68.5%) after 3 attempts, and there were no differences between contacted and uncontacted workers other than number of children (2.7 vs. 2.2; p<0.01). We compiled risk associations for absenteeism (Appendix Table 1).
Respiratory Illnesses
During June 15, 2020‒October 10, 2021, the study identified 169 ILI episodes occurring among 145 persons; of those, 136 (93.8%) persons (for 157 ILI episodes) completed the 7-day follow-up survey and 129 (89.0%) persons (for 149 ILI episodes) completed the 28-day follow-up survey by completion of analysis (Appendix Table 2). The mean (+SD) number of days of fever at the time of testing was 3.3 (+2.0) days and of cough was 3.3 (+1.9) days; 97.5% of samples were collected <7 days after symptom onset. Of the 153 ILI episodes (among 132 unique persons) who had completed SARS-CoV-2 antigen testing by completion of analysis, 43 (28.1%) were positive for SARS-CoV-2. Of 151 ILI episodes (among 131 persons) who had complete influenza and RSV RT-PCR testing, 6 (3.7%) were RSV positive and 0 were influenza positive.
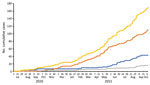
Incidence density for ILI was 12.0/100 person-years and for SARS-CoV-2‒positive ILI was 3.1/100 person-years (Figure 3). The ILI and COVID-19 incidence densities for workers who were nucleocapsid IgG‒negative at enrollment (n = 718) were 7.1/100 person-years and 2.3/100 person-years, respectively. For workers who were positive for nucleocapsid IgG positive at enrollment (n = 616), ILI incidence density was 4.5/100 person-years and COVID-19 incidence density 0.4/100 person-years. Older age was associated with greater risk for SARS-CoV-2‒positive ILI compared with SARS-CoV-2‒negative ILI (mean 35.0 years vs. 29.6 years; p = 0.001); there was no significant difference by sex, presence of any comorbidity, or obesity.
BioFire FilmArray RP2.1 testing (n = 40) on available specimens confirmed 9 of 9 SARS-CoV-2 infections tested and 1 of 1 RSV infection and identified an additional 8 picornaviruses (rhinovirus/enterovirus target on FilmArray) and 6 seasonal coronavirus (3 NL63, 1 OC43, and 2 N229E) ILI cases. The adult worker was usually the index case-pateint within the household for SARS-CoV-2 ILI (>80%) infections (Table 2) and ILI (>85%) (Appendix Table 2).
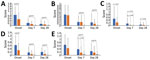
Workers who had SARS-CoV-2‒positive ILI had longer fever duration at the time of diagnosis (day 0; 3.3 days vs. 2.3 days; p<0.01) and increased frequency of anosmia (44.2% vs. 17.3%; p<0.01) and dysgeusia (48.8% vs. 24.6%; p<0.01), compared with SARS-CoV-2‒negative workers (Table 2). SARS-CoV-2 case-patients were also more likely to have difficulty concentrating (41.9% vs. 20.9%; p = 0.01), irritability (58.1% vs. 33.6%; p = 0.01), and dependence on others (37.2% vs. 20.9%; p = 0.04). SARS-CoV-2‒positive workers had higher systemic FluiiQ severity scores (indicating greater disease severity) at diagnosis than did SARS-CoV-2‒negative workers, but other differences in clinical scores remained nonsignificant. SARS-CoV-2‒positive workers reported worse impact scores for daily activities (0.50 vs. 0.22; p = 0.01) and emotions (0.62 vs. 0.31; p<0.01) than for SARS-CoV-2‒negative workers at diagnosis and worse impact on others score at day 7 (0.37 vs. 0.16; p = 0.03), but all other FluiiQ well-being scores showing a similar nonsignificant trend (Table 2; Figure 4). Among ILI cases, we found no significant difference in FluiiQ score based on age, sex, and presence of any comorbidity or obesity. We compiled clinical outcomes of workers who had ILI episodes versus asymptomatic controls (Appendix Table 2).
Economic Outcomes
Compared with SARS-CoV-2‒negative workers who had ILI, SARS-CoV-2‒positive workers had greater self-reported lost income (median US $127.10 vs. $0; p<0.01), and combined (healthcare, transportation, lost wages) total cost (US $147.90 vs. US $12.70; p<0.01) at day 7 (reported over the preceding 2 weeks) (Figure 5). Workers infected with SARS-CoV-2 also had more days of work absence (p<0.01); most (81.8%) had >5 days of work absence. Household expenditures on fruits/vegetables were higher at day 7 for SARS-CoV-2‒positive workers vs. SARS-CoV-2‒negative workers who had ILI (US $19.50 vs. US $13.00; p< 0.01). Differences for all other household expenditures between SARS-CoV-2 test-positive and test-negative workers were not statistically significant.
As of October 10 2021, farm workers in Guatemala in this prospective cohort study experienced a substantial burden of acute respiratory illness during the COVID-19 pandemic, of which 1/4 tested positive for SARS-CoV-2; those with COVID-19 had greater disease severity, absenteeism, and economic losses than workers with SARS-CoV-2‒negative ILI. Similar to limited data for the United States (1), farm workers in Guatemala were at risk for SARS-CoV-2 infection (3.1 cases/100 person-years) throughout 2020–2021. Nucleocapsid IgG at enrollment was protective against subsequent disease; additional analyses will explore this observation. Compared with other members of their households, the agricultural workers nearly always had the index symptomatic case. These findings, along with the critical role agricultural workers play in Guatemala and global food security (4,6), lend support to the prioritization of vaccinating agricultural workers against COVID-19.
Although preliminary, our findings suggest COVID-19 illness was associated with greater overall clinical severity and impairment, which persisted at 7-day and 28-day after illness, than for non‒SARS-CoV-2 ILI cases. COVID-19 symptoms were consistent with those reported elsewhere; higher frequencies of anosmia and dysgeusia and prolonged fever differentiating COVID-19 from other ILI cases. COVID-19 was strongly associated with irritability and difficulty concentrating, consistent with postacute sequelae of SARS-CoV-2 (long COVID) (32,33). The irritability and inability to concentrate, which persisted in some workers at both 7 and 28 days, might place workers at risk (e.g., when using machetes to harvest bananas and when operating heavy equipment). The FluiiQ well-being scores, which include socioemotional and functional activities, generally indicated more severe illness among workers who had COVID-19 compared with workers who had another ILI at the time of diagnosis and day 7; the trend was nonsignificant at 28 days. It is unknown to what extent symptoms or sequelae persist beyond 28 days in this population.
Agricultural workers in this cohort experienced a major economic impact from COVID-19. Self-reported data suggest a major difference in absenteeism, lost earnings, and total costs between COVID-19 and other ILI cases. Median monthly household income (US $363.20), already just below the mean basic monthly food basket price in Guatemala (US $386.30), was reduced greatly for workers who had COVID-19 (median lost income US $127.10, median total cost of illness US $147.90), placing these households at increased risk for food insecurity and economic hardship. Economic insecurity is one of the primary drivers of emigration from Guatemala (34,35); thus, the economic impact and policy implications of COVID-19 on these agricultural workers and their households, as well as others in similar settings, might extend beyond the borders of Guatemala.
Although SARS-CoV-2 was the most frequently detected respiratory pathogen among workers who had ILI, we detected no cases of influenza and only 6 cases of infection with RSV. Influenza and RSV circulate year-round in Guatemala and comprise a substantial proportion of ILI cases in population-based studies in Central and South America (36–39). The lower incidence observed in our cohort suggested mitigation strategies (primarily closing of schools, mask use, and some level of physical distancing) might have been effective in limiting some transmission of influenza and RSV. The observation cases of rhinovirus/enterovirus and seasonal coronaviruses (NL63, OC43, and N229E) in a subset of our cohort is consistent with other reports (40,41), although the reasons for these detections despite physical distancing measures merit further study. The AGRI cohort and similar studies will provide useful observations on the effectiveness of population-based preventive measures, such as vaccines, on the burden of respiratory pathogens. Also, our data demonstrated that syndromic surveillance in the workplace is a feasible population-based approach to rapidly characterize an emerging pathogen.
The AGRI study design had some inherent strengths and limitations. Although the study included weekly visits to worksites to identify symptomatic ILI case-patients, it still required some level of self-reporting to study personnel, and therefore might underestimate incidence. Workers with laboratory-confirmed SARS-CoV-2 are required to isolate and might be incentivized to underreport illness to avoid lost wages, thus providing a bias toward lower incidence and more severe cases of disease being reported. Required isolation probably increased duration of absenteeism for workers who are SARS-CoV-2 positive, although it still reflected the consequences of COVID-19 in this population. Self-reported study outcomes are also subject to recall bias, which we aimed to minimize by including control subjects who had similar follow-up. Laboratory test results are provided to the worker when available; thus self-reported outcomes might be impacted by diagnostic bias.
We did not perform pathogen testing on controls. We used an antigen test for detection of SARS-CoV-2 infection and an ELISA for detection of nucleocapsid IgG, which might have decreased performance compared with PCR and virus neutralization assays, respectively. Testing was nearly always (>97%) performed within 7 days of symptom onset, and future studies will compare various testing approaches. Future studies will also include company-reported data, which will provide a more objective assessment of wages, enabling us to compare self-reported and company-reported metrics. Finally, to decrease the risk for healthy worker bias (42), the study collected postacute (28-day) outcomes on all ILI case-patients and will ultimately measure loss of employment (using company data) as an outcome measure of ILI.
In conclusion, preliminary data from the AGRI cohort suggest major clinical and socioeconomic impacts of respiratory illnesses, especially COVID-19, on agricultural workers in Guatemala. The study demonstrates the feasibility and value of conducting workforce-based syndromic surveillance during epidemic activity and uses several innovative approaches to measure disease outcomes in acute and postacute settings, such as active surveillance and molecular diagnostics within a large banana farm and company-reported economic measures. It also provides a more comprehensive assessment of how communicable diseases economically effect an essential, yet vulnerable, workforce population and their households. Given the high clinical and economic burden of COVID-19 among agricultural workers, and their probable role in household transmission of COVID-19, our results support prioritizing persons working in the agricultural sector for vaccination against COVID-19, potentially through the workplace.
Dr. Olson is an associate professor of pediatric infectious diseases and epidemiology in Department of Pediatrics, Center for Global Health, University of Colorado School of Medicine, Aurora, CO. His primary research interest is integration of novel surveillance systems and field-based molecular diagnostics to study the burden and impact of emerging infectious diseases, host response, and effectiveness of community-based interventions, such as vaccines.
Acknowledgments
We thank the University of Colorado Trifinio Research Team, the University of Colorado Center for Global Health administration, Daniel Jernigan, the Centers for Disease Control and Prevention, and AgroAmerica for contributions; Margot Charette for assistance with mapping; the Colorado State University Diagnostic Laboratory for use of facilities; the Colorado State University Office of the Vice President for Research for providing funding instrumentation; Richard Osborne and Measured Solutions for use of the FluiiQ instrument and interpretation of results; and the Trifinio community for providing study participants.
This study was supported by the National Institutes of Health (NIH)/National Institute of Allergy and Infectious Diseases grant 1K23AI143967, Centers for Disease Control and Prevention (CDC)‒CAR/CGH CDC grant GH002243, and investigator-initiated contributions by Roche Molecular Systems, Roche Diagnostics, and Sanofi Pasteur. D.O. was supported by NIH/National Center for Advancing Translational Sciences Colorado CTSI grant UL1 TR001082 and the Children’s Hospital of Colorado Research Scholar Award. K.Q. was supported by NIH grant 1F32AI150123.
D.O., M.C., M.L., F.H., H.M., K.E., L.S.N., and E.J.A. developed the study and methods, performed investigations, and wrote the paper; G.G., E.B., A.N.C., N.R., K.A., G.M., G.A.B., D.B., K.L., M.S., K.Q., and G.E. developed methods, performed investigations, and administered the study; M.L., M.G., J.M., A.N.C., C.I., L.M.D., E.Z., and E.A.B. analyzed data, visualized the study, and wrote the paper; and D.O., M.C., and E.J.A, supervised and administered the study.
D.O. received grant funding from Roche and Sanofi Pasteur. F.G.H. has served as a consultant to Genentech, Roche, Shionogi, and other companies involved in development or marketing of influenza therapeutics or vaccines. He has received honoraria from the University of Alabama Antiviral Drug Discovery and Development Consortium for Scientific Advisory Board work and from the World Health Organization for document preparation related to influenza. K.M.E. received grant funding from NIH and CDC; is a consultant to Bionet and IBM; and is a member of Data Safety and Monitoring Committees for Sanofi, X-4 Pharma, Seqirus, Moderna, Pfizer, Merck, and Roche.
References
- Lewnard JA, Mora AM, Nkwocha O, Kogut K, Rauch SA, Morga N, et al. Prevalence and clinical profile of SARS-CoV-2 infection among farmworkers in Monterey County, California: June‒November, 2020. Emerg Infect Dis. 2021;27:1330–42. DOIPubMedGoogle Scholar
- Magnusson K, Nygård K, Methi F, Vold L, Telle K. Occupational risk of COVID-19 in the first versus second epidemic wave in Norway, 2020. Euro Surveill. 2021;26:
2001875 . DOIPubMedGoogle Scholar - Stringhini S, Zaballa ME, Pullen N, de Mestral C, Perez-Saez J, Dumont R, et al.; SEROCoV-WORK + Study Group. Large variation in anti-SARS-CoV-2 antibody prevalence among essential workers in Geneva, Switzerland. Nat Commun. 2021;12:3455. DOIPubMedGoogle Scholar
- Ramos AK, Lowe AE, Herstein JJ, Schwedhelm S, Dineen KK, Lowe JJ. Invisible no more: the impact of COVID-19 on essential food production workers. J Agromed. 2020;25:378–82. DOIPubMedGoogle Scholar
- Duff A, Padilla A. Latin America: agricultural perspectives; 2015 [cited 2022 Mar 16]. https://economics.rabobank.com
- Office of the United States Trade Representative. Guatemala [cited 2022 Mar 15]. https://ustr.gov/countries-regions/western-hemisphere/guatemala
- Dally M, Butler-Dawson J, Krisher L, Monaghan A, Weitzenkamp D, Sorensen C, et al. The impact of heat and impaired kidney function on productivity of Guatemalan sugarcane workers. PLoS One. 2018;13:
e0205181 . DOIPubMedGoogle Scholar - Brackbill RM, Cameron LL, Behrens V. Prevalence of chronic diseases and impairments among US farmers, 1986-1990. Am J Epidemiol. 1994;139:1055–65. DOIPubMedGoogle Scholar
- Butler-Dawson J, Krisher L, Asensio C, Cruz A, Tenney L, Weitzenkamp D, et al. Risk factors for declines in kidney function in sugarcane workers in Guatemala. J Occup Environ Med. 2018;60:548–58. DOIPubMedGoogle Scholar
- Keech M, Beardsworth P. The impact of influenza on working days lost: a review of the literature. Pharmacoeconomics. 2008;26:911–24. DOIPubMedGoogle Scholar
- Molinari NA, Ortega-Sanchez IR, Messonnier ML, Thompson WW, Wortley PM, Weintraub E, et al. The annual impact of seasonal influenza in the US: measuring disease burden and costs. Vaccine. 2007;25:5086–96. DOIPubMedGoogle Scholar
- de Francisco Shapovalova N, Donadel M, Jit M, Hutubessy R. A systematic review of the social and economic burden of influenza in low- and middle-income countries. Vaccine. 2015;33:6537–44. DOIPubMedGoogle Scholar
- Burckel E, Ashraf T, de Sousa Filho JP, Forleo Neto E, Guarino H, Yauti C, et al. Economic impact of providing workplace influenza vaccination. A model and case study application at a Brazilian pharma-chemical company. Pharmacoeconomics. 1999;16:563–76. DOIPubMedGoogle Scholar
- Mota NV, Lobo RD, Toscano CM, Pedroso de Lima AC, Souza Dias MB, Komagata H, et al. Cost-effectiveness of sick leave policies for health care workers with influenza-like illness, Brazil, 2009. Emerg Infect Dis. 2011;17:1421–9. DOIPubMedGoogle Scholar
- Johnson RJ, Wesseling C, Newman LS. Chronic kidney disease of unknown cause in agricultural communities. N Engl J Med. 2019;380:1843–52. DOIPubMedGoogle Scholar
- Findings from the National Agricultural Workers Survey (NAWS) 2015‒2016: a demographic and employment profile of United States farmworkers. Washington (DC): US Department of Labor, Employment and Training; 2018.
- Occupational health and safety fact sheet. Buda (TX): National Center for Farmworker Health; 2017.
- Asturias EJ, Heinrichs G, Domek G, Brett J, Shick E, Cunningham M, et al. The center for human development in Guatemala: an innovative model for global population health. Adv Pediatr. 2016;63:357–87. DOIPubMedGoogle Scholar
- Olson D, Lamb M, Lopez MR, Colborn K, Paniagua-Avila A, Zacarias A, et al. Performance of a mobile phone app-based participatory syndromic surveillance system for acute febrile illness and acute gastroenteritis in rural Guatemala. J Med Internet Res. 2017;19:
e368 . DOIPubMedGoogle Scholar - Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF III, Feldman HI, et al.; CKD-EPI (Chronic Kidney Disease Epidemiology Collaboration). A new equation to estimate glomerular filtration rate. Ann Intern Med. 2009;150:604–12. DOIPubMedGoogle Scholar
- Fitzner J, Qasmieh S, Mounts AW, Alexander B, Besselaar T, Briand S, et al. Revision of clinical case definitions: influenza-like illness and severe acute respiratory infection. Bull World Health Organ. 2018;96:122–8. DOIPubMedGoogle Scholar
- Reses HE, Fajans M, Lee SH, Heilig CM, Chu VT, Thornburg NJ, et al.; U.S. COVID-19 Household Investigation Team. Performance of existing and novel surveillance case definitions for COVID-19 in household contacts of PCR-confirmed COVID-19. BMC Public Health. 2021;21:1747. DOIPubMedGoogle Scholar
- Centers for Disease Control and Prevention. Update and interim guidance on outbreak of 2019 novel coronavirus (2019-nCoV) in Wuhan, China, January 7, 2020 [cited 2022 Mar 16]. https://emergency.cdc.gov
- Igloi Z, Velzing J, van Beek J, van de Vijver D, Aron G, Ensing R, et al. Clinical evaluation of Roche SD biosensor rapid antigen test for SARS-CoV-2 in municipal health service testing site, the Netherlands. Emerg Infect Dis. 2021;27:1323–9. DOIPubMedGoogle Scholar
- Koski RR, Klepser ME. A systematic review of rapid diagnostic tests for influenza: considerations for the community pharmacist. J Am Pharm Assoc (2003). 2017;57:13–9. DOIPubMedGoogle Scholar
- Creager HM, Cabrera B, Schnaubelt A, Cox JL, Cushman-Vokoun AM, Shakir SM, et al. Clinical evaluation of the BioFire respiratory panel 2.1 and detection of SARS-CoV-2. J Clin Virol. 2020;129:
104538 . DOIPubMedGoogle Scholar - Osborne RH, Norquist JM, Elsworth GR, Busija L, Mehta V, Herring T, et al. Development and validation of the influenza intensity and impact questionnaire (FluiiQ™). Value Health. 2011;14:687–99. DOIPubMedGoogle Scholar
- World Health Organization. Manual for estimating the economic burden of seasonal influenza. Geneva: The Organization; 2016.
- Living Standards Measurement Study (LSMS). 2019 [cited 2019 Feb 13] https://microdata.worldbank.org/index.php/catalog/lsms/about
- National survey of living conditions (ENCOVI) [in Spanish]. Guatemala City (Guatemala): National Institute of Statistics; 2014.
- Basic food basket (CBA) and expanded (CA). Guatemala City (Guatemala): National Institute of Statistics; 2021.
- Graham EL, Clark JR, Orban ZS, Lim PH, Szymanski AL, Taylor C, et al. Persistent neurologic symptoms and cognitive dysfunction in non-hospitalized Covid-19 “long haulers”. Ann Clin Transl Neurol. 2021;8:1073–85. DOIPubMedGoogle Scholar
- Hellmuth J, Barnett TA, Asken BM, Kelly JD, Torres L, Stephens ML, et al. Persistent COVID-19-associated neurocognitive symptoms in non-hospitalized patients. J Neurovirol. 2021;27:191–5. DOIPubMedGoogle Scholar
- Chishti M, Hipsman F. Increased Central American migration to the United States may prove an enduring phenomenon. Migration Information Source, 2016 [cited 2022Mar 16]. https://www.migratinpolicy.org
- National Immigration Forum. Push or pull factors: what drives Central American migrants to the U.S.? 2019 [cited 2022 Mar 16]. https://immigrationforum.org
- Durand LO, Cheng PY, Palekar R, Clara W, Jara J, Cerpa M, et al. Timing of influenza epidemics and vaccines in the American tropics, 2002-2008, 2011-2014. Influenza Other Respir Viruses. 2016;10:170–5. DOIPubMedGoogle Scholar
- Haynes AK, Manangan AP, Iwane MK, Sturm-Ramirez K, Homaira N, Brooks WA, et al. Respiratory syncytial virus circulation in seven countries with Global Disease Detection Regional Centers. J Infect Dis. 2013;208(Suppl 3):S246–54. DOIPubMedGoogle Scholar
- Vicari AS, Olson D, Vilajeliu A, Andrus JK, Ropero AM, Morens DM, et al. Seasonal influenza prevention and control progress in Latin America and the Caribbean in the context of the global influenza strategy and the COVID-19 pandemic. Am J Trop Med Hyg. 2021;105:93–101. DOIPubMedGoogle Scholar
- McCracken JP, Prill MM, Arvelo W, Lindblade KA, López MR, Estevez A, et al. Respiratory syncytial virus infection in Guatemala, 2007-2012. J Infect Dis. 2013;208(Suppl 3):S197–206. DOIPubMedGoogle Scholar
- Tang JW, Bialasiewicz S, Dwyer DE, Dilcher M, Tellier R, Taylor J, et al. Where have all the viruses gone? Disappearance of seasonal respiratory viruses during the COVID-19 pandemic. J Med Virol. 2021;93:4099–101. DOIPubMedGoogle Scholar
- Fong MW, Leung NHL, Cowling BJ, Wu P. Upper respiratory infections in schools and childcare centers reopening after COVID-19 dismissals, Hong Kong. Emerg Infect Dis. 2021;27:1525–7. DOIPubMedGoogle Scholar
- Chowdhury R, Shah D, Payal AR. Healthy worker effect phenomenon: revisited with emphasis on statistical methods–a review. Indian J Occup Environ Med. 2017;21:2–8. DOIPubMedGoogle Scholar
Figures
Tables
Cite This ArticleOriginal Publication Date: July 06, 2022
1An abstract of this article was presented at the Virtual Meeting of the International Society for Influenza and Other Respiratory Virus Diseases, October 19‒21, 2021; and at the 70th Annual Meeting of the American Society for Tropical Medicine and Hygiene, National Harbor, Maryland, USA, November 17‒21, 2021.
Table of Contents – Volume 28, Supplement—December 2022
| EID Search Options |
|---|
|
|
|
|
|
|


Please use the form below to submit correspondence to the authors or contact them at the following address:
Daniel Olson, Department of Pediatrics, Center for Global Health, University of Colorado School of Medicine, 13199 E Montview Blvd, Ste 310, Aurora, CO 80045, USA
Top