Volume 20, Number 3—March 2014
Dispatch
Role of Waddlia chondrophila Placental Infection in Miscarriage
Cite This Article
Citation for Media
Abstract
Waddlia chondrophila is an intracellular bacterium suspected to cause human and bovine abortion. We confirmed an association between antibodies against W. chondrophila and human miscarriage and identified this organism in placenta or genital tract of women who had had miscarriages. These results suggest a possible role of W. chondrophila infection in miscarriage.
Approximately 25% of pregnant women will experience at least 1 miscarriage (1,2). However, a cause is identified for only 50% of cases (3,4). Intracellular bacteria, which do not grow on media routinely used to isolate human pathogens from clinical samples, represent possible agents of miscarriage of unexplained etiology (4,5).
Waddlia chondrophila, a Chlamydia-related bacterium first identified in samples of bovine abortion tissues, has been associated with human miscarriages (6,7). In a study of 438 serum samples from women attending a recurrent-miscarriage clinic, seroprevalence of W. chondrophila was higher for women who had sporadic (31.9%) and recurrent (33.0%) miscarriages than for women who had uneventful pregnancies (7.1%; p<0.001) (6).
To further investigate the role of W. chondrophila in human miscarriage, we studied 386 women who had had miscarriages or uneventful pregnancies. In addition to serologic analysis, we used PCR and immunohistochemical analysis to detect W. chondrophila in placenta and vaginal samples.
During 2006–2009, a total of 386 women were prospectively enrolled from the obstetrical ward of the University Hospital of Lausanne (Table 1) (8). The miscarriage group was composed of 125 women given a diagnosis of an acute episode of miscarriage in the emergency gynecology unit. The control group was composed of 261 women attending a labor ward, having uneventful pregnancies, and having no history of miscarriage, stillbirth, or preterm labor. Age, black race, and number of lifetime sex partners were different between both groups.
Immunofluorescence testing was performed by using W. chondrophila as antigen as described (6). Eighty-four women had antibodies against W. chondrophila as demonstrated by positive immunofluorescence against total immunoglobulin (Table 1). Among them, 67 women had IgG titers ≥1:64 and 6 women had IgM titers ≥1:32 against W. chondrophila (FluolineG or FluolineM; bioMérieux, Marcy l'Etoile, France). IgG seroprevalence was higher among women who experienced miscarriage (23.2%) than among women who experienced an uneventful pregnancy (14.6%; p = 0.044) (Table 2). When women with and without antibodies against W. chondrophila were compared, their age, contact with animals, education, number of previous sex partners, previous contraceptive use, and place of residence (countryside/city) were not associated with a positive serologic result for W. chondrophila. However, a multivariate logistic regression model indicated that black women were more likely to have antibodies against W. chondrophila (odds ratio [OR] 3.15, 95% CI 1.39–7.16).
As reported (8), we observed an association between miscarriage and Chlamydia trachomatis IgG seropositivity. The association between W. chondrophila miscarriage and seropositivity remained significant even when adjusted for C. trachomatis serostatus and vice versa. In a multivariate logistic regression adjusted for both variables, C. trachomatis and W. chondrophila seropositivity remained independently associated with miscarriage (OR 2.42, 95% CI 1.22–4.79 and OR 1.87, 95% CI 1.08–3.22, respectively).
After extraction of DNA by using the QIAamp DNA Mini Kit (QIAGEN, Hilden, Germany), we tested all vaginal swab specimens and placenta samples by using a 16S rRNA Waddlia spp.–specific real-time PCR as described (9). No PCR inhibition was observed. Thirty-two samples (20 vaginal swab specimens and 12 placenta samples) were positive; no sample being positive in both types of samples. Ten of these positive PCR samples were from women who had had miscarriages; 9 of the 10 vaginal swab specimens had a positive PCR result (Tables 1, 2). Two of these 10 patients who had had miscarriages had IgG against W. chondrophila (patients 36 and 140). Patient 36 had the highest IgG titer (1,024) of the 386 women. Among the control group, 3 patients had IgG against W. chondrophila (titer ≥64). Among these women, 1 had IgG and IgM against W. chondrophila and 1 had only IgM against W. chondrophila (titer 32).
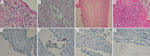
All placenta specimens were examined by a pedopathologist (Table 2; Figure 1, panels A–D). Samples from the 10 women who had miscarriages and positive PCR results showed various histologic features, including deciduitis, chorioamnionitis, and plasmocytes in the decidua, which are compatible with chronic endometritis. Two of the samples showed standard histologic results.
Placentas from the 32 PCR-positive women and 10 PCR-negative controls were tested for W. chondrophila by using immunohistochemical analysis with a specific rabbit polyclonal antibody as described (10). Three placentas showed positive cells (Table 2; Figure 1, panels E–H). Patients 523 and 535, who had had miscarriages, had positive serologic results for total Ig but negative results for IgG and IgM (Table 2). Patient 250 was a woman who had had an uneventful pregnancy and who had positive PCR results for a vaginal swab specimen but negative serologic results. Immunohistochemical analysis showed that W. chondrophila infects mainly cells of the glandular epithelium; W. chondrophila was not found in endothelial cells (Figure 1).
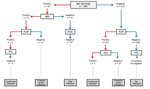
Five women showed strong evidence of W. chondrophila infection, which was confirmed by ≥2 diagnostic tests (Figure 2). Thus, 2 women who had had a miscarriage had IgM and IgG (titer 32) and positive PCR results. Three other women (2 who had had miscarriages and 1 control) showed positive results by PCR and immunohistochemical analysis. Moreover, 31 other women showed some evidence of acute infection (i.e., 27 with a positive PCR result and/or 4 with IgM against W. chondrophila).
Higher seroprevalence in the miscarriage group confirmed the association between miscarriage and W. chondrophila seropositivity observed in a study that investigated a population in London, UK (6). We also identified W. chondrophila DNA in the placenta and vagina of 32 women, including 10 who had had miscarriages. Among these 10 whose PCR result was positive, 4 were considered as having confirmed cases of infection because they also had positive serologic (n = 2) or immunohistochemical (n = 3) results. W. chondrophila in human tissue indicates that this intracellular bacterium might grow or persist within placental cells and might damage the placenta (11). The underlying mechanism of Waddlia-associated miscarriage may involve bacterial proteins, such as heat-shock protein 60, or production of inflammatory cytokines, such as tumor necrosis factor-α (5).
Detection of W. chondrophila in the vagina indicates that the infection might have originated after vaginal colonization. However, no association between sexual activity, use of condoms, and positive serologic results for W. chondrophila was reported in a study (seroprevalence 8.3%) of 517 young men in Switzerland (12).
We identified W. chondrophila in the human genital region. However, entry could occur at another site. W. chondrophila DNA has also been detected in sputa of patients with pneumonia (9,13), or other respiratory tract infections could disseminate to the uterus through the bloodstream. In contrast to our previous study findings (4), seropositivity for W. chondrophila was not associated with contact with animals.
This prospective study confirmed an association between W. chondrophila seropositivity and miscarriage. Four (3.2%) of 125 women who had had miscarriages were positive by serologic analysis and PCR or by PCR and immunohistochemical analysis and were considered as having confirmed cases of infection. One (0.4%) W. chondrophila infection was documented by 2 diagnostic tests in a women in the control group who had not had a miscarriage (p = 0.04). These results suggest a strong association between W. chondrophila infection and miscarriage among women (6,7). When a W. chondrophila–associated miscarriage is suspected, we recommend performing PCR on placenta and vaginal swab specimens and serologic analysis.
Dr Baud is an obstetrician at the University of Lausanne, Lausanne, Switzerland. His research interests are maternofetal medicine, emerging infectious causes of adverse pregnancy outcomes, and fetal therapy.
Acknowledgments
We thank the midwives and doctors for assistance during sampling; Sebastien Aeby for technical assistance; and Francoise Damnon, Karine Lepigeon, and Andre Baud for computer assistance.
This study was supported by an interdisciplinary grant from the University of Lausanne and partially by grants from the Swiss National Science Foundation (32C0B0-116445); the State Secretary for Education and Research, Bern, Switzerland (project no. C05.0141); European Cooperation in Science and Technology Action 855 (Animal Chlamydiosis and Zoonotic Implications); the Institute of Microbiology; and the Department of Obstetrics and Gynecology. D.B. was supported by the Société Académique Vaudoise through a Paul Blanc grant, the Société Industrielle et Commerciale de Produits Alimenlaires Fondation, an Air Canada travel grant, and the Fondation Leenaards through the Bourse pour la Relève Académique.
References
- Regan L, Rai R. Epidemiology and the medical causes of miscarriage. Best Pract Res Clin Obstet Gynaecol. 2000;14:839–54 . DOIPubMedGoogle Scholar
- Carrington B, Sacks G, Regan L. Recurrent miscarriage: pathophysiology and outcome. Curr Opin Obstet Gynecol. 2005;17:591–7. DOIPubMedGoogle Scholar
- Baud D, Greub G. Intracellular bacteria and adverse pregnancy outcomes. Clin Microbiol Infect. 2011;17:1312–22 .PubMedGoogle Scholar
- Baud D, Regan L, Greub G. Emerging role of Chlamydia and Chlamydia-like organisms in adverse pregnancy outcomes. Curr Opin Infect Dis. 2008;21:70–6. DOIPubMedGoogle Scholar
- Baud D, Thomas V, Arafa A, Regan L, Greub G. Waddlia chondrophila, a potential agent of human fetal death. Emerg Infect Dis. 2007;13:1239–43. DOIPubMedGoogle Scholar
- Baud D, Goy G, Osterheld MC, Borel N, Vial Y, Pospischil A, Waddlia chondrophila: from bovine abortion to human miscarriage. Clin Infect Dis. 2011.
- Baud D, Goy G, Jaton K, Osterheld MC, Blumer S, Borel N, Role of Chlamydia trachomatis in miscarriage. Emerg Infect Dis. 2011;17:1630–5. DOIPubMedGoogle Scholar
- Goy G, Croxatto A, Posfay-Barbe KM, Gervaix A, Greub G. Development of a real-time PCR for the specific detection of Waddlia chondrophila in clinical samples. Eur J Clin Microbiol Infect Dis. 2009;28:1483–6. DOIPubMedGoogle Scholar
- Borel N, Casson N, Entenza JM, Kaiser C, Pospischil A, Greub G. Tissue microarray and immunohistochemistry as tools for evaluation of antibodies against Chlamydia-like bacteria. J Med Microbiol. 2009;58:863–6. DOIPubMedGoogle Scholar
- Kebbi-Beghdadi C, Cisse O, Greub G. Permissivity of Vero cells, human pneumocytes and human endometrial cells to Waddlia chondrophila. Microbes Infect. 2011;13:566–74 PubMed. DOIPubMedGoogle Scholar
- Baud D, Jaton K, Bertelli C, Kulling JP, Greub G. Low prevalence of Chlamydia trachomatis infection in asymptomatic young Swiss men. BMC Infect Dis. 2008;8:45 . DOIPubMedGoogle Scholar
- Haider S, Collingro A, Walochnik J, Wagner M, Horn M. Chlamydia-like bacteria in respiratory samples of community-acquired pneumonia patients. FEMS Microbiol Lett. 2008;281:198–202. DOIPubMedGoogle Scholar
Figures
Tables
Cite This Article1These authors contributed equally to this article.
Table of Contents – Volume 20, Number 3—March 2014
| EID Search Options |
|---|
|
|
|
|
|
|
Please use the form below to submit correspondence to the authors or contact them at the following address:
Gilbert Greub, Center for Research on Intracellular Bacteria, Institute of Microbiology, University of Lausanne, Bugnon 48, 1011 Lausanne, SwitzerlandGilbert Greub, Center for Research on Intracellular Bacteria, Institute of Microbiology, University of Lausanne, Bugnon 48, 1011 Lausanne, Switzerland
Top